Legislative Analyst's OfficeAnalysis of the 2002-03 Budget Bill |
The Department of Veterans Affairs (DVA) provides services to California veterans and their dependents, and to eligible members of the California National Guard. The principal activities of the DVA include: (1) providing home and farm loans to qualifying veterans using the proceeds from the sale of general obligation and revenue bonds; (2) assisting eligible veterans and their dependents to obtain federal and state benefits by providing claims representation, subventions to county veterans service offices, and direct educational assistance to qualifying dependents; and (3) operating veterans' homes in Yountville, Barstow, and Chula Vista with several levels of medical care, rehabilitation services, and residential services.
The budget proposes total expenditures of $339 million in 2002-03. This is $2 million less than estimated current-year expenditures. Expenditures of $65 million from the General Fund are proposed for the budget year, which is $2 million, or 3 percent, less than the estimated current-year level.
We find that the Department of Veterans Affairs is not making sufficient efforts to collect reimbursements for services provided at the Yountville home. The resulting cash shortfalls have forced the department to obtain General Fund loans that it is finding difficult to repay, and at times have required the home to reduce services for home residents.
The DVA bills and collects reimbursements to help support the operation of the veterans' homes. At the veterans' homes, the majority of reimbursements come from five sources: (1) Medicare, a federally funded program which pays hospital inpatient and outpatient care, and some skilled nursing care; (2) Medi-Cal, funded by the federal and state governments, which pays skilled nursing facility daily rates and various healthcare costs; (3) member fees, which veterans' home residents pay in accordance with their income and level of care; (4) so-called "aid and attendance," which are federal payments for veterans who need personal care assistance; and (5) the U.S. Department of Veterans Affairs (U.S. DVA), which pays a per diem rate for each veteran in the homes.
Reimbursements are an integral part of the homes' operating budget. As Figure 1 shows, reimbursements are estimated to comprise 51 percent of Yountville's budget in 2001-02 and 2002-03. They are projected to comprise 23 percent of the other homes' budgets in 2001-02, and would increase to nearly 40 percent of their budgets in 2002-03.
|
Figure 1 Reimbursements Are a Significant Source |
|||
|
(Dollars in Millions) |
|||
|
Home |
Reimbursementsa |
Total |
Reimbursement |
|
2001-02 |
|
|
|
|
Yountville |
$34.4 |
$67.4 |
51% |
|
Barstow |
5.0 |
21.5 |
23 |
|
Chula Vista |
3.5 |
15.5 |
23 |
|
All Homes |
$42.9 |
$104.4 |
41% |
|
2002-03 |
|
|
|
|
Yountville |
$34.3 |
$67.2 |
51% |
|
Barstow |
8.4 |
22.1 |
38 |
|
Chula Vista |
7.3 |
20.4 |
36 |
|
All Homes |
$50.0 |
$109.7 |
46% |
|
a Includes United States Department of Veterans Aaffairs per diem. |
|||
|
|
|||
Failure to collect reimbursements, then, can create a greater dependency on the General Fund (a problem in times such as now when the state faces fiscal problems), results in cash shortfalls for the homes, and has a potentially significant effect on the services provided at the homes for residents.
Yountville's Difficulties With New Computer System. The Yountville home, which has been operating in Napa County since 1884, provides five levels of medical and residential care. Its nursing facility cares for about 350 veterans, and its residential and domiciliary facilities care for another 735 residents. Yountville operates a small hospital offering acute care and an outpatient clinic, which provide many services that are billable to Medicare, Medi-Cal, and other, private insurers.
In 1999-00, Yountville implemented a new computer system designed by a company named Meditech to assist the veterans' homes in claiming federal funds and insurance reimbursements to offset the state's costs of operating the homes. The feasibility study report justifying the system estimated that the system would generate $1.5 million in increased revenues from federal funds and reimbursements in the first year of implementations and $6.9 million in the second year. In addition to this billing function, the Meditech system provided a clinical component for documenting and tracking patient care.
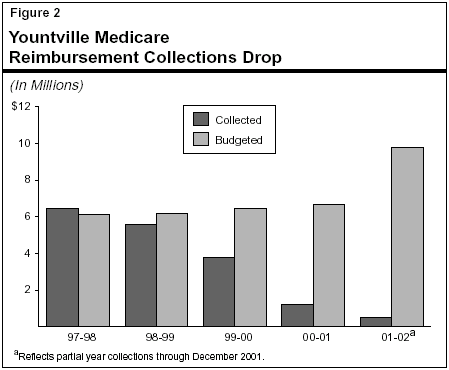
Due to the importance of reimbursements as a funding source, it was critical that Yountville staff input patient care data into the new system in order to generate bills for services provided. The home, however, failed to use the new system effectively, and the promised increase in reimbursements did not occur. Moreover, Medicare reimbursements in particular fell dramatically. Figure 2 illustrates that Medicare payments to the home dropped in 1999-00 by more than $2 million from the prior year, and continued to drop another $2 million in 2000-01. The home also has failed to collect budgeted reimbursements in the current year. The increase in current-year budgeted reimbursements was based upon the expectation that the department would be able to use the Meditech system effectively and that the promised increase in reimbursements finally would be realized.
The department's past difficulty in collecting reimbursements prompted the Legislature to request the Bureau of State Audits (BSA) to review the cash management of the department and the homes. The BSA's report, published in December 2001, found serious data deficiencies, general lack of oversight tools, and poor billing practices. The department generally agreed with the findings of the report and indicated that it was working aggressively to implement stronger managerial controls in this area.
Reimbursements Limited at Barstow and Chula Vista. The Barstow home opened in February 1996 with a capacity to serve 400 veterans. It provides four different levels of skilled nursing and residential care. Currently, the home is half full, serving about 90 veterans in its skilled nursing facility and about 125 veterans in its residential units.
Nursing facilities such as the one operated at the Barstow home can bill Medicare and Medi-Cal for services only if certified to do so by the state's Department of Health Services (DHS).
In July 2000, the Barstow home lost its Medicare and Medi-Cal certification along with U.S. DVA per diem payments for skilled nursing residents. The home had been cited for a number of deficiencies in quality of care standards. Therefore, from July 2000 to January 2002, Barstow was not permitted to bill for any federal reimbursements, resulting in a significant loss of anticipated federal funds. We discuss the consequences of this situation further below.
Barstow's reimbursements also have been below expectations in part because of its low occupancy levels. Even when Barstow was certified, a quarter to a third of the beds remained vacant. Once Barstow lost certification, the home generally did not admit new nursing residents, and occupancy dropped even more. With so many empty beds, the home has not been able to maximize revenue from member fees, U.S. DVA per diem, or Medi-Cal per diem payments.
Due to the problems at Barstow, the department's third and newest home in Chula Vista has not been able to open its skilled nursing facility. Like Barstow, that home has the capacity to serve 400 veterans in skilled nursing and residential facilities. While Chula Vista has received member fees and U.S. DVA per diem for the 200 veterans receiving residential care at the home, it does not yet have services to bill to Medi-Cal or Medicare.
Reimbursements accounted for less than 25 percent of the 2001-02 budgets for Barstow and Chula Vista. For 2002-03, the budget assumes federal certification of both facilities for the full year. Reimbursements thus are estimated to comprise closer to 40 percent of the expenditures of these homes in the budget year.
Member Fees and U.S. DVA Payments Generally Collected. Although the department has serious problems in its ability to bill for Medicare, Medi-Cal and other, private insurance reimbursements, the department appears to be fairly successful at collecting member fees and U.S.DVA payments for which it is eligible. These reimbursements require only a simple calculation of the number of residents and a rate in order to bill for services.
General Fund Usually Pays. The homes have one year to bill Medi-Cal for services rendered, and 18 months to bill Medicare, but do not always adhere to those time limits. For example, the department will not be able to bill for $2 million in reimbursements it expected to realize for services provided in 1999-00, because the time limits for billing Medicare and Medi-Cal have passed.
When problems in achieving budgeted reimbursement levels have occurred in the past, the department has obtained a loan from the General Fund to meet its cash needs and the home continues to spend up to its budgeted authority. The department is obligated to pay back such a loan within six months. As Figure 3 shows, the Yountville home currently has $5.3 million in outstanding General Fund loans. (The home would have had $7.3 million in loans for 2000-01 had it not reduced its expenditures by $2 million that year.) The department was not able to repay the loans within the six-month period.
In 2000-01, a delay in recertification of the Barstow facility made it impossible for that home to collect budgeted Medicare and Medi-Cal reimbursements. In order to be able to continue the home's operations for 2000-01, the shortfall was backfilled with $3.7 million from the General Fund through deficiency legislation, and another $1.8 million was provided through separate legislation. Barstow's decertification therefore cost the state General Fund an additional $5.5 million during that year.
Outside Contractors Hired. The department has hired outside contractors to address both Yountville's failure to collect reimbursements and the administrative problems at Barstow that led to its decertification. During the calendar years of 2001 and 2002, the department paid for about $2 million in consultant services.
|
Figure 3 Yountville General Fund |
|||
|
(In Millions) |
|||
|
Fiscal Year |
Loan |
Paid |
Balance |
|
1999-00 |
$7.8 |
$5.8 |
$2.0 |
|
2000-01 |
5.2 |
1.9 |
3.3 |
|
Totals |
$13.0 |
$7.7 |
$5.3 |
|
|
|||
At the time this analysis was prepared, Barstow had just been recertified by DHS, and was authorized to resume billing Medicare and Medi-Cal as of January 17, 2002. Yountville, on the other hand, did not appear to have made any significant improvements in collecting reimbursements. It is unclear how long it will take the department to implement the changes required to generate the additional dollars needed to operate the home. As Yountville continues to have trouble collecting reimbursements, it becomes more unlikely that the home will be able to repay its General Fund loans any time soon, or that the home will be able to achieve its budgeted level of reimbursements in the current year.
We recommend the adoption of supplemental report language directing the department to report to the Legislature on its cash flow management for an additional fiscal year. We further recommend that the department report at budget hearings on its projected cash needs for the homes in the current year. In addition, we recommend enactment of legislation requiring that any future collections of reimbursements that exceed budgeted levels be used to repay General Fund loans provided in prior years.
The Supplemental Report of the 2001 Budget Act directs the department to submit to the Legislature a series of three reports in the current year regarding how the department is managing its cash flow for the department and its homes. Those reports were due August 31, 2001, December 31, 2001, and February 28, 2002. The supplemental report further directs the Legislative Analyst to evaluate the reports, and to report its findings in the Analysis of the 2002-03 Budget Bill.
On January 25, 2002, we received the reports due in August and December 2001. The February 2002 report follows the publication of the Analysis. Accordingly, this section provides our findings on this subject as specified in the supplemental report.
August 31 Report. This report did not provide sufficient information to complete an analysis of the department's and the homes' cash needs. The report allocated the 2001-02 budget evenly over 12 months, and therefore represented estimated--not actual--cash needs.
December 31 Report. The December report shows actual cash receipts (General Fund dollars and reimbursements) and expenditures for July through November for the homes. It does not provide data for the department. Actual cash receipts are shown for current-year expenses only, however, so that any cash flow needs resulting from the prior year's activities cannot be determined from the report.
The report shows no reimbursement collections during the month of July. It does, however, display expected cash receipts through December 2002 to account for services that are provided through June but billed after the close of the fiscal year. We would note that the December report contains four months of data on which to assess cash needs for the current year.
Yountville's Current-Year Cash Shortfalls. The department's report provides both best-case and worst-case scenarios for Yountville's current-year cash flow needs, but predicts that actual cash needs will fall somewhere between these extremes. The outcome would depend on the effectiveness of efforts to improve reimbursements with the assistance of a contractor.
According to the report, at best the home will face a $1.7 million cash shortfall in April 2002 that would worsen to $7 million in June. The shortfalls would be covered by loans from the General Fund. The home, however, would be able to achieve its budgeted reimbursements in total and repay any outstanding loans by December 2002.
The worst case is that the home will face a $3.8 million cash shortfall in April 2002 that would worsen to about $10.7 million by June. The department would obtain loans from the General Fund to cover the shortfall. A portion of the shortfall would be paid, but the home would end the current year with a $6.6 million deficiency.
Based upon our review of the report, we concur that Yountville is likely to experience serious cash shortfalls in the current year, primarily because of its failure to improve its collections of reimbursements. An exact estimate of the anticipated cash shortfall is difficult to determine at this time, however, due to the availability of only a few months of cash receipt data and the uncertainty of the performance of the department's new contract to improve reimbursement collections. Based upon the data available to us at this time, we estimate that the home will probably need a loan in the range of $2 million to $4 million by April or May.
Based on our additional review of collections for prior-year services, we estimate that the home will not have the cash that would be needed to pay the total $5.3 million balance on the loans that cover previous years' cash shortfalls. Therefore, it is possible that by December 2002 the department could have a cumulative total of about $10 million in outstanding loans.
According to the report, the department does not plan to reduce purchases to accommodate a cash shortfall at Yountville in the current year, as it did in the prior year. The department indicated that because cuts have already been made in the department budget to reduce statewide spending in the current year, no further cuts would be identified for this purpose.
Barstow. Barstow's budgeted cash for operating costs amounts to $20 million in the current year, including about $5 million in expected reimbursements. The report shows that Barstow faces a potential shortfall in June of about $500,000, most of which would be paid by December. If current cash receipt and spending trends continue, Barstow would have a current-year shortfall of $128,000 at the end of December. The shortfall results primarily from a delay of about six weeks in the date the department was recertified for U.S. DVA per diem payments for nursing facility residents. The department asserts that a cost-of-living increase in the U.S. DVA per diem rates should offset these losses. We agree that a potential operating deficit for this home can be avoided.
Chula Vista. Chula Vista's budget provides about $14 million in cash during the current year, including $3.5 million in reimbursements. The report indicates that Chula Vista will end the current fiscal year with a positive cash balance. We would note that the 2001-02 budget assumes that Chula Vista's nursing facility will open by March and that U.S. DVA reimbursements will be available at that time for new residents. The budget also assumes that Medicare and Medi-Cal reimbursements will be available in May. The report assumes that Chula Vista will meet this schedule.
Any delay in the upcoming months in Chula Vista's ability to bill for or collect these reimbursements, however, could affect that home's cash flow. It is not clear at this time whether the home could reduce purchases or personnel costs to offset such cash flow problems. Should no such delays occur in the current year, it would be unlikely that Chula Vista would encounter any cash flow problems in the current fiscal year.
No Recommendations in Report. The supplemental report directed the department to make recommendations for accommodating any cash flow problems in future budgets. The department reported that it was deferring such recommendations until a department contractor could identify the maximum feasible level of collections of Medicare and Medi-Cal claims.
Continued Legislative Oversight. Because the department's cash flow problems have persisted, we recommend that the department report for an additional year on its cash flow management. We recommend the adoption of the following Supplemental Report language under Item 8955-001-0001, which is similar to that in the language for the Supplemental Report to the 2001 Budget Act:
The Department of Veterans Affairs shall submit the following reports to the Chair of the Joint Legislative Budget Committee and the chairs of the fiscal committees of both houses of the Legislature:
(a) On December 31, 2002, the department shall report on the cash flow needs of the department and veterans' homes. The report shall detail the expected expenditures and expected receipts of reimbursements and U.S. Department of Veterans Affairs per diem. The department shall notify the Legislature on what actions it would take to accommodate any cash shortfalls, including any plans to reduce purchases.
(b) On February 28, 2003, the department shall update the report pursuant to paragraph (a). The department shall describe the causes and fiscal implications of the differences between the February 28 and December 31 reports. The department shall notify the Legislature on what actions it would take to accommodate any cash shortfalls, including any plans to reduce purchases.
(c) The reports pursuant to paragraphs (a) and (b) shall provide the status of any outstanding loans for shortfalls occurring in prior fiscal years.
In addition, we recommend that the department report at budget hearings on the magnitude of any cash shortfalls anticipated in the current year.
Legislation for Repayment of Loans. In prior years, the department has sometimes collected reimbursements in excess of budgeted levels, and then submitted a request for the authority to spend the excess money for certain projects. In anticipation that the department's collections might exceed budgeted levels in future years, we recommend enactment of legislation requiring that any future collections of reimbursements that exceed budgeted levels be used to repay General Fund loans provided in prior years. Absent such a provision, the department bears no consequences for its failure to repay its loans. As we noted earlier, the Yountville home currently has outstanding loans of $5.3 million for which payment is late.
We withhold recommendation on the Governor's proposed budget for the Yountville home, until the Legislature is provided information on the outcomes of a contract to improve collections of reimbursements at the facility. We further recommend that the department report at budget hearings on certain measures that will document whether it is improving its ability to collect reimbursements.
The Supplemental Report of the 2001 Budget Act directed the department to report to the Legislature by December 15, 2001 and March 15, 2002 regarding an effort to maximize its reimbursement billings and collections at the Yountville home through the hiring of an outside consulting firm. The December report also was to identify any augmentations needed to the 2002-03 budget to improve the collections.
The Legislature further directed the Legislative Analyst to review the department's December 15, 2001 report and publish its review in the Analysis of the 2002-03 Budget Bill. In the event the department failed to make its report by December 15, 2001, the Legislative Analyst was to recommend specific budget adjustments for the 2002-03 budget intended to improve collections and to consider the cost-effectiveness of shifting the collections activity from the department to a private collector.
The 2001-02 budget contained $800,000 for the department to hire a consultant in July 2001 to improve collections of reimbursements during the 2001-02 fiscal year, particularly Medicare reimbursements for services provided at Yountville. The contractor, Health Management Services (HMS), was hired in December 2001 to provide the required services from January through December 2002.
At the time this analysis was prepared, the department had not submitted the December 15, 2001 report related to this issue. Because the consultant was not selected until late 2001, the department's report would not have been able to provide information on the outcomes of the contract or the cost-effectiveness of the contract, as directed by the supplemental report language.
We address the issues specified in the supplemental report below. In addition, we provide our recommendations for improving collections of reimbursements.
The 2001-02 Budget Act provided $800,000 for DVA to hire an outside contractor to enhance collection of reimbursements at the Yountville home by helping to improve the collection process and providing training related to this effort to home staff. As indicated above, the department hired HMS in late 2001 to provide consultant services from January through December 2002. The HMS will assist directly in the billing of reimbursements for medical services. It will also assess the level of reimbursements the homes should be receiving. Based on an initial assessment of Yountville conducted by HMS, it appears that significant training and process improvements are necessary to ensure the collection of all of the reimbursements owed to the home.
The delay in hiring a contractor for this purpose decreases the likelihood that the department will achieve the budgeted reimbursement levels established for 2001-02.
The supplemental report directs the Legislative Analyst to assess the cost-effectiveness of shifting collections activity from department staff to a private collector. This is an approach already being adopted at the Yountville home on a limited basis. In the fall of 2001, the department hired Certus Corporation to recoup uncollected reimbursements for services provided at the Yountville home between October 1, 1999 and June 30, 2001. Certus billed Medicare nearly $1.3 million in services, of which the department has actually collected about $550,000 so far.
Certus' billings are not enough to solve the home's cash flow problems or enable the home to pay off its $5.3 million loan balance. Certus has indicated that its ability to bill was limited by deficiencies it found in the home's billing processes. For example, insufficient data about medical services provided reportedly precluded the submittal of payable claims.
Given the $64,000 cost for Certus' services, the cost for privatizing these billings was about 12 percent of the total returns to date. However, the Certus contract was intended only to address a backlog of billings, not to provide collections expertise to the home on an ongoing basis. Be cause of its limited purpose, the Certus contract does not provide an adequate measure of the cost-effectiveness of shifting the entire collections activity from the department to a private collector.
A better such measure may be provided by the HMS contract. The cost-effectiveness of the HMS contract can be evaluated based upon the comparison of the additional collections generated with the assistance of the contractor and the cost of the contractor. If HMS determines that the home's maximum billing potential is significantly above historical collections, privatization of these activities could become a more attractive option.
2002-03 Budget. The Governor's proposed budget assumes that the Yountville home can achieve the same level of reimbursements that were budgeted for 2001-02. Specifically, the proposed budget estimates that the home will collect about $23 million in reimbursements (including about $11 million in member fees, $9 million in Medicare reimbursements, almost $2 million in Medi-Cal reimbursements, and $1.5 million in aid and attendance collections) and about $11 million in U.S. DVA per diem dollars.
Given the insufficient data available at this time regarding ongoing efforts to improve the collection of reimbursements, we withhold recommendation on the Yountville home's budget. We believe that significant information regarding those efforts should be available before the May Revision. This information can be used to reassess the proposed budget for Yountville.
Further contracting for billing assistance may be possible in the budget year without budget augmentations. The 2001-02 spending plan included $800,000 for the contract to improve reimbursement collections that was redirected from Yountville's personnel budget. The Governor has proposed to maintain that funding for Yountville in the budget year. If this contracting effort proves to be successful, the Legislature could direct that these funds again be used to contract out for billing services beyond the contract period, which ends December 2002.
Establishing Benchmarks. As we previously discussed, both the BSA and the department's new contractor, HMS, have recently reviewed Yountville's billing practices. Both the BSA report of December 2001 and the new contractor's initial assessment of Yountville's accounts receivables management process recommend specific improvements in collections efforts, including better documentation of the provision of medical services in an accurate and timely manner, and the establishment of standard billing policies and procedures. An internal control review of Yountville's accounting practices conducted by the Inspector General for Veterans Affairs also noted the need for the implementation of better policies and procedures for cash receipts and disbursements.
Given these findings, we recommend that the department report at budget hearings regarding its performance in collecting reimbursements according to certain improvement measures that we specify below. These measures should serve as a "benchmark" for judging the department's performance in this area. This information should also help the Legislature determine whether any adjustments should be made to the proposed budget.
Accordingly, we recommend the department report during budget hearings on:
We note that the department has also been directed to submit a report to the Legislature by March 15, 2002 regarding the performance of its contract in improving billings and collections. This report requires in formation that also will be necessary to evaluate the department's collections activity.
We do not recommend privatizing the administration of the skilled nursing facilities at the existing homes at this time because of the fiscal and operational difficulties of making such a change.
As we discussed in a previous section, Barstow's skilled nursing facility lost its federal certification in July 2000 due to a number of serious deficiencies in its operations. The home's administrative problems prompted DHS to appoint a temporary manager of the facility to improve the quality of care. The DVA subsequently contracted with Country Villa Health Services to provide such services from January 2001 through October 2001. Country Villa assisted Barstow in meeting federal compliance standards to thus regain certification for its skilled nursing facility.
The Supplemental Report of the 2001 Budget Act directed the department to submit to the Legislature by December 1, 2001 its evaluation of the Country Villa contract. That report was to include recommendations as to whether the homes should contract out the administration of its skilled nursing facilities. The Legislature also directed the Legislative Analyst to (1) review and comment on the department's findings and recommendations in the Analysis of the 2002-03 Budget Bill, or (2) in the event the department failed to provide the report, to make recommendations about the utility of contracting for the administration of the skilled nursing facilities at the homes.
We had not received the report that DVA was directed to prepare at the time this analysis was prepared. Accordingly, we provide below our findings and recommendations regarding the potential for privatizing the homes' skilled nursing facilities.
A number of options exist for privatizing the homes' skilled nursing facilities. The Legislature could direct DVA to outsource management (either financial or medical) of the facilities, or it could fully outsource its skilled nursing facility operations, including nursing staff. Alternatively, the department could outsource the entire operation of the home, which includes levels of care other than skilled nursing. Federal law requires only that at least one state department employee oversee a state's veterans' home in order to qualify for federal support.
So far, California's experience with private contracting for the administration of the homes has been limited to the Barstow model, where the department contracted on a temporary basis for the management of the facility, and the current Yountville model, where the department is contracting only for the financial billing function of the facility. (We discussed the issue of privatizing the billing function of the homes in an earlier section.) Food service, laundry, and specialty medical services, among others, have also been provided through contracting.
Some states have gone further in their contracting, however. The California Research Bureau reported in November 2001 that some states such as Oregon, Texas, and Alabama contract out all of their nursing and residential services.
Privatizing the administration of skilled nursing could enhance the quality of care and lower state costs, although such an option is not without its own limitations as we discuss below.
As the state has discovered with Barstow, contracting out for management of the home provided the expertise necessary to ensure quality of care to residents and to avoid further loss of federal funds. The General Fund is at risk for backfilling any loss of federal dollars from the loss of certification when quality of care problems arise.
Contracting for all staff needed to operate the skilled nursing facilities could also have the effect of holding down the cost of such facilities. Our review indicates that costs of operating the skilled nursing facilities in the state's veterans' homes clearly exceeds the costs of operating comparable facilities in the private sector--and may be as much as two to three times higher. The average annual costs for skilled nursing residents in the private sector range from $40,000 to $45,000, while the average annual costs for nursing residents in the state's veterans' homes range from $110,000 to $130,000.
However, while such a shift to private contracting may make sense in theory, there are significant legal constraints involved in replacing civil service employees with privately contracted staff at the existing homes. Another disadvantage is that expertise acquired by the staff through training would be lost.
Privatizing the management portion of the skilled nursing facilities also raises the risk that the state would pay twice for the same management service. A state employee would be required to oversee the home in some capacity, even as a contract manager. Notably, contracting for private management services at Barstow under the Country Villa contract did not reduce state operating costs for the home. The contract cost the state about $900,000 over a period of ten months. The contractor was critical to restoring quality of care as well as federal funding. However, during the period of the contract, the state continued to incur costs for the administrator of the entire home, as well as other managerial staff.
When Barstow was decertified, the home reportedly did not have any licensed nursing home administrators managing the facility. We are advised that Barstow now has several managers who are licensed nursing home administrators. As long as Barstow's managers can ensure quality of care standards, we believe the additional costs of contracting for that purpose are not warranted.
There is evidence that Barstow can meet quality of care standards. Barstow was recertified and found to be in substantial compliance with federal standards. There are also indications at this time that Chula Vista and Yountville, which also have licensed nursing home administrators as part of their management staff, can provide adequate care to the veterans at these homes. Given the indications that the homes can be operated in compliance with federal standards, and the potential legal issues associated with privatizing the full operations of the existing nursing facilities, we do not recommend that the state contract for the administration of the skilled nursing facilities at the homes at this time. However, we would recommend that the Legislature review the idea in the future, particularly if any of the homes again demonstrates an inability to meet federal and state quality of care standards that would jeopardize the state's certification for Medicare and Medi-Cal.
We recommend that the Legislature reassess budgeted reimbursement levels for the Barstow and Chula Vista homes at the time of the May Revision. At that time, more information should be available about whether the homes can activate the additional beds as proposed.
Barstow. Now that Barstow is recertified, the home should be able to increase its occupancy of skilled nursing and intermediate care beds. The budget assumes that the number of residents in skilled nursing care beds will increase from 90 residents to 110 residents in the budget year. The budget also assumes that 50 intermediate care beds become operational by October.
In addition, the budget assumes that 80 additional residential and domiciliary beds will be occupied at Barstow by October. Because Barstow historically has had difficulties both in filling resident spaces and in hiring staff, it is unclear whether the home will be able to meet all of these occupancy targets in the budget year. The home has had problems in the past achieving its budgeted occupancy levels.
Chula Vista. Chula Vista's ability to meet budgeted reimbursement levels will depend on its success in bringing its new nursing facilities on line. First, the facility must be licensed for operation and certified to receive Medicare and Medi-Cal reimbursements. Second, the facility must be able to hire a workforce to provide care to the veterans needing skilled nursing. Third, the facility must have an effective system in place to bill for services and ensure that budgeted reimbursements are collected.
The budget assumes 110 nursing facility beds and an additional 50 intermediate care beds will be occupied by October 2002. These projected occupancy levels would make the home fully operational by October 2002. At this time, there is no apparent reason why Chula Vista should not to able to obtain a license for operation of its nursing facility and to bring its new nursing facilities on line.
In view of the above, we recommend the Legislature assess the department's ability to activate the additional beds at the two homes at the time of the May Revision.