Public Health |
The Department of Health Services (DHS) administers a broad range of public health programs. Some of these programs complement and support the activities of local health agencies in controlling environmental hazards, preventing and controlling disease, and providing health services to populations who have special needs. Other programs are solely state-operated programs such as those that license health facilities.
The Governor's budget proposes $1.9 billion (all funds) for public health local assistance. This represents a decrease of $98 million, or 4.9 percent, from estimated current-year expenditures. The budget proposes $341 million from the General Fund, which is an 11 percent decrease from estimated current-year expenditures. The main reason for this is the proposed elimination of General Fund support for the County Medical Services Program.
Proposition 99, the Tobacco Tax and Health Protection Act of 1988, established a 25-cent surtax on the sale of cigarette and tobacco products in California. The proposition requires that the revenues from the surtax be distributed to six accounts within the Cigarette and Tobacco Products Surtax Fund (C&T Fund) according to specified percentages, and further provides that expenditures from each account must be used for specific kinds of activities.
While Proposition 99 has long been a diminishing revenue source due to decreasing use of cigarettes, recent events are projected to result in a greater reduction in these revenues (see Figure 1, next page). Specifically:
| Figure 1 | ||
| Proposition 99 Revenues Declining | ||
| 1990-91 Through 1999-00
(Dollars in Millions) | ||
| Year | Revenues | Percent Change |
| 1990-91 | $539 | -- |
| 1991-92 | 518 | -3.9% |
| 1992-93 | 499 | -3.7 |
| 1993-94 | 473 | -5.2 |
| 1994-95 | 465 | -1.7 |
| 1995-96 | 462 | -0.6 |
| 1996-97 | 463 | 0.2 |
| 1997-98 | 450 | -2.8 |
| 1998-99 (est.) | 399 | -11.3 |
| 1999-00 (est.) | 390 a | -2.3 |
| a Includes $8.7 million transfer of Proposition 10 funds. | ||
After accounting for these impacts, the Governor's budget estimates that Proposition 99 revenues will decline by more than 11 percent in the current year and by 2.3 percent in 1999-00.
Due to sharp declines in Proposition 99 revenues resulting primarily from the effects of Proposition 10 and the tobacco lawsuit settlement, the budget proposes to reduce most programs that are supported by this fund source. However, funding for state programs that are caseload-driven would be maintained.
In response to the projected declines in Proposition 99 revenues, the budget proposes reductions in expenditures from the C&T Fund in the current and budget years for most of the programs that receive funding from Proposition 99 (see Figure 2). In general, reductions hit hardest in the budget year because the availability of carry-over balances from 1997-98 help support spending in the current year.
The Governor's budget proposes to reduce most programs on a pro-rated basis (within each C&T Fund account), while maintaining funding for caseload-driven programs that might otherwise be supported by the General Fund--specifically the Major Risk Medical Insurance Program, the Access for Infants and Mothers program, the Child Health and Disability Prevention program, and the Breast Cancer Early Detection Program.
In considering the Proposition 99 reductions, the Legislature should keep the following in mind. When Proposition 99 was enacted, it was anticipated that it would be a diminishing revenue source for a number of reasons, including the effects of the antismoking components of the measure itself. The sharp revenue reductions that are expected to result from the combined effects of Proposition 10 and the tobacco lawsuit settlement underscore the continuing problems associated with using this revenue source for ongoing programs.
As Figure 2 (see next page) shows, the Proposition 99 revenue losses lead to significant reductions in a variety of programs, including primary care clinics and other indigent health care activities. Because county health programs receive a large share of Proposition 99 revenues, they would be subject to significant reductions under the budget proposal. While the counties would lose a significant amount of revenues, Proposition 99 is not the main source of funds for county indigent health care. We estimate that this source accounts for roughly 10 percent to 15 percent of the total expenditures for this purpose--although this could vary significantly among the individual counties.
| Figure 2 | ||||
| Proposition 99 Expenditures
Cigarette and Tobacco Products Surtax Fund | ||||
| 1997-98 Through 1999-00
(Dollars in Thousands) | ||||
| Departments/Programs | Actual 1997-98 | Estimated 1998-99 | Proposed 1999-00 | Percent Change From 1998-99 |
| Department of Health Services | ||||
| Chronic Diseases/Smoking Prevention | ||||
| Breast Cancer Early Detection | -- | -- | $13,541 | N/A |
| Media Campaign | $31,224 | $24,503 | 18,848 | -23% |
| Competitive Grants | 27,258 | 34,780 | 17,000 | -51 |
| Committee and Evaluation | 3,509 | 5,433 | 4,309 | -20 |
| Local Lead Agencies | 33,092 | 22,101 | 16,744 | -24 |
| Primary Care and Family Health | ||||
| Clinic Grants | $17,764 | $13,419 | $8,000 | -40% |
| Comprehensive Perinatal Outreach | 4,796 | 3,162 | 1,892 | -40 |
| Child Health and Disability Prevention | 47,878 | 47,490 | 52,908 | 11 |
| Children's Hospitals | 1,078 | 990 | 543 | -45 |
| County Health Services | ||||
| Managed Care Counties | $2,551 | $2,343 | $1,294 | -45% |
| County Medical Services Program Expansion | 12,107 | 9,983 | 6,175 | -38 |
| California Healthcare for Indigents | 161,041 | 146,387 | 88,087 | -40 |
| Rural Health Services | 2,779 | 4,306 | 2,486 | -42 |
| State Administration | 6,180 | 6,874 | 3,549 | -48 |
| Managed Risk Medical Insurance Board | ||||
| Major Risk Medical Insurance Program | $35,021 | $40,094 | $40,820 | 2% |
| Access for Infants and Mothers | 39,914 | 34,649 | 38,098 | 10 |
| Office of Statewide Health Planning and Development | $1,899 | $1,837 | $1,736 | -5 % |
| University of California | $16,095 | $84,431 | $28,991 | -66% |
| Department of Education | $45,746 | $33,311 | $26,910 | -19% |
| Resources programsa | $33,896 | $34,233 | $28,315 | -23% |
| State Board of Equalization | $1,263 | $1,191 | $1,211 | 2% |
| Pro rata charges | $921 | $1,497 | $1,822 | 22% |
| Totals | $526,012 | $553,014 | $403,279 | -27% |
| a Includes transfers to Habitat Conservation Fund and Natural Resources Infrastructure Fund. | ||||
Also, the counties have the option of allocating their tobacco lawsuit settlement funds in 1999-00 to help compensate for the Proposition 99 reductions. Finally, we note that anticipated enrollment growth in the Healthy Families Program, as well as potential health coverage expansions contemplated in the budget (discussed in our analysis of the Health and Human Services Agency) could reduce some of the cost pressures on county indigent health programs.
Whether these revenue reductions should be backfilled, in whole or in part, by the state is an issue for the Legislature when balancing its competing policy interests. We would note, however, given the historical declines in this funding source, that the Legislature is likely to face similar funding pressures in the future from programs primarily supported by this revenue source.
The Governor's budget proposes to eliminate the state's General Fund allocation of $20.2 million to the County Medical Services Program. We comment on the proposal and present some options for the Legislature.
Background. The County Medical Services Program (CMSP) was established in 1983 to provide medical and dental care to low income "medically indigent adults" (MIAs) who are not eligible for the state's Medi-Cal Program and who reside in small counties (see Figure 3, next page, for participating counties). The CMSP governing board, comprised of ten county officials, is responsible for the administration of pooled funds from 34 counties to provide services to approximately 40,000 CMSP clients at an estimated cost of $182 million in 1997-98. The governing board sets eligibility requirements, benefit levels, and provider reimbursement rates, but contracts with the DHS to administer a program offering uniform benefits and to provide claims processing functions.
| Figure 3 | |||
| Counties Participating in the
County Medical Services Program | |||
| 1998-99 | |||
| Alpine | Mendocino | ||
| Amador | Modoc | ||
| Butte | Mono | ||
| Calaveras | Napa | ||
| Colusa | Nevada | ||
| Del Norte | Plumas | ||
| El Dorado | San Benito | ||
| Glenn | Shasta | ||
| Humboldt | Sierra | ||
| Imperial | Siskiyou | ||
| Inyo | Solano | ||
| Kings | Sonoma | ||
| Lake | Sutter | ||
| Lassen | Tehama | ||
| Madera | Trinity | ||
| Marin | Tuolumne | ||
| Mariposa | Yuba | ||
History Behind General Fund Contribution. Prior to 1983, the MIA population was eligible for Medi-Cal coverage. However, in response to the state's budget problems, this population was transferred from the Medi-Cal Program to the counties who were made responsible for their health services. Small counties, with populations of 300,000 or less, were permitted to contract with the state for administration of their programs, and this became known as the CMSP. Thirty-four counties initially chose the option. The counties adopted uniform eligibility criteria and benefits similar to the Medi-Cal Program. Initially, the state allocated $23.2 million to the program for health care services, which was 30 percent less than the estimated amount that would have been spent for services under the Medi-Cal Program. Until 1992-93, the state bore the risk for CMSP cost increases above specified revenue amounts.
Legislation was enacted in 1992 to cap the General Fund responsibility for CMSP at $20.2 million, which was the estimated amount needed for the program in 1991-92.
The CMSP Fund Sources. Funding for CMSP includes realignment revenues (from the 1991-92 realignment legislation), Proposition 99 revenues, county funds (participation fees), hospital settlements (audit recoveries for overpayments to hospitals), and the state General Fund. Figure 4 displays the program's 1997-98 revenues.
| Figure 4 | ||
| County Medical Services Program
Estimated Revenues | ||
| 1997-98
(Dollars in Thousands) | ||
| Source | Amount | Percentage of Total |
| Realignment | $110,749 | 61% |
| Hospital settlements | 27,929 | 15 |
| General Fund | 20,237 | 11 |
| Proposition 99 | 12,514 | 7 |
| County participation fees | 5,459 | 3 |
| Interest | 4,000 | 2 |
| Third party payers | 2,083 | 1 |
| Unclaimed warrants | 8 | -- |
| Totals | $182,979 | 100% |
Governor's Proposal. The Governor's budget proposes trailer bill legislation to eliminate the state's appropriation of $20.2 million from the General Fund to CMSP. The budget indicates that (1) CMSP has substantial fund reserves in its local program account and (2) the counties can reduce costs if necessary.
The CMSP Account Fund Balance. At the end of 1997-98, the most recent year in which its fund condition statement is complete, the CMSP Account showed a balance of $102 million. Of this amount, $10.5 million was allocated for legal costs associated with a pending lawsuit. While the board has not updated its fund condition through 1999-00, we estimate that without the General Fund allocation, the fund will have sufficient resources to support the program for two years beyond the budget year.
Potential Expenditure Reductions. As noted above, the budget indicates that, if necessary, the counties can address revenue shortfalls by reducing expenditures. Such reductions could come in the form of program efficiencies, although the budget does not identify any specific means of achieving savings in this manner. Another way to reduce costs would be to make program changes such as tightening eligibility requirements, limiting benefits, or reducing provider reimbursement rates. These options, however, either directly affect the level of services provided or, in the case of the reimbursement rates, could lead to a reduction in the number of providers which, in turn, could adversely affect patient access to services.
Options. The board should be prepared to discuss potential expenditure reductions during the hearings. As we indicated, the most obvious means of reducing expenditures generally run the risk of adversely affecting patient access to health services. Thus, the Legislature may wish to consider other options in addition to the budget proposal. One possibility would be to adopt the budget proposal only as a one- or two-year reduction. Based on the current trend, however, the board would still need to reduce expenditures at some point in the future.
We presented another option for CMSP in the Analysis of the 1993-94 Budget Bill, when the program was facing potential revenue shortfalls. We raised the possibility of restricting the program to the smallest counties, where the need for state assistance is the greatest, and thereby requiring the larger CMSP counties to operate as independent counties or form consortia with other counties.
Finally, with respect to the larger issue of how indigent health care services should be provided, we note that in our report on state/local restructuring (Making Government Make Sense, in the 1993-94 Perspectives and Issues), we indicated that the state should adopt a more uniform policy for providing indigent health care, and recommended that the state assume responsibility for this function.
Federal funds for the AIDS Drug Assistance Program (ADAP) will be $5 million above the amount assumed in the budget. These additional federal funds can be used to reduce General Fund support for the program, but the General Fund savings may need to be redirected to other HIV-related activities in order to meet the federal maintenance-of-effort (MOE) requirement for future federal grants. We recommend that the department develop a projection of state spending that would count toward the MOE requirement in 1999-00 in order to assess the potential for General Fund reductions.
Program Description and Budget Proposal. The ADAP provides AIDS drugs to HIV-infected persons with (1) incomes below 400 percent of the poverty level, (2) valid prescriptions from a California licensed physician, and (3) no coverage under Medi-Cal or other insurance. Persons with incomes between 400 percent of poverty ($31,560 for one individual) and $50,000 may also receive drugs through ADAP at a share of cost. The budget proposes $136.6 million ($47.5 million General Fund) for ADAP in 1999-00, which is expected to fully fund caseload and costs. This is an increase of 12 percent in total funds, but a decrease of 8 percent ($4.1 million) from the General Fund. The General Fund reduction is the result of an increase in federal funds.
The ADAP's Federal Funding. The ADAP receives its federal funding under Title II of the Ryan White Comprehensive AIDS Resources Emergency (CARE) Act, which is administered by the Health Resources and Services Administration (HRSA) in the U.S. Department of Health and Human Services.
Title II of the act authorizes grants to states to provide health care and support services for people with HIV, and consists of both a base grant and supplemental grant. While the Title II base grant can be used for a variety of services, the supplemental grant solely supports the state's ADAP program. California's Title II base grant for the budget year is expected to increase only slightly, to $30.7 million, but ADAP's supplemental grant will increase significantly from its current-year amount of $43.1 million. In fact, the Governor's budget estimates that the state will receive $60.3 million in federal supplemental funds in 1999-00. Final confirmation of California's share of the next annual grant will not be received until HRSA sends out Notice of Grant Award letters in March 1999.
Subsequent to publication of the budget, HRSA has informed the state that, although the figure will not be made official until the release of the award letter, the state is scheduled to receive $65.3 million, or $5 million more than estimated in the budget.
State MOE Requirement. Federal law includes a state MOE requirement to receive Title II funds. States must maintain nonfederal HIV/ AIDS-related spending levels (which can include the state share of related Medicaid costs) that are at least equal to that of the prior year. According to HRSA staff, a state that fails to meet this requirement forfeits receipt of its entire Title II grant.
The DHS estimates that the state will meet the MOE requirement for the 1999-00 federal grant, which is based on 1997-98 state expenditures compared to 1996-97. It is important, however, to maintain the level of state spending to qualify for future federal grants. In this respect, the Department of Finance indicates that HIV-related Medi-Cal costs are expected to increase by an amount sufficient to offset the proposed $4.1 million reduction in General Fund support for ADAP in the budget year, for purposes of meeting the MOE requirement. We note, however, that DHS has not developed an estimate of the HIV-related costs within the Medi-Cal Program for the budget year.
The DHS Should Develop Projections. Estimates of MOE-countable state spending in the budget year are needed, not only to provide some assurance that the proposed General Fund reduction will not lead to a violation of the requirement but to determine whether the anticipated increase of $5 million in federal funds can be used to achieve additional General Fund savings. Consequently, we recommend that the department provide the estimate to the Legislature prior to budget hearings.
Options for the Legislature. As noted above, the budget proposal for ADAP is based on the assumption that program caseloads and costs will be fully funded. Consequently, the additional $5 million in federal funds could be used to offset proposed General Fund spending in the program. These General Fund savings, however, may need to be redirected to other HIV-related activities in 1999-00--such as the Early Intervention Program--in order to meet the MOE requirement for future federal grants (specifically for 2001-02). An alternative under this scenario would be to maintain the level of General Fund support proposed for ADAP and carry the additional federal funds over to 2000-01, although this would be subject to approval by the federal administration.
The budget proposes to extend the Community Challenge Grant Program for one additional year. We recommend adoption of budget bill language to require the department to revise its grant guidelines to award only tested program designs, similar to the model used by the State Department of Education for its teen pregnancy prevention program.
Program Description and Budget Proposal. The Community Challenge Grant Program (CCGP) was established in 1996-97 to support local community projects to reduce teen pregnancy. Since 1996-97, the Legislature has appropriated $20 million from the General Fund annually to the DHS for competitive grant awards under the CCGP.
Under current law, the program sunsets on June 30, 1999. The budget proposes to extend the program for one additional year and to continue funding it at $20 million in 1999-00. The budget indicates that funding is contingent on savings that would be achieved under another budget proposal that would, if approved by the federal administration, result in federal funding for the state-only family planning program within the Medi-Cal Program.
Background. To provide background, Figure 5 contains a brief description of state-supported programs whose primary focus is teen pregnancy prevention.
| Figure 5 | ||
| State-Supported Teen Pregnancy Prevention Programs | ||
| 1998-99
(In Thousands) | ||
| Agency/Program | Program Description | General Fund Expenditures |
| Department of Health Services | ||
| Community Challenge Grant Program | Competitive awards to local organizations | $20,000 |
| Male Involvement Program | Local projects that focus on male's role in teen pregnancy prevention | 2,507 |
| Information and Education Program | Local family life health education projects in schools and community settings | 3,260 |
| Adolescent Sibling Pregnancy Prevention Program | Case management for "at-risk" siblings of parenting teens | 3,000 |
| State Department of Education | ||
| Teen Pregnancy Prevention Grant Program | Competitive awards to local educational agencies | $10,000 |
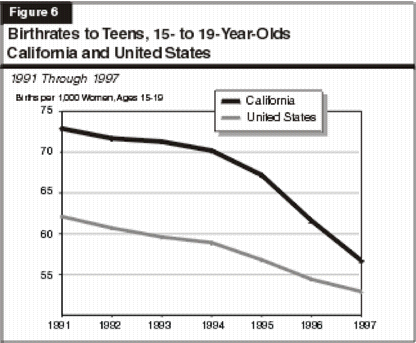
Figure 6 (see next page) illustrates that the teen birthrate has been declining in California and the U.S. in recent years. Between 1991 and 1997, California's teen birthrate declined 22 percent, compared to an average national decline of 14.8 percent. Although California's decline in teen birthrates has out-paced the nation's, the state's rate still exceeds the national average. In 1997, California had 56.7 live births per 1,000 15- to 19-year-old women, while the national rate was 52.9. This may be due, in part, to demographic differences between California and other states.

Department Late in Submitting CCGP Evaluation. The CCGP's authorizing legislation--Chapter 197, Statutes of 1996 (AB 3483, Friedman)-- requires that the department "conduct a statewide independent evaluation of the program" and submit its findings to the Legislature on or before January 1, 1999. To meet the requirement, the department contracted with an independent evaluator, who submitted an interim report to the department in January, essentially describing the implementation of program components. The final evaluation, however, will not be submitted until December 1999.
Recommend Improvements in DHS Grant Proposal Guidelines. The three-year cycle for existing grants ends in the current year. The department plans to initiate a request for new proposals, subject to the availability of funding in the budget act.
We recommend that the DHS model its selection criteria for all new grants after the State Department of Education's (SDE's) Teen Pregnancy Prevention Grant Program. In its 1996 award process, SDE provided applicants with a "menu" of tested program designs upon which to base their grant proposals. The SDE researched and identified program designs that had been proven effective in delaying the onset of sexual activity and reducing the incidence of teenage pregnancy. We believe that funding such grant proposals increases the probability of cost-effectiveness.
Our recommendation can be implemented by adoption of the following language in Item 4260-001-0001:
In awarding grants for the Community Challenge Grant Program, the department shall use criteria to encourage projects based on research and tested program designs, similar to the guidelines used in the State Department of Education's Teen Pregnancy Prevention Grant Program.
We recommend that the year-end unexpended balances in the Cancer Research Fund (projected to be $1.6 million) be transferred to the General Fund because (1) these balances will not be needed to fund the program in 1999-00 and (2) the original source of these funds is the General Fund. (Increase General Fund revenues by $1,555,000.)
The Cancer Research Fund was created by Chapter 755, Statutes of 1997 (AB 1554, Ortiz) to support cancer research. The department administers the Cancer Research Program by contracting with research entities such as the University of California, nonprofit organizations, and foundations. Chapter 755 appropriated $2 million from the General Fund to the Cancer Research Fund in 1997-98 and indicated the intent of the Legislature to appropriate $25 million the following year. The fund received the $25 million from the General Fund in the 1998-99 Budget Act, and the Governor's budget proposes another General Fund transfer of $25 million for 1999-00.
About $1.6 million of the initial $2 million was not expended in 1997-98, and this balance has essentially rolled forward annually to 1999-00. Given that (1) the source of the funds for the Cancer Research Fund is the General Fund and (2) program expenditure requirements are limited to the amount of the budget act appropriation, we see no reason to leave the unexpended balances in the special fund. Moreover, adoption of this recommendation would not impact anticipated expenditures as proposed in the budget. Consequently, we recommend adoption of the following budget bill language (in Item 4260-001-0589) to transfer year-end balances to the General Fund, which would result in an estimated increase of $1.6 million in General Fund revenues:
All unexpended balances in the Cancer Research Fund, as of June 30, 2000, shall be transferred to the General Fund.
We recommend increasing the General Fund amount budgeted for transfer to the Safe Drinking Water State Revolving Fund by $285,000 in order to obtain all available federal funds from the federal fiscal year 1998 grant (an additional $1.4 million). We also recommend that the department report at budget hearings on the advisability of expediting the receipt of additional federal funds available for federal fiscal year 1999. (Increase Item 4260-111-0001 by $285,000 and increase Item 4260-111-0890 by $1,408,000.)
Background. The department maintains the Safe Drinking Water State Revolving Fund to assist public water systems in financing the costs of infrastructure to comply with the requirements of the federal Safe Drinking Water Act. Federal funds are received from the U.S. Environmental Protection Agency (EPA), which provides capitalization grants to states according to a need-based formula.
State Match Requirements. Federal law requires that states match 20 percent of the federal funds. States must appropriate the match no later than the end of the following federal fiscal year (FFY). For example, in order for a state to draw down federal funds from FFY 1998 (October 1997 through September 1998), the 20 percent match must be appropriated by September 30, 1999. The state then has until September 30, 2000 to obligate the funds to local water projects.
Available Federal Funds. By appropriating $15.1 million from the General Fund in the 1998-99 Budget Act, the state received its first federal grant of $75.7 million from FFY 97. Currently, both the FFY 98 federal award of $77.1 million and the FFY 99 federal award of $82.4 million are available for California's use to the extent that the state provides the matching funds.
Budget Proposal. The budget proposes to maintain current-year expenditures of $15.1 million from the General Fund in the budget year in order to draw down $75.7 million in FFY 98 federal grants.
Under this proposal, the state will not receive the balance of the FFY 98 federal award--$1.4 million. We note that according to the EPA, upgrading the state's local public water systems to meet current and anticipated federal regulations will cost $18 billion. Thus, it is apparent that there is a need for additional funds in this program. Accordingly, we recommend augmenting the budget by $285,000 from the General Fund, which is the match needed to obtain the full FFY 1998 grant.
The FFY 99 Funds Also Available. Although the state has until September 30, 2000 to draw down any part or all of the FFY 99 federal grant award, it also has the option to appropriate the state match and thereby acquire these additional federal funds in the budget year. Consequently, we recommend that the department report at budget hearings on the advisability of expediting the receipt of these funds, the ability of the local systems to "ramp up" their spending, and how this would affect these programs in subsequent years. The Legislature, of course, will also have to weigh these factors against the competing demands for state funds in the budget year.
The Managed Risk Medical Insurance Board (MRMIB) administers several programs designed to provide health care coverage to adults and children.
The Major Risk Medical Insurance Program provides health insurance to California residents unable to obtain it for themselves or their families because
of preexisting medical conditions. The Access for Infants and Mothers program provides coverage for women seeking pregnancy-related and neonatal
medical care and whose family incomes are between 200 percent and 300 percent of the federal poverty level. The Healthy Families Program provides
health coverage for uninsured children in families with incomes up to 200 percent of the federal poverty level and not eligible for Medi-Cal. The MRMIB
also contracts for the administration of the Health Insurance Plan of California, which operates an insurance purchasing pool for small employers. The budget proposes $288.7 million from all funds for support of MRMIB programs in 1999-00, which is an increase of 88 percent over estimated
current-year expenditures. This is due primarily to an increase of $91 million in federal funds and $46 million from the General Fund for caseload growth
in the Healthy Families Program. The Healthy Families Program implements the federal Children's Health Insurance Program enacted in 1997. Funding for California generally is on a
2-to-1 federal/state matching basis. Families pay a relatively low monthly premium and can choose from a selection of managed care plans for their
children. Coverage is similar to that offered to state employees and includes dental and vision benefits. The program began enrolling children in July
1998. The Budget Proposal. The Governor proposes $210 million ($71.3 million General Fund) in MRMIB's budget for the Healthy Families Program in
1999-00, which is an increase of about 220 percent over estimated current-year expenditures. After accounting for program expenditures (outreach and
related Medi-Cal expansion) in the Department of Health Services (DHS) and related expenditures in other departments, the budget proposes $323 million
($104.7 million General Fund) for the Healthy Families Program, which is an increase of 146 percent over the current year. The proposed increase is due
primarily to an expected 133 percent increase in caseload in the budget year. We note that the budget does not include funding for provider rate increases
in 1999-00. The rate increases will be negotiated in February and will be included in the May Revision of the budget. The budget projects that enrollment
will increase to 138,000 by the end of the current year and 321,100 by the end of the budget year. To address lower-than-expected enrollment in the Healthy Families Program, the Managed Risk Medical Insurance Board and the Department of
Health Services shortened the application form and prepared fact sheets on immigration status. Enrollment in the Healthy Families Program was initially much lower than anticipated. It is also significantly below the revised estimates by the
University of California at Los Angeles Center for Health Policy Research that 400,000 children are eligible for the program. In order to increase
enrollment, the Legislature appropriated additional funds in the current year for outreach activities. In addition, MRMIB and DHS made certain
administrative changes to the program, including the following. Application Simplified. A new Healthy Families Program application is due to be released in March that reduces the original 28-page booklet to 7 pages.
Under the original application procedures, families had to calculate their monthly income, complete financial worksheets, ascertain which programs their
children were eligible for--Healthy Families, no-cost Medi-Cal, or share-of-cost Medi-Cal--and then mail in their forms to either Medi-Cal or Healthy
Families (or both) to be processed. With the new application, families will send their information to an organization that will determine their eligibility. If
families wish, they can still calculate their income, complete a supplemental application, and send it directly to the Healthy Families Program for
processing. Immigration Fact Sheets--the "Public Charge" Issue. Also by March, MRMIB and DHS intend to disseminate two fact sheets about Medi-Cal and
Healthy Families to address concerns regarding an immigration-related issue known as "public charge." Public charge is a term used by the Immigration and Naturalization Service (INS) to describe persons who are likely to depend on public benefits.
Depending on immigration status, the INS can refuse to allow immigrants to enter the U.S., reenter, or become permanent residents if it determines that
they are likely to rely on public benefits in the future. Also, if a citizen or permanent resident wants to sponsor a family member who wishes to immigrate,
past or current receipt of public benefits may jeopardize his or her ability to be a sponsor. This has led to concern as to whether immigrant parents will be considered "public charges" if their children enroll in the Healthy Families Program.
Because of these concerns, and their potential effect on program enrollment, the state administration requested clarification from the INS on its policy. In
an "interim" response, INS stated that "receipt of benefits by a child--either U.S. citizen or an alien--is not attributed to the alien parent or other family
members for public charge purposes. The only time this general rule would not apply would be if the family were reliant on the child's benefits as its sole
means of support." Based on this letter, MRMIB and DHS plan to release public charge fact sheets to local communities. Actual enrollments for the Healthy Families Program in October 1998 through December 1998 are about 5 percent lower than the budget estimates.
The administration will submit revised estimates for the current and budget years in the May Revision of the budget. After reviewing three months of actual enrollment data (October 1998 through December 1998) that were not available to MRMIB when the budget was
prepared, we find that enrollments during this period are, on average, 5.3 percent lower than estimated in the budget. If this trend were to continue, the
resulting General Fund savings would be about $845,000 in the current year. The impact of the revised application form and the immigration fact sheets,
however, could bring enrollments closer to the budget projection. The administration will update their projections in the May Revision of the budget. The budget proposes a $2.7 million General Fund set-aside to reflect the impact of applying the Medi-Cal income deductions to the Healthy Families
Program for purposes of determining eligibility. Funding the proposal is contingent on savings from another budget proposal to secure federal
funding of the state-only family planning program. Budget Proposal. The budget proposes a set-aside of $2.7 million from the General Fund (and $5.3 million in matching federal funds) to expand the
Healthy Families Program by applying Medi-Cal income deductions when determining eligibility. This is part of a $40 million set-aside, of which
$37.3 million is for health care reforms, pursuant to a plan to be developed by the Secretary of the Health and Human Services Agency (discussed in our
analysis of the agency's budget). The budget indicates that funding for this set-aside is contingent on savings that would be achieved under another budget
proposal that would, if approved by the federal administration, result in federal funding for the state-only family planning program within the Medi-Cal
Program. Expansion Via Income Deductions. The proposed Healthy Families Program expansion would apply Medi-Cal income deductions--such as those for
work expenses, child and dependent care, and court-ordered alimony/spousal and child support--to applicants' gross income levels when determining
program eligibility. This would expand eligibility for families with incomes above 200 percent of the poverty level if the allowable income deductions
bring their net income level to 200 percent of the federal poverty level or below. The MRMIB estimates that this will expand enrollment by 17,500
children in the budget year. By using the same income deductions as the Medi-Cal Program, this proposal would result in administrative efficiencies and avoid confusion on the part
of applicants (some of whom will have children enrolled in both the Medi-Cal and Healthy Families Programs). Thus, from an administrative perspective,
this proposal has merit. With respect to the broader issue of eligibility expansion for the Healthy Families Program, we note that the budget includes such
expansion as one of the options to be considered by the Secretary of the state Health and Human Services Agency. (For a discussion of this and other
options, please see our analysis of the agency's budget.) A developmental disability is defined as a disability, related to certain mental or neurological impairments, that originates before a person's eighteenth
birthday, constitutes a substantial handicap, and is expected to continue indefinitely. The Lanterman Developmental Disabilities Services Act of 1969
entitles individuals with developmental disabilities to receive a variety of services, which are overseen by the state Department of Developmental Services
(DDS). The department contracts with 21 nonprofit regional centers (RCs) to coordinate educational, vocational, and residential services for
approximately 140,000 clients each year. In addition to providing some services directly, such as diagnosis and case management, RCs purchase a variety
of services from providers in the community. Individuals with developmental disabilities have a number of residential options. While most live with their parents or other relatives, thousands live in
their own apartments, with roommates, or in group homes that are designed to meet their medical and behavioral needs. An additional 4,000 live in
state-run developmental centers (DCs). The budget proposes $2.1 billion from all funds for support of DDS programs in 1999-00, an increase of 11 percent over estimated current-year
expenditures. The budget proposes $836 million from the General Fund, which is $118 million, or 16 percent, above estimated current-year expenditures
from this funding source. The increase is primarily due to (1) caseload and cost increases for community-based services and (2) the full-year cost of
program augmentations enacted in the current year. The DDS Community Services Program provides community-based services to clients through the RCs. These services include assessment and diagnosis
of children and adults, early intervention services for young children, placement in residential care facilities and daytime treatment/activity programs,
arrangements for transportation when needed, and family supports such as respite care and counseling. We recommend enactment of legislation requiring the department, along with regional centers and area boards, to incorporate the following issues
into the self-determination pilot projects authorized by Chapter 1043, Statutes of 1998 (SB 1038, Thompson): (1) the extent to which consumer choice
should be limited, (2) how "life quality" assessments can be used to enhance the service planning process, (3) whether case management services can
be provided outside the traditional regional center model in a cost-effective manner, and (4) how to incorporate objective performance measures into
a format that consumers can use to make informed choices about the services they receive. The idea of "self-determination,"--in which developmentally disabled consumers determine which services they need and directly control the funds that
are used to purchase those services--has gained some popularity nationwide in the past few years. In this analysis of the self-determination approach, we
commonly refer to consumers as the decision makers. We note, however, that in many cases a consumer's family, legal guardian, or conservator would
also be involved. We also use the terms "consumer" and "client" interchangeably. New Hampshire Project Considered Successful. The trend toward self-determination was spurred by the Monadnock Project in New Hampshire, which
was started in 1992 using a Robert Wood Johnson Foundation (RWJF) grant. Consumers involved in the project controlled the planning process for all of
their needs and purchased services through a variety of methods, including contracting directly with providers. The consumers were initially given
85 percent of their existing service expenditures, including federal and state funds, and were allowed to purchase services as they wished. The remainder
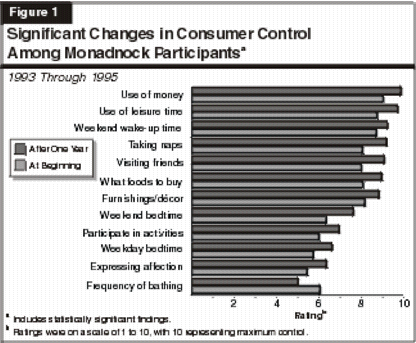
was put into a "risk pool" as a safeguard in case participants needed additional funds. An external evaluation of the project found that Monadnock participants had more control over their daily lives, yet spent 12 percent to 15 percent less on
average than before the project was implemented. The evaluators measured the amount of control participants felt they had over a number of lifestyle
decisions, ranging from control over personal finances, leisure time, and living arrangements to choosing restaurants, clothing, and bedtimes. They found
statistically significant increases in consumer control for 11 of the 26 outcome measures and a significant decrease in only one of the measures (the
researchers did not attempt to explain this decrease). Figure 1 shows the significant changes that were identified. The researchers also asked participants to
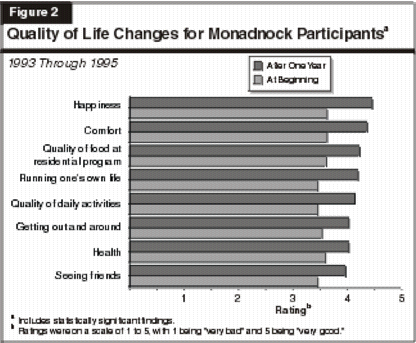
rate the quality of their lives based on a number of factors, such as general health and happiness, relationships with family and friends, and their living
situations. Results were again positive, as shown in Figure 2 (see next page). The above measures are subjective, measuring consumers' perceptions of their life quality and the amount of control they exercised over daily activities.
The evaluators also included more objective measures such as the frequency of outings to visit friends, shop, see movies, and go to church. They reported
an increase in the number of times participants engaged in these activities, although it was not statistically significant. The Monadnock evaluation has several limitations. The researchers did not include a comparison group, which limits the conclusions that can be drawn
from their findings. In addition, incomplete data forced them to estimate some costs associated with client services. Finally, because every
self-determination project is unique, the Monadnock findings may not be generalizable. Despite these limitations, the Monadnock project--which by design provided consumers with more control and less funding--indicates that the concept of
self-determination holds promise for states wishing to increase consumer choice while decreasing system costs. We note that further research might help
to establish a causal relationship between consumer control and life quality, as measured by outcome indicators such as health status. Additional Projects Underway. After the Monadnock success, RWJF funded additional projects in 29 states, which will be evaluated to determine the
effectiveness and cost-effectiveness of different self-determination models. The models being tested include changes in the way that needed services are
identified and provided as well as the use of vouchers, debit cards, and cash grants controlled by consumers. California did not receive a grant from the
foundation, although a second round of funding might become available for which the state could apply. The project director indicates that external
evaluations of each project have been initiated, although results will not be published for at least another year. California Projects May Test Variety of Models. In California, Chapter 1043, Statutes of 1998 (SB 1038, Thompson) provides $750,000 over three years
for pilot projects assessing the effectiveness of different self-determination models. The department is working with the Tri-Counties, Eastern Los
Angeles, and Redwood Coast RCs and their local area boards to structure the projects. California's projects offer an opportunity to examine the
cost-effectiveness of various aspects of self-determination. Specifically, SB 1038 authorizes a number of options, such as: While it remains to be seen which of these options are chosen by the participating RCs, we believe that alternative case management should be included
among the models tested. (We discuss this later in our analysis.) We also suggest that each project be evaluated. These evaluations should include
comparison groups; an analysis of cost-effectiveness; and attention to the advantages, drawbacks, and difficulties encountered while implementing the
various options. In addition, the evaluation should measure several different types of outcomes, recognizing that consumer perceptions of life quality and
the amount of control they feel they have over their lives is one way to measure project success, but that more objective measures such as health and
safety, living arrangements, employment, and the achievement of goals set forth in each consumer's program plan should also be included. Additional Unanswered Questions. While the Monadnock Project results suggest that consumer choice can be increased even with a lower level of
funding, it is unclear whether increasing consumer choice is always cost-effective. In addition to testing some or all of the options listed above, we believe
that the department and participating RCs and area boards should incorporate into the SB 1038 pilot projects several additional questions related to the
cost-effectiveness of increasing consumer choice. These questions include: Conclusion. In summary, we believe that the self-determination concept holds promise as a way to increase consumer control over services and funding
while potentially reducing costs, but that further evaluation is needed to determine which aspects of self-determination are the most cost-effective, produce
the best outcomes, and are the most feasible to implement statewide. We also believe that California's self-determination projects provide an opportunity
to accomplish this and to answer several related questions regarding current system practices, including the use of RC purchase-of-service guidelines and
the incorporation of life quality assessment findings into the planning process. Accordingly, we recommend enactment of budget trailer bill legislation requiring the department, along with participating RCs and area boards, to
incorporate the following issues into the self-determination pilot projects authorized by SB 1038: (1) the extent to which consumer choice should be
limited, (2) how life quality assessments can be used to enhance the service planning process, (3) whether case management services can be provided
outside the traditional RC model in a cost-effective manner, and (4) how to incorporate objective performance measures into a format that consumers can
use to make informed choices about the services they receive. Where appropriate, the department should include its findings in the self-determination pilot
project report that is required to be submitted to the Legislature by January 1, 2001. We recommend a reduction of $2 million in General Fund expenditures from the regional center budget and a corresponding increase in
expenditures from the Program Development Fund, which contains a projected $2 million surplus. (Reduce Item 4300-101-0001 by $2,000,000 and
increase Item 4300-101-0172 by $2,000,000.) The Developmental Disabilities Program Development Fund (PDF) primarily contains fees collected from parents whose children receive services
through the RCs. According to state law, the fund may be used to expand community-based programs for people with developmental disabilities and to
offset General Fund costs. The 1999-00 Governor's Budget shows a year-end surplus of $2 million in the PDF beginning in 1997-98 and continuing through 1999-00. The
department indicates that, for several years, it did not fully account for PDF revenues, and by the time the error was discovered, a reserve of nearly
$2 million had accumulated. This unanticipated increase in available funds was not spent in 1997-98 and is not proposed to be spent in 1998-99 or
1999-00. The budget proposes additional General Fund expenditures for numerous programs that fit the intended purpose of the PDF. Given that the budget fully
funds caseload and cost increases, we recommend that the Legislature reduce the General Fund allocation for RCs by $2 million on a one-time basis, and
increase PDF expenditures by the same amount. The budget proposes $490 million from all funds ($39 million from the General Fund) for support of the DCs in 1999-00. We recommend a technical adjustment to reflect the full budget-year savings from closing the program for patients with developmental disabilities at
Napa State Hospital, for a General Fund savings of $116,000. (Reduce Item 4300-003-0001 by $14,000, Item 4260-101-0001 by $102,000, and Item
4260-101-0890 by $109,000.) Prior to its closure in February 1996, the Stockton Developmental Center housed a number of developmentally disabled residents who required an
increased level of security. At the end of 1995, 178 of these residents were moved to Napa State Hospital, one of the four mental hospitals operated by the
Department of Mental Health (DMH), which had bed space available at the time. The two departments entered into an interagency agreement requiring
DDS to reimburse DMH for the costs of housing and treating DDS clients. Since 1995, the number of DDS-funded beds at Napa has declined steadily. In
1998-99, 115 beds are dedicated to DDS clients at a cost of $18 million ($10 million from the General Fund). The DDS clients at Napa live in buildings that are located behind the newly constructed security fence. However, DMH indicates that it needs these
buildings in order to accommodate projected increases in the number of its patients who require secured facilities. The two departments have agreed to
phase out the DDS program by March 30, 2000. By that time, all of the DDS clients at Napa will be transferred to the developmental centers at Porterville
and Lanterman, where secured units have been built since Stockton DC was closed. The DMH budget includes a net decrease of $5.3 million in reimbursements from DDS, reflecting the planned phase-out of the program. However, the
DDS budget was reduced by only $5.1 million (total funds), which the department indicates is an error. Accordingly, we recommend a technical
adjustment to the DDS budget to reflect the full savings that will result from the program closure in 1999-00, for a General Fund savings of $116,000
($14,000 in the DDS budget and $102,000 in the Department of Health Services.). We recommend that the department report at budget hearings on (1) the status of its negotiations with the Health Care Financing Administration
regarding the continuing freeze on new admissions to the state's Home and Community Based Services federal waiver program, (2) its plan for
enabling regional centers to enroll new clients in the program, and (3) the projected loss of federal reimbursements in 1999-00 if the admissions
freeze is not completely lifted by July 1, 1999, as assumed in the budget. The Home and Community Based Services (HCBS) waiver program enables states to receive federal Medicaid funding for services provided to
developmentally disabled persons in community settings. Recipients are Medicaid beneficiaries who have conditions that would require institutional care
in the absence of community-based services. The waiver is based on the belief that community care is preferable to institutional care because it enables
recipients to live in the least restrictive environment possible and is, on average, less expensive than institutionalization. In California, the HCBS waiver
program is used to fund services for about one quarter of the developmentally disabled clients (an average caseload of 31,000 in 1998-99) served by RCs,
with total annual expenditures of over $400 million (about half of which comes from the General Fund). State Cited For Poor Service Quality. States must seek periodic reauthorization of their waiver programs from the federal Health Care Financing
Administration (HCFA), an agency within the U.S. Department of Health and Human Services. In 1997, after California had requested a renewal of its
HCBS waiver, HCFA officials visited several regional centers and community programs to gauge the quality of services being provided. In December
1997, HCFA released a report citing the state for numerous deficiencies, refused to renew California's waiver program, and required the state to submit a
new waiver application containing quality assurance measures that addressed HCFA's findings. As a result of these findings and other concerns regarding
the quality of community-based care, the 1998-99 Budget Act appropriated about $130 million ($90 million from the General Fund) for provider rate
increases, direct-care staff training, and improved RC case management services. While California prepared its application for a new waiver program, the state was allowed to continue billing for services under the old waiver program.
However, RCs were barred from enrolling new participants in the new waiver program. As a result of this ban on new admissions, the number of people
receiving waiver services decreased, as did the amount of federal funding the state could collect. We note that developmentally disabled Californians
entitled to receive services under the Lanterman Act continued to do so during this period of time. In effect, the admissions ban resulted in lost federal
revenue and an increase in General Fund costs. New Waiver Approved, But Admissions Still Frozen. California's new waiver program was approved effective October 1, 1998. Although DDS had
assumed that the admissions ban would be lifted when the new waiver was approved, HCFA kept the ban in place. According to HCFA, the state must
prove that each RC has implemented appropriate quality assurance measures before the center will be allowed to enroll new waiver participants. The
federal government's decision to maintain the admissions freeze will cost the state an estimated $25 million in lost federal revenue in 1998-99, which must
be made up using General Fund monies. The administration submitted a deficiency request to the Legislature for this amount in January 1999. Optimistic Budget Projections. Although the budget assumes that no RCs will be certified prior to June 30, 1999, it also assumes that all 21 centers will
be certified as of July 1, 1999--just one day later. As a result, the budget projects the collection of all possible federal funding for waiver-eligible services
in 1999-00. Although this could occur, it would require HCFA to reverse its position and allow the state to enroll new waiver participants at all of the
RCs, without requiring them to be certified first. Alternatively, if HCFA maintains its position that each RC be certified before being allowed to enroll
new waiver participants, this will have to be accomplished on a center-by-center basis. This would result in lower federal revenues than estimated in the
budget, and could lead to another deficiency request in 1999-00. At the time that this analysis was written, the department was unable to provide a plan or timeline for certifying RC compliance with the new quality
assurance measures. The department indicated that DDS and HCFA had not established a method for certifying RCs at that point, and that state officials
were still determining whether HCFA was willing to lift the ban on new admissions without requiring all RCs to be certified first. Analyst's Recommendation. As noted above, the ban on new admissions resulted in lost federal funds and increased state costs in 1997-98 and 1998-99.
Although the budget assumes that the ban will be lifted as of July 1, 1999, this may be overly optimistic given HCFA's requirement that RCs be certified
before they may enroll new participants. Accordingly, we recommend that the department report at budget hearings on (1) the status of its negotiations
with HCFA regarding the continuing freeze on new admissions to the state's HCBS federal waiver program, (2) its plan for enabling RCs to enroll new
participants in the program, and (3) the potential loss of federal reimbursements in 1999-00 if the admissions freeze is not completely lifted by July 1,
1999, as assumed in the budget.
Managed Risk Medical Insurance Board (4280)
Healthy Families Program
New Policies Adopted to Increase Enrollment
Monthly Enrollments Falling Behind Budget Projections for Current Year
Budget Proposes to Apply Income Deductions For Determining Eligibility
Department of Developmental Services (4300)
Community Services Program
Self-Determination Holds Promise, Needs Further Evaluation
Program Development Fund Surplus Can Offset General Fund
Developmental Centers Program
Budget Does Not Reflect Full Savings From Napa Program Closure
Budget-Year Projections of Federal Funding May Be Overly Optimistic
Return to 1999-00 Budget Analysis Health and Social Services Table of Contents
Return to 1999-00 Budget Analysis Table of Contents
Return to LAO Home Page