California MedicalAssistance Program(4260) |
At the state level, the Department of Health Services (DHS) administers the Medi-Cal Program. Other state agencies, including the California Medical Assistance Commission (CMAC) and the Departments of Social Services (DSS), Mental Health, Developmental Services, and Alcohol and Drug programs perform Medi-Cal functions under agreements with the DHS. At the local level, county welfare departments determine the eligibility of applicants for Medi-Cal and are reimbursed for those activities. The federal Health Care Financing Administration (HCFA) oversees the program to ensure compliance with federal law.
The budget proposes Medi-Cal expenditures totaling $18.4 billion in 1997-98. The General Fund portion of this spending ($6.9 billion) is essentially unchanged from estimated General Fund spending in the current year. The spending total for the Medi-Cal budget also includes an estimated $2.2 billion (federal funds and local matching funds) for payments to DSH hospitals, and about $1 billion of additional federal funds to match state and local funds budgeted elsewhere for programs operated by other departments.
Fee-for-Service. This is the traditional arrangement for health care in which providers are paid for each examination, procedure, or other service that they furnish. Beneficiaries may obtain services from any provider who has agreed to accept Medi-Cal payments. The Medi-Cal Program uses a variety of "utilization control" techniques (such as requiring prior authorization for some services) in order to avoid paying for medically unnecessary or duplicative services.
Managed Care. Prepaid health plans generally provide managed care. These plans receive monthly "capitation" payments from the Medi-Cal Program for each enrollee in return for providing all of the care needed by those enrollees. These plans are similar to health plans offered by many public and private employers. The DHS expects to have more than half of all Medi-Cal beneficiaries enrolled in managed care plans by the end of 1997-98. Beneficiaries in managed care choose a plan and then must use providers in that plan. Since payments to plans do not vary with the amount of service provided, there is much less need for utilization control. Instead, plans must be monitored to ensure that they provide adequate care to enrollees.
Categorically Linked Eligibles. Roughly four-fifths of the total number of Medi-Cal beneficiaries are in one of the two major cash-grant welfare programs: The Aid to Families with Dependent Children (AFDC) program, which assists low-income single-parent or unemployed families with children; and the Supplemental Security Income/State Supplementary program (SSI/SSP), which assists low-income aged, blind, and disabled persons. Anyone receiving a cash grant under either of these programs is automatically enrolled in Medi-Cal. (This automatic linkage changes under welfare reform, which replaces the AFDC program with the new Temporary Assistance for Needy Families--TANF--program, as we discuss later in this analysis.)
Categorically Related Eligibles (Medically Needy). The Medically Needy eligibility category provides Medi-Cal benefits to families and individuals who meet all of the requirements for either AFDC or SSI/SSP, but who do not apply for a grant or whose income disqualifies them from receiving a grant. Qualifying persons with incomes up to 133 percent of the June 1991 AFDC payment level receive benefits without having any share of cost. Qualifying persons with higher incomes may receive benefits in any month that their medical expenses cause them to "spend down" to the maximum income level.
Long-Term Care. This group includes persons in long-term care (for periods exceeding 30 days), other than categorically-linked persons. Technically, long-term care is not a separate eligibility category; most persons included in this group are Medically Needy. However, special eligibility and income rules apply to some long-term care beneficiaries. We note that this group has large costs in proportion to its size.
Other Women and Children. Medi-Cal coverage also is available to many children and pregnant women not covered under the categorical eligibility groups. Pregnant women (for pregnancy-related services only) and infants are covered up to family incomes of 200 percent of the federal poverty level. Children through age six are eligible for Medi-Cal coverage in families with incomes up to 133 percent of the poverty level, and children through age 13 are covered in families with incomes at or below the poverty level (this age limit increases by one year annually until it reaches age 18). Older children and pregnant women (for all services) are eligible for coverage in the Medically Indigent category if their family income meets the test for the Medically Needy category.
| Figure 10 | ||
| Who Is Eligible for Medi-Cal?
Major Eligibility Categories 1996-97 | ||
| (Dollars in Millions) | ||
| Category | Enrollees
b
(Thousands) |
Benefit
Costs c |
|
Categorically Linked Persons | ||
| Low-Income Families with Children
Must meet the July 16, 1996 AFDC eligibility criteria-- single-parent families and unemployed two-parent families. |
2,920 | $3,115 |
| SSI/SSP Recipients
Low-income aged, blind, or disabled persons. |
1,136 | 5,407 |
|
Categorically Related Persons | ||
| Medically Needy Persons ($1,190)a
Must meet AFDC or SSI/SSP requirements except for income, which may be up to 133 percent of June 1991 AFDC payment level. Persons with higher income may "spend down"to this level. |
545 | $1,577 |
| Long-Term Care
Persons in long-term care (other than those on SSI/SSP or AFDC), primarily persons qualifying as Medically Needy (but not included in Medically Needy amounts above). |
69 | 2,207 |
|
Other Women and Children | ||
| 200 percent of Poverty ($2,690)a
Pregnant women (pregnancy services only) and infants. |
128 | $340 |
| 133 percent of Poverty ($1,819)a
Children ages 1 through 6. |
93 | 55 |
| 100 percent of Poverty ($1,390)a
Children ages 6 through 13. |
32 | 13 |
| Medically Indigent ($1,190)a
Children 14 through 20 and pregnant women (all services)--same income as Medically Needy. |
305 | 508 |
|
Undocumented Persons | ||
| Illegal Immigrants
May qualify in any eligibility group, except those that are categorically linked. Services are limited to emergency, prenatal, and long-term care. |
290 | $642 |
| a Maximum monthly income (no share of cost) for a family of four. Includes $90 work expense disregard. Qualifying child care expenses would increase allowable monthly income by up to $350 for two children. | ||
| b Average monthly totals. | ||
| c Budget estimate, includes both state and federal funds. | ||
Illegal Immigrants. Undocumented immigrants (and nonimmigrant aliens) may receive emergency services (including labor and delivery), prenatal care, and long-term care, provided that they meet the other requirements of any Medi-Cal eligibility category.
Other Categories. Medi-Cal also covers some additional categories of persons, such as low-income adults in nursing facilities and low-income Medicare beneficiaries (for costs not covered by Medicare).
Funding Shifts Reduce General Fund Costs. Funding shifts assumed in the budget reduce General Fund spending by a net total of $316 million in 1997-98, primarily due to the following two major changes:
Budget Savings Proposals. The budget includes the following savings proposals, which reduce General Fund spending in 1997-98 by a combined total of $132 million:
| Figure 11 | |||||||
| Medi-Cal Expenditures
1991-92 Through 1996-97 | |||||||
| (Dollars in Billions) | |||||||
| 1991-92 | 1992-93 | 1993-94 | 1994-95 | 1995-96 | 1996-97 | Average
Annual Increase | |
| General Fund | $4.8 | $5.4 | $5.5 | $6.0 | $6.3 | $6.9 | 7.5% |
| All funds | 11.6 | 13.9 | 16.9 | 16.5 | 16.5 | 18.4 | 9.6 |
Medi-Cal spending totals also include several other recently-established programs that contributed to the increase in spending of federal funds, matched by local funds:
In addition, the Medi-Cal Program has expanded to cover personal care services and now provides more than $300 million of federal matching funds for the In-Home Supportive Services (IHSS) program, administered by the DSS.
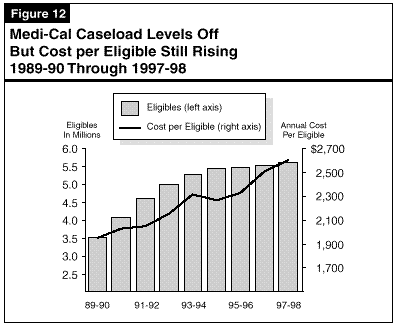
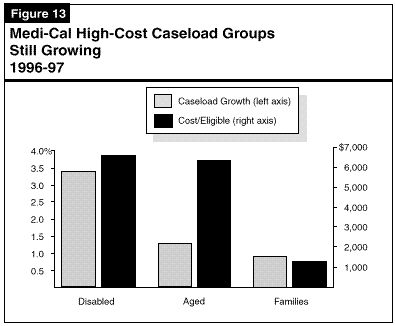
Reasons for Growing Cost Per Eligible. Most of the growth in cost per eligible is due to increases in medical care costs caused by inflation, new and more expensive technologies and drugs, and increased use of services. Some additional growth in the cost per eligible is due to a gradual shift to a more expensive "mix" of eligibles. Specifically, while the AFDC-linked caseload has been declining recently, the number of aged and disabled eligibles continues to grow. Figure 13 illustrates that eligibles in these growing segments of the caseload have an average annual benefit cost that is about five time higher than for AFDC recipients and other family eligibility groups.

Budget Overestimates Medi-Cal Caseload for AFDC/TANF Recipients We recommend reducing the proposed General Fund appropriation for the Medi-Cal Program by $37.6 million in 1996-97 and $70.6 million in 1997-98 because we project that Medi-Cal caseloads for AFDC-linked eligibles will be lower than the budget estimates. (Reduce 1996-97 deficiency appropriation by $37.6 million and Item 4260-101-0001 by $70.6 million.)
The largest group of persons on Medi-Cal (eligibles) consists of families and children who are linked to Medi-Cal because they receive public assistance grants under the AFDC/TANF program. This group comprises just over half of all Medi-Cal eligibles. The budget estimates that the average monthly number of Medi-Cal eligibles in this group will be 2.92 million in 1996-97 and will remain essentially unchanged in 1997-98. The number of AFDC-linked eligibles peaked at slightly over three million in 1994-95 and has been declining since then in line with reductions in the AFDC caseload (please see our analysis of the AFDC/TANF program for a discussion of AFDC caseload trends).
Caseload Currently Below Estimate and Likely to Decline Further. Current caseload data and our own projection of the AFDC-linked Medi-Cal caseload indicate that the budget's caseload estimate for the current year is too high and that the AFDC-linked caseload is likely to decline further in 1997-98, rather than remain constant as the budget projects. Figure 14 shows actual caseloads for this group from 1994-95 through December 1996, together with a comparison of the budget projections and our projections for 1996-97 and 1997-98. As shown in the figure, as of December 1996 the average annual number of AFDC-linked eligibles had declined to 2.90 million, which is about 30,000 eligibles below the level estimated by the budget. Furthermore, caseloads are likely to continue to decline due to continuation of the economic recovery and continuation of certain demographic trends (particularly slow growth in the number of women in their childbearing years and a moderation of unwed births to teens). Based on these factors, our caseload projections shown in Figure 14 indicate a continued decline in the number of AFDC-linked Medi-Cal eligibles through 1996-97 and 1997-98.
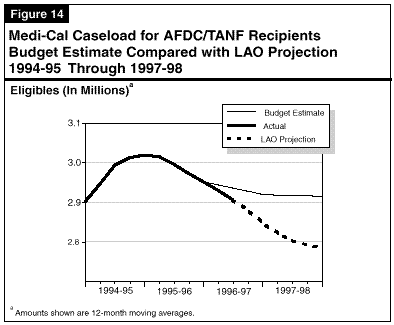
Compared with the budget estimate, our projection of the AFDC-linked Medi-Cal caseload is lower by 71,000 in the current year and by 128,000 in 1997-98 (in terms of average monthly eligibles). Based on the budget's estimated cost per eligible in this group, the total savings over the two years is $219.4 million, of which the General Fund share is $108.2 million ($37.6 million in 1996-97 and $70.6 million in 1997-98). Accordingly, we recommend that the budget proposal be reduced to reflect our caseload projections, which are based on more recent caseload information.
| Figure 15 | |
| Medi-Cal Budget Proposals
Related to Welfare Reform 1997-98 | |
| (Dollars in Millions) | |
| Proposal | General Fund
Fiscal Effect |
| Eliminate prenatal care for illegal immigrants | -$79.9 |
| Phase out long-term care for illegal immigrants |
-- |
| Restrict Medi-Cal for new legal immigrants to emergency services | -2.3 |
| Redetermine eligibility for legal immigrants losing SSI/SSP benefits | 17.0 |
| Redetermine eligibility for children losing SSI/SSP disability
coverage |
0.6 |
Restrictions Do Not Affect Emergency Medical Care. None of the immigrant restrictions in welfare reform affect emergency medical care. Consequently all immigrants who meet the general eligibility requirements for Medi-Cal will continue to be eligible, at a minimum, for emergency Medi-Cal services (plus public health vaccinations and other services related to the control or treatment of communicable diseases), and the state will continue to receive federal Medicaid matching funds for these services.
Illegal Immigrants--Prenatal, Long-Term, and County Indigent Care Potentially Restricted. Generally, the welfare reform law prohibits most federal, state, or local public benefits to illegal immigrants. However, the law allows states to provide such benefits to illegal immigrants (without federal funding) by enacting new laws. (Proposition 187, adopted by the voters in November 1994, also would prohibit nonemergency health care and other services for illegal immigrants, but that measure is enjoined by the courts pending the outcome of legal challenges.)
Based on the welfare reform law, DHS has issued proposed regulations eliminating nonemergency prenatal care and long-term care for illegal immigrants, which are existing Medi-Cal benefits funded entirely by the state. The budget assumes that the regulations eliminating prenatal care become effective July 1, 1997 and result in a General Fund savings of $79.9 million in 1997-98. The budget does not assume any savings from the elimination of long-term care services in 1997-98 (current cost of this program is $10.3 million annually). This is because the budget proposes legislation which would supersede the pending regulations and phase out the program by limiting it to persons already receiving care. We note that federal welfare reform also prohibits the provision of nonemergency health services to illegal immigrants by county indigent health programs.
Option to Restrict Current Legal Immigrants to Emergency Medi-Cal. The welfare reform law allows states to limit Medicaid benefits to emergency care for most current legal immigrants (those who entered the United States prior to August 22, 1996). The budget, however, does not propose that the state exercise this option. As a result, current legal immigrants will continue to be eligible for full-scope Medi-Cal services. In particular, this will allow continued Medi-Cal coverage for legal immigrants who will lose their eligibility for SSI/SSP grants this summer under welfare reform (unless they become citizens). These persons now receive Medi-Cal benefits automatically as SSI/SSP recipients. Although their SSI/SSP benefits and automatic Medi-Cal coverage will end, these individuals will be eligible to continue their Medi-Cal coverage as "medically needy" beneficiaries.
New Legal Immigrants Restricted to Emergency Services. Federally funded Medicaid benefits for most legal immigrants entering the country on or after August 22, 1996 will be restricted to emergency medical services for the first five years of residence. The budget proposes to revise state law to conform state Medi-Cal eligibility to this provision for a General Fund savings of $2.3 million in 1997-98. We discuss this proposal in more detail below.
The Governor's budget proposes legislation to limit Medi-Cal benefits to emergency services for most new legal immigrants who arrive in the United States on or after August 22, 1996. This proposal conforms with the provisions of the federal welfare reform law that limit new immigrants' eligibility for federally funded Medicaid benefits to emergency services. The budget estimates that this proposal will result in savings of $4.6 million ($2.3 million General Fund) in 1997-98.
Legislative Analyst's Office Savings Estimate Is $4.0 Million. The budget savings estimate is based on a monthly cost reduction of $8 per person and 3,340 new immigrants (other than refugees and asylees) enrolling in Medi-Cal each month. Based on more recent immigration data, however, we estimate that the monthly number of new immigrants will be about 25 percent less than the budget assumes. Our analysis of the department's cost information indicates that the per-person monthly savings will be slightly higher than the budget estimate--$9 versus $8. The net effect of these two adjustments is to reduce the savings associated with the budget proposal to $4.0 million ($1.9 million General Fund).
New Immigrants Currently Receiving Full-Scope Benefits. The DHS indicates that it believes that existing state law requires the state to provide full-scope Medi-Cal coverage to otherwise qualified legal immigrants without any distinction as to their date of entry. Consequently, DHS has not restricted benefits to new legal immigrants, and the state currently continues to claim federal matching funds for these expenses. It is not clear whether the federal government will ultimately allow these claims.
Savings from Emergency Services Restriction Is Relatively Small. The savings resulting from limiting Medi-Cal benefits to emergency services is equivalent to about 8 percent of the estimated cost of full-scope Medi-Cal benefits for new immigrants. Put another way, the cost of emergency services is about 92 percent of the cost of full-scope services. These estimates are based on the cost data for providing emergency services to illegal immigrants, the only group currently restricted to emergency services. These costs were then compared with the cost of providing full-scope services to recent legal immigrants (as approximated by cost data for providing full-scope Medi-Cal services to beneficiaries whose primary language is not English) and adjusted for demographic differences between the two groups.
There are several reasons why the cost of emergency Medi-Cal services is roughly comparable to the cost of full-scope services:
the practice in Texas, which limits each authorization for emergency services to the duration of the immediate medical problem.
Cost of Continuing Full-Scope Benefits Depends on Federal Policy. Although the General Fund savings from restricting benefits to new legal immigrants in 1997-98 is only $1.9 million (after our adjustments), the General Fund augmentation needed to continue full-scope services under existing state and federal laws could range from $4 million up to roughly $15 million, as shown in Figure 16. The amount will depend on how the federal government decides to reimburse states that choose to provide full-scope services. The $4 million cost assumes that the federal government uses a "cost neutrality" approach in which it will pay an amount that is equal to what it would have paid for emergency-only services--that is, the cost of emergency services when only those services are provided. These costs tend to be high because they often are provided in more expensive hospital settings. In this case, the state would incur an additional $4 million net cost (both the state share and the federal share)
| Figure 16 | |||
| Cost of Maintaining Full-Scope Medi-Cal for
New Immigrants Depends on Federal Funding Policy 1997-98 | |||
| (Dollars in Millions) | |||
| Total | Federal | State | |
| Full scope
Assuming federal funding based on cost neutralitya |
$50.5 | $23.8 | $26.7 |
| Budget proposal
Emergency services onlyb |
46.5 | 23.8 | 22.7 |
| Additional state cost | $4.0 | ||
| Full scope
Assuming federal funds limited to emergency servicesc |
$50.5 | $12.9 | $37.6 |
| Budget proposal
Emergency services onlyb |
46.5 | 23.8 | 22.7 |
| Additional state cost | $14.9 | ||
| a Federal funding equals the equivalent federal match for providing emergency-only services. | |||
| b Legislative Analyst's estimate based on budget proposal. | |||
| c Federal match provided only for the actual cost of emergency services with no credit for savings due to the reduced cost of providing care in a full-scope setting or savings due to preventive and other care that reduces the need for emergency services. Assumes that the cost of qualifying emergency services equals half of the overall cost of full-scope services. | |||
of providing full-scope services. We estimate that, as more immigrants arrive in future years, costs would increase by roughly $1.8 million annually.
The potential high-end state cost of $15 million assumes that the federal government limits its funding to the actual federal share of the cost of individual emergency services. (To estimate those costs, we assume that the emergency services would account for half of the total cost of full-scope benefits.) The actual costs of emergency services are less than the "equivalent" costs (emergency-only scenario) for various reasons. For example, persons with full-scope coverage are more likely to have a regular doctor and to receive their care in their doctor's office or clinic, whereas persons restricted to emergency services tend to use more costly hospital emergency rooms more often. In this case, the state would have to pay all costs for all nonemergency services--including preventive care and maintenance care that reduce the need for emergency services. We estimate that in subsequent years, state costs would grow by roughly $6.7 million annually.
At the time that this analysis was prepared, the federal Health Care Financing Administration had not yet determined its funding policy in cases where states choose to continue providing full-scope benefits to new legal immigrants.
Congressional intent in limiting federal Medicaid benefits to emergency services for most new legal immigrants appears to have been twofold. One objective was to hold immigrants and their sponsors responsible for meeting their commitment that the immigrant will not become a public charge. A second, related, objective was to generate savings to help finance the overall welfare reform legislation. In California, neither of these objectives is likely to be achieved.
As discussed above, restricting Medi-Cal benefits to new immigrants will reduce costs by a relatively small amount--about 8 percent--saving the state and federal governments a total of $4 million during 1997-98. Moreover, restricting services is unlikely to shift any significant financial responsibility for immigrants' healthcare from the taxpayers to sponsors. This is because most sponsors are unlikely to pay for the health care of a low-income sponsored immigrant (either out-of-pocket or by purchasing health insurance) when emergency Medi-Cal will cover basic health needs at no cost.
The likely result of restricting services, therefore, will be limited and less effective health care for many low-income new immigrants since they will not receive preventive services or regular dental or vision care. And, there will be only a modest savings to the state and federal governments. Maintaining full-scope benefits for new immigrants, however, could be relatively costly to the state (ranging from $4 million to about $15 million in 1997-98, as noted above) because the state would have to backfill federal funding for a potentially significant share of the cost.
Deeming As An Alternative to Restricting Benefits. Sponsor deeming means including a sponsor's income and resources in the calculations that determine eligibility of a sponsored immigrant for means-tested programs. The SSI/SSP and the AFDC welfare grant programs both have had sponsor deeming requirements. Deeming in these programs imposes a limited financial requirement on sponsors. Applying the same type of deeming requirement to Medi-Cal costs, however, would have a much greater potential financial effect on sponsors. Deeming would require sponsors with moderate incomes to impoverish themselves (by meeting "spend-down" requirements) before Medi-Cal would contribute to major medical costs for a sponsored immigrant. Moreover, health insurance may not be available--or available only at a prohibitive cost--for many new immigrants.
The federal welfare reform legislation requires deeming, but only for full-scope Medicaid, which would become available to sponsored noncitizen immigrants after they have been in the country for five years. (Emergency Medicaid services are exempt from deeming.) We expect this deeming requirement to have little effect since many immigrants probably will become citizens as soon as they meet the five-year residence requirement. Furthermore, noncitizen sponsored immigrants probably would choose to continue receiving restricted emergency Medicaid benefits in order to avoid the deeming requirement.
"Premium Deeming" Could Impose A Reasonable Requirement on Sponsors. We believe that a modified form of sponsor "deeming" for Medicaid could achieve a significant reduction in state and federal costs, place a reasonable level of financial responsibility on sponsors, and make full-scope benefits and preventive health care available to low-income new immigrants. Our deeming approach would require sponsors to pay a monthly premium that would cover a portion of the cost of providing Medi-Cal services to new sponsored immigrants. Premiums would be set on a sliding scale according to the sponsor's family income. Implementation of such a deeming program, however, requires enactment of legislation by Congress as well as by the Legislature.
An effective deeming requirement must be both reasonable and enforceable. In our view, a deeming requirement with the following features would meet this two-pronged test:
The deeming requirement outlined above imposes a reasonable financial requirement on sponsors. Federal law now requires sponsors to have incomes of at least 125 percent of the poverty level (currently $19,500 for a family of four), and many sponsors have significantly higher incomes. Sponsor families with middle-class incomes could pay a significant share of the full Medi-Cal cost (about $115 per month per person). Unlike income deeming for eligibility determination, premium deeming would still enable low-income immigrants to obtain Medi-Cal coverage, receive full-scope benefits, and also limit sponsor's financial risk for health care costs to the monthly premium amount.
Assuming that the sliding scale of sponsor premiums was set to recover half of the full cost of Medi-Cal benefits to new immigrants, the General Fund savings in 1997-98 would be about $12 million (on a full-year basis), with equivalent savings to the federal government. These General Fund savings would grow by about $5 million annually.
The premium deeming program that we have described could facilitate the retention of full-scope Medi-Cal benefits for new immigrants and generate significant state savings. Accordingly, we recommend that the Legislature and the administration, working with the state's Congressional delegation, seek federal legislation to authorize California to implement a Medi-Cal premium deeming program for new sponsored legal immigrants.
As discussed above, the federal welfare reform law makes legal immigrants ineligible for SSI/SSP benefits. The federal Social Security Administration (SSA), which administers the SSI/SSP, will notify SSI/SSP recipients who may be affected by the cutoff over the next few months. The SSA expects to complete the redetermination process by August 1997, when benefits will end for all immigrants who are not in an exempt group or have not attained citizenship. Immigrants who lose their SSI/SSP grants also will lose their automatic linkage to Medi-Cal. However, the budget anticipates that essentially all of these individuals will be able to reestablish their Medi-Cal eligibility as a medically needy or medically indigent person. The budget includes $34 million ($17 million General Fund) for the cost to county welfare departments of conducting these eligibility determinations.
Eligibility Determination Should be Less Costly. The budget assumes that reestablishing the Medi-Cal eligibility of these existing immigrants will cost the same as other Medi-Cal eligibility determinations. However, we believe that they should be significantly less costly. These immigrants already have been determined by SSA to be aged, blind, or disabled. Most have incomes that are very low and often fixed and which SSA has previously documented over time. Furthermore, the federal administration has issued a regulation giving states up to 120 days to redetermine eligibility for these immigrants, during which time immigrants will retain their Medi-Cal benefits. Given these circumstances, a streamlined eligibility process would be prudent and should be feasible.
Streamlined Process. Under a streamlined process, SSA would transfer the relevant records for these immigrants directly to DHS or the county welfare offices. Using these records, county welfare departments would be able to continue eligibility until the next regular redetermination period. There would be some initial costs imposed on DHS to accomplish the data transfer, but in most cases there should not be any significant additional redetermination cost. A streamlined process also would minimize burdens on these aged, blind, and disabled individuals and help ensure their continuity of coverage and care. We believe that savings of about half the average intake cost should be achievable by using a streamlined intake process. Thus, intake costs could be reduced by $4.5 million ($2.25 million General Fund)--from $9.1 million to $4.6 million.
Recommendation. In summary, we recommend a reduction of $4.5 million ($2.3 million General Fund) to recognize savings that we believe are achievable by streamlining the eligibility Medi-Cal process for immigrants who will lose their SSI/SSP benefits. We will revise our recommendation, if necessary, prior to budget hearings, based on any additional information provided by the department for streamlining the intake process.
"De-Linking" Has Little Practical Effect on Eligibility. While this "de-linking" represents a basic change in policy, its practical effect is likely to be very small in the near future. This is because the welfare reform legislation continues the AFDC eligibility rules (as they existed in each state on July 16, 1996) for the purpose of determining Medicaid eligibility. That is, families meeting the AFDC requirements that were in effect on July 16, 1996 will qualify for Medicaid benefits regardless of whether they were receiving AFDC benefits on that date or whether they were eligible for AFDC on that date. There are a few exceptions-- states may choose to deny Medicaid benefits to parents who refuse to comply with any TANF work requirements, and the immigrant restrictions discussed above also apply.
In states that choose to limit their TANF programs to exclude some families who would have received AFDC grants, those excluded families still will be eligible for Medicaid coverage. On the other hand, families in states that expand TANF eligibility beyond that of AFDC will have to qualify in a medically needy or indigent category in order to receive Medicaid benefits.
States Given Flexibility Over Income and Asset Limits for Medicaid Eligibility. The welfare reform law allows states considerable flexibility to vary from their July 16, 1996 AFDC eligibility rules for the purpose of determining Medicaid eligibility. States may lower their income standards as far as their May 1, 1988 level, or increase their income and resource standards for inflation (measured by the U.S. Consumer Price Index) that has occurred since July 16, 1996. More significantly, states also may adopt more liberal methods of computing income and resources. This means that states can adopt income or asset "disregards" that effectively increase the amount of income or assets that qualifying families may have and still be eligible for Medicaid coverage.
Prior to the enactment of welfare reform, families qualifying for AFDC had to have low income and meet a "deprivation" test. Generally, this meant that for two-parent families the primary earner must be working less than 100 hours per month and must have a "workforce attachment"--meaning a recent work history. Specifically, the workforce attachment rule generally requires that a parent has worked in at least six quarters out of the last 13 quarters.
The welfare reform legislation removes the workforce attachment requirement for the purpose of Medicaid eligibility. Therefore, two-parent families with parents who have been unemployed for long periods, or who have no work history, would now qualify for Medi-Cal benefits. Young children (and pregnant women) in low-income two-parent families currently are eligible for Medi-Cal coverage either as a medically indigent person or in one of the poverty-level eligibility categories. Consequently, the practical effect of the federal law change will be to extend Medi-Cal coverage to more parents and some older children in certain unemployed two-parent families.
The budget estimate of the AFDC/TANF-linked Medi-Cal caseload in 1997-98 does not include an augmentation for the expansion of eligibility for unemployed families that is mandated by the federal welfare reform law. We do not have an estimate of the costs of this provision. The department should be prepared to provide an estimate during budget hearings.
The welfare reform legislation provides a mechanism whereby up to $500 million may be allocated to the states for the costs of revising Medicaid eligibility procedures in order to determine eligibility under the former AFDC rules. This funding is to be allocated to the states as a temporary increase in the federal matching rate during the first three years of their TANF programs. At the time that this analysis was prepared, the federal administration had not issued guidelines or regulations on the allocation of these funds, but we anticipate such an announcement soon. Accordingly, we recommend that the department report during the budget hearings on the availability of additional federal funds and the potential for any state savings.
The budget continues the past practice of allocating county costs for determining Medi-Cal eligibility for AFDC/TANF applicants to the AFDC/TANF program. Since the AFDC and Medi-Cal programs were categorically linked and both received federal matching funds at the same rate, this practice simplified cost accounting without affecting the amount of federal funds the state received. Under the block grant approach in the new welfare reform law, however, the state receives a fixed amount of federal funds for the TANF program, while the federal government continues to pay for Medi-Cal administrative costs on a 50-50 basis. Consequently, reallocating Medi-Cal eligibility determination costs from AFDC/TANF back to the Medi-Cal Program could result in significant additional federal matching funds and state savings.
Currently, the federal government is considering cost allocation guidelines to address this issue. Given the potential for significant state savings, we recommend that DHS and the DSS report on this issue during budget hearings. (Please see our analysis of the AFDC/TANF program in the DSS for a more detailed discussion of this issue).
The budget proposes a total of $133.9 million ($65.6 million General Fund) for the SB 1732 Construction/Renovation Reimbursement Program in 1997-98--an increase of $103.3 million (339 percent) over estimated spending of $30.5 million in the current year. Under the SB 1732 Program, the Medi-Cal Program makes payments to qualifying DSH hospitals to cover a portion of their debt-service costs for constructing or renovating inpatient facilities. Payments commence after project completion and certification for occupancy by the Office of Statewide Health Planning and Development (OSHPD). The proposed tripling of spending primarily reflects the budget's assumption that a number of major hospital construction projects will be completed in 1997-98.
Our review of the current status of several major projects indicates that they will not be completed in time to require SB 1732 funding in 1997-98. For example, projects at the Santa Clara Valley Medical Center and at the Valley Children's Hospital in Fresno (with budgeted SB 1732 payments totaling $42.8 million in 1997-98) are not scheduled for completion until June 1998. Large, complex projects, such as hospitals, generally have some construction delays. Furthermore, final inspections often identify some problems that must be resolved prior to OSHPD certification. Consequently, the initial payments for these projects probably will be pushed into 1998-99. Hospital financial staff also indicate that payments for a number of completed projects will be less than the budgeted amounts. Based on our review, we estimate that the amount needed for payments in 1997-98 probably will be $84 million ($41 million General Fund) less than the amount budgeted. Accordingly we recommend a reduction of that amount.
Federal Savings Available for SB 1255 Program. We note that the savings in federal matching funds from our recommended reduction ($43 million) will remain available to help support county hospitals and other DSH hospitals in the state. This is because federal savings in the SB 1732 program can be used by the CMAC to make allocations under the SB 1255 program, which provides a federal match to voluntary hospital contributions. The federal match for the SB 1255 program is limited by the Medi-Cal savings generated by CMAC's hospital contracting program, and costs for the SB 1732 program are counted against those savings. Therefore, a spending reduction in one program allows greater spending in the other.
Freestanding Nursing Facilities Less Expensive Than Hospital-Based "distinct part" (DP) Facilities. Nursing care may be provided either in a DP nursing facility, which is part of an acute-care hospital, or in a freestanding nursing facility. The daily Medi-Cal rate for a DP bed averages about $187, whereas the daily rate in a freestanding facility averages less than half as much--about $81. The higher DP rate reflects the higher cost of a hospital environment. During the time that patients continue to occupy an acute-care bed pending transfer to either type of nursing facility, hospitals receive the Medi-Cal "administrative day" rate of about $215.
To encourage the transfer of Medi-Cal patients to freestanding nursing facilities, existing law requires hospitals to seek placements by contacting nursing homes located within a 30-minute drive of a patient's home (or the home of the most frequently visiting immediate family member). Patients may be transferred to a hospital's DP nursing facility only if appropriate freestanding facilities are unable or unwilling to take the patient. However, hospitals currently are not required to contact nursing homes on weekends or holidays and may automatically receive the administrative day rate for those days.
Growth of DP Bed Capacity Increases Cost of Nursing Care. The number of DP beds has more than doubled since 1986, while the number of beds in freestanding nursing facilities has grown very little (although beds in freestanding facilities are about ten times more numerous than DP beds). The higher payment rate for DP nursing beds in combination with the existing oversupply of acute-care hospital beds in California almost certainly explains some of this growth. From a hospital's perspective, converting some beds to DP nursing facilities can serve two purposes. It generates income from otherwise vacant beds (although even the DP rates are much lower than acute-care rates), and it provides continuity and convenience of care for patients who are transitioning from acute care to nursing care, particularly for patients who need only a brief period of nursing care. Because of their higher rates, however, the growth of DP beds increases the cost to Medi-Cal of providing nursing care.
Budget Proposals. The budget includes the following two proposals for legislation to encourage greater use of freestanding nursing facilities and limit the use of DP facilities:
Savings Are Likely to Be Much Less Than Budgeted. The weekend rate proposal may not be feasible without Congressional action to repeal the "Boren Amendment" provision of federal Medicaid law. This provision requires states to pay hospitals and nursing facilities rates that are "reasonably sufficient to cover the costs of an efficiently and economically operated facility." Current rates for hospital administrative days and for DP facility days are based on the department's audits of actual hospital costs. Thus, reducing the rates for weekend days could appear to be arbitrary and therefore in conflict with the Boren Amendment. Without the proposed rate reductions, eliminating the weekend and holiday exception for contacting nursing facilities probably will be less effective than assumed in the budget.
Savings from the moratorium on DP facility expansions also appear overstated because the estimate assumes that all of the patient days for the beds subject to the moratorium will be shifted to freestanding nursing facilities. However, existing DP facilities have unused capacity, so that some portion of the patient days from the moratorium beds will be shifted to other DP beds rather than to freestanding facilities.
Regional Bed Clearinghouses Are a Better Alternative. We agree that reducing unnecessary use of expensive DP beds is important but, for the reasons explained above, the budget proposals are not likely to be very successful at accomplishing that goal. Instead, we suggest enactment of legislation to establish a more cooperative and structured working arrangement between hospitals, nursing facilities, and the state through the use of regional nursing bed clearinghouses. Under this approach, DHS would contract for operation of the clearinghouses in urbanized areas of the state, financed either through Medi-Cal savings from reducing nursing facility administrative costs (as explained below) or by charging user fees. The clearinghouses would monitor the current availability of nursing beds in both freestanding and DP facilities in their region on a daily basis. Hospitals would be required to contact their regional clearinghouse for information about the availability of nursing beds (with no weekend or holiday exception). The Medi-Cal Program would authorize additional hospital administrative days or placement in a DP facility only if the regional clearinghouse could not identify an appropriate available bed in a freestanding facility.
Regional clearinghouses would address several problems inherent in the current process. They would eliminate the need for hospitals to contact multiple nursing facilities and maintain records of these contacts. The clearinghouses also would prevent hospitals from selectively contacting those nursing facilities that are unlikely to have space or be able to accommodate a patient's needs. Furthermore, the clearinghouses would act as a neutral buffer between freestanding nursing facilities and hospitals. Under the current process, nursing facilities may be reluctant to take patients that hospitals would prefer to keep in their own facilities. This is because, while freestanding nursing facilities compete for patients with hospital DP facilities, the freestanding facilities also depend on those hospitals (and their associated physicians) to supply most of their patients. We also note that regional clearinghouses could be expanded to provide centralized information on long-term care resources for consumers.
For these reasons, we recommend enactment of legislation to establish regional nursing bed clearinghouses and require their use in the Medi-Cal Program as an alternative to the budget proposals for lower weekend rates and a moratorium on DP facility expansions.
At the time that this analysis was prepared the department had not submitted three reports required by law or previously requested by the Legislature. These reports would provide information which would permit the Legislature to better evaluate the fiscal implications of the department's programs.
Public Health |
The Governor's budget proposes $1.7 billion (all funds) for public health local assistance. This represents an increase of $95 million, or 6 percent, over estimated current-year expenditures. The budget proposes $314 million from the General Fund, which is 3.8 percent below estimated current-year expenditures.
The CLPP Program identifies lead poisoned children and provides case management to ensure that these children receive the services that they need.
Until 1996-97, the CLPP Program was partially funded by fees assessed on manufacturers of lead products. However, in the case of Sinclair Paints v. The State Board of Equalization, the California courts of appeal ruled that the assessment on lead product manufacturers constituted a tax rather than a fee; and therefore, the assessment requires legislation authorizing such a tax. The state has appealed the case and has continued to collect fees which are held in reserve in the CLPP Fund.
As a result of the court case, the 1996-97 Budget Act appropriated $9.5 million from the General Fund to support the program in the current year. The Governor's budget proposes to continue the $9.5 million from the General Fund ($6.7 million in local assistance and $2.8 million in state operations) in 1997-98, and does not propose to spend any of the CLPP Fund revenues. However, the administration is also proposing budget trailer bill legislation which would permit the use of the fee assessment revenues in the CLPP Fund by deeming the assessment a special tax rather than a fee. In addition, the budget estimates that the assessment will generate $12 million in new revenues in 1997-98. Given this, we believe that it would be consistent with the proposed trailer bill legislation to appropriate these revenues in the budget year for the CLPP Program, rather than use General Fund monies. Accordingly, we recommend amending the budget bill to reflect this action, for a General Fund savings of $9.5 million.
The viral load test is a relatively new method for detecting the development of HIV in infected patients. Research shows that viral load testing predicts the risk of HIV disease progression better than another method that is used--the CD 4 test.
The Governor's budget requests $3.8 million from the General Fund to establish the new viral load test program within the Office of AIDS, and provide the test to about 10,000 clients in the AIDS Drug Assistance Program (ADAP) three times a year.
Proposal Shifts Costs From Counties to State. Under the proposal, the state would pay for the cost of the new test and would make the test available to localities at no cost. The viral load test, however, is currently funded by cities and counties using federal Ryan White Care Act Title I funds (and in some cases Title II funds). Thus, the budget proposal generally represents a cost shift from local governments to the state.
We believe that it would be reasonable to expect counties to continue to pay for the cost of viral load testing. The total cost of the proposal represents about 3 percent of the counties' estimated 1997-98 federal Title I funds. These funds are used for a variety of activities such as dental care, mental health counseling, and transportation.
Proposal Overestimates Cost. The estimated total cost of this proposal is based on a projected cost of $120 per viral load test. However, based on our discussions with providers, we find that $95 per test more accurately reflects the cost that providers will pay. Using $95 per test as the basis, we estimate that the cost of providing the test to 10,000 ADAP patients will be approximately $3 million rather than the $3.8 million requested. Accordingly, we recommend deletion of $800,000 if the Legislature adopts the proposal to use state funds to pay for the test.
Recommendation. In summary, we recommend deleting the proposed appropriation for the new test. Adoption of our recommendation would result in a General Fund savings of $3.8 million. However, if the Legislature should decide to fund this program, we recommend reducing the amount by $800,000, because the budget overestimates the cost of the test.
Background. Tuberculosis (TB) is a contagious disease which is transmitted from one person to another by infectious airborne particles expelled when a person with TB coughs or talks. Research shows that homeless TB patients who begin a course of treatment are much less likely to complete treatment than other patients. Consequently, these individuals are at risk of developing a multi-drug resistant strain of TB, which requires complex and costly treatment and which can be passed on to others.
Budget Proposal. The budget proposes $2.9 million from the General Fund ($2,799,000 in local assistance, and $67,000 in state operations) to provide grants to localities to house homeless TB patients and to detain patients who refuse to take medication. One new position is requested to administer the grants and provide technical assistance to grantees. Under the proposal:
Currently, homeless TB patients are often treated in acute care hospital settings. By avoiding expensive hospitalization, this proposal is designed to produce savings for both the state and counties. The budget includes Medi-Cal savings of approximately $1.5 million from the General Fund in 1997-98 as a result of the proposed program. There is no estimate of county savings in the county-operated indigent health programs.
Findings and Recommendations. We make the following findings and recommendations related to the proposal:
Duration of Housing for Homeless Patients is Overestimated. The budget estimate for housing homeless TB patients assumes that these patients will need housing for a period of six months. This is based on the average time for treatment for TB. We note, however, that not all homeless patients will require a full six months of housing. Some may not become homeless until later in their therapy. Others may find housing during therapy. Based on our discussions with providers in a TB patient housing program currently operating in Los Angeles, we believe that four months is a more likely estimate of the actual duration of housing. This corresponds to the average time needed for housing in the Los Angeles program. Using a four-month housing period as the basis, we recommend a General Fund reduction of $468,000 in the amount proposed for this component of the program.
Detention Costs for Patients Who Refuse to Take Medication is Overbudgeted. The department indicates that, due to the newness of this program, they have no data on which to base an estimate of the cost of detaining individuals who refuse to take their medication. In the absence of such information, the budget for this component of the program is based on an average daily rate of $82 per patient--the rate for a "level B" skilled nursing facility. Our analysis, however, indicates that individuals who are placed in "level B" skilled nursing facilities generally require a higher level of health care services than most TB patients. Therefore, we believe that a "level A" skilled nursing facility, which provides less intensive care than the "level B" facilities, would be a more appropriate yardstick for this proposal. The "level A" facilities provide intermittent nursing care for individuals who generally are capable of taking care of themselves. The average daily rate for the "level A" facilities is $62 per patient. Using the $62 rate as the basis, we recommend a General Fund reduction of $230,000 in the amount budgeted for detention of TB patients who refuse to take their medication.
Summary. Adoption of our recommendations would result in a total General Fund savings of $698,000 in 1997-98.
The Local Health Capital Expenditure Account (of the County Health Services Fund) was established by Chapter 1351 of the Statutes of 1980 (AB 3245, Berman) to provide grants or loans to counties for capital improvements of county health facilities or to purchase equipment. Initial revenues were derived by a transfer of monies from the General Fund.
This program has been inactive for a number of years. No funds have been granted to the counties from the account since 1988-89. We also note that the budget acts of 1991-92 and 1993-94 transferred the unencumbered balances in the account to the General Fund.
The account currently has a balance of $1.2 million, which is the result of loan repayments that have been made since 1993-94 from the single outstanding loan in the program. The budget proposes expenditures of $17,000 from the account to pay for the minor administrative expenses of the department, related to monitoring previously funded capital projects. The department indicates that they do not anticipate providing any additional grants or loans in the future.
Given that the program is essentially dormant and that the account derived its revenues initially from the General Fund, we believe that it would be appropriate to take an action similar to the one taken by the Legislature in 1993-94--transfer the account balances to the General Fund. This would add $1.2 million to General Fund revenues, freeing up these monies for expenditure according to the Legislature's priorities.
Accordingly, we recommend that the Legislature adopt budget bill language to transfer to the General Fund all Local Health Capital Expenditure Account balances in excess of $17,000.
Our recommendation could be implemented by adoption of the following language in a new budget bill item (4260-011-0900):
For transfer by the State Controller from the Local Health Capital Expenditures Account to the General Fund, the amount of the unencumbered balance of the Local Health Capital Expenditures Account in excess of $17,000 as of July 1, 1997, and any unencumbered balance in excess of $17,000 as of June 30, 1998.
The AFLP provides case management and counseling services for pregnant and parenting teens age 17 and under. The program has been shown to be effective in reducing the incidence of low birth weight babies and reducing the school drop-out rate among pregnant and parenting adolescents.
The 1996-97 Budget Act included a $10 million augmentation for (1) the expansion of the AFLP ($7 million) and (2) the development of a new program component geared toward the siblings of teenage parents ($3 million). This augmentation brought the total funding for the program to $19.3 million. This expansion has resulted in 13 new AFLP providers, bringing the total to 48 providers.
The Governor's budget proposes to shift $147,000 from General Fund local assistance to state operations to fund two new positions to provide technical assistance to new AFLP providers, as well as to design and develop program standards for the AFLP siblings program. We agree that it would be reasonable to provide technical assistance to providers. We note, however, that the budget includes $250,000 per year in the current and budget years to contract for training and technical assistance services for the 48 AFLP providers.
We also note that most AFLP providers have been administering the program for more than five years. As a result, these providers generally require less technical assistance. Therefore, the department should be able to redirect staff to handle any new workload demand that is not covered under the department's contract for training and technical assistance.
Based on these findings, we believe that it would be more productive to retain the $147,000 in local assistance where the funds would provide direct services, rather than in state operations for additional technical assistance. Consequently, we recommend rejection of the budget proposal.
Background. Proposition 99, the Tobacco Tax and Health Protection Act of 1988, established a surtax on cigarettes and tobacco products. The proposition provides that the revenues from the surtax are to be distributed to six accounts within the Cigarette and Tobacco Products Surtax Fund (C&T Fund) according to specified percentages, and further provides that expenditures from each account must be for specific kinds of activities. The administration proposes to allocate Proposition 99 funds to the accounts in accordance with the provisions of the proposition, as shown in Figure 17.
Chapter 195, Statutes of 1994 (AB 816, Isenberg), appropriated some of the funds from the Health Education Account (HEA) and the Research Account (RA), to pay for the delivery of health services. In December 1994, the Sacramento Superior Court ruled, in American Lung Association v. Wilson, that the use of tobacco tax monies from the HEA and RA for these health services, violated the terms of the proposition.
In 1995-96, the Legislature enacted Chapter 194/95 (SB 493, Maddy) to permit the allocation of funds for health services programs as reflected in Chapter 195. This was accomplished by allocating funds to the various Proposition 99 accounts according to percentages that were different than specified in the proposition, pursuant to a provision in Proposition 99 that permits the Legislature--with a four-fifths vote--to make changes to the proposition under certain conditions. However, the superior court enjoined the implementation of Chapter 194.
The state appealed both superior court decisions; and the California courts of appeal recently ruled on these appeals.
Courts of Appeal Ruling. In December 1996, the California courts of appeal ruled on the two cases related to Proposition 99--one challenging AB 816, the other SB 493.
| Figure 17 | |||
| Proposition 99 Programs
Proposed Distribution of Revenue Governor's Budget | |||
| (Dollars in Millions) | |||
| Account | 1997-98
Estimated Revenuesa |
Percent
of Total Revenues |
Use of Revenue by Account |
| Health Education | $90.3 | 20% | Programs to prevent and reduce
tobacco use. |
| Hospital Services | 158.1 | 35 | Payments to hospitals for patients who cannot afford treatment. |
| Physician Services | 45.2 | 10 | Payments to physicians for patients who cannot afford treatment. |
| Research | 22.5 | 5 | Tobacco-related disease research. |
| Public Resources | 22.5 | 5 | Equal amounts for (1) wildlife habitat programs and (2) recreation resources. |
| Unallocated | 112.9 | 25 | Any of the uses identified above. |
| Totals | $451.5 | 100% | |
| a Excludes $1.3 million allocated to the State Board of Equalization. | |||
In the case of AB 816, the courts of appeal upheld the Sacramento Superior Court ruling that the use of tobacco tax monies from the HEA and the RA for health care services violated the terms of the proposition. Basically, the court's rationale for this ruling is that the funds in the HEA and the RA were intended to be used for specific purposes--health education programs and tobacco-related research--which do not include health care services as AB 816 provided.
In the case of SB 493, the courts of appeal reversed the lower court's ruling. The appeals court ruled that it is permissible for the Legislature (through a four-fifths vote) to change the percentages of funding allocated to the various accounts. It is not known, at this time, whether these rulings will be appealed to the state Supreme Court.
Budget Proposal. The Governor's budget proposes expenditures of $510 million from the C&T Fund in 1997-98, which represents a reduction of 4.8 percent from the estimated current-year expenditure level. This decrease is due to a projected reduction in C&T Fund revenues. As in the current year, the administration proposes to appropriate Proposition 99 funds through the budget act.
Although the Governor's budget proposes to allocate Proposition 99 funds to the six accounts in accordance with the provisions of the proposition, the budget does propose changes in the distribution of these funds for particular programs. The proposed changes are:
Figure 18 summarizes the proposed changes in expenditures.
Proposed Reauthorization Legislation. The administration's proposal includes the following features:
| Figure 18 | ||||
| Proposition 99 Expenditures
Governor's Budget 1997-98 | ||||
| (Dollars in Thousands) | ||||
| 1996-97 | Governor's
Proposal 1997-98 |
Change | ||
| Amount | Percent | |||
| Department of Health Services | ||||
| Health Services | $47,483 | $70,977 | $23,494 | 49.5% |
| County Health Services | 184,302 | 185,218 | 916 | 0.5 |
| Health Education | 87,752 | 71,637 | -16,115 | -18.4 |
| Department of Education | 43,044 | 35,407 | -7,637 | -17.7 |
| University of California | 60,422 | 24,699 | -35,723 | -59.1 |
| Resources Agency Departments | 21,027 | 20,431 | -596 | -2.8 |
| Managed Risk Medical
Insurance Board |
69,500 | 84,500 | 15,000 | 21.6 |
| Office of Statewide Health
Planning and Development |
5,000 | -- | -5,000 | -100.0 |
| Board of Equalization | 949 | 1,264 | 315 | 33.2 |
| Habitat Conservation Fund | 15,398 | 15,024 | -374 | -2.4 |
| Pro Rata charges | 808 | 921 | 113 | 14.0 |
| Totals | $535,685 | $510,078 | -$25,607 | -4.8% |
The Child Health and Disability Prevention (CHDP) Program provides medical examinations to children. If a medical condition requires treatment identified during the screen, the patient is advised of this, and the county is obligated to provide such treatment if the patient seeks it. These medical conditions cover a wide range of problems, such as dental cavities, ear infections, and more serious conditions such as cancer. As a condition of receiving Proposition 99 funding, counties are required to provide medically necessary treatment, or follow-up treatment, for uninsured children who have a condition detected as part of a CHDP health examination.
Background. Between 1990-91 and 1994-95, the number of children referred for CHDP follow-up treatment increased 46 percent--from 114,190 to 167,000. Data are not available on the number of children treated. County expenditures for follow-up treatment have grown from $8 million in 1991-92 to over $16 million in 1993-94 (the latest year for which data are available). However, despite growth in expenditures, our discussions with state and local program administrators suggest that many children still do not receive treatment that is prescribed as a result of the health screen--generally because their parents do not make the necessary appointments--or receive treatment, but not on a timely basis.
Almost all counties use Proposition 99 funds to pay for CHDP follow-up treatment. Some also use local general funds.
Data Not Collected. The department is responsible for monitoring county compliance with the statutory treatment requirement and has the authority to recover funds from counties that do not comply. However, the department does not collect sufficient data to determine the level of compliance with this requirement and, accordingly, has not enforced it.
What Data Are Available? Under provisions of current law, counties that receive Proposition 99 funds are required to submit cost and utilization data for inpatient/outpatient care, physician services, dental care, and emergency services. These data are insufficient for purposes of monitoring the CHDP treatment requirement for three reasons. First, the department collects information on the number of children referred for treatment, but cannot relate this to the data collected on treatment that is provided. This is because the treatment data are reported as visits and discharges rather than on a per-child basis. Thus, the department cannot distinguish between one child that has three visits to treat a problem related to one referral, and three children who each make one visit, for a total of three visits. Second, the data are specific to Proposition 99 funding. Therefore, treatment services which are paid for with other funds, such as local general funds, are not reported. Third, the data are incomplete because the counties do not report on CHDP treatment provided in all settings. For example, if a child is treated in a county hospital which does not submit a reimbursement claim for CHDP treatment, then neither the treatment nor the expense is linked to CHDP.
What Data Are Needed? In order to determine the extent to which counties are complying with the requirement to provide treatment, counties should be required to submit data on the number of children screened, referred, and treated. They should also submit an explanation for why all children were not treated, if that is the case.
We note that some children may receive treatment in non-county facilities. Thus, the department should direct counties to develop the necessary reporting arrangements with these private providers.
How Should Compliance Be Defined? In enforcing the treatment requirement, the department will need to determine whether the conditions of compliance are met. For example, should counties be expected to provide treatment within a particular time frame? This is an issue the department should consider in developing regulations to enforce the treatment requirement.
Similarly, the department should consider what should be expected of counties with respect to facilitating the provision of treatment. For example, should the counties be required to conduct outreach activities, or set up appointments for treatment after the examinations?
Potential Effects of Enforcing the CHDP Treatment Requirement. Under current law, the state may recover Proposition 99 funds from any county that fails to comply with the treatment requirement. Since this issue deals with enforcement of this provision, it is important to consider the potential effects of such enforcement.
One of the possible effects is that counties may decide to forgo Proposition 99 funds. Due to factors such as regional demographics, some counties may experience a relatively large number of children referred for follow-up treatment; and as a result, the county may find it difficult to meet the costs of treatment. The cost of treating all children could exceed the amount that a county receives in Proposition 99 revenues. This raises the possibility that counties could decide to forgo their Proposition 99 funds rather than meet the requirement. The result, in other words, could be counter to the intent of the provision--to act as an incentive for counties to allocate funds for this purpose.
Thus, while we recommend that the department take steps to enforce the CHDP treatment requirement because it is a provision of current law, we also suggest that the Legislature consider the potential ramifications of doing so. Should the Legislature decide to continue the treatment requirement, we recommend adoption of the following budget bill language in Item 4260-001-0001:
The department shall develop and implement regulations and procedures designed to monitor and enforce compliance with the statutory requirement that counties, as a condition of receiving Proposition 99 funds, provide treatment prescribed pursuant to health examinations in the Child Health and Disability Prevention Program."