Legislative Analyst's OfficeAnalysis of the 2002-03 Budget Bill |
Hospitals face a number of financial pressures in the next several years. Recent federal regulations limiting the amount the state can pay public hospitals participating in the Medi-Cal Program will further exacerbate financial problems for some of these hospitals. In the following pages, we summarize the role of these hospitals in California, examine their financial status, describe the challenges that hospitals face over the next few years, and identify issues that the Legislature might want to investigate further.
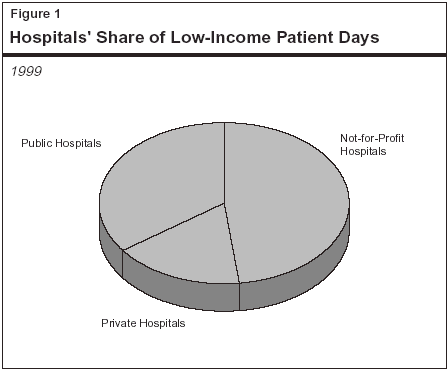
Not-For-Profit and Public Hospitals Care For Most Low-Income Patients. Figure 1 shows the three main types of hospitals in California and the share of low-income patients that they serve. In 1999, nearly half of all Medi-Cal and uninsured patient days were for care provided in not-for-profit hospitals and 35 percent were for care in public hospitals. In contrast, private hospitals provided considerably fewer days of care to low-income patients--only 17 percent of the total. Not-for-profit and public hospitals devote a larger share of their resources to providing care for low-income patients who have less of an ability to pay and, as a result, these hospitals are especially vulnerable to financial pressures.
Financial Condition of Hospitals Is Weakening. Our analysis of data from the Office of Statewide Health Planning and Development (OSHPD) and our review of several studies found that some key measures of financial health indicate that the general financial condition of hospitals in California has weakened in the last several years. The California Healthcare Foundation reported in 2001 that the years 1995 through 1999 were a period of weakening financial health for California's hospitals. It found that hospital operating revenues per discharge declined over this period. This study also reported that in 1999, more than one-half of all hospitals in California lost money from their operations.
Our review of the OSHPD data found significant disparities in the operating margins or "profitability" of different types of hospitals. Investor-owned hospitals appear to be in relatively good financial health with average operating margins of nearly 5 percent in 1999, and 2 percent for the period of June 2000 to December 2000. (According to the California Healthcare Foundation, an operating margin of 3 percent to 5 percent is considered healthy.) In contrast, the operating margin of public hospitals was negative 14 percent in 1999 and dropped to negative 19 percent in the last six months of 2000. A negative operating margin indicates overall losses. The operating margin for not-for-profit hospitals was better--about negative 1 percent in 1999 and negative 2 percent for the period of June 2000 to December 2000. These findings indicate that public and not-for-profit hospitals may be most vulnerable to financial pressures.
California May Have Excess Hospital Beds. The weak financial condition of some hospitals could be in part a result of low hospital bed occupancy rates. Hospital occupancy rates have often been considered a measure of the efficiency of hospital operations because empty beds do not generate revenue while increasing hospital costs. The California Healthcare Foundation report cites numerous studies that have concluded that the state has more hospital beds than it needs. (The question remains whether these beds are in the right places.) The hospital beds currently in place are more appropriate in terms of geography and facility type to the financial and health care needs of 30 years ago. The study finds that the medical practices and technologies used today require significantly fewer inpatient beds, as well as different types of facilities than are actually in operation. For example, advances in technology that reduce the time it takes to heal from a surgical procedure have shifted many procedures to outpatient settings or greatly reduced the amount of recovery time that must be spent in the hospital.
Our analysis of the OSHPD data found that the hospital bed occupancy rates for all California hospitals (excluding data from state hospitals) was 55 percent in 1999 and 54 percent in 2000. In comparison, the average hospital occupancy rate in the United States in 2000 was 65 percent, about 10 percent higher than California's average occupancy rate.
There was significant variance in the occupancy rate depending upon the type of hospital bed. For example, acute respiratory care beds were heavily occupied while half of regular medical or surgical beds were vacant at any given time. We found that the average occupancy rates were relatively consistent between the different types of hospitals, but that rates are more likely to vary according to the size of the hospital.
The combination of hospitals operating at one-half of their potential occupancy and an increase in fiscal pressures could create an opportunity for reform and consolidation in the hospital marketplace. Some of this change has already occurred and data from OSHPD indicates that the number of hospitals operating in the state since 1995 (not including state hospitals) has declined by 25 percent. These closures have resulted in an 11 percent increase in occupancy rates since 1995, most likely because a number of hospital closures occurred during this same time period while the demand for hospital beds remained stable.
We discuss the set of financial pressures hospitals face in more detail below.
Seismic Compliance Costs. Chapter 740, Statutes of 1994 (SB 1953, Alquist), requires all hospitals to meet certain seismic safety standards by 2008 and an even stricter set of standards by 2030. Specifically, the legislation established standards of survivability for nonstructural and structural components of all general acute-care inpatient hospital buildings. The major provisions of Chapter 740 require the following of OSHPD:
The OSHPD estimates that almost 50 percent of California's acute care hospitals will have to be upgraded or replaced to meet the 2030 standards. Chapter 740 does not require the state to have a financing role in its implementation and hospitals may face major difficulties securing the financing to comply with the new standards. The California Healthcare Association (CHA) estimates that compliance would cost billions of dollars over 30 years, but this number has not been independently verified. Noncompliance may mean that hospitals in already underserved areas could face closure or diminished capacity to serve their communities.
Chapter 740 limits the role of the state to assessing seismic safety plans and overseeing hospital compliance with the requirements of the act. The Legislature has recognized challenges posed by the act. Several bills to address the issue were proposed in the 2001-02 session including SB 842 (Speier), which proposes to extend the 2008 deadline by five years for certain hospitals provided that after 2013, they meet the 2030 standard. Also introduced and signed into law were Chapter 228, Statutes of 2001 (AB 832, Corbett), which revises specified seismic evaluation requirements and clarifies OSHPD's ability to grant flexibility to hospitals in meeting seismic safety standards, and Chapter 247, Statutes of 2001 (AB 656, Chan), which extends the deadline for county-owned hospitals to meet certain nonstructural seismic safety requirements.
Compliance Costs for the Health Insurance Portability and Accountability Act. Congress enacted the Health Insurance Portability and Accountability Act (HIPAA) in 1996. As we discussed in the Analysis of the 2001-02 Budget Bill, and this year's Analysis, HIPAA's primary purpose is to improve the portability and continuity of health insurance for workers and their families. Both private and public sector organizations, including hospitals, that provide health care services and use patient or other health care data must comply with HIPAA. Many of these new standards will result in system changes for hospitals and physicians.
A national study by Tillinghast-Towers Perrin estimates the cost for hospitals to comply with certain HIPAA requirements ranges from $725,000 to $3.5 million for each hospital. Similarly, the American Hospital Association estimates that it might cost each hospital approximately $4.6 million annually for the first five years of implementation to comply with all of the HIPAA-related rules or a total of approximately $9 billion for all hospitals in California. The federal government did not provide any funding to assist effected organizations in complying with the rules. However, CHA states that hospitals recognize that compliance with some of the rules will result in a return on the investment once the manual systems are eliminated. According to CHA most, if not all, hospitals have begun work on implementing HIPAA and plan to meet the compliance deadlines.
Reduction in Medicare Payments to Hospitals. The federal Balanced Budget Act of 1997 (BBA) established a new methodology for reimbursing hospitals for services provided to Medicare beneficiaries. The methodology cut total Medicare payments to California hospitals by approximately $5.5 billion for payments in 1998 through 2002. The federal Balanced Budget Refinement Act of 1999 reconsidered the issue and provided about $401 million in federal relief from these cuts to California hospitals. The federal Medicare, Medicaid, and State Child Health Insurance Plan Benefits and Improvement and Protection Act of 2000 provided an additional $621 million to increase payments to California hospitals for outpatient services. The overall reduction in Medicare payments to hospitals still represents a significant decrease in federal funding despite the approximately $1 billion in relief provided to the state's hospitals by the federal government.
Funding Available to Medi-Cal Disproportionate Share Hospitals Has Declined. The state began the Disproportionate Share Hospitals (DSH) Program in 1991 during a period of severe state budget problems to generate new federal funding to supplement Medicaid payments to hospitals that serve a disproportionate share of Medi-Cal and other low-income individuals. The state funds the DSH program by combining local funding from public entities such as counties, the University of California, and hospital districts with federal dollars. (Neither the state nor private hospitals contribute to the program.) Hospitals that serve a disproportionate share of Medi-Cal patients and the uninsured are eligible for DSH funding. In 1998-99, 131 public and private hospitals, about one-in-four statewide, were eligible for Medi-Cal DSH funds.
The BBA fixed in law each state's Medicaid DSH allotment through 2002 and reduced the amount of federal funding that would be available each year. The federal government restored some of the federal DSH funding that it previously cut in 2000, but the result was still a net reduction in the federal allotment. As outlined in the BBA, each state's federal DSH allotment will increase annually starting in federal fiscal year 2003 (during the 2003-04 state fiscal year). For the next three years, the allotment would increase by the previous year's amount in addition to the percentage change in the Consumer Price Index.
The total amount of funding available for DSH hospitals will be will be about $2.1 billion in the current fiscal year and will decrease by $238 million to $1.8 billion in 2002-03.
The State's DSH "Takeout." In addition to the overall decrease in DSH funding described above, the Governor's budget proposes to increase the state's takeout from the DSH allocation. The practice of the state using a portion of DSH funding for the Medi-Cal program began in the early 1990s during state fiscal constraints. By 1995-96, the state was making almost $240 million of this funding available for general Medi-Cal program benefit costs. Over the last several years, as the state's fiscal condition improved, the state reduced its takeout from DSH funding. This resulted in savings to public hospitals because the total amount of funding they transferred to the state decreased while they still received the maximum allowable DSH payments. The state's takeout in 2001-02 is about $30 million.
The Governor proposes to increase the state's takeout from DSH to about $85 million in the budget year (the level in 1999-00) which will result in General Fund savings of $55 million. This action will cause hospitals that participate in DSH to have to increase the amount of funding they must transfer to the state to participate in the DSH program.
Nurse-to-Patient Staffing Ratios. In January 2002, the state proposed nurse-to-patient staffing ratios of one nurse for every six patients on general medical floors of hospitals. Hospitals must adhere to these standards by July 2003. There is some debate about the estimated cost of compliance. The CHA contends that hospitals may have to spend as much as $400 million a year to add 5,000 nurses to meet the new nurse-to-patient ratio requirements. In contrast, a University of California San Francisco professor and associate director of the university's Center for Health Workforce Studies estimates that the regulations would cost hospitals about $137 million a year.
California's Ailing Emergency Services System. Emergency departments (EDs) and trauma centers face growing financial losses. Under state and federal law, any person seeking care at an emergency department must be provided emergency care regardless of their ability to pay. According to OSHPD Hospital Annual Disclosure Reports (1996-99), 14 percent of ED patients were uninsured and 7 percent were paid for by county indigent programs, resulting in little or no compensation to the hospital for these patients. The problem is aggravated by the use of EDs and trauma centers as a point of access for nonemergency services (primary and urgent care). The California Medical Association estimates that more than 80 percent of all Medi-Cal and uninsured patient visits to EDs were for conditions that could have been treated in a nonemergency setting.
Some of the cost of uncompensated care is offset by supplemental Medi-Cal reimbursements and subsidy programs for county facilities. For example, the County Healthcare for Indigents Program provides funding to counties for uncompensated hospital, physician, and other health care services. In addition, separate augmentations have been made to address this issue including $25 million in the current year and a similar amount proposed for the budget year. The 2001-02 Budget Act provides a one-time augmentation of $25 million (General Fund) for local trauma center support to the Emergency Medical Services Authority.
In addition to the financial problems discussed above, the next pressure we will discuss will further exacerbate these problems and could have a significant fiscal impact on the state's General Fund.
A major change in federal rules relating to the reimbursement rates for Medicaid programs appears certain to impose additional financial pressures on California's public (county and University of California) hospitals. This change, more than any other we have described, could increase state costs and require the state to closely examine the Medi-Cal rates it pays hospitals for inpatient and outpatient services.
Change in Federal Rule Will Reduce Medi-Cal Payments to Hospitals. A federal rule change effective March 2002 will phase out a provision in federal regulations that enabled states to increase the federal Medicaid funding they received without increasing their state contributions. Under this practice, some states paid city- or county-owned health care facilities more than the actual cost of health services, thereby generating additional federal funding, and then required the facilities to return the additional funds to the state. Some states, like California, used the additional funding for health-care related expenses. However, many states used little or none of the money for health-related costs.
The new federal rule gradually reduces the amount a state can pay public hospitals by establishing an "upper payment limit" equal to 100 percent of estimated Medicare payments for the same services.
California will have an eight-year period, until 2010, to comply with the rule. To do so, the state will have to eventually lower the payments it makes under the Medi-Cal Program to nonstate owned (county and the University of California) public hospitals by hundreds of millions of dollars annually. The Medi-Cal Program currently pays this class of hospitals more than 150 percent of their costs of care when the amount of contract rate payments and supplemental payments from other funds are taken into account. Since the limit of 100 percent of Medicare payments already applies to private hospitals, they will not be affected by this new regulation.
State Expenditures Might Increase. As the upper payment limit phases in, the state is likely to face difficult questions as to whether it should--or must--step in to maintain the hospital network that serves Medi-Cal patients and the uninsured. In part, this could be accomplished by setting Medi-Cal rates for hospitals at the maximum allowable level of Medicaid funding under federal law, 100 percent of Medicare, instead of negotiating separately with hospitals. The California Medical Assistance Commission (CMAC) estimates that, under this scenario, total General Fund costs (including managed care payments to hospitals) would increase by approximately $500 million General Fund annually. Even after such an increase, CMAC estimates that public hospitals would still be reimbursed significantly less than they were prior to the implementation of the upper payment limit.
Supplemental Hospital Financing Programs Most Likely Will End. Phase-in of the upper payment limit will probably result in the eventual elimination of two of California's supplemental hospital financing programs: the state's Emergency Services and Supplemental Payments fund (also known as the SB 1255 program) and the Medi-Cal Graduate Medical Education program. The elimination of these funding sources will reduce funding to a variety of hospitals including private safety-net, children's, teaching, and public.
Hospital Outpatient Rates Would Increase. Hospitals have been in litigation with the state over reimbursement rates for hospital outpatient services since 1990 in a case known as Orthopaedic Hospital v. Belshe. The DHS had set rates based on what it deemed necessary to encourage enough hospitals to participate in the Medi-Cal Program. However, the courts interpreted federal law to require reimbursement based upon a determination of "reasonable costs".
The settlement of the case is now anticipated to be completed in 2001-02. California's hospitals would be paid $175 million for past Medi-Cal claims and be provided a retroactive increase in Medi-Cal reimbursement rates for outpatient hospital care of 30 percent. Under the proposed settlement, rates would be further increased by 3.3 percent for each of the next three years.
The original terms of the settlement called for a $350 million payment for prior claims, to be evenly split between the federal and state government. However, implementation of the settlement was delayed because of a dispute between the federal and state governments over this portion of the proposed settlement. According to the Governor's office the terms of a new tentative agreement will require that DHS pay its share of the $350 million--$175 million General Fund--and be held harmless for any additional costs for the prior claims. Attorneys representing the hospitals anticipate that final agreement will be reached on the terms of the settlement in spring 2002 and that hospitals will begin receiving settlement payments in May or June 2002. Funding for this purpose is included in the current-year budget.
The state has an interest in the financial stability of the network of hospitals that provide health care services to Californians, especially those public hospitals providing services for patients enrolled in the state's Medi-Cal Program and the uninsured. We outline a number of steps the Legislature could take, even in the current difficult fiscal situation, to maintain the financial viability of California's network of hospitals.
In the following section, we offer a number of options that the Legislature could consider, even as the state faces a serious budget problem, to begin to assess the financial pressures hospitals face. These include directing the OSHPD to assess hospital bed vacancy rates, options for assisting emergency departments, and directing DHS and CMAC to conduct a fiscal assessment of the upper payment limit.
Study Hospital Occupancy. The OSHPD develops policies, plans, and programs to assist health care systems in meeting current and future needs of Californians and improving the overall delivery and accessibility of health care in the state. The Legislature may wish to consider directing OSHPD to review statewide hospital bed occupancy data to examine how the occupancy rates vary by region and to determine, on a regional basis, if there is an oversupply or undersupply of hospital beds. As discussed earlier in this review, there is evidence of excess bed capacity in some areas of the state. The OSHPD should also use occupancy rate data and financial information to identify opportunities for hospital consolidation.
The bed data collected by OSHPD would also enable the Legislature to identify specific areas in the state where there is a shortage or potential shortage of hospital beds. The availability of such data would help the Legislature to determine when and if state assistance is warranted to prevent the closure of hospitals needed to maintain access to services for Medi-Cal patients and the uninsured.
Options for EDs. The Legislature may wish to consider several options related to the cost pressures affecting EDs and trauma centers. As discussed in more detail in our analysis of the Medi-Cal budget, the Legislature could consider increasing the copayment for nonemergency care in EDs in the Medi-Cal and Healthy Families Programs. We believe this approach could relieve some financial pressure on EDs by discouraging nonemergency use.
The Legislature might consider making it easier for providers to access unspent county Emergency Medical Services Funds (EMSF) by removing the restriction that prevents EMSF providers from recovering only half of their cost of uncompensated care. This option is discussed in Options Addressing the State's Fiscal Problem. The most recent fund condition statement (1999-00) indicates that counties had more than $55 million in fund reserves that could be used for uncompensated care in EDs. The Legislature could use this option to augment the overall amount of resources available to support EDs. Alternatively, it may wish to consider using these resources in place of the Governor's budget year proposal to provide a $24.8 million augmentation of Proposition 99 funds to help offset the cost of uncompensated care in EDs.
Conduct Fiscal Assessment of the Upper Payment Limit. The Legislature should consider directing DHS and CMAC to conduct a fiscal assessment to determine the impact of the federal upper payment limit on hospitals. This assessment should estimate the total amount of funding hospitals will lose, and attempt to determine the potential impact of the new rule on the services provided by these hospitals. The assessment should also identify which hospitals are at the greatest financial risk as a result of this federal action. This information will enable the Legislature to fully assess the impact of the upper payment limit rules. A small portion of the DSH takeout that the Governor's budget proposes for DHS and CMAC could be used to provide for staffing and consulting resources needed to initiate work on these issues.
We have described many of the issues that will create serious financial headaches for hospitals during the next several years. We have also suggested some steps the Legislature could take to begin to assess and address these issues.