Legislative Analyst's Office, November 28, 1995

Background Information on
The Health Care "Safety Net"
California's Health Care Delivery System
Currently, Californians receive health care services through a variety of
mechanisms:
- Private Insurance and Medicare. For the most part, individuals
under the age of 65 receive health insurance through their employer or the employer
of a family member. Most persons over 65 and certain disabled persons receive
coverage under the federal Medicare program. Most insured individuals pay for a
portion of their care out-of-pocket through deductibles (where the individual pays a
certain amount each year before the insurance pays benefits) and co-payments (where
the individual pays a certain percentage or a fixed fee each time he or she uses
services).
- Medi-Cal. The state, with assistance from the federal govern
ment, funds health coverage for certain low-income individuals through the Medi-Cal
program. Most of the recipients are members of families with dependent children or
are aged, blind, or disabled.
- Services for Persons Without Health Coverage. Persons who are
without health insurance and are ineligible for Medi-Cal or Medicare must buy
services on a pay-as-you-go basis. They often cannot afford to pay for the services
they receive. For the most part, private providers attempt to avoid incurring
costs for clients who cannot pay for services by referring them to public programs, if
feasible. However, they generally have been able to recoup the costs they incur for
providing these services by increasing charges to insured clients. Public
providers support their costs for providing services to persons who are unable to
pay through a variety of governmental programs collectively referred to as the safety
net. Some private nonprofit providers, such as community clinics, supplement public
services to persons without coverage using funds available from safety net programs
and private grants.
What Is the Safety Net?
California's health care safety net represents the health-related services provided
through counties for persons who lack health insurance or other coverage, such as
Medi-Cal, and cannot pay for health services rendered. Although the state provides a
host of health services through its Medi-Cal and various public health programs,
counties are ultimately responsible for serving those with no other means of public or
private support, as stipulated under Section 17000 of the Welfare and Institutions
Code.
Who Uses the Safety Net?
According to hospital discharge data from the Department of Health Services' (DHS)
Medically Indigent Care Reporting System (MICRS), the state served roughly 1.7
million medically indigent persons in 1992-93 (latest data available). The data show
that a majority of those served: (1) received outpatient services, (2) received services
in Los Angeles County, and (3) were identified as Hispanic. Furthermore, those
receiving indigent care were categorized into these three age groups: 31 percent
below the age of 21, 34 percent between the ages of 21 and 34, and 35 percent age 35
or older.
How Much Does the Safety Net Cost?
Figure 1 shows the amount of state and county expenditures on indigent health care
in 1992-93 -- the latest year in which complete data are available from the DHS. The
department indicates, however, that these data may not be reported by the counties
on a consistent basis. It is not clear, for example, how the expenditure of federal
disproportionate share hospital funds is reported by the counties.

How Has the Safety Net Been Funded?
Funding for the "safety net" has been provided through several different sources over
the years. Below, we describe the major funding sources:
- County Health Services (AB 8 Program). This state program was
established in 1979 in the aftermath of Proposition 13. The AB 8 Program provided
counties block grants to support public health services and inpatient/outpatient care
for low-income persons. In order to receive their full share of state County Health
Services funds, counties were required to provide matching funds based on their
1977-78 health care expenditures, adjusted for inflation and population growth. In
1991, realignment legislation replaced state funding from the County Health Services
program with funds generated from an increase in vehicle license fees (VLF) and
sales taxes.
- Medically Indigent Services Program (MISP). This state program
provided funds to serve the medically indigent adult population for larger counties.
The state established MISP along with the County Medical Services Program (CMSP)
in 1983, when it transferred responsibility for the medically indigent adult (MIA)
population from the state's Medi-Cal program back to the counties. To support this
transfer, the state provided MISP and CMSP counties with General Fund support
equal to 70 percent of the expected cost of serving the MIA population under
Medi-Cal. Eligibility standards and benefit levels varied significantly among MISP
counties, with some offering benefits below those previously provided under the
Medi-Cal program. Realignment in 1991 repealed the MISP and replaced it with
funds generated from an increase in vehicle license fees and sales taxes.
- County Medical Services Program . This state program provides
funds to smaller counties that chose to contract with the state to administer their MIA
programs. The realignment legislation in 1991 transferred responsibility for the CMSP
from the state to the counties, significantly reducing state General Fund support and
replacing it with revenues generated from an increase in vehicle license fees and sales
taxes. Prior to realignment, the CMSP offered medical benefits similar to the
Medi-Cal program; but shortfalls in revenues required the CMSP counties to reduce
provider rates and eliminate certain benefits in 1992.
- State Legalization Impact Assistance Grants (SLIAG). The
federally funded SLIAG reimbursed states for the expenses incurred in assisting
newly legalized persons pursuant to the Immigration Reform and Control Act of
1986. A portion of SLIAG funds was allocated to counties for indigent health services
from 1988-89 through 1994-95.
- Proposition 99. The Tobacco Tax and Health Protection Act of
1988 (Proposition 99) allocates a portion of tobacco tax revenues for county health
services. In 1989, the Legislature established the California Healthcare for Indigents
Program (CHIP) and the Rural Health Services (RHS) Program, which allocate
Proposition 99 funds to expand county indigent health services. In order to receive
CHIP or RHS monies, however, counties must spend a certain level of general
purpose revenues for health services, as specified in statute. Proposition 99 support
for counties has been declining, due to decreasing tobacco tax revenues.
- Realignment. In 1991, the state transferred much of its fiscal
responsibility for health services programs to the counties as part of a "realignment"
of state and local programs. Specifically, the state eliminated funding for the AB 8
Program and MISP, and significantly reduced its support for CMSP. Realignment
legislation replaced those funding sources for counties with revenues derived from an
increase in the state sales tax and the VLF, provided counties continued to spend
their AB 8 match amounts and dedicate their VLF funds for health services.
- County General Funds. In order to receive their realignment
funds and full share of Proposition 99 revenues, counties are required to maintain a
minimum level of county spending on indigent health care, as specified in statute.
Some counties, however, spend more on these services than is statutorily required.
- Disproportionate Share Hospital (DSH) Supplemental Payment Programs.
California has established two programs to provide supplemental
Medi-Cal payments to certain hospitals that provide services to disproportionate
numbers of Medi-Cal and other low-income patients. These programs were estab
lished to assist safety net hospitals in meeting the uncompensated care costs associ
ated with the provision of medical services to uninsured and underinsured patients.
- The SB 855 Program. Chapter 279, Statutes of 1991 (SB 855,
Robbins) established the SB 855 Program. The program, administered by the DHS,
provides supplemental payments to hospitals that serve disproportionate numbers of
low-income individuals. Under the program, public entities that operate
disproportionate share hospitals -- such as counties, special districts, and the Univer
sity
of California system -- are required to transfer funds to the state by means of
intergov
ernmental transfers. These funds are combined with matching federal funds and
redistributed as supplemental payments to all eligible disproportionate share
hospitals, including private hospitals. A hospital may qualify to receive DSH pay
ments if its Medi-Cal inpatient utilization rate exceeds an established threshold or it
uses a minimum percentage of its revenues to provide health care to Medi-Cal and
uninsured patients. Total supplemental payments -- intergovernmental transfers
(county funds) plus matching federal funds -- have grown from $1.6 billion in
1991-92
to $2.2 billion in 1994-95 and are capped at that level by federal law.
- The SB 1255 Program. The California Medical Assistance
Commission (CMAC) administers the SB 1255 Program, established by Ch 996/89 (SB
1255, Robbins). The program provides supplemental payments to certain eligible DSH
hospitals -- generally hospitals that (1) are licensed to provide emergency medical
services and (2) contract with CMAC to serve Medi-Cal patients under the Selective
Provider Contracting Program. Like the SB 855 Program, intergovernmental transfers
are made by public entities, but these transfers are voluntary in the SB 1255
Program. These funds are combined with matching federal funds and redistributed
by the CMAC as supplemental payments to eligible hospitals (including private
hospitals) that demonstrate a need for additional funds.
Major Shifts in Safety Net Funding
Several shifts have occurred within the state's health care safety net over the past five
years.
- Realignment Revenues Lower Than Projected. The 1991 realign
ment legislation fundamentally changed the state and county fiscal relationship.
Although intended to be revenue neutral, realignment resulted in lower than ex
pected funding levels for county indigent health programs. As Figure 2 shows, the
level of realignment revenues initially anticipated for 1991-1992 was not achieved
until 1994-95.

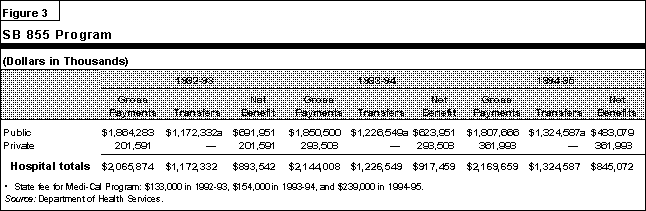
- The SB 855 Program. Figure 3 shows this program's net benefit
(supplemental payments less intergovernmental transfers) to public and private
hospitals for 1992-1993 through 1994-95. Figure 4 shows the amount of uncompen
sated care costs attributed to public and private DSH hospitals. The figures show that
while the percent of the total hospital net benefit received by public hospitals
decreased from 77 percent to 57 percent between 1992-93 and 1994-95, the percent of
uncompensated care costs provided by DSH public hospitals increased from 91.6
percent to 93.5 percent.

- The SB 1255 Program. Figure 5 shows this program's gross
supplemental payments to hospitals, intergovernmental transfers to the state, and net
benefit to public and private hospitals for fiscal years 1992-93, 1993-94, and 1994-95.
Hospitals will negotiate with the CMAC later this fiscal year to determine the 1995-96
amounts, with the exception of Los Angeles County (see below).
| Figure 5 |
| SB 1255 Program |
| (Dollars in Thousands) |
|
|
|
|
|
|
|
|
|
|
|
1992-93 |
1993-94 |
1994-95
|
| Hospital Type
| Gross Payments
| Transfers
| Net Benefit
| Gross Payments
| Transfers
| Net Benefit
| Gross Payments
| Transfers
| NetBenefit
|
| L.A. County hospitals |
$245,000 |
$130,000 |
$115,000 |
$245,000 |
$130,000 |
$115,000 |
$438,000 |
$229,000 |
$209,000 |
| Other county hospitals |
66,545 |
33,500 |
33,045 |
64,400 |
32,000 |
32,400 |
150,400 |
79,000 |
71,400 |
| County subtotals |
$311,545 |
$163,500 |
$148,045 |
$309,400 |
$162,000 |
$147,400 |
$588,400 |
$308,000 |
$280,400 |
|
|
|
|
|
|
|
|
|
|
| L.A. community hospitals |
$7,650 |
--- |
$7,650 |
$9,550 |
--- |
$9,550 |
$12,000 |
--- |
$12,000 |
| Children's hospitals |
8,800 |
--- |
8,800 |
10,700 |
--- |
10,700 |
21,515 |
--- |
21,515 |
| Other community hospitals |
2,925 |
--- |
2,925 |
3,475 |
--- |
3,475 |
9,350 |
--- |
9,350 |
| Community subtotals |
$19,375 |
-- |
$19,375 |
$23,725 |
--- |
$23,725 |
$42,865 |
--- |
$42,865 |
|
|
|
|
|
|
|
|
|
|
| District hospitals |
$500 |
--- |
$500 |
--- |
--- |
--- |
$750 |
--- |
$750 |
| University of California hospitals |
24,000 |
$15,000 |
9,000 |
$24,500 |
$15,000 |
$9,500 |
50,300 |
$30,000 |
20,300 |
| Totals |
$355,420 |
$178,500 |
$176,920 |
$357,625 |
$177,000 |
$180,625 |
$682,315 |
$338,000 |
$344,315 |
| Source: California Medical Assistance Commission. |
- Other DSH Considerations. The federal Omnibus Budget
Reconciliation Act of 1993 placed a cap on how much each hospital can be reim
bursed under the DSH Programs. Basically, hospitals cannot receive more than 100
percent of their uncompensated care costs through DSH supplemental payments,
beginning in 1995-96. Federal regulations to implement these provisions have not
been issued. We note that the DHS has submitted a state plan amendment to the
federal Health Care Financing Administration proposing a method for calculating
uncompensated care costs for hospitals in California, but no decision has been made
on this proposal. Because the regulations have not been adopted and hospital-specific
data are not yet available, an estimate of the impact of the hospital caps on California
is not available at this time.
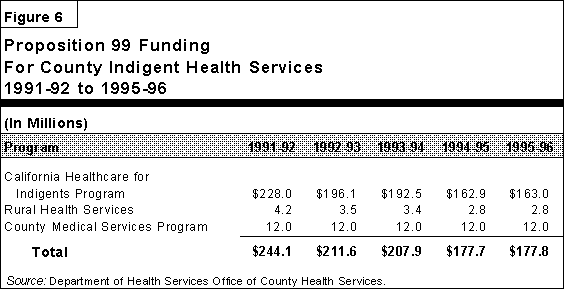
- Proposition 99 Revenues Declining. The decline in tobacco
consumption has led to lower tobacco tax revenues for Proposition 99 programs,
including county health services, as shown in Figure 6. Between 1991-92 and 1995-96,
the amount of tobacco tax revenues counties received is expected to fall from $244.1
million to $177.8 million -- a 27 percent decline.
- Los Angeles County. As a result of its fiscal problems, Los
Angeles County negotiated agreements with the federal government and the state to
receive $514 million in federal funds for 1995-96. Most of these funds will flow
through the SB 1255 Program:
- The county and the CMAC negotiated the early receipt of federal funds
through the SB 1255 Program for 1995-96. Normally these negotiations would have
occurred later in the fiscal year. The county will transfer an additional $170 million to
match an equal amount in new federal funds. Of the $340 million, Los Angeles
County will receive $320 million in SB 1255 payments. The net benefit to the county,
therefore, will be $150 million.
- Contingent upon approval of a federal Medicaid waiver, the county will
transfer an additional $182 million to match an equal amount in federal funds,
thereby receiving $364 million in SB 1255 payments. The net benefit to the county,
therefore, will be $182 million.
- In addition, the county will receive another $182 million in federal funds
through various programs, pursuant to the waiver.
Uninsured Rates Vary Significantly Across California
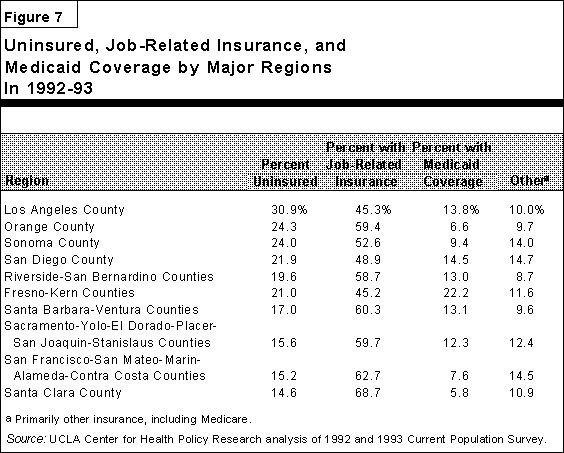
The UCLA Center for Health Policy Research report, entitled Health Insurance
Coverage of Californians, 1989-92, examined recent trends in health insurance in
California. Figure 7 compares the percent of the population lacking insurance and
those covered by insurance or Medi-Cal in larger regions of the state. The report
indicates that Los Angeles County's uninsured rate of 30.9 percent is the highest
among the 30 largest metropolitan areas nationwide. Four other regions -- Orange,
Sonoma, San Diego, and Fresno-Kern Counties -- have uninsured rates in excess of 20
percent.
The report further indicates that the majority of uninsured individuals are employed,
largely in small firms. Those individuals employed full-time in small firms (less than
25 workers) are less likely to receive health insurance compared to employees in
small firms in the rest of the nation -- 36 percent in the state versus 42 percent
nationally. Many of the smaller firms are involved in the agricultural, retail, and
service sectors of the economy.
Public-Private Partnerships
We list below some ways the state and counties have worked with private groups to
improve health services for indigents or those who otherwise would be indigent.
- Lowering Health Insurance Costs for Small Businesses. The state
Managed Risk Medical Insurance Board (MRMIB) administers the Health Insurance
Plan of California (HIPC), which serves as a purchasing pool to leverage lower health
insurance rates for small businesses with 3 to 50 employees. By negotiating with
health insurance companies, the HIPC helped reduce premium rates by an average of
6.3 percent in 1994-95, and expects to lower them by an additional 5.1 percent in
1995-96. Since its inception in 1993, the HIPC has enrolled over 5,000 small businesses
and 97,000 people through 25 different private health plans. Approximately 20
percent of those small businesses enrolled in HIPC did not previously offer health
insurance to their employees.
- Subsidizing Health Insurance. The MRMIB also secures health
insurance for individuals through the California Major Risk Medical Insurance
Program (MRMIP) and the Access for Infants and Mothers (AIM) Program. The
MRMIP has helped secure health insurance for over 19,000 California residents
ineligible for Medicare and unable to obtain coverage in the open market because of
pre-existing medical conditions. The program supplements premiums (to seven
participating health plans) which subscribers pay for comprehensive inpatient and
outpatient health care services. The AIM Program contracts with private health
insurance plans to provide coverage for low-income women seeking preg
nancy-related and neonatal medical care. The program has enrolled over 4,500
women and 11,000 infants through eight private health plans. Both the MRMIP and
AIM Program are funded with tobacco tax (Proposition 99) revenues.
- Contracting Services. Some counties, such as San Diego and
Orange, do not operate their own hospitals or primary care clinics, but contract with
the University of California and with nonprofit, community based groups to provide
their health services. San Diego County has contracts with 21 nonprofit commu
nity-based groups to operate primary care clinics. The clinics reportedly keep their
costs down by private fund raising, using volunteers, and paying lower salaries on
average.
Federal Medicaid Reform
Congress recently passed legislation that would make significant changes to the
federal Medicaid Program (Medi-Cal in California).
Changes in Entitlement to Services. States would be required to
provide some medical assistance to children under age 13 and pregnant women in
families with incomes at or below the federal poverty level and to disabled persons,
as defined by the state.
Increased Flexibility in Some Areas. The legislation would increase
the states' discretion over several key areas, including eligibility criteria and benefit
coverage. States would be authorized to establish the benefit package, with the
exception of two mandatory benefits: (1) immunizations for eligible children and (2)
pre-pregnancy family planning services and supplies, as determined by the state. In
addition, states would no longer be required to: (1) cover specific services; (2)
reimburse specific types of health care providers; (3) reimburse at specific rates; (4)
provide services on a statewide basis; (5) provide services of the same duration,
amount, and scope to all eligible individuals; (6) allow patients "freedom of choice" to
select providers; or (7) reimburse noncontract hospitals and nursing facilities on the
basis of reported actual costs.
Some Strings Are Still Attached. The legislation includes a state
maintenance-of-effort requirement for three population groups: (1) pregnant women
and children in families with incomes below 185 percent of poverty, (2) the elderly,
and (3) the disabled. Also included is a maintenance-of-effort provision for Medicare
premium assistance and payments to Federally Qualified Health Centers and rural
health centers.
Payments to States. A federal maximum allotment would be
established for each fiscal year beginning with federal fiscal year 1996 (October 1995
to September 1996). States would be required to match federal funds up to the federal
cap. Funds would be allotted to states based on a funding formula. The DSH
program would be eliminated, with the payments incorporated into the overall funds
allotted to states according to the funding formula. In addition to this block grant
funding, California would receive an estimated $1.6 billion over five years to partially
offset costs for emergency services provided to undocumented persons.
Proposed Waiver for Los Angeles County. We note that this
legislation puts at risk Los Angeles County's receipt of the $364 million in federal
funds anticipated as a result of the proposed Medicaid waiver.
Return to LAO Home Page







