

The budget proposes Medi-Cal expenditures of $17 billion ($6.2 billion General Fund) in 1996-97. This represents a General Fund increase of $173 million, or 2.8 percent, over estimated current-year expenditures.
At the state level, the Department of Health Services (DHS) administers the Medi-Cal Program. Other state agencies, including the California Medical Assistance Commission (CMAC) and the Departments of Social Services, Developmental Services, Alcohol and Drug Programs, and Mental Health perform Medi-Cal related functions under agreements with the DHS. At the local level, county welfare departments determine the eligibility of applicants for Medi-Cal and are reimbursed for those activities. The federal Health Care Financing Administration oversees the program to ensure compliance with federal law.
Persons eligible for Medi-Cal fall into four major categories:
| Figure 13 Who Is Eligible for Medi-Cal? | ||||||||
|---|---|---|---|---|---|---|---|---|
| (Dollars in Millions) | ||||||||
| Income Level | Other Characteristics | Number Eligible | 1995-96 GeneralFund Expenditures a |
|||||
| Federally Required Categories | ||||||||
| Categorically Needy | ||||||||
| AFDC or SSI/SSP income standard |
| 4,054,300 | $3,811 | |||||
| Other Women and Children | ||||||||
Percent of federal poverty level:
|
| 202,000 | 171 | |||||
| Undocumented Persons and Refugees | ||||||||
|
| 282,600 | 312 | |||||
| Additional Categories in California | ||||||||
| Long-Term Care | ||||||||
| Persons of any income must "spend-down" to $35 per month |
| 70,700 | 1,069 | |||||
| Medically Needy | ||||||||
|
| 522,500 | 782 | |||||
| Medically Indigent | ||||||||
| Same as medically needy |
| 280,500 | 232 | |||||
| Undocumented Persons | ||||||||
| Same as medically needy |
| NA | 75 | |||||
| a Figure reflects current law. Budget reflects $378 million less than amount shown due to assumed receipt of intergovernmental transfers from counties and other factors. | ||||||||
| b State legislation, which established a special income deduction and assets waiver, shifted pregnant women from the state-only 186 percent to 200 percent of federal poverty level program to the federally funded 185 percent program. | ||||||||
Federal law requires the Medi-Cal Program to provide a core of basic services, including hospital inpatient and outpatient care, skilled nursing care, doctor visits, laboratory tests and X-rays, family planning, regular examinations for children under the age of 21, and services in rural health clinics. Many Medi-Cal services require prior authorization and may not be reimbursed unless the service is determined to be medically necessary.
In addition, the federal government provides matching funds for optional services. California currently provides 29 of 34 optional services, but the budget proposes to eliminate eight of them. We discuss this proposal in more detail below.
We also note that pending federal Medicaid reform legislation could change eligibility and benefit provisions. We discuss this legislation later in this analysis.
The major General Fund changes proposed for the Medi-Cal Program in 1996-97 include: (1) $315 million for caseload, utilization, and cost increases; and (2) a net decrease of $142 million in various program changes.
The proposed program changes include the following:
As Figure 14 indicates, General Fund expenditures for the Medi-Cal Program increased from $4.1 billion in 1990-91 to an estimated $6.1 billion in 1995-96, reflecting an increase of about 10 percent annually. Federal funding for the program has increased at a significantly higher rate, largely due to the "SB 855" Program. This program has provided payments to disproportionate-share hospitals since 1991-92. The purpose of these payments is to recognize the financial burden of
uncompensated care on those hospitals that serve a high number of indigent persons not eligible for Medicaid. These payments, and the required county match, comprise on average about $2 billion annually in total expenditures from 1991-92 through 1995-96.
| Figure 14 Medi-Cal Expendituresa 1990-91 through 1995-96 (Dollars in Billions) |
|||||||
|---|---|---|---|---|---|---|---|
| 1990-91 | 1991-92 | 1992-93 | 1993-94 | 1994-95 | 1995-96 | Average Annual Increase | |
| General Fund | $4.1 | $5.8 | $5.4 | $5.5 | $6.0 | $6.1 | 9.8% |
| All funds | 8.8 | 13.8 | 13.9 | 16.9 | 17.3 | 16.5 | 17.5 |
| a Figures for 1991-92 have been adjusted to eliminate one-time costs for change from cash to accrual accounting. Figures for 1995-96 are estimated. | |||||||
In addition, federal funding is budgeted in the current year and for 1996-97 for the Targeted Case Management Program, which reimburses counties for case management activities provided to specific Medi-Cal beneficiaries. These funds comprise $40 million of total expenditures for 1995-96 and the budget year.
The increase in Medi-Cal expenditures over the last five years has resulted largely from caseload increases (which in turn reflect economic and societal changes), utilization changes, and medical care inflation. We discuss these factors below.
Caseload Changes.In prior years, the largest single factor driving program expenditures was the significant increase in the number of persons eligible for Medi-Cal. However, recent data indicate caseload growth is leveling off.
In 1985-86, 2.9 million persons (one out of ten persons in the state) were eligible for the program, while the number of eligibles reached 5.4 million persons (more than one out of every six residents) in 1994-95. As a point of comparison, the number of persons who receive health care coverage through Medi-Cal is about equal to the number of children enrolled in California's public school system, and the Medi-Cal Program is the single largest health-insurer in the state.
In general, three factors accounted for the increase in the number of eligible participants. The "traditional" recipients of Medi-Cal services--primarily AFDC and SSI/SSP recipients--increased significantly during the early 1990s, largely the result of economic and demographic changes. In addition, the Medi-Cal Program caseload increased as a result of state and federal changes that have expanded eligibility to "newer eligibility groups" of recipients. Specifically, the federal government mandated that the state provide medical services to undocumented persons and expand eligibility for pregnant women and children. Similarly, the state elected to extend coverage to pregnant women and their infants beyond the federal requirements. Expenditures due to these state and federal policy changes account for about one-third of total expenditure growth since 1989-90.
Medi-Cal caseloads grew rapidly in the early 1990s but the growth rate began to slow down in 1994-95 (see the Health and Social Services Overview section). The DHS estimates a slight decrease of 0.5 percent in total Medi-Cal eligibles for 1995-96, due to a decline in Public Assistance-AFDC and Medically Needy-AFDC caseloads and a flattening in the Medically Indigent-Children caseload. For 1996-97, the department is projecting a slight increase (0.7 percent) in total Medi-Cal eligibles.
Utilization Changes and Medical Care Inflation.Higher utilization of services by Medi-Cal eligibles and other cost increases are the major factors driving program expenditure increases for 1996-97.
Medical care costs have been increasing at rates that generally exceed other types of inflation. Medi-Cal payment levels for some services (such as for physician services) are discretionary, while others are automatically adjusted pursuant to statute (such as for generic drugs and nursing facilities). Hospital inpatient rates generally are negotiated, but the state has little practical alternative to recognizing at least a portion of the cost increases that hospitals experience. Accordingly, because expenditures for hospital inpatient services, long-term care, and drugs account for the vast majority of Medi-Cal expenditures, medical care inflation has played a significant role in the program's expenditure growth over the last several years.
Societal Changes.Various demographic and societal changes also contributed to Medi-Cal expenditure growth. One societal change that has affected the Medi-Cal Program is the emergence of the AIDS epidemic. In addition, the growth in the number of unmarried teenage women having children, citizen children born to undocumented women, and children born to substance-abusing mothers have increased Medi-Cal eligibility and expenditures.
Unlike federal welfare reform, the Governor's Budget does not assume enactment of the Medicaid reform legislation. We discuss major provisions of the congressional conference agreement and President Clinton's proposal.
As in the case of welfare reform, proposals under consideration at the federal level would make significant changes to the federal Medi-caid Program (Medi-Cal in California).
The conference agreement proposal would repeal Title XIX of the Social Security Act (the Medicaid Program) and replace it with Title XXI of the Social Security Act (the Medigrant Program).
Changes in Program Eligibility and Entitlement to Services.The proposal would require states to provide assistance to (1) pregnant women and children under age 13 with family income at or below the federal poverty level and (2) low-income disabled individuals, as defined by the state; the measure would eliminate the entitlement for all other beneficiaries. States would be required to provide immunizations for eligible children, and pre-pregnancy family planning services and supplies, as defined by the state. The proposal would repeal the federal Vaccines for Children Program.
Increased Flexibility in Some Areas.The proposal would increase the state's discretion over several key areas, including eligibility criteria, benefit coverage, and payment rates. Specifically, states would no longer be required to: (1) cover specific services; (2) reimburse specific types of health care providers, with some exceptions; (3) reimburse at specific rates; (4) provide services on a statewide basis; (5) provide services of the same duration, amount, and scope to all eligible individuals; (6) allow patients "freedom of choice" to select providers; or (7) reimburse noncontract hospitals and nursing facilities on the basis of reported actual costs.
Some Strings Are Still Attached.A state maintenance-of-effort would be required for three population groups and two program areas: (1) pregnant women and children in families with incomes at or below 185 percent of poverty; (2) low-income disabled individuals; (3) low-income elderly; (4) Medicare premium assistance for low-income beneficiaries; and (5) services provided at federally qualified health clinics and rural health clinics.
Payments to States.A maximum federal allotment would be established for each fiscal year beginning with federal fiscal year (FFY) 1996. The proposal specifies a fixed dollar allotment for each state in FFY 96 ($8.9 billion for California) and would establish a maximum allowable annual growth rate for each state for each year thereafter. In addition, the Federal Medical Assistance Percentage (matching funds) would increase from 50 percent to 60 percent, effectively lowering the required state financial participation amount.
The proposal would prohibit the use of these federal funds for undocumented persons and would eliminate the current federal requirement that states provide emergency medical services to undocumented persons. However, 15 states (including California) would receive a total of $3.5 billion over five years for the cost of providing emergency medical services to undocumented persons. California would receive about $1.6 billion from this fund over the five-year period.
Disproportionate Share Hospital Payments. The proposal would incorporate funds for supplemental payments to disproportionate share hospitals into the overall state allotment, but states would have flexibility over the use of the funds. States would be required, however, to describe in the state plan how they intend to provide assistance to these hospitals.
The proposal would amend the current Medicaid Program as follows.
Program Eligibility and Entitlement to Services. The proposal would retain certain provisions of the existing program, including the current mandatory eligibility groups and the requirement to provide all mandatory benefits. States would have the option to expand or simplify program eligibility within certain parameters, but additional federal funding would not be available for the expanded population.
Some Increased Flexibility. Methods for establishing provider reimbursement rates would be revised. States would no longer be required to base reimbursement rates on actual costs for noncontract hospitals and nursing facilities. This provision would apply to federally qualified health clinics and rural health centers beginning in FFY 99. The proposal also would eliminate the need for federal waivers to implement certain types of managed care delivery systems and to provide home- and community-based services as an alternative to institutionalization.
Per Capita Growth Limit Controls Federal Spending.The Medicaid population would be divided into four beneficiary groups for purposes of federal matching payments: the aged, the disabled, nondisabled adults, and nondisabled children. Effective FFY 97, spending per beneficiary would be federally matched up to a specified cap. The spending cap, established for each of the four groups of beneficiaries, would be adjusted annually by an inflation-based growth index and an adjustment to meet budgetary targets. Research and demonstration waivers currently in operation would be subject to the per capita limit. However, federal funds for disproportionate share hospitals, Medicare premiums, the Vaccines for Children Program, and several other programs would be excluded from the cap.
Disproportionate Share Hospital Payments.The proposal would reduce the amount of federal funding available to states for services provided by disproportionate share hospitals. The measure would provide more flexibility in the use of these funds by allowing them to be spent on federally qualified health clinics and rural health centers.
Special Funds.Two special funds would be established to assist states with the costs of uncompensated care and undocumented persons. The ten states with the highest percentage of uncompensated care and Medicaid shortfalls (including California), as measured by the American Hospital Association in its report published November 1992, would receive a total of $3.5 billion over five years. California would receive about $350 million from this fund over the five-year period. The second fund, similar to the congressional provision discussed above, would provide 15 states (including California) with $3.5 billion over five years for the costs of providing emergency medical care to undocumented persons. California would receive about $1.6 billion from this fund over the five-year period.
The budget assumes enactment of federal welfare reform legislation affecting the AFDC, SSI/SSP, and Medicaid programs. We review the budget's assumptions of how the federal legislation would affect the Medi-Cal Program.
Despite President Clinton's veto of H.R. 4--the Personal Responsibility and Work Opportunity Act of 1995--many observers believe that the President and Congress will ultimately reach agreement on a welfare reform bill that will encompass a number of major features of the congressional measure. (See our analysis of the AFDC Program for a detailed description of the proposed changes to the welfare programs.) The Governor's Budget, in fact, assumes the enactment of the H.R. 4 provisions affecting the AFDC Program, the SSI/SSP, and the Medicaid Program. Below we discuss how these welfare changes would affect the Medi-Cal Program.
Current Legal Noncitizens.Under H.R. 4, effective January 1, 1997, most current legal noncitizens would not be eligible for the SSI Program. However, H.R. 4 permits states at their option to continue to provide the full range of Medicaid (Medi-Cal) benefits (emergency and nonemergency medical services) to these noncitizens. The budget proposes to transition the persons who will no longer be eligible for SSI (thereby losing their "categorically needy" Medi-Cal eligibility) to the optional "medically needy" aid category and limit their benefit to emergency medical services only. We note that the proposal does not address what would happen to the individuals currently residing in long-term care facilities.
Newcomer Legal Noncitizens.Under H.R. 4, newcomer noncitizens--individuals arriving after enactment of federal welfare reform--would be ineligible for all federal means-tested programs for five years, with some exceptions including emergency medical services. Under current law, these individuals receive a full range of Medi-Cal benefits. The budget proposes to provide emergency medical services only to these individuals. Although this provision of federal law would take effect immediately upon enactment of the legislation, the budget assumes a state implementation date of January 1, 1997.
Illegal Immigrants. The H.R. 4 would prohibit states from providing certain state and local public benefits, including nonemergency medical services, to illegal immigrants unless the state enacts legislation to authorize the benefit. Currently, the Medi-Cal Program provides long-term care services and prenatal care services to illegal immigrants, and counties provide health care to indigents not eligible for Medi-Cal benefits. The Governor's Budget proposes the following:
We recommend a technical adjustment in the amount proposed for long-term care services because the budget does not reflect the savings from the administration's proposal to eliminate these services for illegal immigrants who apply for benefits after the enactment of federal welfare reform legislation. (Reduce Item 4260-101-0001 by $4,233,000.)
The pending federal welfare reform legislation would prohibit the state from providing nonemergency medical services to illegal immigrants unless the state enacts legislation to authorize the benefit. The administration proposes to reauthorize Medi-Cal long-term care services only for illegal immigrants presently in nursing facilities. However, the budget does not reflect the savings from eliminating these services for new applicants. The administration advises us that this omission was inadvertent. We estimate that the reduced costs for benefits and administration would be approximately $4.2 million (General Fund). Accordingly, we recommend this technical adjustment so that the budget will be consistent with its own assumptions, for an estimated General Fund savings of $4.2 million.
With respect to the department's proposal to eliminate certain optional services, we find that: (1) the proposal could place an additional burden on county indigent health programs; and (2) the department's savings estimate probably is optimistic, due to the federal requirement that Medi-Cal provide necessary transportation.
The budget assumes that the Legislature will enact legislation that will result in net General Fund savings of $34 million by eliminating the following optional service categories from Medi-Cal coverage:
Figure 15 lists the department's estimate of the Medi-Cal savings from eliminating each of these services and an estimate of the average number of Medi-Cal beneficiaries who currently use these services each month. These savings are partially offset by a General Fund cost of $5.1 million in the budget of the Department of Developmental Services to continue the benefits for regional center clients.
| Figure 15 Proposed Elimination of Optional Medi-Cal Services General Fund Savings 1996-97 | |||
|---|---|---|---|
| (Dollars in Millions) | |||
| Service | Average Monthly Users | Estimated Savings | |
| Medical supplies | 49,490 | $17.4 | |
| Nonemergency transportation | 11,400 | 16.0 | |
| Psychology | 4,950 | 2.8 | |
| Podiatry | 13,620 | 2.3 | |
| Acupuncture | 8,140 | 1.8 | |
| Speech and audiology | 680 | 0.4 | |
| Chiropractic | 3,890 | 0.2 | |
| Independent rehabilitation centers | 350 | 0.03 | |
| DHS budget adjustment for developmentally disabled persons | NA | -1.9 | |
| --a | $39.0 | |
| a Total monthly users cannot be estimated, since one beneficiary may use more than one optional service. | |||
"Necessary Transportation" Is Required.Even if optional benefits are eliminated, current federal law requires Medi-Cal to provide "necessary transportation" to beneficiaries. Accordingly, we do not believe that the budgeted savings attributable to the elimination of medical transportation provided in vans can be achieved. Absent legislation to augment the budget, we estimate that this will result in a General Fund deficiency of about $16 million for 1996-97.
Costs May Shift to Other Services.Actual savings from elimination of the proposal's remaining seven optional benefits would depend on behavioral changes on the part of Medi-Cal beneficiaries. In some cases, elimination of optional services clearly will result in savings. In other cases, the savings may be offset because beneficiaries may substitute other Medi-Cal services for the service being eliminated or they may delay receiving treatment and ultimately require more acute care. The budget assumes cost shifts such as these ranging from 0 to 90 percent, depending on the service. The extent to which cost shifts will actually occur, however, is unknown.
Cost Shifts to Counties May Result.We note that counties are the provider of last resort for health services. Accordingly, they may experience increased demand for services they provide, to the extent that beneficiaries are unable to receive care under the Medi-Cal Program.
We recommend modifying the proposal to charge copayments for services to certain Medi-Cal beneficiaries by (1) reducing the pharmacy dispensing fee for all prescriptions, irrespective of whether copayments can be collected, and (2) exempting from the copayment requirement outpatient clinic and physician services, thereby reducing the potential for primary care access problems and cost-shifting that might otherwise result. This will result in a net General Fund savings of $5.5 million in 1996-97. (Reduce Item 4260-101-0001 by $5,527,000.)
The budget assumes enactment of legislation that will result in savings of $46 million ($23 million General Fund) by requiring some Medi-Cal beneficiaries to pay copayments for certain Medi-Cal services, effective October 1, 1996.
Background.Current state law permits Medi-Cal providers to collect copayments for certain services. However, prior budgets have not assumed collection of the copayments because federal law prohibits providers from refusing services to a beneficiary if he or she cannot make a copayment.
Federal law also requires Medi-Cal to exempt beneficiaries in the following categories from copayment requirements:
Proposal Has Potential Drawbacks.The proposed legislation would not change the requirements in current federal law that prohibit providers from refusing to provide services to Medi-Cal beneficiaries if they cannot pay the copayment. Thus, to the extent beneficiaries are unwilling or unable to make the copayments, providers will receive a lower level of net reimbursements.
Most providers who would face reduced Medi-Cal rates under the proposal have not received Medi-Cal rate increases since 1985-86. Accordingly, even though the copayments are small, some providers (such as physicians and outpatient clinics) may respond to the rate reduction by refusing to provide services to Medi-Cal beneficiaries, thereby reducing access to primary care under the Medi-Cal Program. This, in turn, could result in additional costs to Medi-Cal, to the extent that beneficiaries do not receive primary care (or do not seek it due to the copayment requirement) and develop more serious illnesses that require emergency inpatient services.
| Figure 16 Medi-Cal Program Proposed Beneficiary Copayments 1996-97 |
|||
|---|---|---|---|
| Service | Copayment Amount | General Fund Savings (In Thousands) | |
| Prescription drugs | $0.50 to $3 | $12,434 | |
| Physician services | 2 | 4,164 | |
| Dental services | 3 | 2,488 | |
| Hospital outpatient services | 5 | 1,375 | |
| Clinic services | 1 to 3 | 800 | |
| Optometry services | 2 to 3 | 735 | |
| Home health services | 3 | 599 | |
| Durable medical equipment | 3 | 212 | |
| Prosthetics and orthotics | 3 | 86 | |
| Hearing aids | 3 | 39 | |
| Other | -- | 85 | |
| $23,017 | ||
Given these potential drawbacks, we recommend that the Legislature modify the budget proposal, as discussed below.
Expand Pharmacist Rate Reduction. First, as Figure 16 shows, most of the savings from copayments are attributable to reducing the "dispensing fee" that is paid to pharmacists each time they fill a prescription. The current Medi-Cal reimbursement for each prescription is $3.55, plus ingredient costs for the drug. We note that this amount is significantly higher than the amount paid by other "third-party" payers. For example, the state's Public Employees' Retirement System negotiates with health care service plans and, on average, reimburses pharmacists $2.55 per prescription (plus drug ingredient costs)--$1 belowthe Medi-Cal reimbursement rate.
Accordingly, we believe the administration's proposal should be modified to eliminate the additional amount currently paid to pharmacists. Specifically, because the pharmacy dispensing fee is above the rate paid by other third-party payers, we recommend that the Legislature authorize copayments on drugs and reduce the dispensing fee paid to pharmacists by $1 per prescription for allbeneficiaries, irrespective of whether the pharmacist can charge a copayment. The reduced rate should take effect on August 1, 1996 rather than in October as the budget proposes.
We note that the per-prescription reimbursement we recommend ($2.55) essentially conforms the Medi-Cal reimbursement rate to the level currently paid by non-Medi-Cal providers--even if pharmacists are unable to collect anycopayments. Thus, we do not believe the proposal would adversely affect beneficiary access to prescription drugs. We estimate that this action, together with the earlier implementation date, would result in General Fund savings of $10.5 million above the savings proposed in the budget.
Exempt Physician and Clinic Services. We also recommend that a portion of these savings be redirected to eliminate the proposed copayments in those cases where, in our judgment, the potential for primary care access problems and cost-shifting is most clearly an issue--specifically for physician and clinic services. This component of our recommendation would reduce the budgeted level of savings by $5 million from the General Fund.
Impact of Recommendation. The net result of these recommendations would be an additional General Fund reduction of $5.5 million beyond the amount assumed in the budget. In summary, our recommendation would (1) fully conform the Medi-Cal pharmacy dispensing fee to levels paid by other payers, (2) reduce the potential for primary care access problems and cost-shifting, and (3) achieve an additional General Fund savings of $5.5 million.
The budget assumes enactment of federal legislation that would permit the state to reduce reimbursement rates for "distinct part" nursing facilities, for a General Fund savings of $25.7 million in 1996-97.
The budget proposes to reduce, by an average of 20 percent, the reimbursement rates paid to nursing facilities that operate as a "distinct part" of a hospital, for a General Fund savings of $25.7 million in the budget year. Currently, these facilities receive, on average, nearly three times the reimbursement rate paid to freestanding nursing facilities (about $215 per day in distinct part facilities versus about $75 per day in freestanding facilities). The higher rates for distinct part facilities are due to a number of factors, including much higher overhead and labor costs associated with a large hospital.
Under federal law (specifically, a provision commonly referred to as the "Boren amendment"), hospital and nursing facility reimbursement rates paid by Medi-Cal must be "reasonably sufficient to cover the costs of an efficiently and economically operated facility." In general, this requirement has been interpreted to require reimbursement of facilities, including "distinct part" nursing facilities, on the basis of reported actual costs. Thus, in order to reduce distinct part reimbursement rates, the department would need to (1) demonstrate that existing rates exceed the costs to operate these facilities or (2) change a federal law. The budget assumes enactment of federal legislation to repeal the Boren amendment. Such a provision is included in the pending Medicaid reform legislation.
We recommend enactment of legislation to establish a contracting program for nursing facilities similar to the program currently in place for hospitals, for an estimated net General Fund savings of $9.8 million in 1996-97. (Reduce Item 4260-101-0001 by $10,000,000 and increase Item 4270-001-0001 by $175,000.)
In response to recommendations that we made in our Analysis of the 1995-96 Budget Bill, the Legislature adopted supplemental report language requiring the CMAC to evaluate the feasibility of implementing a program of contracting for nursing facility services in the Medi-Cal Program. The commission's report concluded: "A contracting program for the purchase of Medi-Cal skilled nursing services is feasible. There does not appear to be any unique aspect of skilled nursing facilities which would rule out the possibility of conducting competitive negotiations for the purchase of Medi-Cal SNF (skilled nursing facility) services."
Background--Hospital Reimbursement Rates.The CMAC negotiates reimbursement rates with hospitals for inpatient services provided to Medi-Cal beneficiaries. It is generally acknowledged that the commission has been successful in negotiating rates that are lower than those which would otherwise be provided.
We believe the primary reason the CMAC has been able to negotiate savings is due to generally low occupancy rates in California hospitals (frequently less than 50 percent). In effect, the low occupancy rates result in a "buyer's market" for hospital inpatient services, which the CMAC has used to its advantage in negotiating reimbursement rates. Accordingly, most hospitals in California have negotiated rates that are significantly lower than the "cost-based" rate in order to (1) attract the volume of patients who are eligible for Medi-Cal and (2) in many cases, gain access to federal disproportionate share hospital supplemental payments.
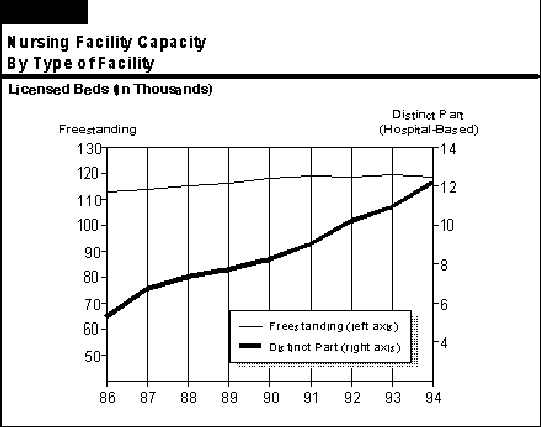
Nursing Facilities.As Figure 17 shows, the number of distinct part (hospital-based) nursing facility beds has more than doubled since 1986, increasing from about 5,000 licensed beds in 1986 to over 12,000 beds in 1994. In contrast, the number of freestanding nursing facility beds has remained fairly steady, increasing by about 1 percent annually over the eight-year period. In other words, hospital-based nursing facility capacity has grown at over ten times the rate of freestanding facilities.
As noted previously in our analysis, Medi-Cal reimburses distinct part facilities at a rate nearly three times the amount it pays for services provided to beneficiaries who receive care in freestanding facilities. This higher reimbursement rate for distinct part facilities almost certainly explains some of the growth in these facilities.
Opportunity Exists for Contracting. Currently, the CMAC does not negotiate rates for long-term care (nursing facility) services. We believe that if a contracting system were implemented for nursing facilities, rate reductions could be achieved because (1) Medi-Cal Program reimbursement provides nursing facilities approximately 65 percent of the revenues they receive, and (2) excess capacity exists in several regions of the state. The statewide average occupancy rate for freestanding nursing facilities has steadily declined from 93 percent in 1986 to about 85 percent in 1994, and the occupancy rate for distinct part nursing facilities declined from 82 percent to 78 percent over the same period.
We also note that the contracting approach has an advantage over across-the-board rate setting, in that the rate would not need to be uniform across the state. This is particularly important because approximately one-third of distinct part facility reimbursements are paid to county-operated facilities and those in rural areas of the state. As a result, under contracting, the state would have the flexibility to achieve lower reimbursement rates in many cases, while retaining the ability to pay higher rates in cases where other policy objectives--such as maintaining access to acute care hospitals in rural areas--are considered to outweigh the need to achieve Medi-Cal Program savings.
Analyst's Recommendation. To take advantage of market conditions, contain growth in the number of higher-cost facilities, and increase state rate flexibility, we recommend enactment of legislation requiring the CMAC to negotiate Medi-Cal reimbursement rates for nursing facilities in those areas of the state where they believe savings can be achieved without adversely affecting access to services.
Although it is not possible to estimate the precise magnitude of savings that could be achieved through CMAC contracting with nursing facilities, we believe it is reasonable to assume General Fund savings of $10 million, or approximately 1 percent of expenditures, for 1996-97. We believe the state will achieve significant savings in subsequent years after full implementation of the contracting program. We further recommend an augmentation of $175,000 from the General Fund, to be matched with federal funds, for four new positions at the CMAC to support the contracting program.
We note that this proposal would require a federal waiver; however, the state has obtained such a waiver to negotiate rates with hospitals. Further, as indicated previously, the budget assumes passage of federal legislation to repeal the Boren amendment, which would eliminate the need for a waiver.
We recommend that the department report, during the budget hearings, on the feasibility of expanding the "assisted living" model of service delivery in order to allow the provision of certain medical services to long-term care Medi-Cal beneficiaries in less restrictive and less costly residential settings (community care facilities rather than nursing facilities).
In California, a continuum of care is available to individuals in need of long-term care. The continuum ranges from certain community care facilities, which provide relatively little medical care, to health facilities such as nursing homes, which do provide medical services. While state law does not specifically define "assisted living" facilities, the concept is generally associated with residential community care facilities serving persons in need of long-term care services. Long-term care recipients are the most expensive group of Medi-Cal recipients, on a per-case basis; while they are an estimated 1.3 percent of the caseload, they account for 17 percent of expenditures for 1995-96. In this analysis, we examine one alternative for reducing these costs by expanding the assisted living concept to include health care services provided to individuals in community care facilities.
Current Long-Term Care Placement Options. Community care facilities include nonmedical residential care facilities which provide incidental medical services (for example, assistance with self-administered medications), room and board, basic supervision, and personal care services. In general, financially needy elderly and disabled individuals residing in community care facilities are eligible for SSI/SSP, and in turn are eligible for the Medi-Cal Program. Generally, these health services cannot be provided in the community care facility. However, health care services may be provided on a short-term basis to individuals residing in community care facilities if they are helping individuals transition from a hospital or nursing facility to community living.
Individuals requiring more intensive medical care are not considered appropriate for acceptance in a community care facility, and instead must be referred to health facilities such as nursing homes. Services for financially needy elderly and disabled individuals residing in nursing facilities are funded primarily by the Medi-Cal Program. Nursing facility rates range from $75 per day in freestanding facilities to $215 per day for distinct part (hospital-based) facilities.
Federal Medicaid Waiver Programs. Currently, the state operates various federal Medicaid waiver programs that target specific population groups. The waivers enable the state to avoid certain federal requirements and allow the provision of services to individuals who, absent these services, would be institutionalized in a hospital or nursing facility. The current waiver programs generally provide health care services to Medi-Cal beneficiaries residing in a home,but not in a community care facility.
The "Assisted Living" Model. The waiver programs in California focus on in-home care, where feasible. Several states, however, have reported significant savings by substituting community-based care, containing a medical component (generally called "assisted living" arrangements) for institutional, or nursing home, services.
There are several ways the state could expand the "assisted living" concept to provide health care services to long-term care Medi-Cal beneficiaries in a less restrictive setting. One alternative would be to seek federal funds, through a Medicaid waiver program, to provide certain long-term medical services for Medi-Cal beneficiaries residing in community care facilities. Alternatively, a state-only program could be established to pay for specific medical services in certain circumstances, when providing these services would be less costly than serving the patient in a nursing facility.
We note that the DHS is currently reviewing other states' activities in this area and analyzing the fiscal impact of various alternatives. Consequently, we recommend that the department report, during budget hearings, on the feasibility of expanding the "assisted living" model and, if expanded, the fiscal impact on the Medi-Cal Program.
We withhold recommendation on the $20 million proposed to consolidate and expand the family planning programs, pending review of additional information.
The budget proposes a $20 million General Fund augmentation to establish a "state-only" Medi-Cal family planning program, effective January 1, 1997. These funds would be combined with $23 million from the General Fund proposed to be redirected from the Office of Family Planning (OFP). (While the budget refers to the new program as a "state-only" program, we note that Medi-Cal beneficiaries receiving services under this program would continue to generate federal funds.)
Background.As Figure 18 (see page 51) shows, the DHS presently offers family planning services through two programs--the Medi-Cal Program for persons meeting the Medi-Cal eligibility criteria (generally AFDC-linked beneficiaries) and the OFP for low-income, non-Medi-Cal eligible persons.
Family planning services, under both programs, include contraceptive services and supplies, and certain health screens, testing, and treatment services. In addition, the OFP program offers more comprehensive education and counseling on reproductive health-related issues, such as sexually transmitted diseases. Family planning services do not include abortions or prenatal care services.
Governor's Proposal. The administration proposes to combine the two state programs currently providing family planning services into one program to be jointly administered by Medi-Cal and the OFP. Under the proposal, the Medi-Cal Program would be responsible for fiscal administration and fraud prevention, while the OFP would develop policies, monitor quality of care, develop outreach and awareness campaigns, and perform program evaluations.
The new program would provide family planning services to all persons with family incomes at or below 200 percent of poverty and at risk of unintended pregnancy. (A person is at risk of unintended pregnancy if he or she is sexually active, not sterilized, and not seeking pregnancy.)
The key features of the program include:
Significant Caseload Increases Projected.The administration proposes several initiatives designed to reduce the number of unwed and teenage pregnancies. This includes additional funding for a statewide media campaign, a new program to award grants to local entities, and development of school curricula. (See our analysis of Public Health programs.) The administration anticipates that these efforts will increase the demand for family planning services. Based, in part, on these proposals, the department projects a significant increase in the number of persons seeking family planning services. The department estimates that 1.3 million low-income women in California are at risk of unintended pregnancy and in need of family planning services. The administration's proposal to expand family planning services assumes 100 percentof these women will receive services when the program is fully implemented in 1997-98.
The department estimates that the non-Medi-Cal component of the program would serve an additional 37,000 persons in the budget year and 127,000 in 1997-98 when the program is fully implemented. The Medi-Cal component (90 percent federal funds and 10 percent General Fund) would serve an additional 119,000 persons in the budget year and 409,000 in 1997-98. The estimates for 1997-98 represent significant increases over the current year--31 percent for the non-Medi-Cal component and 126 percent for the Medi-Cal component.
We note that the above caseload increases would not represent a net increase in the total number of persons receiving family planning services because some persons served in the new program would have otherwise received these services through county health departments or private clinics. Thus, to some extent the proposal would represent a cost shift from counties and private clinics to the state.
| Figure 18 Family Planning Programs Current Programs and the Proposed New Program |
|||
|---|---|---|---|
| Program | Office of Family Planning (OFP) | Medi-Cal Program | New Program |
| Eligibility criteria | Persons ineligible for Medi-Cal, with incomes at or below 200 percent of the federal poverty level | Individuals who meet Medi-Cal eligibility criteria; generally, AFDC-linked beneficiaries below 200 percent of poverty | Same as OFP and Medi-Cal |
| Eligibility determination | By the provider at point of service | County welfare department | Same as OFP (Medi-Cal for full scope services) |
| Average annual caseload | 417,000 | 324,000 | 897,000 in 1996-97 and 1.3 million in 1997-98 |
| Estimated annual expenditures | $46 million General Fund in 1995-96 and $23 million in 1996-97 (and $23 million redirected to new program) | Not available | $43 million General Fund (including redirection from OFP), plus Medi-Cal costs, in 1996-97 |
| Estimated annual cost per eligible | $120 | $160 | $160 |
| Scope of benefits | Contraceptive services and supplies, certain health screens, testing, treatment, and education and counseling on reproductive health-related issues | Same as OFP, except less comprehensive education and counseling services | Same as OFP |
| Copayment or share of cost (SOC) | Persons with incomes over 100 percent of poverty pay a copayment, but cannot be denied services if they do not make the copayment | No SOC for most AFDC-linked beneficiaries; a SOC is required of "medically needy" AFDC eligibles (less than 1 percent of caseload) | Same as OFP |
| Providers |
| All Medi-Cal providers offer family planning services | Same as Medi-Cal and OFP |
| Provider reimbursement system | Annual contract in which providers receive a per capita payment | Fee-for-service claims through the Medi-Cal billing system; capitation rates for persons in managed care arrangements | Billing through the Medi-Cal system |
Funding.The budget proposes a $20 million General Fund augmentation to establish the new program. Figure 19 shows the components of the proposed augmentation, based on a preliminary fiscal analysis provided by the department.
| Figure 19 Proposed Family Planning Program General Fund Augmentation 1996-97 |
||
|---|---|---|
| (Dollars in Thousands) | ||
| Activity | Cost | |
| Increase in the provider rate for the OFP caseload | $8,340 | |
| Increase in the non-Medi-Cal eligible caseload | 5,938 | |
| Increase in the Medi-Cal eligible caseload | 3,100 | |
| New cost to the Medi-Cal billing system for the OFP caseload | 865 | |
| Other (unspecified) | 1,757 | |
| $20,000 | |
We note that, in order to fully fund the program, the department projects it would need an additional $27 million (General Fund) in 1997-98.
Issues Concerning the Proposal. The DHS indicates that the proposal is still under development and certain programmatic and fiscal details are presently unavailable for review. We believe that the general concept of expanding family planning services has merit, based on the goal of reducing unintended pregnancies and the associated savings in other programs, such as welfare. We withhold recommendation at this time, however, due to the following concerns:
Due to major program expansion, over half of all Medi-Cal beneficiaries are scheduled to be enrolled in a "managed care" arrangement by the end of 1996-97.
The department released a "strategic plan" in 1993 intended to rapidly move the Medi-Cal Program toward a "managed care" approach to providing Medi-Cal services throughout California. In this section, we review existing managed care arrangements and the department's strategy for expansion of managed care, and offer comments and recommendations for the Legislature's consideration.
Background.The Legislature and the department have, for several years, attempted to increase the number of Medi-Cal beneficiaries enrolled in managed care arrangements. In particular, legislation accompanying the 1992 Budget Act gave the department broad authority to expand managed care in California, with the goals of improving beneficiary access to care and making the Medi-Cal Program more cost-effective. The department anticipates this number will increase to 3.2 million beneficiaries (58 percent) of the 5.5 million total Medi-Cal eligibles by the end of 1996-97.
Under managed care arrangements, the Medi-Cal Program attempts to control costs by generally reimbursing providers on a "capitated," or per-person basis regardless of the number of services any given individual uses. In addition, the use of specialists and high-cost services requires a physician referral.
This approach contrasts with the fee-for-service system, where Medi-Cal pays providers for each service they provide, and the beneficiary has his or her choice in selecting providers. In a fee-for-service system, utilization is controlled by requiring prior authorization from the Medi-Cal field offices for the more expensive medical services.
The principal managed care arrangements are:
We recommend enactment of legislation requiring that managed care expansion in 12 counties include newly enrolled SSI/SSP-linked beneficiaries, rather than be at the counties' option as the department proposes.
The department's strategic plan focuses on services provided to AFDC-linked beneficiaries and medically indigent children. Additional eligibility categories may enroll at the beneficiary's option, including SSI/SSP-linked beneficiaries.
The department has provided information demonstrating that SSI/SSP-linked beneficiaries are among the eligibility groups where counties are most likely to achieve savings through managed care. According to the department, capitation rates paid to both San Mateo and Santa Barbara Counties in 1995 for their COHS were significantly belowthe fee-for-service equivalent for SSI/SSP-linked beneficiaries. This suggests that these counties have been able to achieve savings among the higher-cost beneficiaries--generally those who are linked to the SSI/SSP Program.
| Figure 20 Counties Designated for Mandatory Implementation of Managed Care 1995-96 and 1996-97 |
||||
|---|---|---|---|---|
| Estimated Implementation Date | ||||
| County | Local Initiative | Commercial Plan(s) | Affected Beneficiaries |
|
| Two-plan model | ||||
| Alameda | 1/96 | 6/96 | 132,409 | |
| Contra Costa | 7/96 | 6/96 | 59,430 | |
| Fresno | NA | 8/96 | 154,201 | |
| Kern | 6/96 | 8/96 | 92,200 | |
| Los Angeles | 10/96 | 8/96 | 1,223,147 | |
| Riverside | 12/96 | 8/96 | 145,332 | |
| San Bernardino | 12/96 | 8/96 | 243,733 | |
| San Francisco | 10/96 | 6/96 | 54,859 | |
| San Joaquin | 2/96 | 8/96 | 87,533 | |
| Santa Clara | 7/96 | 6/96 | 123,137 | |
| Stanislaus | 12/96 | 8/96 | 64,968 | |
| Tulare | 4/96 | 6/96 | 73,538 | |
| COHS model | ||||
| Orange | 9/95 | NA | 128,785 | |
| Santa Cruz | 1/96 | NA | 12,465 | |
| GMC model | ||||
| San Diego | NA | 1/97 | 205,815 | |
| 2,801,552 | |||
| Source: DHS Medi-Cal Managed Care Division. | ||||
Accordingly, we believe that the department's efforts to expand managed care have neglected an area where savings potential exists: the high-cost groups of recipients. We recommend, therefore, the enactment of legislation requiring the inclusion of newly enrolled SSI/SSP-linked beneficiaries in the 12 counties. By limiting the requirement to new beneficiaries, concerns that managed care arrangements would disrupt established beneficiary relationships with a primary care physician would be largely avoided.
We recommend eliminating 48 positions in the department's Medi-Cal field offices and reducing the administrative claims processing contract, to reflect the declining workload due to managed care expansion, for a General Fund savings of $3.3 million. (Reduce Item 4260-101-0001 by $3,280,000.)
The budget proposes expenditures of $28.1 million from all funds ($7.3 million General Fund) in 1996-97 for support of the Medi-Cal field office operations (495 positions). In addition, the budget proposes expenditures of $85.6 million from all funds ($27.5 million General Fund) in 1996-97 for the Medi-Cal claims processing contract.
As stated earlier in our analysis, the department is proceeding with a major expansion of managed care arrangements in the Medi-Cal Program. Consequently, many administrative functions performed for fee-for-service beneficiaries by the department or through contracts with private organizations will instead be administered by managed care providers pursuant to their contracts with the state. These functions include activities performed by Medi-Cal field office staff (such as reviewing and authorizing certain services) and administrative claims processing performed by a private organization under contract with the department. The budget, however, does not reflect the workload-related reductions in the department resulting from the assumption of these responsibilities by managed care providers.
We estimate that these workload reductions would amount to $2.7 million ($716,000 General Fund) for field office staff (48 positions) and $12 million ($2.6 million General Fund) in contract funds for claims processing in 1996-97. Accordingly, we recommend that the budget reflect these reductions for an estimated General Fund savings of $3.3 million.
We note that the department indicates that it is in the process of reviewing its staffing standards and the workload changes due to managed care expansion. We will review the department's findings, if available, prior to the budget hearings and will modify our recommendation, if appropriate.
We recommend that the amount proposed to contract for managed care quality reviews be reduced by $548,000 ($274,000 General Fund) in order to account for the effect of delays in implementing managed care. (Reduce Item 4260-001-0001 by $274,000.)
The budget proposes $1.4 million from all funds ($700,000 General Fund) for the department to contract for an independent review of the quality of services furnished under Medi-Cal managed care contracts, as required under federal law.
According to the department, a review of a managed care contract will not be initiated until the managed care provider has been operating for 12 months, in order to collect sufficient data. The budget proposal assumes that 34 managed care contracts will be in place for over one year and require an independent quality review during 1996-97. Because of delays in implementing managed care, however, we project that only 21 managed care contracts will be in place for over one year and require review in the budget year. Accordingly, we recommend a reduction of $584,000 in all funds ($274,000 from the General Fund).
Return to LAO Home Page