Analysis of the 2004-05 Budget BillLegislative Analyst's Office
|
In California, the federal Medicaid Program is administered by the state as the California Medical Assistance Program (Medi-Cal). This program provides health care services to welfare recipients and other qualified low-income persons (primarily families with children and the aged, blind, or disabled). Expenditures for medical benefits are shared about equally by the General Fund and by federal funds. The Medi-Cal budget also includes federal funds for (1) disproportionate share hospital (DSH) payments, which provide additional funds to hospitals that serve a disproportionate number of Medi-Cal or other low-income patients, and (2) matching funds for state and local funds in other related programs.
At the state level, the Department of Health Services (DHS) administers the Medi-Cal Program. The California Medical Assistance Commission negotiates contracts with hospitals and health plans for the provision of Medi-Cal services. Other state agencies, including the Department of Social Services, the Department of Mental Health, the Department of Developmental Services, the California Department of Aging, and the Department of Alcohol and Drug Programs receive Medi-Cal funding from DHS for eligible services that they provide to Medi-Cal beneficiaries. At the local level, county welfare departments determine the eligibility of applicants for Medi-Cal and are reimbursed by DHS for the cost of those activities. The federal Centers for Medicare and Medicaid Services oversees the program to ensure compliance with federal law.
Proposed Spending. The budget for DHS proposes Medi-Cal expenditures totaling $31 billion from all funds for state operations and local assistance in 2004-05. The General Fund portion of this spending ($11.6 billion) increases by $1.8 billion, or 19 percent, compared with estimated General Fund spending in the current year. The remaining expenditures for the program are mostly federal funds, which are budgeted at a level ($17.8 billion) that is about 3 percent more than estimated to be received in the current year.
More than half of the overall increase in General Fund spending is due to the inclusion in 2003-04 of a program accounting change that reduces program costs on a one-time basis. In addition, one-time savings result from increased federal funds in 2002-03 and 2003-04. Adjusting for these one-time savings, underlying General Fund expenditures for Medi-Cal are projected to grow by $191 million, or about 2 percent, in 2004-05. These additional costs are proposed to be more than offset by spending reductions.
The spending total for the Medi-Cal budget includes an estimated $1.8 billion (federal funds and local matching funds) for payments to DSH hospitals, and about $4.7 billion budgeted elsewhere for programs operated by other departments, counties, and the University of California.
Federal law requires the Medi-Cal Program to provide a core of basic services, including hospital inpatient and outpatient care, skilled nursing care, doctor visits, laboratory tests and x-rays, family planning, and regular examinations for children under the age of 21. California also has chosen to offer 34 optional services, such as outpatient drugs and adult dental care, for which the federal government provides matching funds. Certain Medi-Cal services—such as hospitalization in many circumstances—require prior authorization from DHS as medically necessary in order to qualify for payment.
Based on recent caseload information, 42 percent of the Medi-Cal caseload consists of participants in the state's two major welfare programs, which include Medi-Cal coverage in their package of benefits. These programs are (1) the California Work Opportunity and Responsibility to Kids (CalWORKs) program, which provides assistance to families with children; and (2) the Supplemental Security Income/State Supplementary Program (SSI/SSP), which assists elderly, blind, or disabled persons. Counties administer the CalWORKs program through county welfare offices that determine eligibility for CalWORKs benefits and Medi-Cal coverage concurrently. Counties also determine Medi-Cal eligibility for persons who are not eligible for (or do not wish) welfare benefits. The federal Social Security Administration determines eligibility for SSI/SSP, and the state automatically adds SSI/SSP beneficiaries to the Medi-Cal rolls.
Generally, persons determined eligible for Medi-Cal benefits (Medi-Cal "eligibles") receive a Medi-Cal card, which they use to obtain services from providers. Medi-Cal provides health care through two basic types of arrangements—fee-for-service and managed care.
Fee-for-Service. This is the traditional arrangement for health care in which providers are paid for each examination, procedure, or other service that they furnish. Beneficiaries generally may obtain services from any provider who has agreed to accept Medi-Cal payments. The Medi-Cal Program employs a variety of "utilization control" techniques (such as requiring prior authorization for some services) designed to avoid costs for medically unnecessary or duplicative services.
Managed Care. Prepaid health plans generally provide managed care. The plans receive monthly "capitation" payments from the Medi-Cal Program for each enrollee in return for providing all of the covered care needed by those enrollees. These plans are similar to health plans offered by many public and private employers. More than half (3.3 million of the total of 6.4 million Medi-Cal eligibles in July 2003) are enrolled in managed care plans. Beneficiaries in managed care choose a plan and then must use providers in that plan for most services. Since payments to the plan do not vary with the amount of service provided, there is much less need for utilization control by the state. Instead, plans are monitored to ensure that they provide adequate care to enrollees.
Almost all Medi-Cal eligibles fall into two broad groups of people. They either are aged, blind, or disabled or they are in families with children. More than half of Medi-Cal eligibles are welfare recipients. Figure 1 shows, for each of the major Medi-Cal eligibility categories, the maximum income limit for eligibility for health benefits, the estimated caseload, and the annual benefit cost per person for 2003-04. The figure also indicates, for each category, whether an asset limit applies and whether eligible persons with incomes over the limit can participate on a "spend down" basis. If spend down is allowed, then Medi-Cal will pay the portion of any qualifying medical expenses that exceed the person's "share-of-cost," which is the amount by which that person's income exceeds the applicable Medi-Cal income limit.
|
Major Medi-Cal
Eligibility Categories |
|||||
|
2003-04 |
|||||
|
|
Maximum |
Asset |
Spend |
Enrollees |
Annual |
|
Aged,
Blind, or Disabled Persons |
|||||
|
Welfare (SSI/SSP)
|
$1,419 |
� |
� |
1,301 |
$7,938 |
|
Medically
needy |
954 |
� |
� |
247 |
7,355 |
|
133 percent
of poverty equivalent |
1,419 |
� |
� |
�d |
�d |
|
Medically
needy�long-term care |
Special |
� |
� |
64 |
43,843 |
|
Families |
|||||
|
Welfare (CalWORKs)e |
$1,150 |
� |
� |
1,479 |
$1,459 |
|
Section
1931(b)-onlyf |
1,624 |
� |
� |
2,605 |
1,531 |
|
Medically
needy |
1,190 |
� |
� |
�g |
�g |
|
Children
and Pregnant Women |
|||||
|
200 percent
of poverty�pregnancy service and infants |
$3,157 |
� |
� |
203 |
$3,488 |
|
133 percent
of poverty� |
2,130 |
� |
� |
117 |
1,260 |
|
100 percent
poverty� |
1,624 |
� |
� |
111 |
1,005 |
|
Medically
indigent� |
1,190 |
� |
� |
221 |
1,329 |
|
Medically
indigent adults� |
1,190 |
� |
� |
6 |
12,001 |
|
Emergency
Only |
|||||
|
Undocumented
immigrants may qualify in any category and are limited to emergency
services (including labor and delivery and long-term care) |
822 |
$1,231 |
|||
|
|
|||||
|
a
Amounts are for an aged or disabled couple (including the
standard $20 disregard) or a four-person family with children |
|||||
|
b
Indicates whether persons with higher incomes may receive
benefits on a share-of-cost basis. |
|||||
|
c
Combined state and federal costs. |
|||||
|
d
Enrollment and costs included in amounts of Medically
Needy Aged, Blind, or Disabled persons. |
|||||
|
e
Income limit to apply for CalWORKs (including a $90 work
expense disregard). After becoming eligible, the income limit |
|||||
|
f
Includes Transitional Medi-Cal, which extends coverage for
families who leave CalWORKs or 1931(b)-only for up to 12 months. |
|||||
|
g
Enrollment and costs included in amounts for Section
1931(b) family coverage. |
|||||
Aged, Blind, or Disabled Persons. About 1.6 million low-income persons who are (1) at least 65 years old or (2) blind or disabled of any age receive Medi-Cal coverage. This group constitutes about 24 percent of the estimated total Medi-Cal caseload for the current year. Overall, the disabled make up more than half (61 percent) of this portion of the Medi-Cal caseload. Most of the aged, blind, or disabled persons on Medi-Cal (80 percent) are recipients of SSI/SSP benefits and receive Medi-Cal coverage automatically.
The other aged, blind, or disabled eligibles are in the "medically needy" category. They have low incomes, but do not qualify for, or choose not to participate in, SSI/SSP. For example, aged low-income noncitizens generally may not apply for SSI/SSP (although they may continue on SSI/SSP if they already were in the program as of August 22, 1996). As another example, some of the medically needy persons have incomes above the Medi-Cal limit and participate on a share-of-cost basis. Included in the number of eligibles in the "medically needy" category are aged, blind, and disabled persons with incomes up to 133 percent of the poverty level. Beginning January 1, 2001, these persons could receive Medi-Cal coverage without a share-of-cost.
More than 900,000, or about 56 percent, of the aged or disabled Medi-Cal eligibles are also beneficiaries of Medicare—the federal health insurance program for persons 65 and older and for younger persons with disabilities who cannot work. Medi-Cal generally pays the Medicare premiums and any copayments or deductibles for these "dual eligibles," and Medi-Cal pays for services not covered by Medicare, such as prescription drugs and long-term care. Medi-Cal also provides some limited assistance to a small number of dual eligibles with incomes somewhat higher than the medically needy standard.
The number of Medi-Cal eligibles in long-term care is small—only 64,400 people, or 1 percent of the total caseload. Because long-term care is very expensive, benefit costs for this group total $2.8 billion, or 12 percent, of total Medi-Cal benefit costs.
Families With Children. Medi-Cal provides coverage to families with children in three eligibility categories. The first two categories were created by Section 1931(b) of the Social Security Act, which required states to grant Medicaid eligibility to anyone who would have been eligible for cash-assistance under the welfare requirements in place on July 16, 1996. One of these categories consists of CalWORKs welfare recipients who automatically receive Medi-Cal. The second category—referred to as the 1931(b)-only group—consists of families who are eligible for CalWORKs, but who choose only to receive Medi-Cal services. The income limit for families in this second category is 100 percent of the federal poverty level (FPL). However, once enrolled in Section 1931(b) coverage, families may work and remain on Medi-Cal at higher income levels (up to about 155 percent of the FPL indefinitely, or a higher amount for up to two years).
A third eligibility category, referred to as the medically needy, consists of families who do not qualify for CalWORKs, but nevertheless have relatively low incomes. These families have incomes up to 80 percent of the FPL, have less than $3,300 in assets, and meet additional requirements. Families whose incomes are above the medically needy limits, but who meet all of the other medically needy qualifications, may receive Medi-Cal benefits on a share-of-cost basis.
About 39 percent of all Medi-Cal eligibles are 1931(b)-only and medically needy families. Although these families constitute the largest single group of Medi-Cal eligibles by far, they account for only 17 percent of total Medi-Cal benefit costs. This is because almost all are children or able-bodied working-age adults, who generally are relatively healthy. Similarly, CalWORKs welfare recipients who receive Medi-Cal account for 22 percent of all Medi-Cal eligibles and only 9 percent of total benefit costs.
Women and Children. Medi-Cal includes a number of additional eligibility categories for pregnant women and for children. Medi-Cal covers all health care services for poor pregnant women in the medically indigent category, which has the same income and asset limits and spend-down provisions as apply to medically needy families. However, pregnancy-related care is covered with no share-of-cost and no limit on assets for women with family incomes up to 200 percent of the FPL (an annual income of about $36,800 for a family of four).
The medically indigent category also covers children and young adults under age 21. Several special categories provide coverage without a share-of-cost or an asset limit to children in families with higher incomes—200 percent of the FPL for infants, 133 percent of the FPL for children ages 1 through 5, and 100 percent of the FPL for children ages 6 through 18. Pregnant women and the FPL-group children also may use a simplified mail-in application to apply for Medi-Cal or Healthy Families Program coverage (for children above the Medi-Cal income limits). Medi-Cal also provides family planning services for women or men with incomes up to 200 percent of FPL who do not qualify for regular Medi-Cal.
Emergency-Only Medi-Cal. Noncitizens who are undocumented immigrants, or are otherwise not qualified immigrants under federal law, may apply for Medi-Cal coverage in any of the regular categories. However, benefits are restricted to emergency care (including labor and delivery). Medi-Cal also provides prenatal care and long-term care to undocumented immigrants. These services, as well as nonemergency services for recent legal immigrants, do not qualify for federal funds and are supported entirely by the General Fund. The Governor's mid-year reduction proposal included changes in eligibility for certain immigrants that are discussed later in this section.
The average cost per eligible for the aged and disabled Medi-Cal caseload (including long-term care) is much higher than the average cost per eligible for families and children on Medi-Cal. As a result, almost two-thirds of Medi-Cal spending is for the elderly and disabled, although they account for only about one-fourth of the total Medi-Cal caseload, as shown in Figure 2.
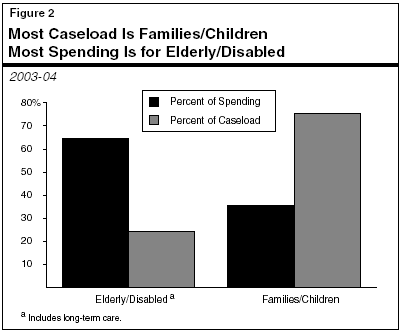
Figure 3 presents a summary of Medi-Cal General Fund expenditures in the DHS budget for the past, current, and budget years.
|
Medi-Cal General
Fund Budget Summarya |
||||||
|
(Dollars in
Millions) |
||||||
|
|
Expenditures |
|
Change
From |
|||
|
|
Actual |
Estimated |
Proposed |
|
Amount |
Percent |
|
Local Assistance |
|
|
|
|
|
|
|
Benefits |
$9,941 |
$9,082 |
$10,825 |
|
$1,743 |
19.2% |
|
County
administration |
509 |
592 |
631 |
|
39 |
6.6 |
|
Fiscal
intermediaries |
103 |
91 |
113 |
|
22 |
24.5 |
|
Totals, |
$10,554 |
$9,765 |
$11,569 |
|
$1,804 |
18.5% |
|
|
|
|
|
|
|
|
|
Support |
$92 |
$95 |
$104 |
|
$9 |
9.9% |
|
Caseload (thousands) |
$6,380 |
$6,620 |
$6,840 |
|
$220 |
3.3% |
|
|
||||||
|
a
Excludes General Fund Medi-Cal budgeted in other
departments. |
||||||
The budget estimates that for the current year the General Fund share of Medi-Cal local assistance costs will decrease by about $789 million (7.5 percent), compared with 2002-03. The bulk of this decrease is for benefit costs, which will total an estimated $9 billion in 2003-04.
General Fund Reduction in 2003-04. The 2003-04 Budget Act decreased General Fund spending from 2002-03 by about $602 million (5.7 percent) with the inclusion of significant one-time savings such as shifting the budgeting for Medi-Cal benefits from an accrual to a cash basis of accounting. The act also included a temporary increase in the federal share of support for the program that reduced General Fund costs in 2003-04 by nearly $570 million.
Mid-Year Reduction Proposals. As noted earlier, a package of mid-year budget reductions proposed by the Governor would result in additional Medi-Cal savings in the current year of nearly $207 million General Fund.
The Governor's budget plan would reduce by 10 percent the rates paid for physician services, pharmaceuticals, dental services, managed care plans, home health care, medical transportation, and certain other medical services. This rate reduction also affects certain non-Medi-Cal programs, including the California Children's Services Program; the Family Planning, Access, Care and Treatment Program; the state-only Family Planning Program; the Genetically Handicapped Persons Program; and the Breast and Cervical Cancer Early Detection Program. The proposed change is expected to reduce state costs by about $160 million in the current year. This rate reduction would be in addition to the 5 percent rate cut included in the 2003-04 Budget Act, and would result in a total rate reduction of 15 percent if adopted. The Governor has also proposed the elimination of a special rate increase for long-term care providers to achieve an estimated state savings of $46 million.
The savings from the two reduction proposals discussed above would be partly offset by a mid-year reappropriation of $60 million General Fund from 2000-01.
The Governor's mid-year reduction package also included several proposals to cap the number of undocumented immigrants, as well as legal immigrants living in the country for less than five years, that receive services from Medi-Cal and the Breast and Cervical Cancer Treatment Program. The budget plan assumes that this proposal will not result in state savings until 2004-05.
January Proposals to Reduce Current-Year Costs. The Governor's January budget plan includes various proposals to achieve a net reduction of $40 million General Fund in the current year. Most of the savings, about $351 million, are attributable to four proposals that are one-time in nature.
The first is a reduction in the amount paid to the Department of Mental Health for mental health services provided to Medi-Cal children and youth, due mostly to the shift from accrual to cash budgeting in 2003-04, but also due to a modest caseload reduction. The second reduction results from the Governor's proposal to modify and delay from 2003-04to the budget year the imposition of a quality improvement fee on managed care plans. Third, the Governor proposes to achieve savings from the recovery of inappropriate payments to the federal government for certain providers. Finally, the budget reflects larger overall savings than expected from the shift in accounting from accrual to cash.
The remainder of the proposals are ongoing in nature. These include a reduction in the interim rate paid to certain hospitals, a change in the methodology used to set rates for clinics, and various rate reductions. Savings of about $26 million would be achieved in the current year, with increased savings expected in 2004-05.
Increased Caseload and Other Costs. The proposed savings discussed above are partially offset by several factors. One of these factors includes greater-than-anticipated growth in the number of children and youth who are participating in Medi-Cal because of the Child Health and Disability Prevention program "gateway" to Medi-Cal, which commenced operation in July 2003 and which is expected to increase costs by more than $39 million.
Other increases in Medi-Cal benefit costs in the current year are due to an increase in the utilization of nursing facilities that is expected to increase state costs by about $20 million and the settlement of three federal audits related to inpatient hospital psychiatric claims that will require the state to repay the federal government about $16 million in 2003-04.
Prepayment of Checkwrite Increases Costs. The Governor proposes that the payments to Medi-Cal providers scheduled for July 1, 2004 be paid instead on June 30, 2004. While this action increases General Fund costs in the current year by $135 million, it would result in one-time savings of $8.5 million in 2004-05. That is because the shift allows the state to take advantage of the temporary increase in federal Medicaid funding that will end in June 2004. The federal government will pay nearly 53 percent of Medi-Cal Program costs until June 30, but will only pay 50 percent of costs as of July 1.
Unrealized Savings Increase Costs. The Governor's budget anticipates that about $91 million in savings from cost-containment activities assumed in the 2003-04 Budget Act will not be realized. If it were not for the current-year reduction proposals there would have been a deficiency in the current year.
The DHS has determined that the delay in the enactment of the 2003-04 Budget Act and the mid-year elimination of budgeted positions have delayed the implementation of certain cost-containment activities, thereby increasing state costs for Medi-Cal services in the current year. Specifically, about $59 million was added to 2003-04 spending because of an anticipated erosion of savings from efforts to reduce fraud, contract for durable medical equipment and lab services, closely manage the care of certain persons, and implement other strategies to recover funds that have been paid inappropriately. The cost increases also include $32 million in savings assumed in the budget act from the addition of staff to resolve aged drug rebate payment disputes. An additional $29 million in anticipated savings in dental services are not expected to be achieved because of a legislative decision to alter a new requirement for X-rays for dental restorations.
The Governor's proposed budget estimates that total General Fund spending for Medi-Cal local assistance will be about $11.6 billion in 2004-05, a net increase of $1.8 billion, or 19 percent, above the estimated spending in the current year. About $1.6 billion of the General Fund increase in spending reflects the budget-year effect of the shift from accrual to cash accounting ($958 million) and the temporary increase in the level of federal funding in 2003-04 ($655 million). Without these one-time savings in 2003-04, the 2004-05 increase in Medi-Cal expenditures from the previous year would be much smaller—$191 million or 2 percent, rather than the much larger increase shown in Figure 3.
Additional increases in expenditures are the result of increases in the price and utilization of services and caseload growth. The budget plan also takes into account an increase in the Medi-Cal caseload in 2004-05 of about 220,000 average monthly eligibles (3.3 percent). This would bring the total number of individuals receiving assistance to 6.8 million—roughly 19 percent of the state's population. These spending increases are partly offset by a series of proposals to reduce program costs through cuts in rates and services and certain one-time savings. Figure 4 summarizes the major components of the change in benefit costs, which we discuss below.
|
Figure 4 Medi-Cal Benefits |
|
|
2004-05 |
|
|
One-Time Increases |
|
|
Funding shift to counties to reduce costs |
$958 |
|
Reduction in federal share of Medicaid funding |
655 |
|
|
|
|
Increased
pharmacy costs |
$253 |
|
Various rate
adjustments |
164 |
|
Increased
cost for Medicare and Medicare HMO premiums |
109 |
|
Nurse to
patient ratios |
31 |
|
Caseload Increases |
|
|
Caseload
shift due to implementation of the Child Health and Disability
Prevention program �gateway� to Medi-Cal |
$110 |
|
Ongoing Savings From
Proposals |
|
|
Additional 10
percent provider rate reductions, revised rates for clinics, and reduced
interim rate for some hospitals |
-$341 |
|
Increased
savings from various 2002 and 2003 proposals to reduce costs for drugs,
supplies, and services |
-184 |
|
Quality
improvement fee for managed care plans (net savings to General Fund) |
-75 |
|
One-Time Savings |
|
|
Checkwrite
prepayment in 2003-04 |
-$278 |
|
Checkwrite
prepayment in 2004-05 |
-144 |
Increased Price and Utilization of Services. In line with a continuing trend that has significantly bolstered Medi-Cal Program expenditures in recent years, the 2004-05 budget plan assumes an increase in the cost of pharmaceuticals of $253 million.
The Governor's budget also includes about $164 million for rate increases for certain clinics and hospitals that offer services to Medi-Cal patients, including the final of a series of rate increases to hospitals that provide outpatient services to fulfill a 2001 legal settlement.
Medi-Cal "buy-in" payments for Medicare premiums would also continue to grow. The Medi-Cal Program pays Medicare premiums for Medi-Cal enrollees who also are eligible for Medicare (dual eligibles) in order to obtain 100 percent federal funding for those services covered by Medicare. The budget estimates that the General Fund cost of these so-called buy-in payments will increase by $109 million in 2004-05.
Chapter 945, Statutes of 1999 (AB 394, Kuehl), requires hospitals to maintain specific staffing levels (established by DHS) for various hospital units, such as critical care units, beginning January 1, 2004. The budget plan includes about $31 million to offset the cost of the mandate for hospitals that provide services to Medi-Cal patients.
In addition to the cost increases identified in Figure 4, costs are also expected to go up for some of the health programs that are passed through the DHS Medi-Cal budget but actually administered by other state departments. Notably, the cost of mental health services administered by the Department of Mental Health, including children's services provided under the Early and Periodic Screening, Diagnosis and Treatment Program, are expected to increase by about $126 million. The increase is due partly to continued growth in program caseload and costs, as well as to technical adjustments related to the shift in Medi-Cal accounting and the anticipated end of a one-time increase in the federal share of cost for the Medicaid Program.
Caseload Increases. The Governor's budget plan anticipates that caseload costs would increase in 2004-05 by $110 million due to the implementation of a program in July 2003 that will preenroll children in Medi-Cal and the Healthy Families Program who are screened for medical problems through the Child Health and Disability Prevention program.
Some of these costs would be offset by the continued effect of steps taken last year to tighten eligibility procedures. Last year's budget plan included provisions intended to reduce caseloads by (1) ensuring that county workers completed redeterminations of Medi-Cal eligibility on a timely basis and (2) establishing a process that requires adult beneficiaries to report on their eligibility for Medi-Cal or be disenrolled from services.
Also, the Governor's mid-year reduction proposal to impose caps on caseloads for various immigrant programs as discussed earlier is expected to result in savings of $23 million in the budget year.
Ongoing Savings From Proposals to Reduce Costs. The spending plan takes into account the estimated ongoing effect of several reductions proposed to reduce rates paid to Medi-Cal providers in the current year and budget year that would achieve combined savings of $341 million in 2004-05.
As discussed above, the Governor's mid-year reduction plan included a 10 percent rate cut in the current year on selected providers in addition to the 5 percent provider rate cut imposed in the 2003-04 Budget Act. The mid-year proposal would achieve a total of $460 million in state savings in 2004-05—$300 million more than the $160 million in savings to be achieved in 2003-04—because they would be in effect for the full fiscal year.
Also included in the Governor's $341 million in proposed savings are two other actions that would reduce rates. One would modify the reimbursement rates for certain clinics that provide services to Medi-Cal patients to achieve estimated savings of $28 million. The proposal would base rates on audited cost reports from 1999 and 2000 rather than on unaudited cost reports from 2000. The budget plan also assumes a 10 percent reduction in the interim amount initially paid to noncontract hospitals that serve Medi-Cal patients (the amounts paid to hospitals are later adjusted to reflect actual costs) for an estimated savings of $13 million.
Additional state savings of $184 million are expected to result from the full-year implementation in 2004-05 of various strategies adopted in the 2002-03 and 2003-04 Budget Acts to reduce costs and utilization for prescription drugs, durable medical equipment, and medical supplies.
The Governor's budget plan proposes to levy a quality improvement fee on managed care health plans. The fee would generate additional revenues of $300 million that would be offset by a $225 million increase in Medi-Cal expenditures to provide a rate increase to health plans, for a net savings to the state General Fund of $75 million. This proposal is a modification of a measure in the 2003-04 Budget Act that the administration indicates could not be implemented in 2003-04 because of federal restrictions.
One-Time Savings. The budget plan assumes significant General Fund savings from one-time actions that shift the timing of payments to providers. One proposal, discussed above, is to shift the provider payment ordinarily made on July 1, 2004 to June 30, 2004 to take advantage of a greater federal Medicaid cost-sharing ratio that expires on the latter date. This shift in payments would have the effect of reducing state expenditures in the budget year by $278 million.
In a separate, but similar action, the Governor's budget plan proposes to delay all other checkwrites to providers during the budget year by one week. Since Medi-Cal is now budgeted on a cash basis, this change would result in one-time state savings of $144 million in 2004-05 because the last checkwrite of the fiscal year would be shifted to 2005-06. The extra week would also allow the department additional time to review the payments to detect fraudulent claims.
Figure 5 illustrates how the Medi-Cal caseload and per-eligible costs have changed since 1994-95, along with projections of these measures for 2003-04 and 2004-05 based on the budget estimates.
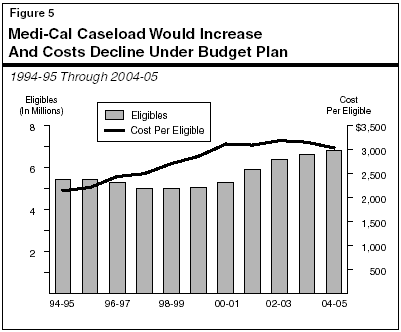
The budget projects that in the current year the number of eligibles will grow and the cost of benefits per eligible will decline. The increase in caseload and decline in the cost per eligible for the program is projected to continue in the budget year.
Caseload. Between 1994-95 and 1996-97, the Medi-Cal average monthly caseload was relatively constant, averaging about 5.4 million eligibles. The Medi-Cal caseload subsequently dropped by almost 300,000 eligibles (5 percent) in 1997-98. The change in the Medi-Cal caseload roughly paralleled changes in the CalWORKs welfare caseload. The caseload began a sharp drop at that time in response to the turnaround in the state's economy, and greater emphasis on moving families from welfare-to-work in the wake of the enactment of state and federal welfare reform legislation. Another factor contributing to declining welfare and Medi-Cal caseloads was probably the reluctance among immigrant Californians to make use of public benefits because of concerns about whether such use might adversely affect their ability to naturalize or to sponsor the immigration of family members in the future.
From 1997-98 through 2000-01, the Medi-Cal caseload remained relatively flat even though the CalWORKs caseload continued to decline. The Medi-Cal caseload did not decline during this period primarily because of the backlog of eligibility determinations for former CalWORKs recipients that resulted from the delay in implementation of Section 1931(b) Medi-Cal eligibility by DHS and the counties.
The caseload began to grow rapidly during 2001-02 and 2002-03 primarily due to a variety of eligibility expansions and simplified eligibility processes. Growth in eligibles is expected to continue in 2003-04 and 2004-05, but at a slower rate.
Cost Per Eligible. The average annual growth rate of the estimated cost of benefits per eligible (excluding pass-through funding to other departments and local governments) is 4 percent during the period of 1994-95 through 2004-05. This is greater than the rate of general inflation during this period (nearly 2 percent) as measured by the Gross Domestic Product deflator.
While the caseload has gone up and down over the past decade, the cost trend per eligible had been almost steadily upward until 2001-02. While the number of families on welfare in the Medi-Cal population declined during this period, the proportion of relatively higher-cost aged and disabled beneficiaries had increased, driving up the average cost per eligible for the Medi-Cal population as a whole.
The turnaround in the trend seen since that time appears to be partly the result of an increase in the number of healthy beneficiaries rather than a decrease in health care costs. The simplification that has occurred in the eligibility process means that the Medi-Cal Program probably is retaining a greater number of children and families on its caseload who do not regularly need health care services compared to other beneficiaries, such as the aged, blind, and disabled.
Based on the Governor's budget plan, these costs would decrease by about 1 percent in the current year and further decrease by nearly 4 percent in the budget year. This decrease can be partly attributed to the Governor's proposals to phase in additional provider rate reductions in the current year and budget year.
We find that the budget's overall estimate for the Medi-Cal caseload is reasonable, but believe that there is both upside and downside risk to the estimate. While it is possible that the population of aged beneficiaries will be greater than budgeted, it is also possible that the population of nonwelfare families and children will be less than assumed in the Governor's budget plan. We will monitor caseload trends and recommend appropriate adjustments at the time of the May Revision.
Figure 6 shows the budget's forecast for the Medi-Cal caseload in the current year and 2004-05. The majority of the projected Medi-Cal caseload increase occurs in the families and children eligibility categories. The budget plan estimates that the caseload for this group will increase by 4 percent in the current year and an additional 3 percent in the budget year. Nonwelfare families account for most of the changes in Medi-Cal eligible families and children. The budget estimates that the caseload of Medi-Cal eligible nonwelfare families will increase by about 7 percent in the current year, and then increase by 6 percent in the budget year.
|
Medi-Cal Caseload |
|||||||
|
(Eligibles in
Thousands) |
|||||||
|
|
|
|
Change
From 2002-03 |
|
Change
From 2003-04 |
||
|
|
2002-03 |
2003-04 |
Amount |
Percent |
2004-05
|
Amount |
Percent |
|
Families/children
|
4,572 |
4,741 |
169 |
4% |
4,890 |
148 |
3% |
|
CalWORKs |
1,549 |
1,479 |
-70 |
-5 |
1,453 |
-26 |
-2 |
|
Nonwelfare families |
2,434 |
2,605 |
171 |
7 |
2,769 |
164 |
6 |
|
Pregnant women |
203 |
208 |
5 |
3 |
215 |
6 |
3 |
|
Children |
386 |
449 |
63 |
16 |
453 |
4 |
1 |
|
Aged/disabled
|
1,549 |
1,617 |
68 |
4% |
1,679 |
62 |
4% |
|
Aged |
584 |
616 |
31 |
5 |
650 |
34 |
6 |
|
Disabled (includes blind) |
965 |
1,001 |
37 |
4 |
1,029 |
28 |
3 |
|
Undocumented
Persons |
259 |
262 |
3 |
1% |
271 |
10 |
4% |
|
Totals |
6,380 |
6,620 |
240 |
4% |
6,840 |
220 |
3% |
Some of the projected current-year and budget-year growth in the nonwelfare families and children caseload is the result of the implementation of a "gateway" in the Child Health and Disability Prevention (CHDP) program. The Governor's budget estimates that efforts to expedite the enrollment of CHDP children into more comprehensive health care coverage will result in nearly 146,000 eligibles being added to the Medi-Cal Program in 2004-05. Additional caseload growth is expected to result from the enactment of two laws in 2003 that simplified eligibility processes for children who receive free meals through the National School Lunch Program or are eligible for Food Stamps.
The overall projection of nonwelfare families and children caseload growth is consistent with past trends. However, the effect of ongoing changes in the Medi-Cal Program is hard to predict and there could be significant revisions to the projection for various reasons. For example, these changes include modifications of eligibility determination procedures adopted in the 2003-04 Budget Act with the intent of reducing caseloads and implementation of the CHDP gateway.
Caseloads for the aged, blind, and disabled are expected to grow by about 68,000 beneficiaries or 4 percent in the current year and by an additional 62,000 beneficiaries or about 4 percent in the budget year. The growth in the current year is due to underlying caseload growth trends as well as a projected increase in caseload due to a Superior Court ruling in a case known as Craig v. Bonta. This ruling requires DHS to provide Medi-Cal benefits to persons terminated from the federal SSI/SSP program retroactively to June 30, 2002.
Caseload increases for the aged are being driven primarily by those aged individuals who qualify as medically needy. This eligibility category is expected to grow by 29,100 or nearly 18 percent to 191,900 in 2004-05. This is a substantially larger year-to-year caseload growth increase than the 7 percent increase that is estimated will occur between 2002-03 and 2003-04. The most recent data that we have reviewed suggest that caseload in this category may be growing even faster than projected and that the current-year and budget-year estimate may understate funding requirements for these eligibles. However, in discussions with DHS, the department has indicated that the most recent data may be skewed by the effect of Craig v. Bonta and that updated information would be provided at the time of the May Revision.
Potential Risks to Accuracy of Caseload Projections and Cost Estimates. The accuracy of the department's caseload projections and cost estimates are dependent upon a number of other more general factors not discussed above. Among the factors that could cause the Medi-Cal program's caseload and costs to vary from the projections are:
Analyst's Recommendation. In summary, we do not recommend any specific budget adjustment for caseload at this time because we believe that there is both upside and downside risk to the estimate. While it is possible that the population of aged beneficiaries will be greater than budgeted, it is also possible that the eligibility determinations and CHDP gateway implementation will result in fewer eligibles than assumed in the Governor's budget plan. Given this situation, we will continue to monitor the Medi-Cal caseload trends and the Legislature's actions on the Governor's mid-year proposals, and will recommend appropriate adjustments at the time of the May Revision.
We will address various aspects of the Governor's estimates of program costs later in this analysis.
As discussed above, the Governor's 2004-05 budget plan proposes a series of actions to help address the state's fiscal problems and operate the Medi-Cal Program. We discuss his proposals to reduce program costs through the establishment of a quality improvement fee for managed care health plans and to cap enrollment for certain groups of immigrant beneficiaries in the "Crosscutting Issues" section of this Analysis. Our assessment of his proposal to transfer eligibility determinations for the Breast and Cervical Cancer Treatment Program to the counties is discussed in the "Public Health" section of this Analysis. Finally, our assessment of his proposals to reduce reimbursements for various Medi-Cal providers, reform the Medi-Cal Program, and increase staff to process prior authorizations for prescription drugs and medical services are discussed below.
The Governor's budget plan proposes a 10 percent rate cut for certain providers in addition to a 5 percent cut enacted in the 2003-04 Budget Act for combined current-year and budget-year state savings of $960 million. There is a significant risk whether the state would achieve this level of savings because of ongoing litigation over the issue. As it considers the Governor's proposal for deeper rate cuts, we recommend that the Legislature examine alternative approaches that would strike a balance between concerns over how such reductions would affect access to care and quality of care for Medi-Cal beneficiaries and the need to address the state's serious fiscal problems.
Further Reductions Proposed. As discussed earlier in this analysis, the 2003-04 Budget Act and related budget legislation adopted a 5 percent cut in the rates paid for physician services, pharmaceuticals, dental services, managed care plans, home health care, medical transportation, and certain other medical services delivered to Medi-Cal beneficiaries. The rate cut, which was to have taken effect on January 1, 2004, was expected to reduce state costs by about $103 million in the current year. The savings in 2004-05 from full-year imposition of the 5 percent reduction would have been roughly $237 million.
As shown in Figure 7, the Governor's mid-year budget reduction package includes a proposal to reduce rates by another 10 percent, bringing the total rate reduction to 15 percent and the total savings assumed in the current fiscal year to $263 million. The Governor's 2004-05 budget plan assumes that the full 15 percent reduction would continue at least through the end of 2004-05 and generate $697 million in savings in 2004-05. The rate reductions would be in effect until January 2007. Thus, the Governor's budget plan, if adopted by the Legislature and upheld by the courts, would result in combined current-year and budget-year savings amounting to $960 million.
|
Provider Rate
Reductions: |
||||
|
(In Millions) |
||||
|
|
Total |
Pharmacy |
Managed Care |
All Other |
|
2003-04 |
|
|
|
|
|
5 percent |
$103 |
$46 |
$31 |
$27 |
|
10 percent |
160 |
92 |
9 |
59 |
|
Totals |
($263) |
($137) |
($40) |
($86) |
|
2004-05 |
|
|
|
|
|
5 percent |
$237 |
$99 |
$62 |
$76 |
|
10 percent |
460 |
199 |
99 |
162 |
|
Totals |
($697) |
($299) |
($160) |
($238) |
|
Two-Year Savings |
$960 |
$436 |
$200 |
$324 |
|
|
||||
|
Detail may not total due to rounding. |
||||
Ruling Blocks Implementation of First Rate Reduction. Litigation initiated by the state's Medi-Cal providers means it is possible that the state will achieve only some of the savings assumed to result from provider rate reductions.
A preliminary injunction issued by a federal district court in December has partly blocked, at least for now, the implementation of the first 5 percent reduction in rates for providers who serve fee-for-service patients. The decision was based on a claim that the rate cuts violated a federal law requiring that the rates paid to Medicaid providers be adequate to ensure quality care and access to care for beneficiaries. The court held that DHS had failed to analyze the potential effects of the rate cut in regard to these factors. The ruling means it is almost certain that legal action will be brought challenging the Governor's proposal to reduce rates an additional 10 percent.
The December court ruling did not apply to all providers who were subject to the 5 percent rate reduction; the cut enacted for managed care health plans was allowed to remain in effect. Thus, as things now stand,
the state would still be able to achieve General Fund savings from managed care rate cuts of at least $40 million in 2003-04 and an additional $160 million in 2004-05 if the Governor's proposal for a full 15 percent rate reduction were adopted by the Legislature. However, managed care plans have filed a "notice of dispute" with DHS challenging the department's rate calculation methodology which, if successful, would jeopardize the potential savings.
The state appealed the court's decision in early January in its entirety, and has also taken steps to attempt to win the immediate reinstatement of at least part of the savings by submitting to the court a DHS analysis of the adequacy of Medi-Cal pharmacy rates that had been completed in 2002. The court is expected to rule on the issue within 60 days of the filing of the appeal. As shown in Figure 7, restoration of the 5 percent rate reduction for pharmacies, and adoption of the Governor's proposal for an additional 10 percent rate reduction for pharmaceutical providers, would enable the state to achieve savings of nearly $436 million over two years.
At the time this analysis was prepared, the Legislature had not yet acted upon the Governor's mid-year reduction proposal, which was to have taken effect in January 2004. Even if the department ultimately prevails on any portion of the litigation and the injunction is lifted, some of the savings assumed in the mid-year proposal from the 10 percent cut would be lost. Federal and state rules do not permit rates to be cut retroactively when providers have not received advance notice of such a change. However, since advance notice was given to providers regarding the 5 percent rate reduction, the savings could be achieved retroactively to January 1, 2004, if this reduction were subsequently permitted by the courts.
Analyst's Recommendation. In our February 2001 report, A More Rational Approach to Setting Medi-Cal Physician Rates, we took note of evidence from health research conducted nationally indicating that the rates paid to medical providers can affect the quality of care and access to care provided to Medicaid patients. We also acknowledged, however, that there is no simple formula that relates rate levels to health care access and quality.
The rate reductions proposed by the Governor, in our view, are likely to have significant effects on the operation of the Medi-Cal Program. The Legislature, however, faces the difficult choice of balancing these concerns against the state's serious fiscal problems.
We would recommend that, as the Legislature examines the Governor's rate cut proposal, it also consider some alternatives that would enable it to strike a balance between these competing concerns. The Legislature could moderate the size of the rate reduction; apply it selectively to certain providers and moderate the impact on others, depending on the available evidence as to how quality of care and access to care might be affected; or further limit by statute the time period the rate reductions would be in effect.
Any of these approaches would diminish at least somewhat the level of savings proposed by the administration from rate reductions. Thus, if it were to reject or significantly modify the Governor's plan, the Legislature should also consider ways to achieve alternative budgetary solutions in order to address the state's fiscal problems. Our office has identified a number of options and recommendations for reducing state costs or increasing state revenues in The 2004-05 Budget: Perspectives and Issues and this Analysis. Such a review of alternative budget solutions may prove necessary, in any event, if the state is unable to overcome legal challenges now pending that could prevent a portion of the provider rate reductions from taking effect.
We recommend rejection of the Governor's request for 36 additional positions to process treatment authorization requests (TARs) because our analysis shows that increasing the number of staff who process TARs is not the most cost-effective way to address the growth in TAR volume. We propose instead steps to give the Department of Health Services the authority it needs to better manage its TARS workload and to improve the TARS process. (Reduce Item 4260-001-0001 by $1 million.)
Governor's Budget Proposal Would Add Staff. State law requires Medi-Cal providers to submit TARs to obtain authorization for reimbursement for specific procedures and services. Some of the services that require TARs include certain prescription drugs, long-term care claims, and inpatient hospital claims. The volume of TARs has increased significantly during the past three years. The number of TAR reviews conducted by DHS increased 17 percent in calendar year 2002, and another 17 percent in 2003. The department anticipates the upward trend in TARs reviews will continue, primarily driven by a surge in the number of TARs submitted for drug prescriptions.
The Governor's 2004-05 budget plan would increase by 36 the number of staff that review prior authorizations for certain prescription drugs and medical services for Medi-Cal patients. The additional staff are expected to cost $4 million ($1 million from the General Fund) in 2004-05. These additional resources would bring the total budget for TARS reviews to roughly $70 million ($20 million General Fund) and the total staffing level to 685.
The budget plan also proposes statutory language that would give DHS the discretion to examine a sample of TARs for medical services and prescription drugs, instead of the current requirement that every such request be reviewed.
Recent Study Found Significant Problems With TARs Processing. A study commissioned last year by the Medi-Cal Policy Institute (which recently became part of the California Healthcare Foundation), a non-profit group which studies Medi-Cal and other state health programs, found significant problems with the Medi-Cal TAR process. Among the study's findings:
Proposed Language and Other Steps Could Reduce TAR Volume. As we noted above, the Governor's budget plan proposes statutory changes to give DHS greater flexibility in terms of how many TARs must be reviewed for certain services and drugs.
Our analysis indicates that this language would be effective in helping the department to better manage its workload. For example, under the proposal DHS could choose to review only a sample of certain drugs, such as over-the-counter drugs, that generate a high volume of prescriptions but that are low-cost and low-risk to patients. Similarly, DHS could spend less staff time reviewing hemodialysis or other services that have high TARs approval rates and are less likely to be abused.
While the legislative changes sought by the administration appear to be warranted, our review of the DHS request for 36 additional personnel indicates that it does not fully take into account the potential reduction in workload and staffing needs that could result from adoption of the statutory changes.
Analyst's Recommendation. Based on our analysis, we believe that DHS could better address the increasing volume of TARs by focusing initially on actions that reduced its workload rather than by increasing the number of staff who process TARs. Accordingly, we recommend that the Legislature adopt the statutory changes proposed by the administration giving the department the discretion it needs to manage this workload more effectively, but deny at this time the request for additional positions. The Legislature could reconsider the request next year after the effect of the statutory changes on TARs workload trends had been determined.
We also recommend that the Legislature direct DHS to take additional steps to reduce its TAR workload. For example, the Legislature may wish to consider directing DHS to conduct routine analyses of the various types of claims subject to TAR reviews based upon such criteria as the medical risks for patients and the costs and benefits of the reviews to the Medi-Cal Program. The DHS should also be directed to implement the SURGE system for pharmacy claims on a statewide basis by the end of the 2004-05 fiscal year.
The Governor's budget plan offers a package of proposals for long-term reform of the Medi-Cal Program that it estimates would achieve General Fund savings of $400 million beginning in 2005-06. In general, the proposal warrants careful consideration by the Legislature given our projections of continued caseload and expenditure growth in the program and the state's fiscal difficulties. However, some key details of the proposal are still lacking. We recommend that the Legislature direct the Department of Health Services to present more detailed information about the reform plan at budget hearings so that it will be in a better position to assess the policy implications and savings that would actually be achieved by the administration's plan. We also recommend changes to (1) the request for staffing and funding to develop the proposal and (2) managed care enrollment procedures.
Two Major Components. The Governor's budget plan presents two major proposals to reform the Medi-Cal Program for the stated purpose of providing the state with the flexibility to meet the essential needs of program beneficiaries at costs that are affordable to the state. The budget plan requests $3.2 million ($1.5 million from the General Fund) for additional resources for DHS to initiate such a reform effort, including 15 positions and funding for two contracts. No savings from the adoption of the proposal are anticipated in the budget year, but the Governor's budget plan estimates that the proposal would result in state savings of $400 million in 2005-06.
We summarize the Governor's two major proposals as follows:
We describe the Governor's proposals in more detail below. However, we note that the administration proposals, at this point, represent only broad and conceptual options for legislative consideration. The budget plan offers few details to explain many aspects of the Governor's plan, indicating instead that these are to be developed by the administration in consultation with the Legislature and "stakeholders" with an interest in the operation of the Medi-Cal Program, such as beneficiaries and providers. In our discussion below, we provide background information that may assist the Legislature in assessing the Governor's plan once more details are forthcoming.
Some Federal Provisions Can Be Waived. The Centers for Medicare and Medicaid Services (CMS), the federal government agency that administers the Medicaid Program, has the authority to grant to states waivers of certain Medicaid statutes to enable them to explore innovative service delivery and financing approaches to providing health care services. Under the Governor's proposal, the DHS would obtain a Section 1115 Medicaid Demonstration Waiver that would allow the state to implement changes in the structure of Medi-Cal.
While the changes proposed in such waivers can be sweeping, they are subject to renewal every five years and states must be able to demonstrate that the changes will not increase federal government costs for the Medicaid program. Some states have already obtained waivers comparable in many respects to the one proposed by the administration.
Medi-Cal Eligibles Could Be Divided Into Categories. The DHS indicates that one element of its waiver request may be to split Medi-Cal eligibles into three categories.
One category would include beneficiaries who are guaranteed eligibility for Medicaid services under federal law. This category would presumably include children and adults who are eligible to receive CalWORKS cash grants and persons who receive SSI/SSP benefits.
A second, separate group could be Medi-Cal eligibles who are mandated to get coverage under federal law except for the fact that their income slightly exceeds federal eligibility standards.
The third category could be "medically needy" eligibles—both children and adults in families to whom the state at its option has chosen, without any federal requirement, to expand health coverage. This category could include families who do not qualify for CalWORKS cash assistance but nevertheless have relatively low incomes.
Benefits Could Vary by Eligibility Category. The administration has suggested that it might seek to create a three-tiered benefit structure that would provide varying levels of benefits for the three categories of eligibles described above. Beneficiaries who received coverage entirely at the state's option, for example, might receive a more restricted package of benefits that more strongly resembled private insurance and that included financial limits on the services covered by the state. Eligibles for whom the federal government mandates health coverage would presumably receive a more elaborate package of Medi-Cal benefits.
Additional Waiver Features Possible. The administration has indicated that it also contemplates an effort through the waiver to simplify and align eligibility standards for Medi-Cal with other programs that assist low-income persons. Another possible waiver component identified by the administration is the implementation of more effective requirements that patients contribute copayments to partly offset the cost of certain services, such as a provision allowing a physician to require a copayment as a condition of receiving nonemergency medical services. The administration is also proposing to seek a federal waiver which would allow it to redefine federal requirements for Early and Periodic Screening, Diagnosis and Treatment, which have been interpreted to require a broad and costly array of services for children and youth.
Costs and Savings From Implementation. The budget plan requests ten additional staff positions for DHS in 2004-05 at a cost of about $700,000 ($350,000 General Fund), as well as an additional $250,000 in funding ($125,000 from the General Fund) for professional consultants, as well as $4.3 million ($1.5 million General Fund) to make changes to existing information technology systems to help prepare this component of the waiver request and to begin to implement a multitiered structure for the Medi-Cal Program. The Governor's proposal indicates that additional resources may be needed for these purposes in 2005-06 and subsequent years. The administration anticipates that these costs will be more than offset by future savings from the implementation of the reforms.
From 22 Counties to 36. Under the Governor's reform proposal, the DHS would also seek to expand enrollment for parents and children in the Medi-Cal managed care system into 14 additional counties that currently operate under the fee-for-service system. This would bring the total number of counties operating under the Medi-Cal managed care system to 36 and result in the transition of about 414,000 beneficiaries from fee-for-service into managed care. Henceforth, enrollment of these families into managed care would become mandatory upon enrollment in the Medi-Cal Program.
This geographic expansion of managed care would require modification of various federal waivers, federal approval of the state's plan, the execution of contracts with additional managed care health plans, and efforts to resolve concerns with the various groups affected by such a change, including beneficiaries and providers.
Costs and Savings From Implementation. The budget plan proposes to increase DHS staff by five to implement this expansion at a cost of $400,000 ($200,000 General Fund), as well as $250,000 ($126,000 General Fund) in additional funding for a state contractor that enrolls Medi-Cal beneficiaries in managed care plans.
The 2004-05 budget plan assumes that no savings would result from the adoption of this proposal in the budget year, due to the time needed to develop a plan, to subsequently secure federal approval of the modification of existing waivers to permit the expansion, and to obtain state and federal approval of nonbid contracts with managed care plans.
Implementation would be phased in beginning in 2005-06. Net savings of $16 million ($8 million from the General Fund) are projected for 2005-06, with annual ongoing savings of $33 million ($16.5 million from the General Fund) anticipated in 2006-07 and thereafter. These savings are based on the assumption that the state will pay capitation rates to health plans equivalent to 95 percent of what it would cost the state to provide medical services to these beneficiaries under the fee-for-service system. The budget plan also assumes some funding would be set aside for a contractor who would be responsible for enrolling beneficiaries in managed care.
In addition to expanding mandatory managed care to families and children, the administration indicates that it will develop a strategy to encourage the voluntary enrollment of additional aged, blind, and disabled persons into Medi-Cal managed care plans.
While we believe the Governor's proposals for expansion of managed care warrant consideration by the Legislature, we do have concerns about three aspects of this proposal.
Some Positions Not Needed Yet. Our review of the Governor's proposals indicates the administration is requesting full and immediate staffing to address a workload that will actually phase in more gradually over the budget year and 2005-06. Specifically, we believe that three of the five positions will not be needed until after DHS has obtained the necessary federal approvals for the expansion and has entered into new contracts with managed care plans. The DHS does not expect these steps to be completed until 2005-06. Deletion of the three unneeded positions from the 2004-05 budget would reduce the DHS request by $200,000 ($100,000 General Fund).
Some Existing Managed Care Plans in Trouble. At least two of the existing Medi-Cal managed care plans (both County Organized Health System [COHS] plans) have indicated that they face serious financial problems. It appears likely that other COHS plans may also encounter problems in the future. At the same time that the administration examines an expansion of managed care, it should also consider what steps the state should take to ensure that the existing managed care system remains financially stable. We discuss this issue and our recommendations to the Legislature in more detail later in this section of our Analysis.
Contractor Costs for Enrollment Could Be Reduced. As noted earlier, the Governor's reform plan would increase funding for the state contractor that enrolls Medi-Cal beneficiaries in managed care. The current three-year contract is scheduled to expire as of September 2004.
The DHS has the option of authorizing three one-year extensions of the contract at an estimated cost of about $50 million per year ($25 million General Fund). The Governor's proposal to expand Medi-Cal managed care into additional counties assumes that this contract will be extended for several years, and further assumes an increase in the cost of the contract of about $7.5 million ($3.8 million General Fund) in 2005-06.
Under the current process that exists in certain counties, a person who enrolls in Medi-Cal is given up to 30 days after enrollment to choose a managed care plan. To assist the enrollee in making this decision, the enrollment contractor mails each participant a package containing information about the health plans in that county at a cost of about $5 per mailing. An identical second enrollment package is sent out later in the month. The state currently spends about $8 million on such mailings each year.
Our analysis indicates that the state could achieve significant savings on the costs of these mailings by allowing new enrollees who have already decided on a health plan to enroll in that plan at the time they apply for Medi-Cal benefits. Such a change would reduce the contractor's mailing and enrollment processing costs and expedite the enrollment of beneficiaries into managed care health plans. We estimate the state would achieve savings in the low millions of dollars annually from such a change.
In general, the administration's proposal to reform the Medi-Cal Program warrants careful consideration by the Legislature, given our projections of continued caseload and expenditure growth in the program and the state's fiscal difficulties. However, many of the details the Legislature needs to fully understand and assess the proposals were not available at the time this analysis was prepared. Consequently, we cannot say at this time whether the proposal will achieve the overall savings level of $400 million in 2005-06 that was estimated in the budget plan. This is also the case in regard to the proposal to establish a multitiered restructuring of eligibility and benefits as part of a federal waiver. For this reason, we withhold recommendation at this time on the request for funding to implement this component of the reform package until more information is available.
According to the administration, additional information about this proposal will be provided to the Legislature at the time of the May Revision. We recommend that DHS be directed instead to present more detailed information about its reform plan at budget hearings prior to the May Revision so that the Legislature will be in a better position to assess its policy implications and the savings that would result from adoption of the administration's plan. The May Revision timeline proposed by the administration is so late in the budget process it may not provide the Legislature with sufficient time to examine the proposal and, if warranted, consider modifications and improvements to the suggested approach.
We also recommend that the Legislature modify the administration's proposal for funding and staffing to expand managed care to delete three of the five positions and $200,000 ($100,000 General Fund) associated with these positions because, as we discussed earlier in this analysis, these resources will not be needed until 2005-06.
We further recommend that the Legislature direct DHS to modify its current arrangements with its managed care enrollment contractor. Specifically, individuals applying for Medi-Cal in managed care counties who have decided on a health plan should be able to enroll in a plan at the same time that they apply for Medi-Cal. The DHS should estimate the potential savings from this change, so that the Legislature can enact an appropriate and corresponding reduction to the Medi-Cal Program budget.
In addition to the concepts proposed by the Governor for reforming the Medi-Cal Program, we believe that the Legislature should consider other opportunities that we have identified to improve the program and achieve savings. These include providing coordinated care to the aged and disabled, simplifying eligibility for families by combining Medi-Cal and Healthy Families coverage, improving the eligibility determination process, studying the impact of Medicare legislation, and advocating for federal changes in the Medicaid Program.
Broader Reform Approach Warranted. The Governor's approach for longer-term reform of Medi-Cal addresses some of the key factors affecting the quality of services and the continuing growth in the cost of the program. Our analysis indicates that this concept, while substantive, does not fully address all of the major problems which affect the operation of Medi-Cal and all of the major "cost-drivers" that are increasing state expenditures for these benefits.
The Legislature may wish to consider a more comprehensive approach to reform that examines other opportunities that we have identified to improve the program and to achieve state savings. These proposals, which are discussed in more detail below, include:
The Legislature should also consider the impact of federal Medicare legislation enacted this fall in its deliberations over how to reform Medi-Cal and consider advocating for federal government changes to the Medicaid Program that could result in a reduction in state costs.
Coordinating Care for the Aged and Disabled to Reduce Costs. The Legislature may wish to consider the concept of expanding enrollment in managed care plans to the group of Medi-Cal beneficiaries who would probably benefit the most from a shift away from fee-for-service coverage—the aged or disabled.
In our companion document to this Analysis, The 2004-05 Budget: Perspectives and Issues, we describe the current Medi-Cal health care delivery system and evaluate its strengths and weaknesses in regard to addressing the health care needs of these beneficiaries. We identify which additional groups of aged or disabled Medi-Cal beneficiaries are good candidates for an expansion of managed care, and offer recommendations to improve the operation of the existing Medi-Cal managed care system that could facilitate their shift from fee-for-service medicine to a more coordinated system of care. Our proposal would go beyond the Governor's plan which proposes to expand managed care chiefly by extending such coverage to families in additional counties.
Restructure Medi-Cal and Healthy Families Into a Family Coverage Model. As the Legislature considers the Governor's reform proposal, it may also want to consider opportunities to combine and restructure the Medi-Cal and Healthy Families programs into a new family health plan that would unify coverage. Many families who are eligible for these programs are not enrolled in them because of their complex and confusing eligibility requirements and procedures. Furthermore, the current structure of the programs often results in situations in which parents and children within the same family must be enrolled in separate programs with differing program requirements and choices of health care providers. We presented a model approach for addressing these concerns in our June 1999 report, A Model for Health Coverage of Low-Income Families.
The model of coverage that we describe in our report could result in increased state costs because there would be an overall increase in the number of persons receiving health benefits. However, this model could be designed so that it would be cost-neutral or result in net savings if the Legislature combined some of its components with some of the strategies for reform that the administration has proposed, such as a multitiered eligibility and benefits package. For example, aligning the health care benefit package that Medi-Cal beneficiaries receive with the benefits offered under Healthy Families coverage, and imposing copayments and premiums for certain beneficiaries, would reduce state costs.
County Eligibility Determinations: Options Exist for Savings. In our discussion of Medi-Cal expenditures in the Analysis of the 2003-04 Budget Bill, we identified significant problems with the present system by which counties administer determinations of program eligibility with funding provided by the state. Our analysis raised concerns about the growing cost to the state of eligibility activities and about the performance of these functions by the counties.
We proposed in that analysis that the Legislature examine several options for reform of this aspect of the Medi-Cal Program, such as centralizing eligibility determinations at the state level using the Internet-based system called Health-e-App. We found that such an approach might significantly reduce the cost of eligibility determinations and ensure greater uniformity in the processing of applications.
Federal Medicare Prescription Drug Reform Act. In December 2003, the President signed the Medicare Prescription Drug Reform Act, a measure that will take full effect on January 1, 2006. The act will result in major changes in both the Medicare and Medicaid programs. Most significantly, the new federal law will require the Medicare program to pay some of the pharmaceutical costs for dual eligibles (that is, Medicare-eligible persons who are also enrolled in Medicaid). Until then, state Medicaid programs, including Medi-Cal, will be responsible (with the help of federal Medicaid matching funds) for the cost of prescription drugs for dual eligibles. The measure also implements a number of other significant program changes, including requirements that state Medicaid programs contribute some state funding to the federal government after drug coverage shifts to Medicare. The measure also increased the premiums charged to persons enrolled in Medicare, which, in some cases, are paid for by Medi-Cal.
Because of the complex and interacting effects of the different provisions of the new federal legislation, its net fiscal effect on the Medi-Cal Program is not clear at this time. We are advised that DHS is now conducting a detailed analysis of how its provisions will affect California. The results of that review and the effect of the law on the way the Medi-Cal Program is operated should be taken into account as reform of the Medi-Cal Program is considered by the Legislature.
Options for Federal Medicaid Reform. Our analysis indicates that reforms could be implemented at the federal level in the Medicaid program which, if adopted, could eventually reduce state Medi-Cal costs by as much as hundreds of millions of dollars annually.
For example, one of these potential changes directly relates to the Governor's Medi-Cal reform proposal to encourage the voluntary enrollment of aged and disabled persons (which may include dual eligibles) into Medi-Cal managed care plans. Currently, the state is somewhat limited in its ability to manage the care of dual eligibles because of the difficulty in coordinating the Medicaid and Medicare programs. Both the federal and state governments might reduce their future Medicaid costs if the federal government changed its rules to allow states to share in savings they were able to achieve through better coordination of care for dual eligibles, such as through disease management services. Because states like California have no way now to share in the savings from such activities, they have little financial incentive to implement such changes.
Analyst's Recommendation. The Governor's plan to reform the Medi-Cal Program intends to address some of the key factors affecting the quality of services and the continuing growth in the cost of the program. In reviewing the Governor's proposal, we believe that the Legislature should also consider other opportunities that we have identified to improve the program and achieve savings. These include providing coordinated care to the aged and disabled, simplifying eligibility for families by combining Medi-Cal and Healthy Families coverage, and improving the eligibility determination process. The Legislature should also consider studying the impact of Medicare legislation, and advocating for federal changes in the Medicaid Program.
The Governor's budget plan assumes that the Health Plan of San Mateo (HPSM), which provides services to roughly 50,000 Medi-Cal beneficiaries, will not be in operation in 2004-05. The HPSM is one of the County Organized Health System (COHS)—a form of managed care—that contracts with Medi-Cal in eight counties. At least two of these plans reportedly face financial problems and others may in the future. The failure of HPSM or other COHS plans could prove costly to the state. Accordingly, we recommend that the Legislature initially reject the administration proposal to budget for the phase-out of HPSM and direct the Department of Health Services to explore alternatives that would permit it to remain in operation. The Legislature should also consider several options to address the COHS plan's financial problems in order to avoid an increase in General Fund costs and the other serious consequences of their loss for Medi-Cal beneficiaries.
COHS Model of Managed Care. The first Medi-Cal managed care system to be organized was the COHS model. (The other two systems are known as the Geographic Managed Care [GMC] model and the Two-Plan model.) The COHS model allows a county to establish a county-controlled health plan to arrange for the provision of medical services, utilization control, and claims administration for Medi-Cal beneficiaries. About 550,000 Medi-Cal beneficiaries received care from COHS plans in 2003. This accounts for nearly 9 percent of all Medi-Cal enrollees and about 16 percent of Medi-Cal managed care enrollees. The COHS model operates in eight counties (Monterey, Napa, Orange, San Mateo, Santa Barbara, Santa Cruz, Solano, and Yolo).
The COHS counties are different from the counties that operate the other two types of Medi-Cal managed care systems in that enrollment in a COHS plan is mandatory for nearly all the Medi-Cal beneficiaries residing in that county. This includes families, children, and aged, blind, and disabled persons. In contrast, enrollment in managed care in the counties that operate the GMC and Two-Plan models is voluntary for aged, blind, and disabled persons but mandatory for families and children. Because the aged, blind, and disabled populations are much more likely to utilize high-cost medical services, COHS plans receive higher capitation rates, on average, than health plans in the other two systems of Medi-Cal managed care.
Some Plans Facing Financial Problems. The COHS plans are subject to licensure under the Knox-Keene Health Care Service Plan Act (Act) by the Department of Managed Health Care (DMHC). In addition, under the Act, COHS plans are obligated to meet certain state requirements meant to ensure their continued financial stability and solvency in order to continue in operation. Generally, these requirements obligate a health plan to demonstrate that it can achieve a positive cash flow from its operations and can show fiscal soundness by assuming full financial risk during its history of operation. If these requirements are not met, DMHC ordinarily would conduct a detailed examination of the health plan and recommend steps that should be taken to ensure the plan's continued operation.
A couple of COHS plans have reported recently to the state that they face a risk of fiscal insolvency within the next several years. One COHS in particular, HPSM, has indicated that it is near to falling out of compliance with DMHC's cash flow requirement. The health plan has proposed to close several times and most recently reported that it will remain open only until the summer of 2004. The Santa Barbara Regional Health Authority (SBRHA) has also reported that it might be unable to meet DMHC's requirements in the near future.
The Governor's Budget Proposal. The Governor's 2004-05 budget plan assumes that HPSM will cease operation at the end of June 2004 and that the county would revert to the fee-for-service system for the delivery of Medi-Cal services in the budget year. This health plan was one of the first Medi-Cal managed care plans and has been serving Medi-Cal patients since 1982. As a result, the approximately 50,000 enrollees would no longer receive services from the managed care plan, but would receive services from fee-for-service providers. We estimate that costs would increase by no more than $30 million ($15 million General Fund) under this proposal because it is more expensive to provide health care services in a fee-for-service system.
We have identified several factors that have likely contributed to the COHS plans' fiscal challenges. These include an outdated capitation rate-setting methodology, capitation rates that we are advised have not kept pace with inflation, the redirection of Medi-Cal "profits" to serve persons and provide services outside of the Medi-Cal system, rates paid to health care providers that are greater than Medi-Cal fee-for-service rates, and DHS' failure to adequately monitor COHS plans' finances.
Rate-Setting Methodology Is Outdated. The methodology DHS uses to determine capitation rates is outdated in that it is based on historical fee-for-service rates rather than any current information about the actual cost of health care services being provided by health plans to individuals in a managed care environment. This means that rates are based on a mix and utilization rate of medical services that may not reflect those of Medi-Cal beneficiaries receiving care from COHS plans. As a consequence, rates could be too high for some beneficiaries and too low for others. The DHS is in the process of changing its rate-setting methodology. However, this may prove difficult, because Medi-Cal data systems do not collect accurate and complete information about the cost and utilization of health care services by COHS patients. These data are critical to setting appropriate rates for COHS plans.
Capitation Rates Reportedly Lagging Inflation. Although COHS plans' rate data are confidential and not available for our review, we have been advised by some plans that their capitation rates have not kept pace with inflation. Thus, COHS plans might be facing financial challenges because they serve large numbers of aged, blind, and disabled Medi-Cal beneficiaries for whom medical costs are generally growing the fastest. These patients are most likely to be heavy prescription drug and hospital users—two of the most rapidly growing components of health care spending.
"Profits" Used for Services and Persons Outside of Medi-Cal. A number of COHS plans have generated some level of excess revenue or profits because, for some years, the cost of the medical services they provided was less than the Medi-Cal capitation rates they received from the state. Some of these profits have gone into COHS plans' reserves and were used to shore up their operations during periods when their expenditures exceeded revenues. However, some plans have also used their profits to expand health coverage to low-income uninsured persons who are not eligible for Medi-Cal, as well as to provide services beyond those ordinarily covered by Medi-Cal. While using Medi-Cal revenues for these purposes is permitted under state rules, it may have resulted in some COHS financially overextending themselves.
Rates Paid to Health Care Providers Are Greater Than Fee-for-Service Rates. Some COHS plans have used the profits that have resulted from high capitation payments to reimburse providers at rates greater than the amount the same provider would have been paid under fee-for-service Medi-Cal. For example, HPSM and SBRHA reimburse providers at 120 percent of Medi-Cal fee-for-service rates. This policy has helped these plans entice additional providers into participation in the Medi-Cal Program and improved access to medical care for Medi-Cal beneficiaries. However, this approach also appears to be creating cost pressures that are contributing to the financial instability of these plans.
Lack of Monitoring of COHS Finances. Another factor that appears to be contributing to the problems now facing some COHS plans is the state's lack of an adequate system to monitor the plans' financial condition for Medi-Cal-specific operations. At present, DHS does not require plans to provide detailed supplemental financial reporting for Medi-Cal activities that would enable the state to fully understand why some of the plans are in financial trouble and to what extent Medi-Cal rates contribute to the problem. The DHS also does not conduct financial examinations and on-site reviews to determine when financial problems exist or the proper remedies when problems are discovered. Under state law, plans are not required to provide such financial reporting and DHS is not required to conduct such in-depth reviews. These types of intensive monitoring activities would also go beyond the current role of DHS and DMHC for regulating the basic financial solvency of health plans.
If COHS plans were, for some reason, to discontinue operation, we have concluded, based upon our analysis, that the resulting shift of Medi-Cal patients from COHS plans to a fee-for-service system would have a negative fiscal impact on the state, could also reduce the access to care for patients, and would eliminate the monitoring of the quality of patient care.
Our analysis focused on a shift to a fee-for-service system, rather than to some other form of managed care, because significant barriers exist to shifting patients to another system of managed care in nearly all COHS counties. These barriers include the lack of other managed care plans in such counties and federal restrictions on the operation of managed care plans absent a federal waiver allowing expansion that could be difficult and time-consuming to secure.
Medi-Cal Program Costs Would Increase. Our analysis indicates that net state costs for the Medi-Cal Program would probably increase if COHS plans stopped operating and, as a result, Medi-Cal beneficiaries in those counties received their care instead from fee-for-service providers.
Enrolling Medi-Cal beneficiaries in COHS plans instead of fee-for-service for their health care has resulted in significant savings to the state. The DHS estimates that Medi-Cal beneficiaries typically receive health care services from a COHS plan at about 81 percent of the cost of fee-for-service providers. These savings would presumably erode if the COHS plans were terminated and replaced with a fee-for-service system. We estimate the closure of HPSM would result in an increase in state costs of $15 million. If all COHS plans ceased operation, the net cost to the state could be as much as $300 million ($150 million General Fund).
The COHS plans save money for the state because the capitation rates paid to them result in an average cost of care per Medi-Cal beneficiary that is less than the equivalent cost of fee-for-service coverage. The plans provide health care services for a lower cost and stay within their capitation rates in part by better coordinating patient care, such as offering prenatal care that subsequently saves on emergency room costs, and by providing preventative care, such as tobacco cessation programs. The COHS plans also help to control the duplicative or unnecessary use of medical services. The fee-for-service system, in contrast, generally allows patients to receive care from any number of providers as frequently as they wish, and does not necessarily ensure that the health care services they do receive are the ones that are medically necessary.
Access to Providers Could Be at Risk. As we noted earlier, the closure of COHS plans would result in a shift of Medi-Cal beneficiaries to fee-for-service health care providers. Our analysis indicates that such a change could reduce their access to doctors and hospitals and in some cases increase the period of time that they would have to wait to receive care.
In some counties, COHS plans reimburse providers at rates that exceed Medi-Cal fee-for-service rates for the same medical services. Upon the closure of such a COHS plan, some providers may be unwilling to treat Medi-Cal patients at fee-for-service rates that were lower than those they previously received for these same patients from a COHS plan. If a significant number of providers opted out of providing care for Medi-Cal patients, access to care could become more difficult for participants in the program.
There is additional evidence (although not necessarily specific to COHS plans) that suggests that a Medicaid managed care approach can increase access to care for Medi-Cal beneficiaries that shift from fee-for-service medicine. One recently published national study found that disabled and aged patients receiving care from fee-for-service providers wait longer for appointments and must travel further to obtain care than those enrolled in managed care. Another recent California study found that patients who are enrolled in Medicaid managed care subsequently experience improved access to care and become less reliant on emergency rooms for routine care.
Several factors help to explain why enrollment in a COHS plan often equates to better access to care for patients than under a fee-for-service system.
First, under program rules, Medi-Cal patients enrolled in managed care (including COHS plans) must be ensured access to a network of primary care and specialist health care providers. Providers participating in the Medi-Cal Program on a fee-for-service basis are not subject to these provisions. Second, health plans licensed by the state (including COHS plans) are required to comply with various state standards to ensure timely patient access to care. Third, federal law requires that Medicaid managed care plans (including COHS plans) take specific steps to help potential enrollees in Medicaid to understand their health care benefits. For example, health plans must make available free interpretation services for enrollees who are not fluent in English, and to publish health plan information in the prevalent non-English language in the area.
Monitoring of Quality of Care Would End. A shift of patients from COHS plans to a fee-for-service system would mean that the state would no longer monitor the quality of their health care.
The DHS, as part of its oversight responsibilities for Medi-Cal managed care plans, including the COHS plans, conducts annual external quality reviews to measure health plan performance in regard to the quality of health care services provided to Medi-Cal beneficiaries. These studies include the measurement of more than 40 individual quality indicators. A summary of health plans performance in regard to these measures is publicly reported annually by DHS. In addition to this process, Medi-Cal managed care plans are rated by the DMHC on their quality (together with their commercial plans) and the results are included in an annual Quality of Care Report Card that is made available to the public on the Internet.
The DHS does not comparably attempt to measure the quality of care that is delivered by fee-for-service health care providers. The state, in effect, assumes that if Medi-Cal beneficiaries do not like the quality of care they receive from one fee-for-service provider, they will seek out another. However, this assumption does not take into account the possibility that the number of fee-for-service providers participating in the Medi-Cal Program could be insufficient to give Medi-Cal beneficiaries a real opportunity to change providers in response to problems in the quality of their services.
There are some strategies counties could pursue on their own to address their financial problems. For example, some COHS plans have indicated that they could improve their fiscal condition through such actions as reducing rates paid to health care providers and pharmacies, and diversifying their revenue sources by providing coverage for other patients in addition to Medi-Cal beneficiaries. To diversify their revenue sources these plans might be able to contract, for example, with counties to provide health care coverage for county employees.
There are other options the Legislature may wish to consider to help address the financial crisis that some of the COHS plans could face in the near future. We would note that the options outlined below are not mutually exclusive. One or more of them could be implemented together. In addition, several of the options would result in additional costs. These costs, however, should be viewed in the context of an even greater cost to the state from the potential failure of COHS plans.
Improve Outdated Rate-Setting Methodology. The capitation rates that COHS plans are paid are an important component of ensuring their financial stability. One option is to ensure that DHS reforms its process for setting rates for capitation payments paid to COHS plans, particularly for their aged, blind, and disabled populations. This would require modifying DHS data gathering systems to collect accurate and complete information about the cost and utilization of services provided to COHS members. To obtain this information, DHS could provide incentives to encourage the plans' submission of complete and accurate data to the state. The DHS could use the improved data to develop appropriate capitation rates.
Given the inadequacy of the data now collected by the state, it is not clear at this time whether these changes would result in a net increase or decrease in Medi-Cal capitation rates.
Reduce the Financial Risk of COHS Plans. One option for helping to ensure the continuation of the COHS plans would be to modify the COHS model to reduce their financial risk. For example, the state could decide that COHS plans would no longer be financially responsible for the cost of some or all prescription drugs, or certain other fast-growing medical costs.
Such a shift in financial responsibilities would result in a reduction in costs for COHS plans and an increase in costs for fee-for-service Medi-Cal expenditures. The exact fiscal impact of such a change is unknown.
Limit COHS Plans Use of Profits for Non-Medi-Cal Activities. As we noted earlier, the state has been allowing Medi-Cal managed care plans, including COHS plans, to use Medi-Cal profits to cover services not available under Medi-Cal and to provide services to persons not eligible for Medi-Cal. To some extent, this issue is dwindling as COHS plans become less able to generate excess revenues. The DHS could be asked to examine whether the state could achieve savings by prohibiting this practice.
Monitor Health Plan Financial Condition. Oversight of COHS plans and other plans that participate in Medi-Cal managed care could be increased in two respects. First, legislation could be enacted that would direct managed care health plans that contract with Medi-Cal to provide supplemental financial reporting for Medi-Cal. Second, legislation could be enacted that would require DHS to conduct regular and thorough independent examinations of the financial condition of these plans. This examination could include on-site, in-depth reviews of health plans, in regard to their administrative efficiency, and operational cost-effectiveness. As we noted above, the DHS does not conduct such reviews at this time. The information obtained by DHS through detailed financial reports and examinations could be used to ensure that problems are corrected before they affect the financial health of COHS plans and the quality of care received by Medi-Cal beneficiaries.
The state should encourage COHS plans to develop their own solutions to their financial problems. However, as our analysis indicates, the loss of COHS plans could result in a significant net increase in state expenditures once clients in failed COHS plans reverted to more expensive fee-for-service coverage. As we have discussed, there could be other consequences too for Medi-Cal beneficiaries—including less access to providers, and an end to regular monitoring of the quality of their care.
As a first step to address this issue, we recommend that the Legislature initially reject the administration proposal to budget for the phase-out of the Health Plan of San Mateo (HPSM). Instead, the Legislature should direct DHS to explore cost-effective alternatives that would permit the HPSM to remain in operation. The DHS should report back to the Legislature regarding the outcome of these efforts prior to the May Revision.
We recommend that the Legislature also consider the options for state actions to help mitigate the financial problems affecting HPSM and other COHS plans. These options include directing DHS to improve its rate-setting methodology for COHS plans, reducing the financial responsibility of COHS plans, directing DHS to examine the plans' practice of using profits for non-Medi-Cal activities, and enacting legislation to increase the state's financial oversight of COHS plans. The Legislature may wish to conduct hearings examining the financial problems of HPSM and the other COHS plans in the appropriate health policy committees, and direct DHS to comment at those hearings on the various options we have identified for addressing these issues.
During the past four years, the Legislature has approved significant increases in resources to combat fraud in the Medi-Cal Program. While these actions have resulted in increased savings and allowed the state to avoid some additional program costs, fraud remains a major concern in the Medi-Cal program. In this analysis, we explain the structure of the Department of Health Services' (DHS) antifraud program and how it compares to national models of fraud control in fee-for-service Medicare and Medicaid. We identify areas in which the DHS could be more effective in combating Medi-Cal fraud and offer recommendations as to how DHS could better manage and structure its antifraud efforts. We also review the Governor's 2004-05 budget proposals for expansion of antifraud efforts and recommend changes. Reduce Item 4260-001-0001 by $2,354,000.
Defining Medi-Cal Fraud. Medi-Cal fraud occurs when either Medi-Cal providers or beneficiaries engage in activities that result in the wrongful expenditure of Medi-Cal funds. Beneficiary fraud generally results when individuals provide false information to become eligible for Medi-Cal or when they otherwise obtain benefits improperly. Provider fraud generally occurs when Medi-Cal providers deliberately misrepresent themselves or intentionally deceive the Medi-Cal program for their own financial gain.
Estimates vary on the amount of fraud in the national health care system and in Medi-Cal. One national expert on the subject has estimated the level of provider fraud in the fee-for-service portion of California's Medi-Cal Program to be roughly 10 percent. This estimate is consistent with those of the U.S. General Accounting Office in regard to the pervasiveness of fraud generally in government health care programs. If that 10 percent estimate were correct, provider fraud in fee-for-service Medi-Cal would total about $1.8 billion dollars in 2003-04, with a loss of about $850 million to the General Fund, before any savings and cost avoidances achieved by DHS through its antifraud efforts were taken into account.
Most indicators point to provider fraud as being a larger concern in terms of its current fiscal impact on the Medi-Cal Program than beneficiary fraud. Provider fraud schemes typically include over-billing, double-billing, billing for services not provided, false claims, and falsification of diagnoses to support billing for unnecessary medical services. In fact, the range of Medi-Cal fraud schemes that have come to light as a result of increased scrutiny during the past few years is extensive. The state has responded with a significant expansion of its antifraud efforts, and has focused mainly on provider fraud.
Federal Requirements. Under federal law, the single state agency administering the Medicaid program, which is DHS for California, is required to conduct investigations of possible fraud and abuse. Where fraud is suspected, DHS is also required by federal law to refer cases to the state's chief prosecutory agency, which in California is the Attorney General. The state is also required by federal law to maintain a separate entity to conduct criminal investigation and prosecution of Medi-Cal fraud, which in California is the State Medicaid Fraud Unit in the Attorney General's office.
The Centers for Medicare and Medicaid Services (CMS), which oversees the Medicaid program at the federal level, issues reports to states providing them guidance and information on "best practices" to follow in their fraud control efforts, and reviews and reports on state antifraud activities. In addition, the Office of Inspector General in the U.S. Department of Health and Human Services assesses and reports on the annual performance of state Medicaid fraud control units.
Antifraud Approaches in Fee-for-Service and Managed Care System. Medi-Cal provides health care services through two basic types of arrangements—fee-for-service and managed care. Fee-for-service is the traditional arrangement for health care in which providers are paid for each examination, procedure, or other service they furnish. The providers bill the state Medi-Cal system for their services and are paid by the state through a state contractor, which is often called a "fiscal intermediary." Most states have focused their antifraud efforts on the fee-for-service part of the Medi-Cal program.
Under managed care, health care plans, primarily Health Maintenance Organizations, contract with the Medi-Cal Program and receive a monthly "capitation" payment or a predetermined monthly amount per-person. The health plans in return assume financial risk for providing a defined package of health care benefits to beneficiaries.
Under this arrangement, physicians and other health care providers are directly paid by the managed care health plans, not the state, as is the case in fee-for-service Medi-Cal. Thus, this arrangement has the effect of shifting most of the burden for detecting and eliminating provider fraud from the state to the managed care plans. A health plan that failed to control provider fraud would place itself at risk of becoming unprofitable, because the state payments to them for beneficiaries are set in advance. We discuss managed care fraud and strategies for addressing this problem in more detail later in this analysis.
Antifraud Program Expansion. As recently as 1999-00, DHS had 89 staff performing functions related to provider overutilization, provider education, and audits for recovery. As can be seen in Figure 8, the state significantly increased its antifraud efforts since that time, beginning in 2000-01.
|
Department of
Health Services |
|||||
|
Positions |
2000-01 |
2001-02 |
2002-03 |
2003-04a |
2004-05a |
|
Change |
192.2 |
-9.0 |
40.0 |
130.5b |
61.0 |
|
Totals |
233.2 |
224.2 |
264.2 |
394.7b |
455.7 |
|
|
|||||
|
a
Governor's 2004-05 budget proposal. |
|||||
|
b
Reflects position reductions resulting from the implementation of
Control Section 4.10 of the 2003-04 Budget Act. |
|||||
The most recent expansion, authorized as part of the 2003-04 budget plan, added 161.5 new positions and $16.5 million ($8.1 million General Fund) to DHS for this effort. However, we are advised by the Department of Finance that 31 antifraud positions have been eliminated in response to Control Section 4.10 of the 2003-04 Budget Act, leaving a net gain of about 131 positions in place. The department is currently in the process of filling these positions. At the time this analysis was prepared, DHS reported that 47 positions had been filled and that hiring offers had been extended to candidates for most of the remaining unfilled positions.
The Governor's proposed 2004-05 budget plan proposes to consolidate 20 auditor positions from the State Controller's Office into DHS to continue ongoing antifraud activities currently performed by an interagency agreement. In addition, 41 more positions would be added to increase the number of field audits of hospitals and related billings. Finally, the Governor's budget plan would convert 15 previously approved limited-term positions that would otherwise expire to permanent status. (We discuss the Governor's proposed expansion in more detail below.)
How DHS Antifraud Efforts Are Organized. The DHS' complement of antifraud staff is distributed among several separate offices and divisions within the department. Most are assigned to the following organizations: (1) the payment systems division; (2) the managed care division; (3) the office of legal services; (4) the licensing and certification division; (5) the Medi-Cal fraud prevention bureau, and (6) the audits and investigations division.
Audits and investigations is the central coordination point for antifraud activities. It tracks fraudulent providers and beneficiaries involved in various fraud schemes, gathers referrals of cases for investigation, analyzes data, audits providers, conducts antifraud investigations, and coordinates antifraud activities with other governmental agencies. It also serves as the central referral point for suspected Medi-Cal fraud to the Department of Justice, the Federal Bureau of Investigation, and other agencies.
State Contracts Out Some Antifraud Activities. In addition to DHS's antifraud staff, the state contracts out some antifraud functions to three separate vendors. Electronic Data Systems (EDS) is the state's Medi-Cal fiscal intermediary, performing the claims processing function. Included in EDS's contract is funding for the EDS's provider review unit that performs antifraud functions. The EDS contract contains an incentive clause that allows EDS to keep 10 percent of the program savings that it generates through its antifraud efforts.
The DHS contracts with Delta Dental, a managed care health plan which processes Medi-Cal dental claims and treatment authorization requests (TARs) for certain dental services, and maintains a surveillance and utilization review unit.
Finally, the DHS also contracts with the MEDSTAT Group, a firm which has developed a database of Medi-Cal claims from all the entities that pay Medi-Cal claims, such as EDS, county mental health, and the Child Health and Disability Prevention (CHDP) program. The MEDSTAT Group uses its database to conduct checks on the existing claim systems and to look for overpayments to providers that may be due to fraud.
"Cost Avoidances" and "Savings." One of the primary measures used by DHS to gauge the effectiveness of its antifraud efforts is the amount of cost avoidances and savings that these efforts generate. A cost avoidance is deemed to have resulted primarily when new providers who are potentially fraudulent are prevented from enrolling in the Medi-Cal Program. Savings are deemed to occur when providers already enrolled in the program are found to be engaging in fraud or abuse and their activities are stopped.
The DHS estimates that cost avoidances amounting to $316 million for the General Fund will be achieved in 2003-04 as a result of the antifraud efforts implemented since 2000-01. These cost avoidances for the General Fund are projected to increase by $93 million in 2004-05 to a total of $409 million. Similarly, General Fund savings are estimated to reach $371 million in 2003-04 as a result of antifraud efforts undertaken since 2000-01, and these savings are expected to grow by $203 million in 2004-05 to $574 million. (Later in this analysis, we discuss whether the savings and cost avoidance estimates are reliable.)
Although the DHS Medi-Cal antifraud program has grown rapidly in recent years, our analysis indicates that these resources have not always been allocated in the most efficient or cost-effective manner. In part, as we will discuss further in this analysis, this is due to a lack of information regarding the pervasiveness of fraud in various aspects of the Medi-Cal program—information critically necessary to targeting fraudulent activity.
California is not alone in the fight against fraud, however. Other states and national experts have studied the problem and identified a number of "best practices" for addressing the provider fraud problem which, as referenced earlier, appears to be the most significant fraud problem at this time. Below we describe a model fee-for-service fraud control strategy, and compare DHS's antifraud efforts with these best practices.
Professor Malcolm K. Sparrow from Harvard's John F. Kennedy School of Government, one of the nation's leading experts on health care fraud, has outlined a model fraud control strategy with seven main components for fee-for-service programs. We summarize these seven components below.
Measure the Prevalence of Fraud. Sparrow indicates that routine and systematic measurement is the foundation of a model fraud control strategy. This requires: (1) the selection of a statistically valid sample of claims; (2) an audit of each claim; and (3) rigorous external validation of the claim information sufficient to identify any fraudulent claims. The important measure is the proportion of total claims paid that are fraudulent—which is assumed to roughly represent the proportion of program costs lost to fraud.
Allocate Resources Based Upon Measurement of the Problem. Under the model fraud control strategy, the amount of resources and personnel dedicated to antifraud efforts should be directly related to the size of the problem as determined by measurement. Under this approach, the state would cease adding resources at the point at which the state would achieve a diminishing return on its antifraud expenditures. In the absence of measurement, Sparrow indicates, antifraud resources are typically based on "best guess" estimates of the size of the problem and the workload increases generated by fraud-detection and referral systems. Neither of these factors necessarily indicates the amount of resources warranted to address the fraud problem.
Clearly Designate Who Is Responsible for Fraud Control. Sparrow indicates that one entity should have overall responsibility for and command of the state's antifraud efforts. A loosely coordinated effort between separate departments and divisions will not result in a coherent antifraud strategy, in his view. Without an overall coordinated approach, he indicates, the state will miss opportunities to achieve efficiencies and in some cases engage in redundant activities. If these functions are dispersed, one governmental division may be unaware that the same work is being done in another division.
Take a Problem-Solving Approach. Sparrow advocates adopting a "problem-solving" approach to fraud control that places emphasis on fraud control rather than on functions such as investigation and detection. Instead of measuring output in terms of caseload, the problem-solving approach focuses resources on the most critical fraud control problems. For example, if a new type of fraud scheme were discovered, the conventional approach might be to focus on detecting additional cases and prosecuting those who were caught. In contrast, under the problem-solving approach, once a specific fraud scheme is identified, the fraud control team's focus would be on developing preventative measures and controls that would make it impossible to continue the fraud scheme and to ensure that it could not be successful in the future. Under this approach, what Sparrow terms the "unit of work" changes from measuring fraud control in terms of caseload, to looking at the overall problem and developing broad-based, permanent solutions. This more flexible approach to fighting fraud is intended to facilitate efforts by state agencies to seek out and identify new and emerging fraud schemes.
Focus on Early Detection. The problem-solving approach allows for early detection and intervention before too much damage is done by fraud schemes. The objective is to discover emerging fraudulent practices so that the control operation can counteract them in their early stages of development. This proactive approach makes identifying emerging problems and taking preemptive action a priority, as opposed to permitting fraud problems to become endemic and antifraud efforts to be reactive in nature.
Strengthen Prepayment Controls. Sparrow indicates that an effective strategy must provide controls that help prevent the loss of state funds in payments to fraudulent providers. This involves, at a minimum, automatic suspension of large payments (above a predetermined amount) pending review of suspicious claims. Providers would also be monitored for sudden increases in the amount of their claims as well as for claim totals that exceed the reasonable norms for their medical specialty. Also, a small proportion of claims should routinely and randomly be selected for validation.
Every Claim Should Face Risk of Review. According to Sparrow, payment systems should be established so that every claim should be at some risk of review regardless of its dollar amount, its nature, or the reputation of the claimant. When prepayment inquiries can be conducted which can show a claim to be suspicious, and can do this quickly, the fraud-control team can then suspend all claims pending from the same source and place them under intense scrutiny. This reduces the vulnerability of payment systems to large-scale computerized billing schemes.
Some Components Missing. How does California's fee-for-service Medi-Cal antifraud effort compare with the model for fraud control described above? Our analysis indicates that the state's existing program contains some of its specific components, but that others are missing or incomplete. Our findings are summarized in Figure 9.
|
LAO�s
Comparison of California�s Antifraud |
||
|
|
Implemented |
Under
Implementation |
|
Commitment
to routine systematic measurement. |
|
� |
|
Resource
allocation based on the seriousness of the problem.a |
|
� |
|
Clear
designation of responsibility for fraud control. |
|
� |
|
Adoption
of a problem-solving approach to fraud control. |
� |
|
|
Deliberate
focus on early detection of new types of fraud. |
� |
|
|
Prepayment,
fraud-specific controls. |
� |
|
|
Some
risk of review for every claim. |
� |
|
|
|
||
|
a
Contingent on implementation of routine systematic measurement. |
||
One of the key antifraud components that DHS is now implementing is an effort to measure the extent of fee-for-service provider fraud within Medi-Cal. Part of the 2003-04 expansion of antifraud activities was for funding and staff positions to conduct an "error rate study" in order to estimate the extent of fraudulent claims through a random sampling process. Since the enactment of the budget plan, the state has received an additional $601,000 in federal funds from CMS to participate in an effort to determine by November 2004 how much of the state's fee-for-service provider payments for health care are not legitimate.
The DHS currently does not have a system to allocate resources based on the seriousness of the problem. However, once the results of the error rate study are available, the DHS will have the information necessary to allocate resources more efficiently. In addition, the DHS currently does not have a clear designation of responsibility for all fraud control activities within the department, according to a recent Bureau of State Audits (BSA) report.
We are advised by the department that it is currently working to implement all the identified components of the model strategy for fraud control. However, until the ongoing study of the prevalence of fraud within the Medi-Cal Program is completed in November 2004, DHS will not have all of the data it needs to implement all components of a model program.
The Model Fraud Control Strategy and Managed Care. The model fraud control strategy outlined above applies primarily to fee-for-service Medicaid programs. However, Sparrow indicates that some components of the strategy apply equally well to managed care plans. For example, the idea that fraud-control resources should be allocated in accordance with measurements that objectively determine the size and seriousness of the problem is equally as true in managed care as it is for fee-for-service medicine.
Some differences in approach, however, are necessary. In traditional fee-for-service cases, Medi-Cal provider fraud investigations typically focus on the overutilization of services and fraudulent billings. Fraud in managed care typically involves the unwarranted delay of care or denial of care to beneficiaries, practices that encourage the underutilization of services. In essence, this is an intentional violation of the managed care company's contract with the state to provide specified health services. To ensure that the managed care organizations are fulfilling their contractual obligations, the DHS already has some measures in place to monitor whether managed care providers are promptly delivering appropriate care. However, the state does not collect reliable encounter data—records of the health care services provided to beneficiaries that managed care plans are required to report. The data now being collected from health plans are often incomplete.
Fraud can also be committed against the managed care organization by providers or beneficiaries that, as we noted earlier, can negatively affect the health plan's profitability. The health plans thus have a strong incentive to control this type of fraud in order to remain profitable. However, this does not mean that the health plans will necessarily be effective in controlling fraud within their own organizations, nor does it mean that they will not commit any fraud themselves.
Effectively Targeting Managed Care Fraud. The CMS, the federal agency that oversees state Medicaid programs, has identified six broad areas in which fraud and abuse pose a risk for managed care systems. These are: (1) improper procurement of managed care contracts; (2) misleading consumers to get them to enroll in managed care programs while inappropriately disenrolling high-cost beneficiaries; (3) causing an underutilization of services by making them unduly difficult for legitimate beneficiaries to obtain; (4) the submission of improper claims and improper billing procedures; (5) fee-for-service type fraud by providers against health plans; and (6) embezzlement and theft.
None of these schemes involves the submission of false claims directly to the state, as is typically seen under fee-for-service fraud. Thus, many of the detection and investigative strategies and techniques developed to combat fee-for-service fraud are largely ineffective against the abuses that are more typical in a managed care setting.
Some Antifraud Controls in Place. There are currently some measures in place to ensure that health plans fulfill their contractual obligations to provide care. Medi-Cal managed care health plans are obligated to report information about the quality of the services they are providing to beneficiaries according to a commonly used Health Plan Employer Data and Information Set standards. The DHS conducts the Consumer Assessment of Health Plans Survey to assess Medi-Cal members' satisfaction with their health coverage. In addition, most Medi-Cal managed care plans are Knox-Keene licensed and regulated by the state's Department of Managed Health Care.
More Could Be Done. As noted earlier, fraud in managed care typically involves the unwarranted delay of care or denial of care to beneficiaries. The DHS does monitor managed care organizations through the measures described above. However, a recent BSA report recommended that the DHS complete an assessment (now under way) of how it can use encounter data to monitor managed care plan performance and identify areas where it should conduct more focused studies to investigate potential plan deficiencies. Our analysis indicates that, without reliable encounter data, DHS does not have sufficient information to adequately determine whether or not managed care providers are promptly delivering appropriate care.
According to federal guidelines for addressing fraud in Medicaid, accurate and complete encounter data should be used to monitor utilization of health care, access to care, and the quality of care. In addition, encounter data can be used as a management tool to monitor whether managed care companies are in compliance with their contract terms.
The state's antifraud program has periodically expanded during the past four years in reaction to growing concern about the level of fraud in the Medi-Cal Program. A recent examination by the BSA concluded that antifraud activities are not adequately coordinated within DHS. As described above, antifraud functions are spread across several units at DHS and require coordination with other state, local, and federal agencies. Notably, the DHS was unable to provide an organization chart identifying specific positions dedicated to antifraud activities within various DHS units. Thus, we agree with the BSA report and believe the lack of coordination is partly due to the rapid expansion of the program. Given the size of the program and the potential magnitude of the fraud problem, the state should consider a systematic, coordinated, and long-term approach to curtailing Medi-Cal fraud in keeping with legislative intent and the recommendations of national experts and federal agencies.
Strategic Planning Necessary. The approach we propose would be in accord with CMS guidelines, which suggest that each state Medicaid agency should identify all of the state's fraud and abuse prevention and detection activities, its key partners and stakeholders, and their respective roles and responsibilities. The CMS guidelines indicate that antifraud measures should apply to both fee-for-service and managed care coverage; should include clearly defined, measurable goals and outcomes for antifraud activities; and should include systems to measure and assess areas of vulnerability to fraud and ways to address them. These CMS guidelines are intended to ensure that the state's antifraud efforts are comprehensive, coordinated, and that any future increase in funding and positions are at appropriate levels. The "model fraud control strategy" we described above is aligned with CMS guidelines.
Savings as a Measurement of Effectiveness. The DHS currently measures the effectiveness of its antifraud efforts in terms of savings and cost avoidances. Effective antifraud efforts do result in savings and an avoidance of costs. However, the recent BSA audit found the DHS estimates are unreliable and, in some cases, potentially overstate actual savings.
Instead of measuring the effect of antifraud efforts just in terms of savings, the effectiveness of antifraud activities should also be measured on an ongoing basis against the overall extent of fraud.
Specifically, the performance of a fraud control unit could be measured by its success in lowering or suppressing the level of fraudulent claims the system pays, a factor which could be measured periodically. A target level for prevalence of fraud within a particular part of the Medi-Cal Program could be set, and lowered over time.
Fight Against Fraud Requires Realistic Expectations. Increasing resources to combat Medi-Cal fraud will not usually produce overnight results, but is more likely to pay off in the long run. For example, the expansion of 161.5 antifraud positions approved by the Legislature last year is projected to generate $20 million in General Fund savings in 2003-04, but is expected to provide more than triple that level of state savings—about $75 million—in 2004-05.
Savings can take time to achieve because of the sometimes lengthy process involved in hiring additional staff, training the staff, and placing them in the field where they can begin to have an effect on fraud. For this reason, expansion of antifraud activities does not tend to have a significant immediate impact, and expansions should be carefully planned and considered based on their long-term impact on the Medi-Cal Program.
Achieving several hundreds of millions of dollars in additional antifraud savings annually from such efforts may be an appropriate long-term goal for the Medi-Cal Program. But it is highly unlikely that such an outcome could be achieved as a short-term solution to the state's current fiscal difficulties. Later in this analysis, we make recommendations as to how the state could improve the overall effectiveness of its efforts by taking a systematic and coordinated long-term approach to addressing the fraud problem.
Nine New Antifraud Initiatives Proposed. The Governor's 2004-05 budget plan includes nine initiatives to combat Medi-Cal fraud. Three of these would provide an increase in resources for DHS, either through shifts of personnel from other departments, adding staff and funding, or the conversion of limited-term positions that would otherwise expire to permanent status. The proposals are as follows:
Five additional antifraud initiatives proposed in the 2004-05 spending plan are to be accomplished within DHS' existing resources. These include:
In addition to these antifraud efforts that would be implemented during the budget year, the Governor's budget plan proposes to implement counterfeit-proof prescription pads in 2005-06 to reduce forgery and altering of prescriptions. The significant lead-time to implement this change means that it is projected to result in no savings in 2004-05, but savings to the General Fund in 2005-06 are expected to range between $7 million and $14 million.
Hospital Auditing Positions Appear to Be Premature. We believe all but one of the Governor's antifraud proposals warrant approval by the Legislature at this time. The exception is the proposal to add 41 auditors to the DHS staff in 2004-05 to conduct additional reviews of hospital claims.
As noted above, the Legislature authorized a total of 161.5 additional positions for antifraud activities for 2003-04. At the time this analysis was prepared, we were advised that DHS was still recruiting and filling many of these positions. As a result, we believe it would be premature to approve further expansion of the DHS audits and investigations unit before the department has fully implemented the sizable expansion approved for the prior year and demonstrated that it can achieve the savings that were to have resulted from these additional positions. This further expansion should also wait until the error rate study is completed that will shed light on which types of antifraud activities warrant a greater focus.
Our analysis has identified areas in which the Department of Health Services (DHS) could improve the overall effectiveness of its antifraud efforts by taking a systematic and coordinated long-term approach to addressing the fraud problem. Based on these principles we recommend: (1) denial of the Governor's proposal to increase staffing for audits of hospitals; (2) that DHS report at budget hearings regarding how encounter data could be used to prevent managed care fraud; and (3) increased legislative oversight of DHS antifraud efforts through additional reporting requirements.
Specifically, we recommend the following actions:
Governor's 2004-05 Antifraud Initiatives. We recommend that the Legislature deny the Governor's proposal to expand hospital audits at this time. Any significant increase in DHS staffing to expand the audits and investigations unit, in our view, should await the outcome of the error rate study which will allow the DHS to identify specific fraud problems and target resources in the most cost-effective manner. At that time, the Legislature will have the additional data it will need to determine whether further expansion of the state's antifraud program is justified or whether resources already provided for the overall antifraud effort should be redirected within the program to expand audits of hospitals.
We recommend approval of all of the Governor's other budget proposals.
Improved Encounter Data Could Help Reduce Fraud in Managed Care. We recommend that DHS be directed to report at budget hearings regarding how it could improve the accuracy and completeness of encounter data from managed care plans, and how that data could be used to monitor the performance of managed care and prevent fraud.
Improve Legislative Oversight to Ensure Strategic Planning. We recommend that the DHS be directed to report to the Legislature by January 2005 regarding: (1) the results of the error rate study, (2) its proposed fraud reduction targets established in response to the data from the error rate study,(3) the proposed timeframe for achieving these targets, (4) the cost-effectiveness of ongoing antifraud activities, and (5) DHS' progress towards implementing the components of a model fraud control program.
Adoption of the following supplemental report language is consistent with this recommendation:
The Department of Health Services (DHS), shall report to the Chair of the Joint Legislative Budget Committee and the chairs of the fiscal committees for both houses of the Legislature, information regarding the state's Medi-Cal antifraud program. The DHS shall include, but not be limited to (a) the results of the error rate/payment accuracy measurement study, (b) fraud reduction target(s) that have been established based on the data from the error rate/payment accuracy study, (c) the time frame for achieving the target(s), (d) the cost-effectiveness of antifraud activities, and (e) progress towards implementing the components of a "model fraud control program." The department's findings shall be reported to the Joint Legislative Budget Committee and the fiscal and policy committees of both houses of the Legislature by January 1, 2005.
A Department of Finance (DOF) audit has raised significant concerns about how the Department of Health Services (DHS) is managing a more than $230 million a year contract for Medi-Cal claims processing activities. Although DOF's audit unit presented recommendations to address the weaknesses identified by its review, our analysis indicates that there has been insufficient follow-up efforts to ensure that DHS implements the necessary changes. We recommend that the Legislature take steps to ensure that DHS is held accountable and that the problems identified in the audit are fully addressed.
Background. The DHS contracts with a private firm, EDS, for claims processing services and other Medi-Cal Program functions related to the management of the Medi-Cal Program. An audit was conducted by the Office of State Audits and Evaluations (OSAE), a DOF auditing unit, last year because of concerns about the growing scope, size, complexity, and cost of the California Medicare/Medi-Cal Information Systems (CA-MMIS), the information technology system maintained and operated by EDS to carry out these functions.
State payments to EDS have risen about 23 percent a year during each of the last five years. Total payments to EDS are expected to be $232 million ($69 million General Fund) in 2004-05.
OSAE Audit Findings. An audit completed in June 2003 by OSAE raised significant concerns with regard to DHS' management of the EDS contract. The audit found weaknesses in DHS' oversight of the contract that, in our view, raise a concern that the state could potentially overpay the contractor for the services it provides. Some of the key audit findings were as follows:
DHS Has Taken Some Steps, But More Are Needed. The DHS submitted to OSAE its response to the audit in December 2003. The response indicates that DHS is in agreement with the findings and recommendations, and identifies some steps that it will take to comply with the audit's recommendations. However, in respect to many of the recommendations, DHS generally notes its agreement but does not indicate what specific steps it will take to implement the recommendation.
At the time our analysis was prepared, OSAE had not required DHS to submit a corrective action plan or reports about its progress towards implementing the recommendations, an approach we understand is customary for most OSAE audits. The DOF has indicated that it will instead monitor DHS' management of the contract through the state budget process. The DHS also has indicated that it does not intend to develop a corrective action plan on its own.
We are concerned that this approach will prove insufficient to ensure that DHS corrects the problems identified in the audit and is held accountable for achieving progress in these efforts. For example, absent the preparation of a corrective action plan, DHS will lack a standard management tool to guide its audit compliance activities and to ensure that the department's strategy to implement the recommendations has been thoughtfully developed and therefore more likely to be successful. In addition, the lack of such a plan or any regular reporting on audit compliance activities we believe prevents OSAE and DOF budget staff from being able to effectively monitor DHS' progress toward implementation of the OSAE recommendations.
Analyst's Recommendation. The OSAE audit indicated that, absent corrective action, the state is at risk for overpaying EDS for Medi-Cal Program activities. Accordingly, we recommend that the Legislature adopt supplemental report language directing DHS to develop and submit a corrective action plan to OSAE and the Legislature, and submit reports to OSAE and the Legislature every six months, beginning July 1, 2004, regarding its progress towards implementation of the audit recommendations. In addition, we recommend that the Legislature request BSA to conduct a follow-up audit by July 2005to assess DHS' progress towards improving the management of its contract with EDS.
The following supplemental report language is consistent with this recommendation:
It is the intent of the Legislature that the Department of Health Services (DHS) develop and submit a corrective action plan to the Department of Finance's Office of State Audits and Evaluations and to the Legislature that identifies the actions it plans to take toward implementing the recommendation described in the report entitled, "Final Audit Report—Examination of the Department of Health Services Fiscal Intermediary Contract With Electronic Data Systems for Medi-Cal Claims Processing." It is also the intent of the Legislature that on July 1, 2004, January 1 and July 1, 2005, that DHS submit semiannual reports to the Office of State Audits and Evaluations and to the Legislature regarding its progress towards implementation of the audit recommendations. The legislative reports shall be provided in writing to the Chair of the Joint Legislative Budget Committee and the chairs of the fiscal committees of both houses of the Legislature.
Los Angeles County has been receiving additional funding from the state and federal government under a federal waiver project to help financially stabilize the county's health care system. The Legislature provided funding to the Department of Health Services (DHS) for an independent contractor to monitor the project. However, this contract was recently terminated. We recommend that the Legislature take steps to ensure that DHS will continue to adequately monitor the project.
Background. At the start of the 1995-96 fiscal year, Los Angeles County faced a $655 million budget deficit in health services operations and the potential collapse of its medical "safety net" programs. Basically, these programs provided health care services to low-income individuals who were also uninsured. State, federal, and county officials collaborated to develop a five-year plan to address the crisis by financially stabilizing the county health system and, over time, moving it away from expensive hospital-based services toward community-based primary care and preventative services. The federal government approved the plans as a Medicaid demonstration project that was to end during 1999-00.
The project was renewed for another five years for the period of 2000-01 through 2004-05 and included $900 million in federal funds that would be phased out over the five-year extension period, $150 million in state funds, and $400 million in county funds.
According to the county, it has met many of the reform objectives. However, without a further extension of the demonstration project or alternative revenues, the county anticipates its public health care system will face future budget shortfalls. The county estimates its health services budget will have a positive balance in the current year through 2005-06, but will incur shortfalls beginning in 2006-07 that will grow to $655 million by the end of 2007-08.
State Monitoring Effort Reduced. Unlike the previous waiver, the most recent waiver required the state to provide a General Fund contribution estimated to be about $30 million annually. Given the state's financial commitment and vested interest in the county's success in establishing a more cost-effective and efficient health care system, DHS committed to hiring an independent contractor to measure Los Angeles County's compliance with the waiver goals.
To date, the contractor has submitted two draft annual reports to DHS for fiscal years 2000-01 and 2001-02. It is anticipated that these two reports will be finalized within the next 60 days, at which time they will be made available to the Legislature. In addition, DHS expects to receive one additional status report. However, no further activities by the contractor will occur, we have been advised, because DHS has terminated the contract as of November 2003 as part of an overall response to a requirement in Section 4.10 of the 2003-04 Budget Act for reductions in state program operations.
Lack of Oversight Could Place State at Risk. The threat of growing deficits for the Los Angeles County health care system beginning in 2006-07, and the anticipated phase-out of hundreds of millions of dollars in annual federal subsidies puts the state at risk of being called upon to provide substantial financial assistance to the county after the waiver program expires. The DHS has indicated that, despite its termination of the monitoring contract, it intends to use its own staff to conduct limited monitoring of the county's demonstration project activities. The DHS indicates that this will involve reviewing documents, participating in conference calls about the project, and attending oversight committee meetings.
However, it is not clear that this level of oversight will be adequate or as rigorous as the Legislature had intended when it approved funding for the contractor. For example, the contractor had been expected to monitor the county's procedures for ensuring that health care providers have adequate training and qualifications. It does not appear that DHS will perform these more detailed monitoring activities.
Analyst's Recommendation. It appears likely that the termination of the contract will reduce the state's oversight of the Los Angeles County project. Given the state's major stake in the county's success in transitioning to a financial stable health care system, we recommend that the Legislature take steps to ensure that DHS continues to adequately monitor these efforts. Specifically, we recommend that DHS be directed to report at budget hearings on the findings of the final monitoring reports prepared by the contractor. The Legislature should also direct DHS to provide more detailed information on the specific monitoring activities it will carry out during the remainder of the project to help ensure that the goals of the restructuring effort are met.