Health and Social Services
Federal Medicaid Match |
The budget does not reflect the full amount of state savings that would result from the administration's proposal to increase California's federal Medicaid matching rate--specifically, the savings resulting from an increase in federal Title XXI funds (related to the state's Healthy Families Program). Consequently, we recommend a technical correction so the budget will be consistent, for a General Fund savings of $2.3 million in 1999-00. (Reduce Item 4260-113-0001 by $122,000, item 4280-101-0001 by $1,985,000, and item 4440-101-0001 by $232,000.)
The Governor's budget proposes, in the budget for the Department of Health Services (DHS), that the federal administration adopt a methodology change that would increase the federal Medicaid matching rate for California from 51.67 to 53.36 percent in federal fiscal year 2000, effective October 1999 (see our analysis of the California Medical Assistance Program [Medi-Cal]). The budget reflects General Fund savings of $210 million in the Medi-Cal program as a result of the proposed increase in federal Title XIX Medicaid funds. The budget, however, omits the corresponding savings that would be achieved due to the resulting increase in federal Title XXI funds for the state's Healthy Families Program (HFP), which has an enhanced federal matching rate that is tied to the federal Medicaid rate. This would affect the budgets in the Managed Risk Medical Insurance Board, the DHS, and the Department of Mental Health. Accordingly, we recommend a technical correction to make the budget consistent, which would result in General Fund savings of $2.3 million in 1999-00.
We also note that the budget places all the General Fund savings associated with the Medi-Cal program in the DHS, whereas some of these savings would occur in other departments where the state match for Medicaid funds is budgeted. (The Department of Social Services, for example, indicates that about $8 million of the savings should be reflected in its budget.) According to the DHS, these adjustments will be made in the May revision of the budget.
Health and Social Services
Health and Human Services Agency (0530) |
The Secretary of the California Health and Human Services Agency (formerly the Health and Welfare Agency) is directly responsible to the Governor for general policy formulation in the health and human services area.
The budget proposes $2.3 million ($1.3 million from the General Fund) to support the agency in 1999-00, which is approximately the same as estimated current-year expenditures.
The budget proposes a $37.3 million General Fund set-aside to implement a plan for health care reforms that will be submitted by the Secretary of the California Health and Human Services Agency.
We identify several approaches for the Legislature to consider regarding (1) expansion of health care coverage for uninsured working families in the Healthy Families Program (HFP) and the California Medical Assistance Program (Medi-Cal), (2) simplification of administration, and (3) improved participation.
The budget includes a "set-aside" of $37.3 million from the General Fund that is reserved for expenditure on health care reforms, pursuant to a plan to be submitted by the Secretary of the Health and Human Services Agency. According to the administration, this plan may be submitted either as a budget proposal or as a proposal for separate legislation. Funding for the set-aside is contingent on federal action because it is tied to federal approval of a waiver to provide Medicaid funding for family planning services currently funded entirely by the state, which the budget assumes will result in $122 million of General Fund savings in 1999-00. In his budget summary, the Governor indicates that the plan will give consideration to the following issues, many of which involve the HFP, a program that currently provides health insurance for children:
Millions of Californians are uninsured--they do not have health coverage, whether job-based, privately purchased, or through a public program such as Medi-Cal. For example, The State of Health Insurance in California, 1998, recently published by the Health Insurance Policy Program of the University of California, estimates that seven million nonelderly Californians are uninsured, and California has one of the lowest rates of health insurance coverage in the nation. The large number of uninsured persons has raised concerns about the adequacy of health care services for a significant portion of the state's population, and it has imposed a large burden on county indigent care programs, community clinics, and other components of the state's health care "safety net."
The options presented in the budget for the Secretary's consideration all seek to increase health insurance coverage. Additional coverage has been the goal of many recent legislative proposals, including enactment of the HFP to expand health coverage for children. However, it is important to remember that health care coverage is a means, rather than an end. Coverage does no good unless it provides effective care. Moreover, increasing the proportion of the population that is insured does not necessarily result in an equivalent increase in the proportion who are healthy since most people are generally healthy regardless of insurance status. A survey reported in The State of Health Insurance in California, 1998, indicates that although the uninsured are twice as likely as the insured to report their health status as fair or poor, the great majority of both groups reported their health status as either good or excellent (82 percent for the uninsured). This is not surprising, since many of the uninsured are teens and younger adults, who generally tend to be healthy.
Furthermore, while studies have shown that the insured make greater use of health care services than the uninsured, everyone has some access to care. Emergency treatment at hospitals is legally guaranteed to all regardless of ability to pay. County indigent care programs and other elements of the health care safety net provide a significant amount of free or low-cost care to the uninsured. Medi-Cal, in effect, provides "major medical" coverage for unenrolled, but eligible, children and families. Finally, some people still pay directly for care.
Criteria for Evaluating Expansion Proposals. Health care programs can be very expensive, and their cost can grow rapidly if not carefully controlled. Given limited state resources, it is crucial to target any health coverage expansions where they will be the most effective and make the best use of existing resources and funding streams. With this in mind, we suggest the following criteria for evaluating proposals to expand coverage:
The new federal CHIP program and recent changes in federal Medicaid laws and regulations provide the state with a number of approaches to further expand health care coverage to working families, with federal funds providing one-half to two-thirds of the cost. Expanding coverage will require state (and/or local) funding to cover the nonfederal share of costs. However, we believe that simplifying eligibility could produce some partially offsetting administrative savings to the state and that expanding coverage could reduce county indigent care costs.
We further suggest that the Legislature consider funding for coverage expansion on its on merits within the Legislature's overall fiscal priorities and available resources rather than tying it to a single action, such as federal approval of the family planning waiver.
We have identified a number of approaches for expanding coverage. These approaches include variations of--or more specific means of implementing--the options mentioned in the Governor's budget, as well as other approaches for the Legislature's consideration, as listed below:
Implementing these approaches in a coordinated and cost-effective manner probably would require the state to seek a Section 1115 demonstration project waiver from the federal government. Waiver authority might be needed, for example, to unify eligibility criteria and benefit packages under Medi-Cal and the HFP, and possibly to enable the state to use the federal share of any administrative savings to provide additional financing for extended coverage. Waiver authority also may be needed to allow the state to charge premiums on a sliding-scale basis for Medi-Cal beneficiaries at higher income levels.
In summary, we believe that there are a number of avenues available to the Legislature for expanding health care coverage for working families using available federal matching funds, and building on the existing Medi-Cal and HFP.
Department of Health Services (Medi-Cal) (4260) |
In California, the federal Medicaid Program is administered by the state as the California Medical Assistance (Medi-Cal) Program. This program provides health care services to welfare recipients and other qualified low-income persons (primarily families with children and the aged, blind, or disabled). Expenditures for medical benefits are shared about equally by the General Fund and by federal funds. The Medi-Cal budget also includes additional federal funding for (1) disproportionate share hospital (DSH) payments, which provide additional funds to hospitals that serve a disproportionate number of Medi-Cal or other low-income patients, and (2) matching funds for state and local funds in other related programs.
At the state level, the Department of Health Services (DHS) administers the Medi-Cal Program. Other state agencies, including the California Medical Assistance Commission (CMAC), the Department of Social Services (DSS), the Department of Mental Health, the Department of Developmental Services, and the Department of Alcohol and Drug Programs receive Medi-Cal funding from DHS for eligible services that they provide to Medi-Cal beneficiaries. At the local level, county welfare departments determine the eligibility of applicants for Medi-Cal and are reimbursed by DHS for the cost of those activities. The federal Health Care Financing Administration (HCFA) oversees the program to ensure compliance with federal law.
Proposed Spending. The budget for DHS proposes Medi-Cal expenditures totaling $21.1 billion from all funds for state operations and local assistance in 1999-00. The General Fund portion of this spending ($7.4 billion) decreases by a relatively small amount ($68.8 million or 0.9 percent) compared with estimated General Fund spending in the current year. The spending total for the Medi-Cal budget includes an estimated $3.5 billion (federal funds and local matching funds) for payments to disproportionate share hospitals (DSH), and about $1.8 billion of federal funds to match $1.6 billion of state and local funds budgeted elsewhere for programs operated by other departments, by counties, or by the University of California. Including these other state and local funds, total proposed Medicaid spending in California would be about $22.7 billion in 1999-00, according to the budget.
Federal law requires the Medi-Cal Program to provide a core of basic services, including hospital inpatient and outpatient care, skilled nursing care, doctor visits, laboratory tests and x-rays, family planning, and regular examinations for children under the age of 21. California also has chosen to offer 32 optional services, such as outpatient drugs and dental care, for which the federal government provides matching funds. Certain Medi-Cal services--such as hospitalization in many circumstances-- require prior authorization from DHS as medically necessary in order to qualify for payment.
Most of the Medi-Cal caseload consists of participants in the state's two major welfare programs, which include Medi-Cal coverage in their package of benefits. These programs are (1) the California Work Opportunity and Responsibility to Kids (CalWORKs) program, which provides assistance to families with children and replaces the former Aid to Families with Dependent Children (AFDC) program, and (2) the Supplemental Security Income/State Supplementary Program (SSI/SSP), which assists elderly, blind, or disabled persons. Counties administer the CalWORKs program and county welfare offices determine eligibility for CalWORKs benefits and Medi-Cal coverage concurrently. Counties also determine Medi-Cal eligibility for persons who are not eligible for (or do not wish) welfare benefits. The federal Social Security Administration determines eligibility for SSI/SSP, and the state automatically adds SSI/SSP beneficiaries to the Medi-Cal rolls.
Generally, persons who have been determined eligible for Medi-Cal benefits (Medi-Cal "eligibles") receive a Medi-Cal card, which they use to obtain services from providers who agree to accept Medi-Cal patients. Medi-Cal uses two basic types of arrangements for health care--fee-for-service and managed care.
Fee-for-Service. This is the traditional arrangement for health care in which providers are paid for each examination, procedure, or other service that they furnish. Beneficiaries may obtain services from any provider who has agreed to accept Medi-Cal payments. The Medi-Cal Program employs a variety of "utilization control" techniques (such as requiring prior authorization for some services) designed to avoid costs for medically unnecessary or duplicative services.
Managed Care. Prepaid health plans generally provide managed care. The plans receive monthly "capitation" payments from the Medi-Cal Program for each enrollee in return for providing all of the covered care needed by those enrollees. These plans are similar to health plans offered by many public and private employers. By the end of 1998-99, DHS expects to have about half (2.5 million) of the projected 5 million Medi-Cal eligibles enrolled in managed care organizations. Beneficiaries in managed care choose a plan and then must use providers in that plan for most services. Since payments to the plan do not vary with the amount of service provided, there is much less need for utilization control by the state. Instead, plans must be monitored to ensure that they provide adequate care to enrollees.
Almost all Medi-Cal eligibles fall into two broad groups of people. They either are aged, blind, or disabled or they are in families with children. More than two-thirds of Medi-Cal eligibles are welfare recipients. Figure 1 shows for each of the major Medi-Cal eligibility categories the maximum income limit in order to be eligible for health benefits, and the estimated caseload and total benefit costs for 1998-99. The figure also indicates for each category whether an asset limit applies and whether eligible persons with incomes over the limit can participate on a "spend-down" basis. If spend-down is allowed, then Medi-Cal will pay the portion of any qualifying medical expenses that exceed the person's "share of cost," which is the amount by which that person's income exceeds the applicable Medi-Cal income limit.
| Figure 1 | |||||
| Who is Eligible for Medi-Cal?
Major Eligibility Categories | |||||
| 1998-99 | |||||
| Maximum Monthly Income Or Granta | Asset Limit Imposed? | Spend-DownbAllowed? | Enrollees (Thousands) | Annual Benefit Costs (Millions)c | |
| Aged, Blind, or Disabled Persons | |||||
| Welfare (SSI/SSP) | $1,201 | -- | 1,125 | $6,299 | |
| Medically needy | 934 | 112 | 670 | ||
| Medically needy--long term care | Special limits | 68 | 2,241 | ||
| Families, Pregnant Women, Children | |||||
| Single-parent or unemployed families | |||||
| Welfare (CalWORKs) | $1,009d | -- | 2,444 | $3,057 | |
| Section 1931(b) only | 1,009e | -- | --f | --f | |
| Medically needy | 1,190 | 467 | 783 | ||
| Any women or children | |||||
| Pregnant women | |||||
| 200 percent of poverty-- pregnancy services | $2,832 | -- | -- | 102 | $372 |
| Medically indigent--all services | 1,190 | 11 | 96 | ||
| Children | |||||
| 200 percent of poverty-- infants | $2,832 | -- | - | 40 | --g |
| 133 percent of poverty-- ages 1 through 5 | 1,914 | -- | -- | 97 | $67 |
| 100 percent poverty--ages 6 through 18 | 1,461 | -- | -- | 57 | 37 |
| Medically indigent--ages 0 through 21 | 1,190 | 268 | 409 | ||
| Emergency-Only | |||||
| Undocumented immigrants who qualify in any eligibility group are limited to emergency services (including labor and delivery and long-term care). | 216 | $502 | |||
| a Amounts are for aged or disabled couple (blind slightly more) or for a four-person family with children (including a $90 work expense disregard). | |||||
| b Indicates whether persons with higher incomes may receive benefits on a share-of-costs basis. | |||||
| c Combined state and federal costs. | |||||
| d Income limit to apply for CalWORKs (including a $90 work expense disregard). After becoming eligible, the income limit increases to $1,680 (family of four) with the maximum earned income disregard. | |||||
| e Applicant income limit; increases to $2,080 after enrollment. | |||||
| f Not fully implemented in 1998-99. Enrollment and costs included in amounts for CalWORKs recipients. | |||||
| g Costs included in amount for 200 percent of poverty pregnant women group. | |||||
Aged, Blind, or Disabled Persons. About 1.3 million low-income persons who are (1) at least 65 years old or (2) disabled or blind persons of any age receive Medi-Cal coverage. Overall, the disabled make up more than half (61 percent) of this portion of the Medi-Cal caseload. Most of the aged, blind, or disabled persons on Medi-Cal (86 percent) are recipients of SSI/SSP welfare benefits and receive Medi-Cal coverage automatically. The other aged, blind, or disabled eligibles are in the "medically needy" category. They also have low incomes, but do not qualify for, or choose not to participate in, the SSI/SSP program. For example, aged low-income noncitizens generally may not apply for SSI/SSP (although they may continue on SSI/SSP if they already were in the program as of August 22, 1996). As another example, about 17 percent of the medically needy persons in this category have incomes above the Medi-Cal limit and participate on a share-of-cost basis.
The number of Medi-Cal eligibles in long-term care is small, only 68,000 people or 1.3 percent of the total caseload; but because long-term care is very expensive, benefit costs for this group total $2.2 billion, or 15 percent of total Medi-Cal benefit costs.
Almost 60 percent of the aged or disabled Medi-Cal eligibles also have health coverage under the federal Medicare Program. Medi-Cal generally pays the Medicare premiums, deductibles and any co-payments for these "dual beneficiaries," and Medi-Cal pays for services not covered by Medicare, such as drugs and long-term care. Medi-Cal also provides some limited assistance to a small number of Medicare eligibles who have incomes somewhat higher than the medically needy standard.
Families. About half of all Medi-Cal eligibles are CalWORKs welfare recipients in single-parent or unemployed families, who receive Medi-Cal coverage under the state's "Section 1931(b)" Program (discussed later in this analysis). Although CalWORKs recipients constitute the largest group of Medi-Cal eligibles by far, they account for only 21 percent of total Medi-Cal benefit costs. This is because almost all CalWORKs recipients are children or nondisabled working-age adults, who generally are relatively healthy.
Single-parent or unemployed families who are not in CalWORKs also may enroll in Medi-Cal in the Section 1931(b) Program or in the medically needy family category. Medi-Cal covers both the adults and the children in these families. The income and asset limits for medically needy families are somewhat higher than for Section 1931(b) applicants (who must meet essentially the same requirements as CalWORKs applicants). However, once enrolled, Section 1931(b) families may work and remain on Medi-Cal at higher income levels. Qualifying families with higher incomes also may participate in the medically needy category on a share-of-cost basis.
Women and Children. Medi-Cal includes a number of additional eligibility categories for pregnant women and for children. Women and children in these categories may be in any type of family, including working, two-parent families. Medi-Cal covers all health care services for poor pregnant women in the medically indigent category, which has the same income and asset limits and spend-down provisions as apply to medically needy families. However, pregnancy-related care is covered with no share of cost for women up to 200 percent of poverty (an annual income of $33,984 for a family of four, including a $90 monthly work expense disregard).
The medically indigent category also covers children and young adults through age 20. Several special categories provide coverage without a share of cost or an asset limit to children in families with higher incomes--200 percent of poverty for infants, 133 percent of poverty for children ages 1 through 5, and 100 percent of poverty for children ages 6 through 18. Chapter 624, Statutes of 1997 (SB 903, Lee) extended the 100 percent of poverty group to ages 14 through 18 and eliminated the asset limit for poverty-group children. Chapter 624 also authorized the use of a simplified mail-in application for pregnant women and poverty-group children.
Emergency-Only Medi-Cal. Noncitizens who are undocumented immigrants, or are otherwise not qualified immigrants under federal law, may apply for Medi-Cal coverage in any of the regular categories. However, benefits are restricted to emergency care (including labor and delivery). Medi-Cal also provides prenatal care and nonemergency long-term care to undocumented immigrants. These services, as well as nonemergency services for recent legal immigrants, do not qualify for federal funds and are supported entirely by the General Fund.
The average cost per eligible for the aged and disabled Medi-Cal caseload (including long-term care) is much higher than the average cost per eligible for
families and children on Medi-Cal (most of whom are CalWORKs recipients). As a result, more than half of Medi-Cal spending is for the elderly and
disabled, although they account for only about one-fourth of the total Medi-Cal caseload, as shown in Figure 2 (see next
page).
Figure 3 (see page 29) presents a summary of Medi-Cal General Fund expenditures in the DHS budget for the past, current, and budget years.
| Figure 3 | |||||
| Medi-Cal General Fund Budget Summary
Department of Health Servicesa | |||||
| 1997-98 Through 1999-00
(Dollars in Millions) | |||||
| Actual 1997-98 | Estimated 1998-99 | Proposed 1999-00 | Change From 1998-99 | ||
| Amount | Percent | ||||
| Support (state operations) | $66.6 | $65.5 | $66.1 | $0.6 | 0.9% |
| Local Assistance | |||||
| Benefits | $6,384.6 | $6,942.4 | $6,863.7 | -$78.7 | -1.1% |
| County administration (eligibility) | 287.3 | 328.4 | 355.7 | 27.3 | 8.3 |
| Fiscal intermediaries (claims processing) | 66.8 | 72.6 | 69.5 | -3.1 | -4.3 |
| Hospital construction debt service | 20.4 | 54.5 | 39.6 | -14.9 | -27.3 |
| Subtotals, local assistance | ($6,759.1) | ($7,397.9) | ($7,328.5) | (-$69.4) | -0.9% |
| Totals | $6,825.7 | $7,463.4 | $7,394.6 | -$68.8 | -0.9% |
| a Excludes General Fund Medi-Cal spending budgeted in other departments. | |||||
The budget estimates that the 1998-99 General Fund share of Medi-Cal benefit costs will total $6.9 billion--an increase of $538 million (8.4 percent) compared with 1997-98. The primary reason for the higher spending is an increase in the cost and utilization of services (caseload remains almost flat--a decline of 1 percent). Provider rate increases account for $156 million of added General Fund cost. These rate increases include a 6.1 percent increase for nursing facilities, costing an estimated $80.7 million (partly reflecting the effects of recent increases in the minimum wage on nursing facility operating costs). Additionally, rate adjustments added in the 1998-99 Budget Act account for $51.6 million of the General Fund cost increases, mostly to enhance rates for primary and preventive care by physicians, which had not been adjusted, in many cases, since the 1980s. The 1998-99 Budget Act also increased General Fund costs by $40 million by reducing the amount of DSH funds retained by the state to offset General Fund Medi-Cal costs, and it provided $25 million from the General Fund for a Fresno regional burn and trauma center. The department also indicates that drug costs and hospital use have increased significantly in the current year.
In addition to the higher cost of benefits, other local assistance costs are up by $81 million (General Fund) in the current year compared with 1997-98. County administration costs have increased by $41.1 million, partly due to a new policy of allocating to Medi-Cal a portion of eligibility determination costs for CalWORKs applicants in order to maximize federal funding, and also because of new costs to implement the Medi-Cal portions of the Healthy Families Program. The General Fund cost for hospital construction debt service payments increases by $34.1 million in 1998-99 because several major projects were completed recently.
Although some of the spending increases noted above were anticipated in the 1998-99 Budget Act, others were not. Furthermore, the budget assumed a number of savings that did not occur, and caseload, although declining, is above the budget estimate. As a result, the 1999-00 Governor's Budget now estimates that Medi-Cal local assistance spending from the General Fund will exceed the current-year budget appropriation by $507 million. The major components of the additional spending, are as follows:
"Uncertainty" Savings Did Not Materialize--$132 Million. The 1998-99 Budget Act assumed that spending on Medi-Cal benefits would be at the bottom of the uncertainty range around the department's midpoint estimate (a 2 percent savings). Actual trends have gone in the other direction, and the 1999-00 Governor's Budget eliminates the savings from this "uncertainty adjustment."
Caseload Above Estimate--$109 Million. The Medi-Cal caseload is 3.5 percent above the 1998-99 budget estimate. Almost all of the increase is in the CalWORKs-related portion of the Medi-Cal caseload, and results from automatically continuing the Medi-Cal eligibility of former CalWORKs recipients due to delays in implementing the new Section 1931(b) Medi-Cal eligibility category.
Drug Costs Are Up--$78.8 Million. The department primarily attributes this spending increase to a more rapid than anticipated shift to new, more expensive, antipsychotic medications.
Continuation of Prenatal Care for Undocumented Women-- $64.4 Million. The 1998-99 Budget Act assumed savings from the elimination of this state-only Medi-Cal service. The 1999-00 Governor's Budget funds continuation of this service through the budget year pending the outcome of litigation challenging implementation of regulations to end the program. (The budget also funds state-only long-term care for undocumented immigrants, also the subject of litigation, through the budget year, but funding for this service was included in the 1998-99 Budget Act.)
Longer Hospital Stays for Labor and Delivery--$31 Million. The budget indicates that recent federal and state legislation mandating minimum hospital stays for labor and delivery have increased the average length of stay and resulted in increased costs for these services over the amount anticipated in the 1998-99 Budget Act.
Managed Care Rate Increase--$24 Million. The 1998-99 Budget Act did not include funding for rate increases (averaging 4.7 percent) which have been granted by the department to managed care plans in the 12 counties operating under the "two-plan" model. The budget does not identify the cost of additional rate increases granted by the CMAC to the six county-operated Medi-Cal managed care plans and to plans operating under the "geographic managed care" model in Sacramento and San Diego Counties.
Reduced "Crossover" Savings--$12.6 Million. The department is implementing limits on crossover payments to hospitals for services to Medi-Cal beneficiaries who are also covered by Medicare. Under these limits, Medi-Cal covers patient co-payments only to the extent that the Medicare payment falls short of the equivalent Medi-Cal rate. Detailed claims analysis indicates that savings will be somewhat less than anticipated.
The Governor's budget estimates that total Medi-Cal spending from the General Fund (in the DHS budget) will be $7.4 billion in 1999-00, which is a slight decline of $68.8 million, or 0.9 percent, from estimated current-year spending. The budget also estimates that the total Medi-Cal caseload will decline by 1 percent (about 50,000 persons). The projected spending decline, however, results from assumed increases in federal funds and a one-time recovery of past excess crossover payments. Absent these special adjustments, projected General Fund spending for Medi-Cal local assistance would increase by $274 million, or 3.7 percent, in 1999-00. The major General Fund spending changes and assumptions in the budget are discussed in Figure _.
Increased Federal Matching Rate--$210 Million Savings. The budget assumes that the federal government will increase California's Federal Medical Assistance Percentage (FMAP) for federal fiscal year (FFY) 00, beginning October 1, 1999, to 53.36 percent, compared with the announced FFY 00 FMAP of 51.67 percent. The state contends that the announced FMAP is based on faulty population estimates for California by the U.S. Census Bureau, which were used in the formula to determine the state's FMAP.
Family Planning Waiver--$122.2 Million Savings. The budget assumes federal approval of a Medicaid demonstration project waiver that would provide 90 percent federal funding for the existing state-only family planning program, which serves low-income persons who are not Medi-Cal eligible. Currently, this program is supported entirely by the General Fund.
Retroactive Recoupment of Hospital Crossover Payments-- $50.5 Million Savings. The department proposes to recoup the portion of Medi-Cal payments made to hospitals in excess of the Medi-Cal/Medicare crossover limits. The recoupment period dates back to May 1994, while the crossover limits were being challenged in the courts. Congress included a provision in the 1997 Balanced Budget Act clarifying the state's authority to impose crossover limits, and enabling the state to recoup these overpayments. Hospitals will be made whole for this recoupment by the federal government under Medicare's "bad-debt" provisions.
Audit Exception for Institutions for Mental Disease (IMD)-- $44.4 Million Cost. The federal government has disallowed payments for the cost of physician and other ancillary services for Medi-Cal eligibles who reside in IMDs, which the state has claimed as Medicaid costs since July 1992. The budget includes $44.4 million from the General Fund to satisfy this federal audit exception, and indicates that the state will no longer fund these services because there is no state authority to do so, and because responsibility for these services was transferred to counties in the realignment of mental health services.
County Administration--$27.3 Million Cost Increase. General Fund costs for county eligibility determination activities increase by 8.3 percent in 1999-00. Most of the increase is for an annual "cost-of-doing-business" adjustment of 3.9 percent ($9.5 million), processing Section 1931(b) eligibility determinations ($7.9 million increase), and expiration of enhanced federal funding for outreach for children's coverage ($2.8 million). The county administration budget also includes an increase of $2.8 million for various Medi-Cal administrative costs incurred by the Department of Developmental Services.
Some Likely Costs Not Included in the Budget. The January budget includes no funding for any rate increases for nursing homes or for managed care organizations in 1999-00. The current-year General Fund cost of these rate increases is more than $100 million. The nursing home rate increase generally is added in the May Revision. The budget also does not include any funds for hospital outpatient rate increases (potentially tens of millions of dollars) that may be necessary, depending on the outcome of a rate study. Hospitals successfully challenged the basis for the state's current rates in Orthopaedic Hospital v. Belshe, and a court order in that case requires DHS to set new rates that have a reasonable relationship to costs. The department expects to establish the new rates in early 1999-00. Furthermore, there is no funding in the budget to pay San Diego County's mandate reimbursement claim of $15.2 million for past health care costs for medically indigent adults. The basis for this claim was affirmed by the California Supreme Court, and the claim is likely to be acted on by the Commission on State Mandates before the end of 1999-00.
Figure 4 shows Medi-Cal caseload and General Fund spending since 1991-92. During the period 1991-92 through 1995-96, both caseload and spending rose in a roughly similar manner. The average annual growth rates were 4.3 percent for caseload and 6.8 percent for spending. Starting in 1996-97, however, the two trends diverge sharply, as caseload has declined while costs have continued to grow. From 1995-96 through the current year (as estimated in the budget) caseload has declined at an average annual rate of 2.7 percent, but costs have continued to rise at an annual rate of 7.8 percent. The "spread" between the growth rates for spending and caseload has grown from 2.5 percent in the earlier period to 9.7 percent from 1995-96 through the current year.
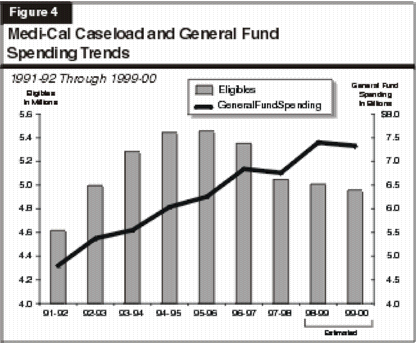
The continued upward trend in spending reflects, in part, costs for recently completed hospital construction projects and the ongoing increase in county administration costs. The primary driver of the spending growth, however, is an increase in the cost and utilization of services by Medi-Cal beneficiaries. Figure 5 illustrates this trend. From 1991-92 through 1995-96, the average cost per Medi-Cal eligible grew at an annual rate of 3.2 percent. Between 1995-96 and 1998-99, however, the annual rate of growth has increased to an average of 7.8 percent.
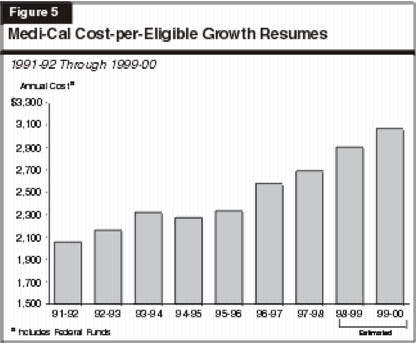
Case Mix Change Contributes to Increased Cost Per Eligible. Higher costs and greater utilization of services are the main reasons why Medi-Cal spending is increasing in the face of declining caseload. But a changing caseload mix also contributes to a higher cost per eligible and dampens any caseload savings. This is because the number of elderly and disabled Medi-Cal eligibles is holding steady, while the number of families and children on Medi-Cal declines (primarily due to declining CalWORKs welfare rolls). On average, the cost per eligible for the elderly or disabled is about four and one half times that for families and children. Consequently there has been a gradual shift to a more expensive mix of eligibles.
Between 1995-96 and 1998-99, the percentage of the Medi-Cal caseload that are elderly or disabled increased from 23 percent to 26 percent. Since the average Medi-Cal cost per eligible for the elderly and disabled is more than four times higher than for children and families, even this relatively modest change in the mix contributes to the increasing overall cost per eligible. We estimate that about 10 percent of the increase in the average cost per eligible in the current year is due to this case mix effect. Harder to estimate, is the possible effect of a selective decline in the CalWORKs caseload. This would occur to the extent that persons leaving CalWORKs (or choosing to stay off welfare) tend to be healthier than those who remain on CalWORKs.
The significant cost increases since 1995-96 happen to coincide with the implementation of the two-plan model for Medi-Cal managed care in most of the larger counties, and the implementation of a county-organized health system in Orange County. During this time, enrollment of Medi-Cal eligibles in managed care plans has increased from roughly 25 percent to almost 50 percent. Consequently, the expansion of Medi-Cal managed care has not resulted in any readily apparent slowing of spending growth, although it is possible that spending might have grown even faster without the managed care expansion.
The Medi-Cal budget includes a total of $332 million of General Fund savings that depend on two federal actions : (1) an increase in the Federal Medical Assistance Percentage (the federal sharing ratio for Medi-Cal benefit costs) and (2) approval of a Medicaid waiver to provide federal funding for the current state-only family planning program. Neither of these assumed actions is assured.
As mentioned in our earlier description of the 1999-00 Medi-Cal spending proposal, the budget assumes that the federal government will approve two state requests that would result in a total of $332 million of General Fund savings in the Medi-Cal Program.
The FMAP Increase--$210 Million. On January 12, 1999, the Secretary of the U.S. Department of Health and Human Services announced the FMAPs that will be in effect for each state during FFY 00 (October 1999 through September 2000). California's FFY 00 FMAP is 51.67 percent. The budget assumes that the federal government will revise California's FFY 00 FMAP to 53.36 percent. This increase in the federal share of Medi-Cal costs would reduce state General Fund costs by $210 million (a small portion of these savings would occur in the budgets of other departments, and will be reallocated in the May Revision of the budget).
The FMAP is calculated according to a federal statutory formula based on the relationship of per capita personal income in each state to the national average over a moving three-year period. The lower a state's per capita personal income relative to the nation, the higher its FMAP. Per capita personal income is derived by taking the U.S. Department of Commerce's estimate of total state personal income and dividing it by the U.S. Census Bureau's estimate of state population. Accordingly, a higher population estimate for a state will reduce the calculated per capita personal income and result in a larger FMAP.
The Governor's budget indicates that the Census Bureau's population estimates for California are too low because they continue to show a net movement of people from California to other states, whereas the Department of Finance (DOF) estimates that California has been gaining population from other states in recent years in response to an improved economy. The bureau uses federal tax return information, which tends to have a significant lag, to track population movement between states. The DOF, however, uses more recent drivers' license information to estimate net migration for California.
We believe that the administration is correct, and an increase in the state's FMAP is justified. However, no mechanism currently exists to make that adjustment for FFY 00. Under federal law, the determination of FMAPs by the federal Health and Human Services Secretary is "conclusive," and therefore there is no process for appealing it. Furthermore, allocating more population to California requires reducing the population estimates of other states and adjusting their FMAPs accordingly. This probably is not feasible in the short term, since there is no national database of drivers' license information. Alternatively, Congress could address the state's concern by adding funds to the federal FFY 00 budget to provide an ad hoc adjustment for California. In any case, the budget's assumption of an increase in California's FMAP creates a General Fund risk.
Family Planning Waiver--$122.2 Million. Currently, California's family planning program serves both Medi-Cal eligibles and those whose incomes are under 200 percent of poverty, but exceed the normal Medi-Cal income limits. The state receives 90 percent federal funding for family planning services for those who are Medi-Cal eligibles, but no federal funds for those who are not Medi-Cal eligible. The budget proposes to shift the state-only portion of the existing family planning program to 90 percent federal funding under a Medicaid demonstration project waiver that will require federal approval.
Several states have received family planning waivers or are currently applying for them. Oregon, for example, recently received this type of waiver to substantially expand its family planning program to individuals not previously served by that state. Waiver programs, however, must be "budget neutral" (that is, have no net cost) to the federal government. In the Oregon expansion, the additional federal costs for expanding coverage will be more than offset by the estimated federal Medicaid savings from reduced pregnancies. California's proposal is similar to Oregon's, but does not involve an expansion of coverage beyond that which currently is provided by the state.
The 1996 federal welfare reform legislation created a new Medicaid eligibility category, often referred to as "Section 1931(b)" (established in Section 1931(b) of Title XIX of the Social Security Act [the Medicaid law]). This new eligibility category replaces the previous automatic ("categorical") link to Medicaid for families on welfare.
Section 1931(b) makes anyone eligible for Medicaid who would have met their state's former requirements for Aid to Families with Dependent Children (AFDC) in effect on July 16, 1996. This guarantees Medicaid eligibility to people who would have met the former AFDC rules, regardless of whether states chose to be more restrictive in their Temporary Assistance for Needy Families (TANF) welfare programs, which replaced AFDC.
Section 1931(b) also allows states to expand Medicaid eligibility for low-income families by adopting income or resource standards that are more liberal than the former AFDC standards. This flexibility generally allows states to maintain automatic Medicaid coverage for TANF welfare recipients even if they adopt TANF eligibility criteria that are more liberal than their former AFDC requirements. For example, two factors used by the state to determine eligibility known as "earned-income disregards" and "asset limits" under California's TANF welfare program-- CalWORKs--are somewhat higher than under the state's July 1996 AFDC rules. The CalWORKs legislation, required DHS to increase the state's Section 1931(b) income and asset limits to the amounts needed in order to provide automatic Medi-Cal coverage to all CalWORKs recipients.
However, Section 1931(b) eligibility is not limited to welfare recipients. Families who meet the state's Section 1931(b) requirements are eligible for Medi-Cal regardless of whether they are on welfare. Furthermore, states can use their Section 1931(b) flexibility to expand Medicaid eligibility beyond their TANF welfare limits.
Overlaps With the Medically Needy Program Increase Medi-Cal's Complexity. For many years, California's Medically Needy Program has provided no-cost Medi-Cal coverage for poor families who are not on welfare. The requirements for Section 1931(b) eligibility are very similar to those for the Medically Needy Program, but they are not the same, and these differences increase the complexity of the county eligibility determination process without necessarily expanding coverage by very much. Section 1931(b) eligibility has higher earned-income disregards than the Medically Needy Program, but lower income limits for initial qualification. Section 1931(b) eligibility also provides up to two years of transitional Medi-Cal coverage when earnings increase above its income limits, whereas the Medically Needy Program does not include transitional coverage. Both programs have complex asset limits that differ in a number of details. The 1998-99 budget trailer bill for health (Chapter 310, Statutes of 1998 [AB 2780, Gallegos]) took one step toward simplification by increasing the general asset limit under Section 1931(b) from the CalWORKs limit of $2,000 to the asset limit used in the existing Medi-Cal Medically Needy Program--$3,300. However, other differences in the asset rules still exist, particularly with respect to vehicles.
More than 250,000 former California Work Opportunity and Responsibility to Kids recipients have been kept on the Medi-Cal rolls indefinitely due to delays by the Department of Health Services in issuing criteria and implementation guidelines for Section 1931(b) eligibility. We estimate that the General Fund cost of Medi-Cal coverage for these beneficiaries will total about $90 million through 1998-99, and that most of this cost will be for persons who would not otherwise be enrolled in Medi-Cal.
Section 1931(b) eligibility became effective in California on January 1, 1998, along with the implementation of the CalWORKs program. However, DHS did not issue any guidance to the counties for determining Section 1931(b) eligibility at that time. Instead, DHS directed counties to indefinitely hold persons leaving welfare in the existing "Edwards" Medi-Cal eligibility category pending the development of specific Section 1931(b) eligibility criteria.
More Than 250,000 Persons Retained on Medi-Cal in the "Edwards Hold." The purpose of the Edwards category (named after the Edwards v. Kizer court case) has been to provide a brief (one- to two-month) period of extended eligibility for persons terminated from CalWORKs, or the former AFDC program, during which counties attempt to contact those persons and determine whether they qualify for transitional Medi-Cal coverage or coverage under another Medi-Cal category. Persons who respond and qualify are placed in the appropriate category. Others are dropped from the Medi-Cal rolls.
Figure 6 shows that the Edwards Hold has had a significant effect on the CalWORKs-related component of the Medi-Cal caseload. During 1997, prior to the hold, this caseload declined steadily by between 25,000 to 30,000 persons per month. After counties began to implement the Edwards Hold in February 1998,the regular CalWORKs caseload on Medi-Cal (the CalWORKs "base") continued its steady decline. However, the "continuing eligibility" portion of the CalWORKs-related caseload (Edwards cases and transitional Medi-Cal) has grown rapidly, so that the total CalWORKs-related Medi-Cal caseload has remained essentially flat. Figure 6 illustrates the growth in the Edwards caseload since January 1998. In the figure, we allocate this growth in the Edwards caseload to the Edwards Hold component, while retaining the baseline January 1998 number of Edwards eligibles in the regular Continuing Eligibility caseload component. Each month, persons terminated from CalWORKs are added to the Edwards category, and remain there indefinitely, so that as of November 1998, this additional caseload in the Edwards Hold had accumulated to about 250,000 persons.

On September 30, 1998--nine months after the effective date of Section 1931(b) eligibility--DHS issued an "all-county letter" that provided procedures for determining Section 1931(b) eligibility, and instructed counties to immediately send out redetermination forms to Edwards Medi-Cal eligibles, terminate eligibility for those who do not respond, and complete eligibility reviews by April 30, 1999 for those who do respond. By May 1999, under the schedule in the letter, all of the Edwards Hold should be eliminated--either by termination from Medi-Cal or by reclassification into transitional Medi-Cal, Section 1931(b), or another regular Medi-Cal eligibility category.
Only a small proportion of the Edwards Hold eligibles are likely to remain on Medi-Cal after the redetermination process is completed. The primary eligibility categories for which families in the Edwards Hold caseload might qualify would be transitional Medi-Cal or Section 1931(b) coverage. However, only about 15 percent of the eligibles in the Edwards category made use of transitional Medi-Cal (which has no income limit initially) prior to implementation of the Edwards Hold. Although some families who have gone off of welfare will qualify for Section 1931(b) coverage, the caseload impact probably will be modest since Section 1931(b) eligibility duplicates other existing Medi-Cal eligibility categories (such as Medically Needy and transitional coverage) to a large extent. Finally, counties often do not have current addresses or phone numbers for Edwards beneficiaries, and a significant number who do receive redetermination forms do not return them. Information concerning many of the Edwards Hold beneficiaries now may be more than 12 months old, making contacting them more problematic.
Managed Care Costs Continue Regardless of Use of Services. Most Edwards Hold beneficiaries are enrolled in Medi-Cal managed care plans because the Edwards category is one of the mandatory enrollment categories for Medi-Cal managed care (in those counties with mandatory managed care). This means that the state has continued to pay monthly premiums to managed care plans for those Edwards Hold beneficiaries, regardless of whether they use services, have other coverage, or even have left the state. For those Edwards beneficiaries still in fee-for-service Medi-Cal, the state would also be overpaying because some of those beneficiaries would not otherwise qualify for Medi-Cal.
General Fund Costs for Edwards Hold Beneficiaries Will Total About $90 Million. We estimate that the cumulative General Fund cost for Edwards Hold eligibles will total approximately $90 million, assuming that counties complete their redeterminations by the end of 1998-99. For the reasons discussed above, it is likely that most of the persons in the Edwards Hold would not have been on the Medi-Cal rolls (beyond the normal one or two months in the Edwards category) if Section 1931(b) eligibility had been implemented in a timely manner. Accordingly, most of the $90 million General Fund cost is attributable to the implementation delay, and would not have been incurred had there been timely implementation of Section 1931(b) eligibility.
We recommend that the department (1) provide a progress report at budget hearings on the Section 1931(b) redeterminations and (2) identify any additional resources or county incentives needed to complete the redeterminations expeditiously.
The cost of the Edwards Hold could increase further if counties do not complete their Section 1931(b) eligibility redeterminations in the next few months. As of January 1999, few, if any, redeterminations had been completed. Moreover, the County Welfare Directors Association indicates that there may be additional delays in completing redeterminations because of (1) the large number of Edwards Hold cases, (2) staffing limitations, (3) the complexity of the process (the DHS guidance letter with attachments was more than 100 pages long), and (4) the need for clarification by DHS of the eligibility rules in some special circumstances.
No Incentive for Counties to Complete Redeterminations Quickly. Fiscal incentives for most counties run counter to quick completion of these redeterminations. Counties pay none of the benefit costs of Medi-Cal, and continuation of Medi-Cal coverage may reduce their indigent health care costs (by providing services to individuals who otherwise would be the responsibility of county indigent care programs). Also, county hospitals and health systems that participate in Medi-Cal managed care may benefit from continued capitation payments on behalf of individuals in the Edwards Hold.
Redeterminations Should Be Expedited. Section 1931(b) redetermination delays could result in tens of millions of dollars of additional General Fund costs for benefits and managed care premiums for individuals who do not qualify for (or may not want to participate in) Medi-Cal. Furthermore, additional delays will reduce the likelihood that counties will be able to reach those persons in the Edwards Hold who qualify for, and wish to receive, continued Medi-Cal coverage, as addresses and phone numbers become more outdated. In view of these facts, DHS should require counties to (1) send out eligibility redetermination packages immediately, (2) remove those who cannot be located or who do not respond from the Medi-Cal rolls, and (3) perform redeterminations on an expedited basis for those who respond and request continued coverage. In those instances where an eligibility determination requires further clarification from DHS, eligibility can be continued pending that clarification. Accordingly, we recommend that the department (1) provide a progress report at budget hearings on the Section 1931(b) redeterminations and (2) identify any additional resources or county incentives needed to complete the redeterminations expeditiously.
We recommend General Fund reductions totaling $126.7 million ($2.7 million in 1998-99 and $124 million in 1999-00) because we project that Medi-Cal caseloads for the California Work Opportunity and Responsibility to Kids (CalWORKs)-related eligibles will be lower than the budget estimates due to (1) elimination of the Edwards Hold cases and (2) ongoing large declines in the CalWORKs welfare caseload. (Reduce 1998-99 deficiency appropriation by $2,653,000 and Item 4260-101-0001 by $124,077,000.)
The budget estimates that the CalWORKs-related portion of the Medi-Cal caseload will decline by 3.9 percent (98,700 eligibles) in the current year and by an additional 3.3 percent (80,400 eligibles) in 1999-00. These caseload declines are much smaller than the DSS' estimate of the percentage declines in the number of persons in the CalWORKs welfare caseload--14.4 percent in the current year and 11.1 percent in 1999-00.
Effect of Edwards Hold Should Be Temporary. As we discuss in the preceding issue, the Edwards Hold is the major reason why the Medi-Cal caseload declines more slowly than the CalWORKs welfare caseload in the current year. However, this should be a temporary phenomenon limited to the current year. If DHS and the counties focus their efforts, then redetermination of eligibility for the great majority of the Edwards Hold caseload should be completed prior to 1999-00, and we expect (for the reasons explained above) that most of the Edwards Hold caseload will not remain on the Medi-Cal rolls.
Underlying Caseload Decline Continues. Aside from the Edwards Hold, the trend for the CalWORKs-related Medi-Cal caseload has been steadily downward (as shown in Figure 6), and this trend has been consistent with the declines in the CalWORKs welfare caseload. Moreover, our projection of the caseload trend for CalWORKs-related eligibles (excluding the Edwards Hold) yields essentially the same 11.1 percent decline forecasted by DSS for the CalWORKs welfare caseload. In other words, we believe that the decline in the CalWORKs-related Medi-Cal caseload in 1999-00 should reflect the underlying trend, after adjusting for the elimination of the excess caseload in the Edwards Hold. In doing so, the caseload decline in 1999-00 is larger than in the current year--not smaller, as the budget estimates.
According to DHS, the reason why the budget's projected decline in the CalWORKs-related Medi-Cal caseload is much less than the decline in the CalWORKs welfare caseload is because the budget assumes that most of the eligibles currently in the Edwards Hold and most of those who leave the CalWORKs welfare rolls in 1999-00 will remain eligible and enrolled in Medi-Cal. This has not been the case in the past, and recent trends appear no different. However, DHS cites two new developments as the basis for expecting a much slower caseload decline--the new Section 1931(b) eligibility category and the imposition of sanctions on adult CalWORKs recipients who fail to participate in work activities.
We see no reason to expect that Section 1931(b) eligibility, as currently structured, will significantly increase the proportion of former CalWORKs recipients who remain enrolled in Medi-Cal in 1999-00. This is because the Section 1931(b) eligibility criteria primarily duplicate coverage that has been available for some time to former CalWORKs recipients, especially transitional Medi-Cal. Furthermore, the use of transitional Medi-Cal already is reflected in the underlying caseload trend.
Failure of able-bodied adult CalWORKs recipients to participate in work activities will result in elimination of their portion of the grant and their removal from the CalWORKs rolls. However, sanctioned adults will remain eligible for Medi-Cal, and this will cause the number of CalWORKs-related eligibles in Medi-Cal to be somewhat larger than the number of individuals in CalWORKs. According to the DSS CalWORKs estimate, however, this effect will be small--affecting only about 2 percent of the CalWORKs caseload in 1999-00.
Analyst's Projections Indicate Caseload Savings of $126.7 Million. We have developed our own projections of the eligibles in the CalWORKs-related Medi-Cal caseload for the current year and 1999-00. Our projections phase out the Edwards Hold caseload by July 1, 1999, and then assume an 11.1 percent decline in the basic Medi-Cal CalWORKs-related caseload (consistent with the DSS estimate of CalWORKs recipients and with recent trends in the basic Medi-Cal caseload for this group). However, we have added an additional 62,223 eligibles to our base projection in 1999-00. The addition is the sum of DSS's estimates of (1) the number of sanctioned CalWORKs recipients and (2) the additional CalWORKs recipients who will leave welfare for work due to the new work requirements (assuming that they all remain on Medi-Cal). Based on our projections, the Medi-Cal caseload will be less than the budget estimate by 5,800 eligibles in the current year and by 274,300 eligibles in 1999-00 (on an average monthly basis). We estimate that the lower caseloads will reduce General Fund spending below the budget estimate by $2.7 million in the current year and by $124 million in 1999-00--a total General Fund savings of $126.7 million.
The department has adopted income limits for Section 1931(b) Medi-Cal eligibility significantly higher than necessary to meet the Legislature's mandate to cover California Work Opportunity and Responsibility to Kids recipients. Furthermore, while the budget includes additional administrative costs for this new eligibility category, it fails to recognize added benefit costs. We recommend that the Department of Health Services provide an estimate of additional Medi-Cal benefit costs associated with Section 1931(b) eligibility at budget hearings.
As noted above, existing state law extends Section 1931(b) Medi-Cal coverage to CalWORKs recipients. Specifically, Section 14005.30 of the Welfare and Institutions Code directs DHS to use the state's flexibility under federal law to adopt less restrictive income and resource eligibility standards and methodologies "to the extent necessary" to allow all CalWORKs recipients to be eligible for Medi-Cal. The department's Section 1931(b) eligibility standards, however, go significantly beyond the CalWORKs standards.
Section 1931(b) Income Limits Exceed CalWORKs Limits. Figure 7 compares the maximum allowable monthly income (for a family of three with one earner) under the department's Section 1931(b) guidelines with the comparable income limits under CalWORKs and under the former AFDC standards (as of July 16, 1996). These income limits are those that apply after families have initially qualified for coverage. As in CalWORKs and the former AFDC program, families must meet a lower income standard for initial qualification, but once in the program they are entitled to earned income disregards that allow them to retain additional earnings. As the figure shows, the Section 1931(b) monthly income limit is $343 above the CalWORKs limit (the income at which the grant is reduced to zero), and $569 above the former AFDC income limit.
| Figure 7 | ||
| Comparison of Monthly Income Limits
Under Section 1931(b) Medi-Cal , CalWORKs, and AFDC 1998-99 | ||
| (Family of Three With One Earner) | ||
| Monthly Income /percent of poverty level | Difference from Section 1931(b) Limit | |
| Section 1931(b) | $1,790 / 157 percent | -- |
| CalWORKsa | $1,447 / 127 percent | -$343 |
| AFDCa (July 16, 1996) | $1,221 / 107 percent | -$569 |
| a High cost counties. Cases without an able-bodied parent can qualify for a higher income limit of $1,589 if they have sufficient earned income. | ||
The reason for the higher Section 1931(b) limit is that DHS mixed elements of CalWORKs and AFDC eligibility rules in a way that results in a standard that is considerably higher than in either of the welfare programs. Primarily this involves using the "need" standard to set the basic income limit (as in AFDC) instead of the maximum grant (as in CalWORKs), and allowing the more generous CalWORKs earned income disregard. Because the need standard is higher than the maximum grant, the DHS guidelines result in an income limit that is significantly greater than allowed in either CalWORKs or the former AFDC program.
The DHS Bases Action on Federal Guidance. The department indicates that its expansion of Section 1931(b) income standards is necessary to comply with guidance from the federal Health Care Financing Administration (HCFA), which administers Medicaid law. That law generally requires each Medicaid eligibility category to have a single eligibility standard. Both CalWORKs and the former AFDC program use the need standard as the basis for determining the income eligibility of applicants (who do not qualify for the earned income disregard). Substituting the CalWORKs maximum grant level for the need standard for Section 1931(b) eligibility is not possible, according to DHS, because it would disqualify some applicants from Medi-Cal who would meet the welfare qualifications. Consequently, DHS retained the need standard as the basic income standard for Section 1931(b) applicants, and believes that it is required to use the same standard for recipients as well under the federal requirement for a single Medi-Cal income standard.
Implementation of Section 1931(b) raises complex issues, and federal policy still is evolving as specific issues arise in each state. The department's understanding of HCFA's position, however, was based on informal communications, not specific written guidance. Nor did the department submit an eligibility proposal to HCFA that was more consistent with the limitations of the Legislature's mandate. Additionally, the department did not alert HCFA to the significant eligibility expansion that would result from the interaction of the CalWORKs and AFDC methodologies in approach that HCFA suggested. Furthermore, DHS did not explore alternatives to avoid expanding Section 1931(b) eligibility more than necessary to cover CalWORKs recipients. Such approaches might include, for example, adopting an income disregard formula for Medi-Cal eligibility that lies between the AFDC and CalWORKs formulas to offset the use of the more generous need standard as the basic income test.
No Funding In Budget for Section 1931(b) Benefit Costs Outside of CalWORKs-Related Caseload. The budget includes $18.1 million from the General Fund for Section 1931(b) eligibility administration for nonwelfare recipients in 1999-00. However, it does not include any benefit costs for this new Medi-Cal eligibility category other than for the CalWORKs-related caseload. For example, some families in the existing Medically Needy Program will qualify under Section 1931(b) and remain eligible for Medi-Cal without a share of cost when their income increases. Accordingly, we recommend that DHS provide an estimate of additional Medi-Cal benefit costs associated with Section 1931(b) eligibility at budget hearings.
We recommend a General Fund reduction of $1,550,000 in the amount proposed for smoking cessation drugs for Medi-Cal enrollees because the budget overestimates the number of enrollees who are smokers. (Reduce Item 4260-101-0001 by $1,550,000.)
The department added smoking cessation drugs (such as the nicotine patch) to the Medi-Cal drug formulary on January 1, 1999, and the budget estimates that this action will increase General Fund drug costs by $9.1 million in 1999-00. The cost estimate assumes that 25 percent of Medi-Cal enrollees over the age of 15 are smokers, based on national smoking prevalence data. Due in part to the state's antismoking efforts, however, smoking is less prevalent in California than in the rest of the nation. Furthermore, the Medi-Cal population has a disproportionately large number of women, who tend to smoke less than men.
Based on smoking prevalence data in California according to age, sex, and ethnicity, we estimate that the number of Medi-Cal enrollees who are smokers is 426,000 versus the budget estimate of 500,000. Our estimate is based on smoking prevalences listed in Tobacco Control in California: Who's Winning the War?, an evaluation of the tobacco control program reported to DHS in June 1998 by the Cancer Prevention and Control Program of the University of California, San Diego. The difference of 74,000 smokers reduces the cost estimate by $1.6 million (General Fund). Accordingly, we recommend a General Fund reduction of $1.6 million.
We recommend that the department report at budget hearings on its progress in developing new methods of setting Medi-Cal rates for Medi-Cal managed care plans, nursing homes, and hospital outpatient services.
The department has been considering basic changes in its approaches to setting rates for the following three major categories of Medi-Cal services.
Spending on these services totals billions of dollars annually, and they affect most Medi-Cal enrollees. Accordingly, we recommend that the department report on its rate setting plans at budget hearings.
We withhold recommendation on $39.6 million requested from the General Fund (plus $42.4 million of federal matching funds) for debt-service payments for hospital construction projects, pending receipt and analysis of the basis for the request. We recommend that the department report at budget hearings with a projection of future annual program costs for projects that have received a state funding commitment.
The budget proposes a total of $82 million ($39.6 million General Fund) for the Hospital Construction/Renovation Reimbursement Program established by Chapter 1635, Statutes of 1988 (SB 1732, Presley). Estimated spending for the program in the current year is $112.3 million ($54.5 million General Fund). Under the SB 1732 program, the Medi-Cal Program makes supplemental payments to qualifying "disproportionate share" hospitals that contract with CMAC to serve Medi-Cal patients. These payments cover a portion of the debt-service costs for constructing or renovating hospital facilities. Federal matching funds for these debt-service payments are financed out of the Medicaid savings that result from CMAC's hospital contracting program, which operates under a federal waiver.
At the time this analysis was prepared, the department had not provided the Legislature with a specific basis for its 1999-00 budget request, such as a status update for each hospital construction project, a listing of the debt-service costs by project, and a calculation of the required state contribution by project. A number of major projects have been completed recently or are nearing completion, which could affect costs significantly. Accordingly, we withhold recommendation on the 1999-00 budget request for the SB 1732 program pending receipt of justification for the amount requested.
Projection of Future Costs Needed. Several major projects--including the Riverside, San Bernardino, and Santa Clara County hospitals--have been completed recently and several others are nearing completion, including the UC Davis Medical Center expansion, Natividad Medical Center in Monterey, and the Tower project at St. Francis Hospital in Los Angeles. These projects will have a significant effect on future annual state costs for this program. Cost projections for this program also are important for determining how much "room" will remain available for federal funding within the CMAC waiver savings for additional hospital construction projects, such as the replacement of the Los Angeles County-University of Southern California Hospital. Cost projections also are important in determining the amount of funds available for financing other waiver programs, such as SB 1255 hospital supplemental payments (Chapter 996, Statutes of 1989 [SB 1255, Robbins]) and supplemental payments to teaching hospitals. Accordingly, we recommend that the department report at budget hearings with a projection of the future annual costs of the program for projects to which the state already has committed.
We recommend enactment of legislation directing the department to revise the Medi-Cal estimate process in order to make it a much more useful and timely tool for budgeting, monitoring, and evaluating the Medi-Cal Program.
The Medi-Cal Program is huge, with General Fund spending in the DHS budget totaling $7.4 billion in the current year--almost as much as the $7.8 billion of General Fund spending for all segments of higher education and more than any other program outside of education. Including all other federal, state, and local funds, total annual Medi-Cal spending is almost $23 billion--a significant component of total health care spending in the state. About 5 million people are enrolled in Medi-Cal. However, the basic tool used by the administration, the Legislature, and other parties to monitor the program and evaluate proposed changes-- the annual Medi-Cal estimate--is outdated and inadequate for the task.
Outdated Approach. The estimate's format and approach have changed little for 20 years. Meanwhile, the Medi-Cal Program has changed substantially, and the capabilities of computers and software have grown exponentially. The estimate's focus remains limited to generating a fixed group of statistical trends of fee-for-service utilization and cost for certain categories of services. These trends may or may not do a reasonable job of forecasting spending (to our knowledge, DHS has not performed a rigorous analysis of the estimate's accuracy), but they provide almost no help in explaining why changes occur. Modern computers and database software are much more powerful and flexible. They are not rigidly confined to broad trends, but can explore many potential relationships and "drill down" in the data to find specific causes of changes.
The estimate combines regular Medi-Cal spending with various programs outside of DHS (sometimes only portions of programs) that also flow through Medi-Cal, and it combines all funding sources in its trend presentations. Consequently, it is not possible, in many cases, to readily identify the General Fund impact of a cost trend or whether that trend results from regular Medi-Cal services or from ancillary programs operated by other departments.
Finally, the estimate treats Medi-Cal managed care, which now serves about half of all enrollees, as an afterthought. An estimate of managed care spending is added onto the fee-for-service estimate without presenting any meaningful information about caseload and rates for the managed care plans.
The Past is Forgotten. The estimate presents no actual spending figures for the past year. There is no update to the previous May Revision estimate to take account of developments after February (the cutoff for May Revision data). The department produces an Annual Statistical Report for Medi-Cal several years in arrears, but this report is for calendar years rather than fiscal years; on a cash basis, rather than the budget's accrual basis; and excludes most managed care data. As a result there are no actual spending trends for Medi-Cal, only trends of past May Revision estimates.
New Proposals Are Buried in the Estimate. The 1999-00 Medi-Cal estimate for benefit costs and county administration includes a total of 127 "policy changes." In reality, there are only a handful of new policy changes proposed in the Medi-Cal budget (the major ones being the federal funding assumptions). The other policy changes merely track the effects of past actions or external factors, such as regular changes in the federal funding percentage on the spending estimate. While the tracking information is useful, new proposals should be separated out to highlight them for the Legislature's consideration.
Linkages With Other Programs Not Addressed. The estimate does not include any analysis or discussion of developments and trends in other major programs that have substantial effects on Medi-Cal spending and services. These other programs include Medicare, county mental health systems, and programs for the developmentally disabled. Medi-Cal caseload estimates are not coordinated with welfare caseload estimates by DSS.
Basis for Estimates Often Not Given. The spending estimates presented in many of the policy changes are explained by a simple set of calculations using assumptions that are simply asserted. For example, the estimate includes $11.8 million due to the addition of the heart medication Coreg to the Medi-Cal formulary. This figure is based on 263,841 prescriptions at $89.70 each (with a phase-in period), but the policy change is silent as to the basis for these assumptions.
Baseline Estimate Should Be Made Available When Completed. The department completes work on the Medi-Cal estimate in November of each year, except for the addition of new policy proposals for the Governor's budget that still await administration decisions. However, none of the estimate is made available to the Legislature until January, when the budget is submitted. We see no reason why the basic estimate (absent new policy proposals) should not be provided to the Legislature as soon as it is done.
An Opportune Time for Change. There are two reasons why 1999-00 presents a particularly opportune time for change. First, revising the estimate will require focus and commitment by department leadership over a period of time. This perspective may be easier to take at the beginning of an incoming administration. Second, work is rapidly advancing on a major new Medi-Cal information system--the Management Information System/Decision Support System, which is expected to be operational this summer. This system, costing more than $40 million, is a modern database information system that should be able to provide the type of analytical power and flexibility needed to make the Medi-Cal estimate a much more useful tool for monitoring and evaluating the program.
Recommendation. For the reasons above, we believe that it is time to fundamentally revise the Medi-Cal estimate. Accordingly we recommend enactment of legislation directing DHS to restructure the estimate in the following ways:
We recognize that revising the approach for the Medi-Cal estimate is a significant task for the department, and that some additional temporary resources may be needed to accomplish it. If so, then we further recommend that the department identify and report on those needs at budget hearings.