Health and Social Services
Department of Aging (4170) |
The budget proposes expenditures of $156.3 million ($41.5 million General Fund) for the CDA in 1998-99. This represents a 28 percent increase in General Fund expenditures over the current year, due to the proposed expansion of several programs.
Background. The CDA's programs are carried out at the local level by the Area Agencies on Aging (AAA). There is one AAA for each Planning and Service Area (PSA). The budget proposes to expand the following programs administered by the CDA into PSAs where they do not currently exist:
Figure 8 shows the additional sites necessary to provide each PSA with at least one site for each program.
| Figure 8 | |||||||||
| California Department of Aging
Proposed Program Expansion | |||||||||
| Planning and
Service Area |
Programs Proposed to Be Expanded
a | ||||||||
| ADCRC | L | FG | SC | RR | RPOS | BB | MSSP | ADHC | |
| Del Norte, Humboldt | X | X | X | ||||||
| Lassen, Modoc,
Shasta,
Siskiyou, Trinity |
X | X | X | X | X | X | |||
| Butte, Colusa,
Glenn,
Plumas, Tehama |
X | X | X | X | X | ||||
| Nevada, Placer,
Sacramento, Sierra, Sutter, Yolo, Yuba |
X | X | X | ||||||
| Marin | X | X | X | X | X | ||||
| San Francisco | |||||||||
| Contra Costa | X | X | X | X | X | X | |||
| San Mateo | X | X | X | ||||||
| Alameda | X | X | |||||||
| Santa Clara | X | X | X | X | |||||
| Continued | |||||||||
| San Joaquin | X | X | X | ||||||
| Alpine, Amador,
Calaveras, Mariposa, Tuolumne |
X | X | X | X | X | X | |||
| San Benito, Santa Cruz | X | X | |||||||
| Fresno, Madera | X | X | X | X | |||||
| Kings, Tulare | X | X | X | X | X | X | X | X | |
| Inyo, Mono | X | X | X | X | X | X | X | X | X |
| San Luis Obispo,
Santa Barbara |
X | X | X | X | X | X | |||
| Ventura | X | X | X | X | X | X | X | X | |
| Los Angeles County | X | ||||||||
| San Bernardino | X | X | X | X | |||||
| Riverside | X | X | X | X | X | X | |||
| Orange | X | X | X | X | X | ||||
| San Diego | X | X | X | ||||||
| Imperial | X | X | X | X | X | X | X | ||
| Los Angeles City | X | X | |||||||
| Lake, Mendocino | X | X | |||||||
| Sonoma | X | X | X | X | X | ||||
| Napa, Solano | X | X | X | X | X | X | X | X | |
| El Dorado | X | X | X | X | X | X | X | X | |
| Stanislaus | X | X | X | X | X | X | |||
| Merced | X | X | X | X | X | X | X | X | |
| Monterey | X | X | X | ||||||
| Kern | X | X | X | X | X | X | |||
| Totals | 10 | 23 | 21 | 26 | 28 | 25 | 1 | 13 | 9 |
| aADCRC--Alzheimer's Day Care Resource Center; L--Linkages; FG--Foster Grandparent; SC--Senior Companion; RR--Respite Registry; RPOS--Respite Purchase of Services; BB--Brown Bag; MSSP--Multipurpose Senior Services Program; and ADHC--Adult Day Health Care. | |||||||||
The budget proposes expenditures of $12.2 million ($9.1 million General Fund) to expand these programs in 1998-99, including $3.3 million ($2.7 million General Fund) in one-time start-up costs. The budget assumes that the expansion would begin in February 1999. The full-year expansion costs in 1999-00 are estimated to be $20.5 million ($14.4 million General Fund).
Proposed MSSP Expansion. The largest component of the budget proposal is the expansion of the MSSP--$5.8 million in 1998-99, including $2.8 million General Fund. The MSSP provides case management services to frail elderly clients in order to prevent or delay institutionalization. Clients must be at least 65 years of age, Medi-Cal eligible, and certifiable as appropriate for nursing facility placement. Currently, there are 6,000 full-time equivalent "slots" in 19 PSAs, serving about 8,000 people statewide each year.
The department has estimated the need for MSSP services based on the size of the disabled elderly population in each PSA. Figure 9 shows for each PSA (1) the department's estimate of potential MSSP clients, (2) the current distribution of MSSP slots, and (3) the department's proposed distribution of new slots.
The figure indicates that the proposed expansion would not distribute new MSSP slots according to the estimated need for MSSP services. For example, the expansion would create a new 600-slot site in the Riverside PSA, but would leave the neighboring San Bernardino and Orange PSAs--which have a higher projected level of need--with only their existing 200 slots. The expansion would also create a new 400-slot site in the Kings-Tulare PSA, but would leave the neighboring Fresno-Madera PSA, which is projected to have twice the level of need, with half the number of slots. Clearly, the proposed MSSP expansion would not match the distribution of MSSP slots with the projected need for these services.
Proposed Expansion of Other Programs. The department does not have specific indicators of need for the other programs. Based on our discussions with the department, however, we believe that the size of the age 60-plus population is a reasonable proxy for the level of need for the services provided by these programs. However, the budget proposes to expand most of these programs by replicating the size of an "average existing site" in the PSAs that are currently without a site. This plan is unlikely to match the distribution of service capacity with the need for services for two reasons. First, the PSAs without existing program sites tend to have smaller age 60-plus populations, and therefore have a lower level of need for services than PSAs with existing sites. Second, although PSAs without existing sites vary in terms of the size of their age 60-plus populations, the proposal would establish sites of equal size in each new PSA.
Figure 10 (see page 28) illustrates these two problems by describing the proposed expansion of the Linkages program--the second largest component of the budget proposal ($3 million General Fund in 1998-99). The Linkages program provides case management services to about 2,000 functionally impaired adults and frail elderly each year who are at risk of institionalization, but who need not be Medi-Cal eligible. Figure 10 re-
| Figure 9 | ||||
| Proposed Expansion of MSSP
Potential Clients and Full-Time Service Slots | ||||
| Planning and Service Area | Potential
Clients |
Current
Slots |
Proposed
New Slots | |
| Del Norte, Humboldt | 138 | 130 | -- | |
| Lassen, Modoc, Shasta, Siskiyou, Trinity | 296 | -- | 200 | |
| Butte, Colusa, Glenn, Plumas, Tehama | 371 | 200 | -- | |
| Nevada, Placer, Sacramento,
Sierra, Sutter, Yolo, Yuba |
1,907 | 200 | -- | |
| Marina | 103 | 200 | 100 | |
| San Francisco | 2,548 | 400 | -- | |
| Contra Costa | 760 | -- | 300 | |
| San Mateo | 742 | 200 | -- | |
| Alameda | 1,927 | 410 | -- | |
| Santa Clara | 2,127 | 200 | -- | |
| San Joaquin | 760 | 200 | -- | |
| Alpine, Amador, Calaveras, Mariposa, Tuolumneb | 98 | -- | 200 | |
| San Benito, Santa Cruz | 234 | 250 | -- | |
| Fresno, Madera | 1,505 | 200 | -- | |
| Kings, Tulare | 822 | -- | 400 | |
| Inyo, Monob | 24 | -- | -- | |
| San Luis Obispo, Santa Barbara | 468 | 200 | -- | |
| Ventura | 599 | -- | 300 | |
| Los Angeles Countyc | 17,197 | 1,810 | -- | |
| San Bernardino | 1,617 | 200 | -- | |
| Riverside | 1,407 | -- | 600 | |
| Orange | 2,500 | 200 | -- | |
| San Diego | 3,133 | 500 | -- | |
| Imperial | 466 | -- | 200 | |
| Los Angeles Cityc | -- | -- | -- | |
| Lake, Mendocino | 180 | 300 | -- | |
| Sonomaa | 268 | -- | -- | |
| Napa, Solano | 426 | -- | 200 | |
| El Doradob | 73 | -- | -- | |
| Stanislaus | 607 | 200 | -- | |
| Merced | 332 | -- | 200 | |
| Monterey | 373 | -- | 200 | |
| Kern | 830 | -- | 400 | |
| aPSAs currently share a 200-slot MSSP site. The proposed expansion would serve 100 additional clients in the Marin PSA. | ||||
| bPSAs would share a 200-slot MSSP site. | ||||
| cFigures for the Los Angeles County PSA include data for the Los Angeles City PSA. | ||||
| Figure 10 | |||
| Proposed Expansion of Linkages Program
Current and Proposed Full-time Service Slots | |||
| Planning and Service Area | 60-Plus
Population |
Current
Slots |
Proposed
New Slots |
| Del Norte, Humboldt | 28,036 | 120 | -- |
| Lassen, Modoc, Shasta, Siskiyou, Trinity | 56,192 | -- | 151 |
| Butte, Colusa, Glenn, Plumas, Tehama | 73,601 | -- | 151 |
| Nevada, Placer, Sacramento,
Sierra, Sutter, Yolo, Yuba |
297,630 | -- | 151 |
| Marin | 43,909 | -- | 151 |
| San Francisco | 143,907 | 110 | -- |
| Contra Costa | 150,067 | -- | 151 |
| San Mateo | 115,361 | 109 | -- |
| Alameda | 199,086 | 266 | -- |
| Santa Clara | 222,315 | -- | 151 |
| San Joaquin | 84,789 | 123 | -- |
| Alpine, Amador, Calaveras, Mariposa, Tuolumne | 38,376 | -- | 151 |
| San Benito, Santa Cruz | 40,851 | -- | 151 |
| Fresno, Madera | 132,748 | -- | 151 |
| Kings, Tulare | 65,288 | -- | 151 |
| Inyo, Mono | 5,890 | -- | 151 |
| San Luis Obispo, Santa Barbara | 113,427 | -- | 151 |
| Ventura | 101,761 | -- | 151 |
| Los Angeles County | 747,310 | 481 | -- |
| San Bernardino | 205,743 | -- | 151 |
| Riverside | 241,246 | -- | 151 |
| Orange | 376,659 | -- | 151 |
| San Diego | 412,207 | 138 | -- |
| Imperial | 18,409 | -- | 151 |
| Los Angeles City | 498,206 | 318 | -- |
| Lake, Mendocino | 33,630 | 158 | -- |
| Sonoma | 72,997 | -- | 151 |
| Napa, Solano | 74,934 | -- | 151 |
| El Dorado | 26,850 | -- | 151 |
| Stanislaus | 63,963 | -- | 151 |
| Merced | 26,477 | -- | 151 |
| Monterey | 50,442 | 135 | -- |
| Kern | 92,194 | -- | 151 |
ports for each PSA (1) the size of the age 60-plus population, (2) the current distribution of Linkages slots, and (3) the proposed distribution of new slots.
The figure shows that replicating the average existing site in new PSAs would give the tiny Inyo-Mono PSA a larger service capacity (that is, more Linkages slots) than more populated PSAs with existing Linkages sites, such as San Diego, San Mateo, and San Francisco. In addition, the figure shows that Inyo-Mono would have the same service capacity as larger PSAs receiving new Linkages sites, such as Orange, Fresno-Madera, and Santa Clara. Consequently, the proposed expansion of the Linkages Program would not match the distribution of service capacity with the need for services.
Recommendation. Because the proposed expansion of CDA programs would not allocate new service capacity according to the need for services, we withhold recommendation on the budget proposal. Further, we recommend that the department develop, prior to the budget hearings, an allocation plan that would better align new service capacity with the need for services.
The Federal Medical Assistance Percentage (FMAP) determines the federal share of costs in the Medicaid Program (Medi-Cal in California) as well as certain other programs. The FMAP will increase from 51.23 percent to 51.55 percent beginning October 1, 1998.
The federal share of costs in the MSSP program is based on the FMAP. The budget, however, does not reflect the change in the federal share of costs. We estimate that the additional federal funds would result in General Fund savings of $125,000 in 1998-99. Accordingly, we recommend that the budget be amended to reflect these anticipated savings.
Department of AlcoholAnd Drug Programs (4200) |
The budget proposes $352 million from all funds for support of DADP programs in 1998-99, which is a decrease of 9.3 percent from estimated current-year expenditures. The budget proposes $82 million from the General Fund in 1998-99, which is a decrease of $6 million, or 7.4 percent, below estimated current-year expenditures. The decrease is primarily due to a one-time carryover of $25 million ($6 million General Fund) from 1996-97 to 1997-98.
The DADP administers the Drug Medi-Cal (D/MC) program, an optional benefit under the state Medi-Cal program. The Governor's budget proposes expenditures of $64.7 million ($31.7 million from the General Fund for this program in 1998-99). However, the proposal does not take into account the increased federal sharing ratio for Medi-Cal services, from 51.23 to 51.55 percent, effective October 1, 1998. The effect of this change is to increase the amount of federal funds and reduce the amount of General Fund. Accordingly, we recommend that the budget be adjusted to reflect the increase in federal funds. If this change is taken into account, General Fund expenditures would decrease by $317,000.
Department of Health ServicesState Operations (4260) |
The budget proposes $666 million from all funds ($201 million from the General Fund) and 5,033 personnel-years of staff for DHS state operations in 1998-99. Proposed General Fund spending represents an increase of 19 percent compared with estimated General Fund spending in the current year. Excluding a proposed new allocation of $25 million for ovarian and prostate cancer research, the budgeted growth in DHS state operations is 4.4 percent.
The budget requests a total of $1,725,000 ($863,000 from the General Fund) to add 19 new positions and make permanent three limited-term positions for the California Zero Fraud Tolerance Initiative. The proposal would add 12 new fraud investigators located at ports of entry along the Mexican Border and at major airports. These investigators work with the U.S. Immigration and Naturalization Service (INS) to identify aliens seeking to enter the state who are nonresidents and have fraudulently used Medi-Cal services in the past. Aliens who are so identified are referred to the INS for possible exclusion.
The budget also proposes to add seven new investigators to screen visa applicants for prior Medi-Cal use, verify residence of hospital patients, and consult in cases of document fraud. The budget also assumes that the new positions will result in $2.2 million of General Fund savings in 1998-99 (and indicates that the savings could potentially be greater) by preventing fraud.
Proposed Investigator Positions. The budget request seeks to make three current limited-term airport investigator positions permanent and add the following new positions:
High Travel Needs Not Justified. The budget request includes a total of $208,000 ($104,000 General Fund) for travel, budgeted at the department's "heavy" travel allotment of almost $11,000 annually for each of the new positions. The need for heavy travel, however, has not been justified. The border inspectors will be working regular shifts at permanent border crossings--primarily in the San Diego metropolitan area. The new staff to handle foreign inquiries should not require any travel. Reducing travel to $2,000 per position would provide adequate funding for attending training and meetings and results in a General Fund savings of $83,000.
Investigators. The department's budget request does not justify the need to hire the new border and hospital investigators at the senior classification. Budgeting these 13 positions at the entry level, Special Investigator I class, saves $50,000 (General Fund).
Peace Officers and Guns Unnecessary For Some Tasks. All of the requested new positions are armed peace officers. The budget provides guns, ammunition, and body armor for all of the new positions. While there may be some justification for using armed peace officers at the border crossings, where access is uncontrolled and criminal apprehensions are not uncommon, we question whether the other positions require armed peace officers. The need for armed inspectors to verify the residence of hospital patients has not been explained. Furthermore, we fail to understand what threat requires arming investigators who will be running computer checks on visa applicants who are overseas or who are consulting on document verification. Classifying these positions more appropriately as analysts saves $57,000 (General Fund), and an additional General Fund savings of $3,000 results from deleting ammunition, guns, and body armor requested for these seven positions.
The budget estimate includes General Fund cost increases of $1.4 million in 1997-98 and $4.8 million in 1998-99 to offset a loss of revenue from the recovery of Medi-Cal costs from estates, insurance companies, and other third parties. The department indicates that the revenue loss results from its inability to fill 39.3 authorized, but vacant, positions due to budget constraints. The department advises that the General Fund cost of filling the positions would be $1,090,000 in 1998-99. Since filling the positions would result in a net General Fund savings of $3.7 million, leaving the positions vacant, rather than filling them, appears to constrain the budget. Accordingly, we recommend an augmentation in the department's state operations budget to fund the vacant positions and a reduction in the Medi-Cal local assistance budget to recognize the resulting third-party recoveries for a net savings of $3.7 million.
The DHS budget requests 293 new authorized positions for 1998-99, raising the total number of authorized positions in the department to 5,832. The request for almost 300 new positions comes despite the fact that the department has 731 vacant positions in the current year. With the additional positions, the number of vacant positions will increase to 799 (13.7 percent of all authorized positions) in 1998-99, according to the budget, in order to meet the department's "salary savings" requirement.
All departments have some vacant positions due to normal personnel turnover and hiring delays, but generally these unavoidable vacancies are only about 5 percent of total positions (the statewide average is 4.9 percent). The high vacancy rate at DHS results from intentionally leaving positions vacant in order to live within the dollars provided in the budget. The discrepancy between positions and funding may result, in part, from the department's failure to adjust its staffing levels after unallocated funding cuts made in previous years. Instead of identifying low-priority functions and eliminating those positions, the department has absorbed funding cuts by increasing its salary savings allotment (savings from position vacancies). As a result, the department's staffing looks considerably more formidable on its organization chart than it is in reality.
Budgeting such a high vacancy rate undermines the Legislature's ability to effectively oversee the department's programs because it weakens the Legislature's oversight of the organization and staffing of the department. The programs or functions that are adversely affected by vacancies are determined by chance or by the preferences of department administrators, without giving the Legislature an effective means of reviewing these decisions. For this reason, we recommend that the department develop and present to the budget subcommittees a revised staffing plan that identifies and proposes to eliminate approximately 500 vacant positions to reduce its salary savings requirement to 5 percent and eliminate forced vacancies.
California MedicalAssistance Program (Medi-Cal) |
At the state level, the Department of Health Services (DHS) administers the Medi-Cal Program. Other state agencies, including the California Medical Assistance Commission (CMAC), the Department of Social Services (DSS), the Department of Mental Health, the Department of Developmental Services, and the Department of Alcohol and Drug Programs receive Medi-Cal funding from DHS for eligible services that they provide to Medi-Cal beneficiaries. At the local level, county welfare departments determine the eligibility of applicants for Medi-Cal and are reimbursed by DHS for the cost of those activities. The federal Health Care Financing Administration (HCFA) oversees the program to ensure compliance with federal law.
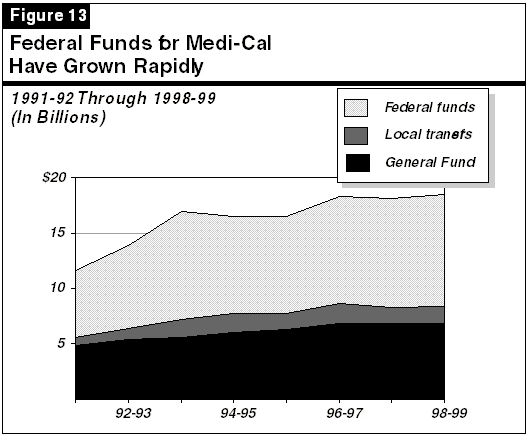
Proposed Spending. The budget for DHS proposes Medi-Cal expenditures totaling $18.7 billion from all funds for state operations and local assistance in 1998-99. The General Fund portion of this spending ($6.9 billion) increases by a relatively small amount ($41.6 million or 0.6 percent) compared with estimated General Fund spending in the current year. The spending total for the Medi-Cal budget includes an estimated $2.8 billion (federal funds and local matching funds) for payments to DSH hospitals, and about $1.4 billion of federal funds to match state and local funds budgeted elsewhere for programs operated by other departments, by counties, or by the University of California. Including these other state and local funds, total proposed Medicaid spending in California would be about $20.1 billion in 1998-99.
Generally, persons who have been determined eligible for Medi-Cal benefits (Medi-Cal "eligibles") receive a Medi-Cal card, which they may use to obtain services from providers who agree to accept Medi-Cal patients. Medi-Cal uses two basic types of arrangements for health care--fee-for-service and managed care.
Fee-for-Service. This is the traditional arrangement for health care in which providers are paid for each examination, procedure, or other service that they furnish. Beneficiaries may obtain services from any provider who has agreed to accept Medi-Cal payments. The Medi-Cal Program employs a variety of "utilization control" techniques (such as requiring prior authorization for some services) designed to avoid costs for medically unnecessary or duplicative services.
Managed Care. Prepaid health plans generally provide managed care. The plans receive monthly "capitation" payments from the Medi-Cal Program for each enrollee in return for providing all of the covered care needed by those enrollees. These plans are similar to health plans offered by many public and private employers. By the end of 1998-99, DHS expects to have just over half (2.5 million) of the projected 4.9 million Medi-Cal eligibles enrolled in managed care organizations. Beneficiaries in managed care choose a plan and then must use providers in that plan for most services. Since payments to the plan do not vary with the amount of service provided, there is much less need for utilization control by the state. Instead, plans must be monitored to ensure that they provide adequate care to enrollees.
Aged, Blind or Disabled Persons. About 1.3 million low-income persons who are (1) at least 65 years old or (2) disabled or blind persons of any age receive Medi-Cal coverage. Overall, the disabled make up more than half (61 percent) of this portion of the Medi-Cal caseload. Most of the aged, blind or disabled persons on Medi-Cal (85 percent) are recipients of SSI/SSP welfare benefits and receive Medi-Cal coverage automatically. The other aged, blind or disabled eligibles are in the "medically needy" category. They also have low incomes, but do not qualify for, or choose not to participate in, the SSI/SSP Program. For example, aged low-income noncitizens generally may not apply for SSI/SSP (although they may
| Figure 11 | |||||
| Who is Eligible for Medi-Cal?
Major Eligibility Categories | |||||
| 1997-98 | |||||
| Maximum
Monthly Income Or Grants a |
Asset
Limit Imposed? |
Spend-
Down b Allowed? |
Enrollees
(Thousands) |
Annual
Benefit Costs (Millions) c | |
| Aged, Blind, or Disabled Persons | |||||
|
$1,156 | -- | 1,103 | $5,417 | |
|
934 | 112 | 876 | ||
|
Special
limits |
69 | 2,177 | ||
| Families, Pregnant Women, Children | |||||
| Single-parent or unemployed families | |||||
|
$1,014
d |
-- | 2,582 | $3,017 | |
|
1,190 | 436 | 724 | ||
| Any women or children | |||||
| Pregnant women | |||||
|
$2,765 | -- | -- | 92 | $336 |
all services |
1,190 | 11 | 95 | ||
| Children | |||||
poverty--infants |
$2,765 | -- | -- | 40 | --
e |
|
1,869 | --
f |
-- | 93 | $56 |
|
1,428 | --
f |
-- | 38 | 21 |
|
$1,190 | 278 | $371 | ||
| Emergency-Only | |||||
| Illegal immigrants and nonimmigrant aliens who qualify in any eligibility group are limited to emergency services (including labor and delivery and long-term care). | 235 | $509 | |||
| aAmounts are for aged or disabled couple (blind slightly more) or for a four-person family with children (including a $90 work expense disregard). | |||||
| bIndicates whether persons with higher incomes may receive benefits on a share-of-costs basis. | |||||
| cCombined state and federal cost. | |||||
| dIncome limit to apply for CalWORKs (including a $90 work expense disregard). After going on aid, the income limit increase to $1,355 (family of four) with the maximum earned income disregard. | |||||
| ecosts included in amount for 200 percent of poverty pregnant women group. | |||||
| fReflects changes made by Chapter 624, Statutes of 1997 (SB 903, Lee), which are scheduled to take effect in March 1998. | |||||
continue on SSI/SSP if they already were in the program as of August 22, 1996). As another example, about one-fifth of the medically needy persons in this category have incomes above the Medi-Cal limit and participate on a share-of-cost basis.
The number of Medi-Cal eligibles in long-term care is small, only 69,000 people or 1.3 percent of the total caseload; but because long-term care is very expensive, benefit costs for this group total $2.2 billion, or 16 percent of total Medi-Cal benefit costs.
About half of the aged or disabled Medi-Cal eligibles also have health coverage under the federal Medicare Program. Medi-Cal generally pays the Medicare premiums, deductibles and any co-payments for these "dual beneficiaries," and Medi-Cal pays for services not covered by Medicare, such as drugs and long-term care. Medi-Cal also provides some limited assistance to a small number of Medicare eligibles who have incomes somewhat higher than the medically needy standard.
Families. About half of all Medi-Cal eligibles are CalWORKs welfare recipients in single-parent or unemployed families, who automatically receive Medi-Cal coverage. Although CalWORKs recipients constitute the largest group of Medi-Cal eligibles by far, they account for only 22 percent of total Medi-Cal benefit costs. This is because almost all CalWORKs recipients are children or nondisabled working-age adults, who generally are relatively healthy.
Single-parent or unemployed families who are not in CalWORKs also may enroll in Medi-Cal in the medically needy family category. Medi-Cal covers both the adults and the children in these families. The income and asset limits for medically needy families are somewhat higher than for CalWORKs applicants. Qualifying families with higher incomes also may participate in the medically needy category on a share-of-cost basis.
Women and Children. Medi-Cal includes a number of additional eligibility categories for pregnant women and for children. Women and children in these categories may be in any type of family, including working, two-parent families. Medi-Cal covers all health care services for poor pregnant women in the medically indigent category, which has the same income and asset limits and spend-down provisions as apply to medically needy families. However, pregnancy-related care is covered with no share of cost for women up to 200 percent of poverty (an annual income of $33,180 for a family of four, including a $90 monthly work expense disregard).
The medically indigent category also covers children and young adults through age 20. Several special categories provide coverage without a share of cost or an asset limit to children in families with higher incomes--200 percent of poverty for infants, 133 percent of poverty for children ages 1 through 5, and 100 percent of poverty for children ages 6 through 18. Chapter 624, Statutes of 1997 (SB 903, Lee) extends the 100-percent-of-poverty group to ages 14 through 18 and eliminates the asset limit for poverty-group children. The budget indicates that these changes will be implemented in March 1998.
Emergency-Only Medi-Cal. Noncitizens who are illegal immigrants or who are not here as immigrants (such as tourists or students) may apply for Medi-Cal coverage in any of the regular categories (except those linked to welfare). However, benefits are restricted to emergency care (including labor and delivery). Existing coverage for prenatal care (a state-only program) was scheduled to end in February 1998, according to the Governor's budget, pursuant to restrictions placed on services to nonqualified aliens as a result of the federal welfare reform legislation of 1996. However, DHS now indicates that the termination of prenatal services has been delayed until March 1998 due to litigation. Nonemergency long-term care continues to be provided "until various legal issues are resolved," according to the budget.
The budget estimates that the 1997-98 General Fund share of Medi-Cal benefit costs will be $119.4 million (1.8 percent) less than in 1996-97 and that there will be a slight additional reduction of $15.3 million in 1998-99. These reductions in General Fund benefit costs primarily result from declines in the CalWORKs-related portion of the Medi-Cal caseload and from a modest increase in the federal medical assistance percentage (FMAP) for California, which is the federal share of Medi-Cal benefit costs. Increases in the cost and utilization of health care services, however, offset some of these savings and moderate the spending decline for benefits.
The budget projects that total Medi-Cal local assistance costs from the General Fund will increase by $39.5 million (0.6 percent) in 1998-99. This is because increased costs for county administration and for debt service payments more than offset the slight decline in projected spending on benefits.
| Figure 12 | |||||
| Medi-Cal General Fund Budget Summary
Department of Health Servicesa | |||||
| 1996-97 Through 1998-99
(Dollars in Millions) | |||||
|
Actual 1996-97 |
Estimated 1997-98 |
Proposed 1998-99 |
Change
From
1997-98 | ||
| Amount | Percent | ||||
| Support (state
operations) |
$64.6 | $66.2 | $68.2 | $2.0 | 3.1% |
| Local Assistance | |||||
| Benefits | $6,474.9 | $6,355.5 | $6,340.1 | -$15.3 | -0.2% |
| County
administration
(eligibility) |
312.2 | 317.6 | 349.9 | 32.3 | 10.2 |
| Fiscal
intermediaries
(claims processing) |
41.5 | 72.5 | 72.2 | -0.3 | -0.5 |
| Hospital
construction
debt service |
9.6 | 34.6 | 57.5 | 22.8 | 66.0 |
| Subtotals,
local assistance |
($6,838.3) | ($6,780.1) | ($6,819.7) | ($39.5) | (0.6%) |
| Totals | $6,902.9 | $6,846.4 | $6,887.9 | $41.6 | 0.6% |
| aExcludes General Fund Medi-Cal spending budgeted in other departments. | |||||
Caseload--$199 Million Savings. The major reason for the savings in the current year is that the budget's caseload estimate is 3.3 percent (173,300 eligibles) less than the amount assumed in the 1997-98 budget appropriation. The lower caseload results in estimated General Fund savings of $199.4 million. The biggest adjustment is for CalWORKs eligibles (a reduction of 75,300 from the 1997-98 budget assumption). CalWORKs-linked eligibles now are estimated to decline by 8.4 percent in the current year (a decline of 236,000 from 1996-97). The more rapid decline in CalWORKs eligibles results in about $44 million of savings compared with the budget appropriation. However, there are even larger caseload-related savings in other eligibility groups. A reduction of about 27,000 disabled eligibles (versus the 1997-98 budget assumptions) results in about $100 million of savings. There also has been a steeper than anticipated decline in the number of illegal immigrants on Medi-Cal, which will save about $40 million.
Rate Increases--$60.8 Million Cost. The current-year estimate includes General Fund increases of $38.3 million to increase managed-care rates by 6.4 percent (effective October 1997) and an additional $22.5 million increase in nursing home rates to include the "ripple" effect of the minimum wage increase on wages of higher-paid employees.
Prenatal Elimination Delayed--$22.4 Million Cost. The administration assumes the elimination of prenatal care for illegal immigrant women on February 1, 1998, rather than in October 1997 as the 1997-98 budget assumed. This results in increased costs of $22.4 million. Costs will increase by an additional $6.2 million, however, due to a further one-month delay resulting from recent litigation, as noted earlier in this analysis.
"Estimate Uncertainty" Adjustment--$110 Million Reduction. On a net basis, the cost increases identified above and other smaller changes offset about $72 million of the estimated caseload savings. The budget, however, includes an additional downward General Fund adjustment of $109.6 million to the Medi-Cal estimate in the current year (and $133 million in 1998-99). This adjustment represents a 2 percent reduction to the midrange cost estimate produced by the DHS Medi-Cal forecasting model. According to DHS, the adjustment is warranted by (1) more recent drops in the CalWORKs caseload that were not reflected in the data used to prepare the budget forecast and (2) potential distortions in the fee-for-service cost trends in the model that result from the current shift of eligibles to managed care. The department also notes that it believes that its Medi-Cal estimating model has a variance of plus or minus 4 percent, based on the accuracy range of other large economic models; and that the budget adjustment reduces the estimate by half of this variance range.
Caseload and FMAP Savings Offset by Cost/Utilization Growth. Total Medi-Cal eligibles are projected to decline by 148,000 (2.9 percent) in 1998-99, resulting in a General Fund savings of about $102 million. An increase in the FMAP for California saves an additional $65.8 million (the FMAP will be 51.55 percent by October 1998). These savings, however, are almost entirely offset by underlying increases in the cost of health care services and in the rate of utilization of these services, which increase General Fund spending by approximately $165 million.
Uncertainty Adjustment--$133 Million Reduction. The 1998-99 budget projection includes an "estimate uncertainty" adjustment of $133 million, similar to the current-year adjustment described above.
Termination of Prenatal Benefits--$43.7 Million Savings. Full-year savings from eliminating prenatal care for illegal immigrants reduces General Fund spending by an additional $43.7 million compared with the current year.
Healthy Families--$20.6 Million Increase. The Legislature and Governor recently enacted a new Healthy Families Program, which expands health coverage for children. The Medi-Cal changes associated with this new program include (1) providing one month of continued eligibility for children who otherwise would lose Medi-Cal eligibility in order to allow for transfers to the Healthy Families insurance program, (2) extending Medi-Cal coverage to children ages 14 through 18 in families with incomes up to 100 percent of poverty, and (3) eliminating the asset limitation for children who apply for Medi-Cal. The budget increase also provides a total of $5 million from the General Fund for Medi-Cal outreach activities. Most of the Healthy Families-related General Fund spending is budgeted to receive an enhanced federal match of about 2-to-1.
Developmental Services Case Management--$17 Million Increase.Proposed Medi-Cal spending includes an additional $17 million for transfer to the Department of Developmental Services for increased case management services.
Full-Scope Benefits for New Legal Immigrants--$14.9 Million Increase. This increase reflects the full-year cost of providing full-scope Medi-Cal coverage to qualifying recently-arrived legal immigrants. The federal government will share in the costs only for emergency services. Nonemergency services are being provided on a state-only basis starting December 1997.
Hearing Screens for Newborns--$1.3 Million Increase. The budget proposes to require hearing screens for newborns as part of the Governor's Early Childhood Prevention Initiative. The budget estimates that 30 percent of Medi-Cal babies will be screened in 1998-99.
Hospital Debt Service--$22.8 Million Increase. This increase reflects the anticipated completion of several major construction projects for hospitals with a significant proportion of Medi-Cal patients, for which the state has previously agreed to share in the repayment of construction debt.
County Administration--$32.3 Million Increase. The budget includes an increase of $17.9 million in county administration costs for caseload growth (subject to later revision for caseload trends). An additional increase of $7.8 million funds the full-year cost of administering a new Medi-Cal eligibility category that was created by the federal welfare reform legislation. Finally, allocating a portion of the cost of eligibility determinations for CalWORKs applicants to the Medi-Cal Program results in an increase of $7.7 million in the Medi-Cal budget, but results in an overall savings in state funds due to reductions reflected in the CalWORKs Program.
Some Potential Costs Not Included in the Budget. The January budget includes no funding for any rate increases for nursing homes or for managed care organizations in 1998-99. The current-year General Fund cost of these rate increases totals about $70 million (these costs usually are added in the May Revision). The budget also does not include any funding to pay San Diego County's mandate reimbursement claim for $15.2 million for health care costs for medically indigent adults. The basis for the county's claim was affirmed by the California Supreme Court, which also set aside a lower court award to the county and remanded the claim to the Commission on State Mandates to determine the amount of any reimbursement to the county. The commission expects to adjudicate the claim this summer.

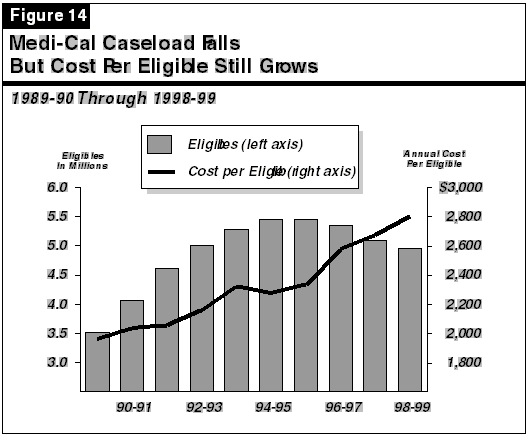
The earlier rapid growth in General Fund spending was largely driven by a rapid increase in the Medi-Cal caseload, as shown in Figure 14 (see next page). The most important reason for the end of rapid spending growth is that the Medi-Cal caseload is now declining. The budget estimates that the number of Medi-Cal eligibles will fall by 4.8 percent in the current year and projects an additional decline of 2.9 percent in 1998-99. Essentially all of this decline is due to large reductions in the CalWORKs-related portion of the Medi-Cal caseload, which the budget estimates will decline by an estimated 8.4 percent in 1997-98 and by 6.5 percent in 1998-99. The total number of Medi-Cal eligibles in other categories remains almost constant.
Figure 14 also illustrates why spending remains roughly flat, despite the significant caseload reductions in the budget. The cost of services per Medi-Cal eligible continues to rise--offsetting the caseload savings. Most of the increase in the cost per eligible results from increases in medical care costs caused by inflation, new and more expensive technologies and drugs, and increased use of services. A significant portion of the projected increase in the cost per Medi-Cal eligible, however, results from a shift to a more expensive caseload "mix," as shown in Figure 15.
 The
average cost per eligible for the aged and disabled Medi-Cal caseload (including
those in long-term care) is more than four-and-a-half times greater than the
average cost per eligible for families and children on Medi-Cal (most of whom
are CalWORKs beneficiaries). Because the number of aged and disabled Medi-Cal
eligibles is holding steady, while the number of families and children on Medi-Cal
declines, a gradual shift to a more expensive mix of eligibles is occurring.
Figure 15 shows that the budget estimates that the average cost per eligible
will grow by 4.8 percent in 1998-99, compared with the current year. We
estimate that one-third of this increase is due to the change in case mix, so
that the growth in the cost of Medi-Cal services with a constant case mix would
be 3.2 percent.
The
average cost per eligible for the aged and disabled Medi-Cal caseload (including
those in long-term care) is more than four-and-a-half times greater than the
average cost per eligible for families and children on Medi-Cal (most of whom
are CalWORKs beneficiaries). Because the number of aged and disabled Medi-Cal
eligibles is holding steady, while the number of families and children on Medi-Cal
declines, a gradual shift to a more expensive mix of eligibles is occurring.
Figure 15 shows that the budget estimates that the average cost per eligible
will grow by 4.8 percent in 1998-99, compared with the current year. We
estimate that one-third of this increase is due to the change in case mix, so
that the growth in the cost of Medi-Cal services with a constant case mix would
be 3.2 percent.
| Figure 15 | ||||
| Medi-Cal Program
Changing Case Mix Increases Cost Per Eligible | ||||
| 1998-99 | ||||
|
Eligibility Category |
Eligibles | Cost Per Eligible | ||
| Number
(Thousands) |
Percent
Change
From 1997-98 |
Amount | Percent Change From 1997-98 | |
| Disabled | 801 | -0.6% | $ 6,980 | 4.0% |
| Aged | 489 |
-- |
$ 6,497 | 2.3 |
| Families and children | 3,656 | -6.2 | $ 1,387 | 2.8 |
| Totals | 4,947 | -2.9% | $ 2,799 | 4.8% |
| Cost per eligible--percent change with constant case mix | 3.2% | |||
Reporting Requirement. The 1997-98 Budget Act directed our office to report on the effect of the increasing number of Medi-Cal eligibles enrolled in managed care on the DHS Medi-Cal estimating process. We also were directed to identify any methodology issues that require further study and refinement to ensure the accuracy of the Medi-Cal estimate.
In enacting the 1997-98 budget, the Legislature reduced the department's Medi-Cal cost estimate by $64 million from the General Fund. The Legislature took this action based on our finding that the ongoing shift of Medi-Cal eligibles to managed care was distorting the cost trends used in the DHS Medi-Cal estimating model, resulting in an overestimate. The reason for the department's overestimate was that the model depended primarily on fee-for-service cost trends, which were overstated because the model did not adjust for the effect of the shift of generally less costly persons into managed care.
The DHS Has Revised Its Methodology. The Medi-Cal estimate in the 1998-99 Governor's Budget incorporates two adjustments intended to correct the upward bias discussed above. First, the estimate budgets the cost of persons shifting to managed care at the managed care rates, rather than at projected average fee-for-service costs, which are higher. This adjustment reduces the estimate by $14.9 million and $18.9 million in 1997-98 and 1998-99, respectively (about half General Fund). The second adjustment reduces the 1998-99 estimate by an additional $75 million (about half General Fund). This adjustment reduces the cost of the remaining fee-for-service eligibles.
Legislative Analyst's Office Initial Assessment. Our preliminary review of the department's adjustments to the Medi-Cal estimating model suggests that they appear to be appropriate. They seem to correct for distortions in the model caused by the current shift to managed care. Also, the magnitude of the proposed adjustments does not appear unreasonable. However, we did not have an opportunity to review the adjustments or the methodology behind them prior to the release of the budget, and the department has not yet provided us with its calculations for the adjustments. We will evaluate them as part of our overall review of the Medi-Cal estimate for the May Revision of the budget, as discussed in our next finding.
In addition to the specific adjustments for the shift to managed care discussed above, the Medi-Cal estimate also includes General Fund savings that result from global adjustments that reduce the department's mid-point cost projections for Medi-Cal benefits by 2 percent. The department believes that its Medi-Cal estimating model has a range of uncertainty of plus or minus 4 percent. The adjustments represent half of this range, on the minus side. The department indicates that the global adjustments are warranted by recent continued caseload drops and because of the uncertain impacts of the shift to managed care on cost trends for fee-for-service Medi-Cal eligibles.
Although we raised concerns about overestimates in the Medi-Cal model last year, the current downward adjustments for uncertainty appear to be arbitrary. As we discussed in our previous finding, the budget estimate already includes two specific adjustments intended to correct trend distortions caused by the shift to managed care. Furthermore, the most recent caseload data appear to be consistent with the budget's Medi-Cal caseload projections.
At this time, we believe that the most prudent course is to exclude these adjustments from the budget estimate, which would increase estimated General Fund spending in the budget for Medi-Cal by a cumulative total of $242.6 million in 1997-98 and 1998-99. For the May Revision, we will provide the Legislature with a specific recommendation on adjustments to the updated Medi-Cal estimate, based on a more detailed evaluation of the department's methodology and using the most recent available caseload and expenditure information.
The budget includes a total of $18.9 million ($9.4 million General Fund) in the current year and $35.8 million ($17.9 million General Fund) in 1998-99 for county Medi-Cal administrative functions related to caseload growth for beneficiaries who are not on welfare. (Most county administration costs for welfare recipients are included in the Department of Social Services' budget). The funding for caseload increases would cover administrative costs for an additional 62,806 average monthly nonwelfare Medi-Cal eligibles in 1997-98 and a further increase of 58,674 eligibles in 1998-99. The county administration estimate is based on a straight-line projection of administrative workload trends over the last five years, during which caseloads generally increased. This estimate is made independently from the Medi-Cal caseload estimate.
Based on our review, however, we conclude that the department's proposal is overbudgeted because it does not reflect recent and projected trends in the nonwelfare Medi-Cal caseload. Specifically, the nonwelfare portion of the Medi-Cal caseload has been essentially flat for the last year, and the Medi-Cal caseload estimate projects that the size of this group will remain almost constant through 1998-99 (while the caseload on welfare declines). Because it is a linear trend, the county administration workload projection continues to assume caseload growth that is no longer occurring. There will be some additional county Medi-Cal workload as more welfare recipients find jobs and shift to transitional Medi-Cal categories that provide temporary continued coverage. However, the budget separately includes an additional $5.1 million (state and federal) for this purpose in 1998-99.
Based on the Medi-Cal caseload estimate, no caseload adjustment for county administration is necessary in the current year, and only $2.4 million ($1.2 million General Fund) will be needed in 1998-99. Accordingly, we recommend reducing the current-year General Fund spending estimate by $9.4 million and reducing the 1998-99 General Fund budget request by $16.7 million.
Health Coverage for Families That Are Not on Welfare. Most low-income working families do not have access to affordable employer-sponsored health coverage (particularly for dependents). State and federal policies have been adopted to maintain health coverage for families that leave welfare for work, and to make it available for working poor families. These policies stem from a desire to (1) protect and improve the health of poor families--especially children--and (2) eliminate the incentive to be on welfare in order to receive health coverage. Working poor families may obtain free or subsidized health coverage in a number of Medi-Cal categories or in several other state programs, including the following:
These programs currently provide health coverage for almost one million Californians.
Transitional Medi-Cal
Because transitional Medi-Cal coverage directly helps those leaving welfare for work, such coverage has taken on more importance in the context of welfare reform.
1997-98 Budget Legislation Expands Transitional Medi-Cal. The 1997-98 budget trailer bill for health services (Chapter 294, Statutes of 1997 [SB 391, Solis]) includes a number of provisions to expand eligibility for, and increase participation in, transitional Medi-Cal coverage as outlined below:
The 1997-98 Budget Act provided $1.5 million ($138,000 General Fund) to improve outreach and simplify the eligibility process for transitional Medi-Cal. The Governor's budget proposes to continue this funding in 1998-99.
Participation Rates. Relatively few of the families who leave the CalWORKs rolls participate in the transitional Medi-Cal program. Based on DHS caseload data, we estimate that less than 10 percent of those leaving the welfare rolls participate in the initial six months of transitional coverage. Of those who do enroll in the initial six-month transitional period, about 40 percent go on to participate in the second six-month period of coverage. As of September 1997, enrollment in transitional coverage was about 60,000 for the first six-month period and about 20,000 for the second six-month period. Although participation rates remain low, enrollment in the transitional categories has grown rapidly over the last year, increasing by 31 percent between September 1996 and September 1997.
Benefit Costs. Not only do relatively few of those leaving welfare use transitional coverage, but those that do participate use less expensive health services and/or use them less often. Specifically, the department estimates that the average annual cost per eligible in the transitional coverage programs is $518, which is about half of the average annual Medi-Cal benefit cost for CalWORKs recipients.
Factors Underlying the Low Participation Rate. The apparent low participation rate in transitional coverage is somewhat misleading because many of those who leave the welfare rolls are not eligible for transitional coverage. Frequently, people are terminated from welfare because they have stopped filing required reports. And of these, some (perhaps a substantial number) have not filed due to a temporary disruption in their lives, such as moving to another county, and soon return to the welfare rolls (and automatic Medi-Cal coverage) after the disruption is over. A DSS analysis of AFDC enrollment found that about a third of those leaving welfare returned to the rolls within six months. Other persons leave the state's welfare rolls on a more permanent basis, but not because of increased earnings. For example, they may move to another state or receive help from their family so that they no longer need welfare.
Usually, county eligibility workers do not immediately know why families stop reporting, and need additional information to redetermine Medi-Cal eligibility. Pending redetermination, these families are placed in a temporary continuing Medi-Cal category (called the Edwards v. Kizercategory, after a court decision), generally for one month. Based on the information that they provide, these families then are placed in transitional Medi-Cal or in another Medi-Cal category if they (or their children) are eligible. If, however, the family cannot be located or does not provide information, their Medi-Cal eligibility ends, and their potential eligibility for transitional coverage remains unknown.
For the reasons discussed above, the meaning of the apparent low participation rate (and low cost of care) in transitional Medi-Cal is unclear. It may indicate serious shortcomings in education and outreach or that the eligibility redetermination process needs to be changed. On the other hand, it may be that most people who go off welfare do not qualify for transitional Medi-Cal and there is no need for fundamental changes in existing practice. Likewise, the low cost of transitional benefits may indicate that beneficiaries are not able to access adequate care, or it may indicate that they need less care (because women returning to work may delay childbearing, for example).
We believe that a number of approaches could be used to gain a better understanding of participation rates for transitional Medi-Cal and determine the need for program changes. For example, DHS and DSS could analyze recent caseload data to better estimate how many of those who leave CalWORKs return to welfare or to another Medi-Cal eligibility category in a short time; DHS and the counties could perform follow-up interviews with a sample of former welfare recipients; and DHS could survey clinics and community organizations. Accordingly, we recommend that DHS report at the time of budget hearings on the extent to which qualified families are using transitional Medi-Cal; the department's use of the funding provided in the 1997-98 Budget Act, and progress to date in carrying out the outreach, education, and monitoring and evaluation improvements mandated in Chapter 294; and any program changes needed to improve the transitional Medi-Cal program.
The budget proposes $2,563,000 ($1,281,500 General Fund) for the cost of providing extended transitional Medi-Cal benefits in 1998-99. Under the extended benefit, the state would provide transitional Medi-Cal for up to two years, rather than the current one-year limit. Federal Medicaid law limits transitional benefits to a maximum of one year, but federal law also allows HCFA to issue waivers of many Medicaid requirements, including the one-year limit, to enable states to expand coverage. Waivers, however, require a finding of budget neutrality--that is, the waiver must not increase federal costs compared with projected spending under existing law. State law (Chapter 294) makes extended transitional coverage contingent on federal approval.
Chapter 197, which originally authorized the extension of transitional coverage, was enacted in July 1996--a month prior to passage of federal welfare reform. When Chapter 197 was enacted, the offsetting federal savings required to gain a waiver for extending transitional Medi-Cal were to have come from reduced AFDC costs that would result because continued health coverage would help low-income working families stay off welfare. California, however, did not submit a formal waiver request until after enactment of federal welfare reform in August 1996, which replaced the federal matching funds in the AFDC program with the TANF block grant. As a result of this change to a block grant, the state cannot claim federal savings from reducing the CalWORKs caseload.
The state's initial waiver request was rejected by HCFA in July 1997. The DHS currently is seeking HCFA approval for a modified waiver to allow the state to provide an additional year of transitional coverage to determine if their subsequent use of Medi-Cal services over a five-year period is less than for families that received only one year of transitional coverage prior to the waiver. Accordingly, we withhold recommendation, pending the outcome of those discussions.
New Medi-Cal Coverage for Welfare "Look-Alikes"
The 1996 federal welfare reform legislation eliminated the previous automatic ("categorical") link between welfare and Medicaid that had existed under the former AFDC Program. Instead, families that receive welfare assistance under the new TANF Program must separately meet Medicaid eligibility criteria in order to qualify for health coverage.
Welfare Reform Created New "1931(b)" Eligibility Category. In order to ensure that health coverage would remain at least as accessible to poor families after welfare reform as it was under the former AFDC categorical linkage, Congress created a new class of Medicaid eligibles under Section 1931 of Title XIX of the Social Security Act (the Medicaid law). Section 1931(b) requires states to grant automatic (categorical) Medicaid eligibility to anyone who would have met the AFDC requirements in place in that state on July 16, 1996. This guarantees continued Medicaid eligibility to welfare "look-alikes," people who would have met the former AFDC rules, regardless of whether states choose to be more restrictive in their TANF welfare programs.
States Can Use 1931(b) Category to Retain Link Between Welfare and Medicaid. The federal welfare reform legislation gave states flexibility in Section 1931(b) to revise the July 16 requirements by adopting more liberal income or resource standards (or, alternatively, reduce the income standard down to its level on May 1, 1988). The legislation also allows states to continue Medicaid coverage expansions authorized under previously granted AFDC waivers. This flexibility generally allows states to retain automatic Medicaid coverage for TANF welfare recipients even if their TANF eligibility criteria are more liberal than their former AFDC eligibility criteria. States can do so by adopting 1931(b) criteria that are no more restrictive than their TANF requirements, so that all of their TANF welfare recipients automatically become eligible for Medicaid under Section 1931(b).
Section 1931(b) eligibility, however, is not limited to welfare recipients. Anyone who qualifies is eligible for Medi-Cal, regardless of whether they are on welfare or not.
The CalWORKs Program Linked to Medi-Cal Through 1931(b) Requirement. The legislation establishing the CalWORKs Program-- Chapter 270, Statutes of 1997 (AB 1542, Ducheny, Ashburn, Thompson, and Maddy)--requires the state to exercise its option under federal law to increase its 1931(b) income and resource standards to the new CalWORKs levels. (The maximum earned income "disregard" after going on aid and the asset limit both are higher under CalWORKs than under the state's July 1996 AFDC rules.) Increasing the 1931(b) income and asset standards to the CalWORKs amounts--"CalWORKs conformity"--ensures that all CalWORKs recipients will automatically qualify for Medi-Cal. Because of 1931(b) requirements, however, families that meet the CalWORKs requirements now are eligible for Medi-Cal regardless of whether or not they are on welfare.
Medi-Cal Eligibility for Poor Families Expands Under 1931(b). There are four ways in which Section 1931 can expand Medi-Cal eligibility beyond the current Medi-Cal Medically Needy Program for poor working families who are not on welfare:
The Governor's budget does not address the eligibility expansions authorized under Section 1931(b) that we have discussed above. For example, the Medi-Cal budget estimate does not include any additional benefit costs due to increased eligibility for transitional Medi-Cal or potentially greater earnings disregards that may result from eligibility expansions under Section 1931(b). Furthermore, the budget proposal to increase county administration funding for 1931(b) determinations (discussed in the next recommendation in this section) is fundamentally flawed. Finally, the administration does not address coordination of 1931(b) eligibility with eligibility under the existing Medically Needy category, and does not indicate how 1931(b) eligibility will be monitored and linked with transitional Medi-Cal eligibility.
Prior to budget hearings, the department should develop a specific and comprehensive proposal and cost estimate for implementing Section 1931(b) Medi-Cal eligibility. Figure 16 (see next page) summarizes issues that we have identified and that should be addressed in the plan and indicates potential options for the state.
| Figure 16 | ||
| Issues and Options for Implementing Section 1931(b)
Medi-Cal Eligibility Comparison With Existing CalWORKs and Medi-Cal Medically Needy Programs | ||
| CalWORKs | Medi-Cal
Medically Needy |
Section 1931(b)
Eligibility Issues/Options |
| Monthly Income Limit
(Examples for family of four) | ||
| Options | ||
income disregard |
|
|
| Issues | ||
| ||
| Asset Limits | ||
| Options | ||
|
|
|
| Continued | ||
| Asset Limits | ||
| Issues | ||
| ||
| Unemployment Test for Two-Parent Families | ||
| Options | ||
|
|
|
| Issues | ||
| ||
| Linkage and Access to Transitional Medi-Cal Coverage | ||
| Options | ||
| ||
| Issues | ||
| ||
| ||
The budget proposes an increase of $62.5 million in 1998-99 ($15.6 million General Fund and $46.9 million federal funds) to cover additional county administration costs for (1) determining Section 1931(b) eligibility for families and children applying for Medi-Cal (other than those also applying for welfare) and (2) monitoring ongoing cases with respect to 1931(b) eligibility. The budget also estimates that the counties will require an additional $31.3 million ($7.8 million General Fund and $23.5 million federal funds) in the current year for these tasks.
Federal funds would be provided at a three-to-one matching ratio from California's share of a special allocation provided to help states cover added administrative costs to implement Section 1931 Medicaid eligibility provisions. This proposal would use $70.4 million of California's total share of $83 million from the special allocation. After the $83 million is exhausted, the federal share of these costs will revert to the regular 50 percent share for Medicaid administrative costs.
The budget assumes that making 1931(b) eligibility determinations will add an average of 30 minutes per intake and 5 minutes per month for each continuing Medi-Cal case involving children. The budget proposal indicates that these 1931(b) screenings are needed to determine whether Medi-Cal recipients will be eligible for transitional coverage if they become employed, and to notify beneficiaries of this eligibility.
New Determinations Will Substitute for Existing Workload. Currently, county eligibility workers generally first screen families applying for Medi-Cal to determine whether they qualify for medically needy coverage for both parents and children. Families that exceed the medically needy income or asset limits, or who are working two-parent families, then are evaluated for eligibility under the medically indigent or poverty-level programs, which cover only children or pregnant women.
The new 1931(b) income and asset limits for Medi-Cal intakes (which are the same as the CalWORKs application limits) are somewhat less than the medically needy limits. To accommodate this new category, families should first be evaluated for 1931(b) eligibility. Most families that currently fall into the medically needy category probably will qualify in the 1931(b) category instead, and those that do not will be evaluated for other categories in the same manner as done currently. Thus, the 1931(b) determination will simply substitute for the current medically needy determination in most cases.
We also note that screening for 1931(b) eligibility will not be feasible for children and pregnant women who use the new simplified mail-in application process authorized by Chapter 624, Statutes of 1997 (SB 903, Lee) because those forms will not include information about assets.
For the reasons discussed above, additional funding for 1931(b) eligibility determinations is unnecessary. Accordingly, we recommend deleting the proposed augmentation and reducing the associated current-year expenditures.
In the current year and 1998-99, the Medi-Cal budget includes about $37 million annually from the General Fund for the 1997-98 rate increase for long-term-care facilities that was effective on August 1, 1997. However, the budget does not include any funding for a 1998 rate increase.
Existing law requires DHS to audit nursing homes in order to determine their costs and to adjust rates annually in August to reflect those costs. This process conformed with the "Boren Amendment" provision of federal law, which required Medi-Cal rates for long-term care facilities to be sufficient to cover the costs of "efficiently and economically operated" facilities. Congress repealed the Boren Amendment in the Balanced Budget Act of 1997, however, so the state no longer is bound to provide cost-based rates to long-term care facilities.
The budget indicates that DHS will convene interested parties to consider alternatives to the current rate-setting mechanism for 1998-99 and subsequent years. We note, in this respect, that we have previously recommended that the state contract for Medi-Cal nursing facility services through the California Medical Assistance Commission (CMAC), as the state does for hospital inpatient services, in order to obtain the best rates and ensure adequate capacity for Medi-Cal patients (please see our Analysis of the 1996-97 Budget Bill, p. C-44).
Because long-term care is a major Medi-Cal expense and a critical service on which many elderly and disabled people depend, we recommend that the department report at budget hearings on its plans for revising the way in which nursing home payments are determined.
Finally, we note that the Legislature directed DHS in the 1997-98 Budget Act to report on the feasibility of using regional clearinghouses to facilitate the transfer of Medi-Cal patients from hospitals to nursing homes. The department indicates that it currently is in the process of completing this report.